Summary
This study compares the safety and effectiveness of two methods for the prophylaxis of post-operative thromboembolism in neurosurgical patients: A: low-dose heparin (5,000 IU×2 s.c.) started preoperatively and continued daily for one week post-operatively, and B: per-operative electrical calf muscle stimulation with groups of impulses plus post-operative dextran infusions every other day for one week.
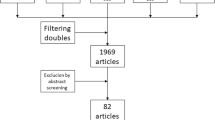
Neurosurgical patients aged 40 years or more with normal laboratory coagulation values and operated under general anaesthesia were included. The 125:I-fibrinogen uptake test (FUT) was used for screening and phlebography for verification of deep venous thrombosis (DVT). 122 patients entered the study and 104 completed the prophylactic protocol, 58 in group A and 46 in group B. The two groups were comparable according to pre-operative data and distribution of diagnoses.
89 patients completed screening for post-operative DVT. We found an overall incidence of 5/49 (10 percent) DVT in group A and 5/40 (13 percent) in group B, compared to a frequency of 32–50 percent for controls without prophylaxis reported in the literature6, 16, 18. In spite of prophylaxis our patients with intracranial neoplasms and intracranial vascular disease showed a relatively higher incidence of DVT, 4/23 (17 percent) and 4/14 (29 percent) respectively, compared to patients with spinal diagnoses 2/25 (8 percent). In combination with cranial diagnoses paretic lower limbs meant an apparent risk factor, 4/7 (57 percent). However, paretic limbs appearing in cases with spinal disorders did not predetermine an unsuccessful prophylaxis, 2/14 (14 percent).
Blood loss, transfusion requirements and post-operative complications did not differ significantly between the two prophylactic groups.
It is concluded that both methods reduce the incidence of post-operative DVT in neurosurgical practice and that they can be used with safety. However, the basic mechanisms behind thromboembolism following parenchymatous brain lesions ought to be studied further to enable a better understanding of the thromboembolic complications and further improvement of the prophylaxis.
Similar content being viewed by others
References
Armitage, P., Statistical Methods in Medical Research, pp. 135–138. Oxford: Blackwell Scientific Publications. 1971.
Auer, L., Disturbances of the coagulatory system in patients with severe cerebral trauma I. Acta Neurochir.43 (1978), 51–59.
Barnett, H. G., Clifford, J. R., Liewelly, R. C., Safety of minidose heparin administration for neurosurgical patients. J. Neurosurg.47 (1977), 27–30.
Becker, J., Scampi, B., The incidence of postoperative venous thrombosis of the legs. Acta Chir. Scand.139 (1972), 357–367.
Brisman, R., Mendell, J., Thromboembolism and brain tumours. J. Neurosurg.38 (1973), 337–338.
Cerrato, D., Ariano, C., Fiacchino, F., Deep vein thrombosis and low-dose heparin prophylaxis in neurosurgical patients. J. Neurosurg.49 (1978), 378–381.
Di Ricco, G., Marini, C., Rindi, M., Ravelli, V., Lutzemberger, L., Tusini, G., Giutini, C., Pulmonary embolism in neurosurgical patients: diagnosis and treatment. J. Neurosurg.60 (1984), 972–975.
Flanc, C., Kakkar, W. W., Clarke, M. B., The detection of venous thrombosis of the legs using I-labelled fibrinogen. Br. J. Surg.55 (1968), 742–747.
Hallenbeck, J. M., Furlow, Jr., T. W., Gralnick, H. R., Influence of Factor VIII/von Willebrand Factor Protein (F VIII/vWF) and F VIII/vWF-Poor Cryoprecipitate on Post-Ischemic Microvascular Reperfusion in the Central Nervous System. Stroke12 (1981), 93–97.
Immelmann, E. J., Jeffery, P., Benatar, S. R., Elliot, M. S., Smith, J. A., Funston, M. R., Shepstone, B. J., Ferguson, A. D., Jacobs, P., Pretorius, J. P. G., Louw, J. H., Failure of low-dose heparin to prevent significant thromboembolic complications in high-risk surgical patients: interim report of prospective trial. Br. Med. J.1 (1979), 1447–1450.
Kågström, E., Local Cerebral Blood Flow in the Recirculation Period Following Complete and Incomplete Cerebral Ischemia. An Experimental Study in Rats. Thesis Lund 1982.
Lindström, B., Holmdahl, C., Jonsson, O., Korsan-Bengtsen, K., Lindberg, S., Petrusson, B., Pettersson, S., Wikstrand, J., Wojciechowski, J., Prediction and prophylaxis of postoperative thromboembolism. A comparison between peroperative calf muscle stimulation with groups of impulses and dextran 40. Br. J. Surg.69 (1982), 633–637.
Lindström, B., Korsan-Bengtsson, K., Jonsson, O., Petrusson, B., Pettersson, S., Wikstrand, J., Electrically induced shortlasting tetanus of the calf muscles for prevention of deep vein thrombosis. Br. J. Surg.69 (1982), 203–206.
Powers, S. K., Edwards, M. S. B., Prophylaxis of thromboembolism in the neurosurgical patient: A review. Neurosurgery4, (1982), 509–513.
Tapaninaho, A., Deep vein thrombosis after aneurysm surgery. Acta Neurochir. (Wien)74 (1985), 18–20.
Valladares, J. B., John Hankinson, M. B., Incidence of lower extremity deep vein thrombosis in neurosurgical patients. Neurosurgery6 (1980), 138–141.
Wetzel, N., Anderson, M. C., Shields, T. W., Pulmonary embolism as a cause of death in the neurosurgical patients. J. Neurosurg.17 (1960), 664–668.
Zelikovski, A., Zucker, G., Eliashiv, A., Reiss, R., Shalit, M., A new sequential pneumatic device for the prevention of deep vein thombosis. J. Neurosurg.54 (1981), 652–654
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Boström, S., Holmgren, E., Jonsson, O. et al. Post-operative thromboembolism in neurosurgery. Acta neurochir 80, 83–89 (1986). https://doi.org/10.1007/BF01812279
Issue Date:
DOI: https://doi.org/10.1007/BF01812279