Abstract
Objective
To evaluate the influence of tidal volume on the capacity of pulse pressure variation (ΔPP) to predict fluid responsiveness.
Design
Prospective interventional study.
Setting
A 31-bed university hospital medico-surgical ICU.
Patients and participants
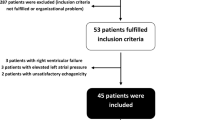
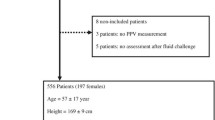
Sixty mechanically ventilated critically ill patients requiring fluid challenge, separated according to their tidal volume.
Intervention
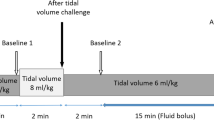
Fluid challenge with either 1,000 ml crystalloids or 500 ml colloids.
Measurements and results
Complete hemodynamic measurements including ΔPP were obtained before and after fluid challenge. Tidal volume was lower than 7 ml/kg in 26 patients, between 7–8 ml/kg in 9 patients, and greater than 8 ml/kg in 27 patients. ROC curve analysis was used to evaluate the predictive value of ΔPP at different tidal volume thresholds, and 8 ml/kg best identified different behaviors. Overall, the cardiac index increased from 2.66 (2.00–3.47) to 3.04 (2.44–3.96) l/min m2 ( P <0.001). It increased by more than 15% in 33 patients (fluid responders). Pulmonary artery occluded pressure was lower and ΔPP higher in responders than in non-responders, but fluid responsiveness was better predicted with ΔPP (ROC curve area 0.76±0.06) than with pulmonary artery occluded pressure (0.71±0.07) and right atrial (0.56±0.08) pressures. Despite similar response to fluid challenge in low (<8 ml/kg) and high tidal volume groups, the percent of correct classification of a 12% ΔPP was 51% in the low tidal volume group and 88% in the high tidal volume group.
Conclusions
ΔPP is a reliable predictor of fluid responsiveness in mechanically ventilated patients only when tidal volume is at least 8 ml/kg.



Similar content being viewed by others
References
Sakka SG, Bredle DL, Reinhart K, Meier-Hellmann A (1999) Comparison between intrathoracic blood volume and cardiac filling pressures in the early phase of hemodynamic instability of patients with sepsis or septic shock. J Crit Care 14:78–83
Michard F, Teboul JL (2002) Predicting fluid responsiveness in ICU patients: a critical analysis of the evidence. Chest 121:2000–2008
Tavernier B, Makhotine O, Lebuffe G, Dupont J, Scherpereel P (1998) Systolic pressure variation as a guide to fluid therapy in patients with sepsis-induced hypotension. Anesthesiology 89:1313–1321
Coriat P, Vrillon M, Perel A, Baron JF, Le Bret F, Saada M, Viars P (1994) A comparison of systolic blood pressure variations and echocardiographic estimates of end-diastolic left ventricular size in patients after aortic surgery. Anesth Analg 78:46–53
Perel A, Pizov R, Cotev S (1987) Systolic blood pressure variation is a sensitive indicator of hypovolemia in ventilated dogs subjected to graded hemorrhage. Anesthesiology 67:498–502
Pinsky MR (2004) Using ventilation-induced aortic pressure and flow variation to diagnose preload responsiveness. Intensive Care Med 30:1008–1010
Vieillard-Baron A, Loubieres Y, Schmitt JM, Page B, Dubourg O, Jardin F (1999) Cyclic changes in right ventricular output impedance during mechanical ventilation. J Appl Physiol 87:1644–1650
Vieillard-Baron A, Chergui K, Augarde R, Prin S, Page B, Beauchet A, Jardin F (2003) Cyclic changes in arterial pulse during respiratory support revisited by Doppler echocardiography. Am J Respir Crit Care Med 168:671–676
Michard F, Boussat S, Chemla D, Anguel N, Mercat A, Lecarpentier Y, Richard C, Pinsky MR, Teboul JL (2000) Relation between respiratory changes in arterial pulse pressure and fluid responsiveness in septic patients with acute circulatory failure. Am J Respir Crit Care Med 162:134–138
Berkenstadt H, Margalit N, Hadani M, Friedman Z, Segal E, Villa Y, Perel A (2001) Stroke volume variation as a predictor of fluid responsiveness in patients undergoing brain surgery. Anesth Analg 92:984–989
Feissel M, Michard F, Mangin I, Ruyer O, Faller JP, Teboul JL (2001) Respiratory changes in aortic blood velocity as an indicator of fluid responsiveness in ventilated patients with septic shock. Chest 119:867–873
Reuter DA, Felbinger TW, Schmidt C, Kilger E, Goedje O, Lamm P, Goetz AE (2002) Stroke volume variations for assessment of cardiac responsiveness to volume loading in mechanically ventilated patients after cardiac surgery. Intensive Care Med 28:392–398
Szold A, Pizov R, Segal E, Perel A (1989) The effect of tidal volume and intravascular volume state on systolic pressure variation in ventilated dogs. Intensive Care Med 15:368–371
Reuter DA, Bayerlein J, Goepfert MS, Weis FC, Kilger E, Lamm P, Goetz AE (2003) Influence of tidal volume on left ventricular stroke volume variation measured by pulse contour analysis in mechanically ventilated patients. Intensive Care Med 29:476–480
The Acute Respiratory Distress Syndrome Network (2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med 342:1301–1308
Brower RG, Lanken PN, MacIntyre N, Matthay MA, Morris A, Ancukiewicz M, Schoenfeld D, Thompson BT (2004) Higher versus lower positive end-expiratory pressures in patients with the acute respiratory distress syndrome. N Engl J Med 351:327–336
Jardin F, Genevray B, Brun-Ney D, Bourdarias JP (1985) Influence of lung and chest wall compliances on transmission of airway pressure to the pleural space in critically ill patients. Chest 88:653–658
Michard F, Chemla D, Richard C, Wysocki M, Pinsky MR, Lecarpentier Y, Teboul JL (1999) Clinical use of respiratory changes in arterial pulse pressure to monitor the hemodynamic effects of PEEP. Am J Respir Crit Care Med 159:935–939
Teboul JL, Pinsky MR, Mercat A, Anguel N, Bernardin G, Achard JM, Boulain T, Richard C (2000) Estimating cardiac filling pressure in mechanically ventilated patients with hyperinflation. Crit Care Med 28:3631–3636
Esteban A, Anzueto A, Frutos F, Alia I, Brochard L, Stewart TE, Benito S, Epstein SK, Apezteguia C, Nightingale P, Arroliga AC, Tobin MJ (2002) Characteristics and outcomes in adult patients receiving mechanical ventilation: a 28-day international study. JAMA 287:345–355
Brun-Buisson C, Minelli C, Bertolini G, Brazzi L, Pimentel J, Lewandowski K, Bion J, Romand JA, Villar J, Thorsteinsson A, Damas P, Armaganidis A, Lemaire F (2004) Epidemiology and outcome of acute lung injury in European intensive care units. Results from the ALIVE study. Intensive Care Med 30:51–61
Denault AY, Gasior TA, Gorcsan J, Mandarino WA, Deneault LG, Pinsky MR (1999) Determinants of aortic pressure variation during positive-pressure ventilation in man. Chest 116:176–186
Bradley TD, Holloway RM, McLaughlin PR, Ross BL, Walters J, Liu PP (1992) Cardiac output response to continuous positive airway pressure in congestive heart failure. Am Rev Respir Dis 145:377–382
Jardin F (2004) Cyclic changes in arterial pressure during mechanical ventilation. Intensive Care Med 30:1047–1050
Vieillard-Baron A, Chergui K, Rabiller A, Peyrouset O, Page B, Beauchet A, Jardin F (2004) Superior vena caval collapsibility as a gauge of volume status in ventilated septic patients. Intensive Care Med 30:1734–1739
Bendjelid K, Suter PM, Romand JA (2003) The respiratory change in preejection period: a new method to predict fluid responsiveness. J Appl Physiol 96:337–342
Romand JA, Shi W, Pinsky MR (1995) Cardiopulmonary effects of positive pressure ventilation during acute lung injury. Chest 108:1041–1048
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
De Backer, D., Heenen, S., Piagnerelli, M. et al. Pulse pressure variations to predict fluid responsiveness: influence of tidal volume. Intensive Care Med 31, 517–523 (2005). https://doi.org/10.1007/s00134-005-2586-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-005-2586-4