Abstract
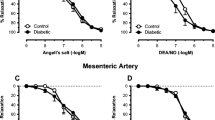
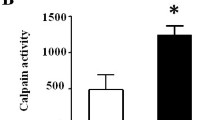
Hyperglycaemia and oxidative stress are known to acutely cause endothelial dysfunction in vitro, but in the initial stages of diabetes, endothelium-dependent relaxation is preserved. The aim of this study was to investigate how endothelium-dependent relaxation is maintained in the early stages of type 1 diabetes. Diabetes was induced in Sprague–Dawley rats with a single injection of streptozotocin (48 mg/kg, i.v.), and after 6 weeks, endothelium-dependent and endothelium-independent relaxations were examined in the thoracic aorta in vitro. Lucigenin-enhanced chemiluminescence was used to measure superoxide generation from the aorta. Diabetes increased superoxide generation by the aorta (2,180 ± 363 vs 986 ± 163 AU/mg dry tissue weight). Acetylcholine (ACh)-induced relaxation was similar in aortae from control (pEC50 7.36 ± 0.09, R max 95 ± 3 %) and diabetic rats (pEC50 7.33 ± 0.10, R max 88 ± 5 %). The ACh-induced relaxation was abolished by the combined presence of the nitric oxide synthase inhibitor N-nitro-l-arginine (L-NNA, 100 μM) and an inhibitor of soluble guanylate cyclase, 1H-[1,2,4]oxadiazolo[4,3-a]quinoxalin-1-one (ODQ, 10 μM) in control rats, but under the same conditions, the diabetic aortic rings showed significant relaxation to ACh (pEC50 6.75 ± 0.15, R max 25 ± 4 %, p < 0.05). In diabetic aortae, the addition of haemoglobin, which inactivates nitric oxide, to L-NNA + ODQ abolished the response to ACh. The addition of the potassium channel blockers, apamin and TRAM-34, to L-NNA + ODQ also abolished the relaxation response to ACh. Diabetes significantly elevated plasma total nitrite/nitrate and increased expression of endothelial nitric oxide synthase (eNOS) and calmodulin in aortae. These data indicate that after 6 weeks of diabetes, despite increased oxidant stress, endothelium-dependent relaxation is maintained due to the increased eNOS expression resulting in increased NO synthesis. In diabetic arteries, NO acts both through and independently of cGMP pathways to cause relaxation.





Similar content being viewed by others
Abbreviations
- EDHF:
-
Endothelium-derived hyperpolarising factor
- eNOS:
-
Endothelial nitric oxide synthase
- sGC:
-
Soluble guanylate cyclase
- ODQ:
-
1H-[1,2,4]Oxadiazolo[4,2-a]quinoxalin-1-one
- L-NNA:
-
N-Nitro-l-arginine
- TRAM-34:
-
1-[(2-Chlorophenyl)(diphenyl)methyl]-1H-pyrazole
- IKCa :
-
Intermediate-conductance calcium-activated potassium channel
- SKCa :
-
Small-conductance calcium-activated potassium channel
- ROS:
-
Reactive oxygen species
- PHMBA:
-
p-Hydroxymercuribenzoic acid
References
Abboud K, Bassila JC, Ghali-Ghoul R, Sabra R (2009) Temporal changes in vascular reactivity in early diabetes mellitus in rats: role of changes in endothelial factors and in phosphodiesterase activity. Am J Physiol Heart Circ Physiol 297:H836–H845
Adak S, Wang Q, Stuehr DJ (2000) Arginine conversion to nitroxide by tetrahydrobiopterin-free neuronal nitric-oxide synthase. Implications for mechanism. J Biol Chem 275:33554–33561
Alencar JL, Chalupsky K, Sarr M, Schini-Kerth V, Vanin AF, Stoclet J-C, Muller B (2003) Inhibition of arterial contraction by dinitrosyl-iron complexes: critical role of the thiol ligand in determining rate of nitric oxide (NO) release and formation of releasable NO stores by S-nitrosation. Biochem Pharmacol 66:2365–2374
Alper G, Olukman M, Irer S, Çalayan O, Duman E, Ylmaz C, Ülker S (2006) Effect of vitamin E and C supplementation combined with oral antidiabetic therapy on the endothelial dysfunction in the neonatally streptozotocin injected diabetic rat. Diabetes Metab Res Rev 22:190–197
Altan VM, Karasu C, Özüari A (1989) The effects of type-1 and type-2 diabetes on endothelium-dependent relaxation in rat aorta. Pharmacol Biochem Behav 33:519–522
Ammar RF Jr, Gutterman DD, Brooks LA, Dellsperger KC (2000) Free radicals mediate endothelial dysfunction of coronary arterioles in diabetes. Cardiovasc Res 47:595–601
Bartnik M, Norhammar A, Ryden L (2007) Hyperglycaemia and cardiovascular disease. J Intern Med 262:145–156
Batenburg WW, Kappers MH, Eikmann MJ, Ramzan SN, de Vries R, Danser AH (2009) Light-induced vs. bradykinin-induced relaxation of coronary arteries: do S-nitrosothiols act as endothelium-derived hyperpolarizing factors? J Hypertens 27:1631–1640
Bates JN, Harrison DG, Myers PR, Minor RL (1991) EDRF: nitrosylated compound or authentic nitric oxide. Basic Res Cardiol 86(Suppl 2):17–26
Beckman JS, Crow JP (1993) Pathological implications of nitric oxide, superoxide and peroxynitrite formation. Biochem Soc Trans 21:330–334
Bitar MS, Wahid S, Mustafa S, Al-Saleh E, Dhaunsi GS, Al-Mulla F (2005) Nitric oxide dynamics and endothelial dysfunction in type II model of genetic diabetes. Eur J Pharmacol 511:53–64
Bojunga J, Dresar-Mayert B, Usadel K-H, Kusterer K, Zeuzem S (2004) Antioxidative treatment reverses imbalances of nitric oxide synthase isoform expression and attenuates tissue-cGMP activation in diabetic rats. Biochem Biophys Res Commun 316:771–780
Brahler S, Kaistha A, Schmidt VJ, Wolfle SE, Busch C, Kaistha BP, Kacik M, Hasenau AL, Grgic I, Si H, Bond CT, Adelman JP, Wulff H, de Wit C, Hoyer J, Kohler R (2009) Genetic deficit of SK3 and IK1 channels disrupts the endothelium-derived hyperpolarizing factor vasodilator pathway and causes hypertension. Circ 119:2323–2332
Brondum E, Kold-Petersen H, Simonsen U, Aalkjaer C (2010) NS309 restores EDHF-type relaxation in mesenteric small arteries from type 2 diabetic ZDF rats. Br J Pharmacol 159:154–165
Bryan RM, You J, Golding EM, Marrelli SP (2005) Endothelium-derived hyperpolarizing factor: a cousin to nitric oxide and prostacyclin. Anesthesiology 102:1261–1277
Bullen ML, Miller AA, Dharmarajah J, Drummond GR, Sobey CG, Kemp-Harper BK (2011) Vasorelaxant and antiaggregatory actions of the nitroxyl donor isopropylamine NONOate are maintained in hypercholesterolemia. Am J Physiol Heart Circ Physiol 301:H1405–H1414
Cameron JD, Cruickshank JK (2007) Glucose, insulin, diabetes and mechanisms of arterial dysfunction. Clin Exp Pharmacol Physiol 34:677–682
Chan ECH, Drummond GR, Woodman OL (2003) 3′,4′-Dihydroxyflavonol enhances nitric oxide bioavailability and improves vascular function after ischemia and reperfusion injury in the rat. J Cardiovasc Pharmacol 42:727–735
Clark SG, Fuchs LC (1997) Role of nitric oxide and Ca++-dependent K+ channels in mediating heterogeneous microvascular responses to acetylcholine in different vascular beds. J Pharmacol Exp Ther 282:1473–1479
Csanyi G, Lepran I, Flesch T, Telegdy G, Szabo G, Mezei Z (2007) Lack of endothelium-derived hyperpolarizing factor (EDHF) up-regulation in endothelial dysfunction in aorta in diabetic rats. Pharmacol Rep 59:447–455
Dalsgaard T, Kroigaard C, Misfeldt M, Bek T, Simonsen U (2010) Openers of small conductance calcium-activated potassium channels selectively enhance NO-mediated bradykinin vasodilatation in porcine retinal arterioles. Br J Pharmacol 160:1496–1508
Ding H, Hashem M, Triggle C (2007) Increased oxidative stress in the streptozotocin-induced diabetic apoE-deficient mouse: changes in expression of NADPH oxidase subunits and eNOS. Eur J Pharmacol 561:121–128
Ellis A, Triggle CR (2003) Endothelium-derived reactive oxygen species: their relationship to endothelium-dependent hyperpolarization and vascular tone. Can J Physiol Pharmacol 81:1013–1028
Fang XD, Yang F, Zhu L, Shen YL, Wang LL, Chen YY (2009) Curcumin ameliorates high glucose-induced acute vascular endothelial dysfunction in rat thoracic aorta. Clin Exp Pharmacol Physiol 36:1177–1182
Frank PG, Hassan GS, Rodriguez-Feo JA, Lisanti MP (2007) Caveolae and caveolin-1: novel potential targets for the treatment of cardiovascular disease. Curr Pharm Des 13:1761–1769
Garcia VMC, Ochoa JE, Elias MM (1999) Effect of early stage of experimental diabetes on vascular functions in isolated perfused kidneys. J Auton Pharmacol 19:97–103
Garcia-Pascual A, Labadia A, Jimenez E, Costa G (1995) Endothelium-dependent relaxation to acetylcholine in bovine oviductal arteries: mediation by nitric oxide and changes in apamin-sensitive K+ conductance. Br J Pharmacol 115:1221–1230
Goel A, Zhang Y, Anderson L, Rahimian R (2007) Gender difference in rat aorta vasodilation after acute exposure to high glucose: Involvement of protein kinase C beta and superoxide but not of Rho kinase. Cardiovasc Res 76:351–360
Gomes MB, Affonso FS, Cailleaux S, Almeida AL, Pinto LF, Tibirica E (2004) Glucose levels observed in daily clinical practice induce endothelial dysfunction in the rabbit macro- and microcirculation. Fundam Clin Pharmacol 18:339–346
Guo Z, Xia Z, Jiang J, McNeill JH (2007) Downregulation of NADPH oxidase, antioxidant enzymes, and inflammatory markers in the heart of streptozotocin-induced diabetic rats by N-acetyl-L-cysteine. Am J Physiol Heart Circ Physiol 292:H1728–H1736
Hink U, Li H, Mollnau H, Oelze M, Matheis E, Hartmann M, Skatchkov M, Thaiss F, Stahl RAK, Warnholtz A, Meinertz T, Griendling K, Harrison DG, Forstermann U, Munzel T (2001) Mechanisms underlying endothelial dysfunction in diabetes mellitus. Circ Res 88:e14–e22
Jay D, Hitomi H, Griendling KK (2006) Oxidative stress and diabetic cardiovascular complications. Free Radic Biol Med 40:183–192
Jesmin S, Zaedi S, Maeda S, Yamaguchi I, Goto K, Miyauchi T (2006) Effects of a selective endothelin A receptor antagonist on the expressions of iNOS and eNOS in the heart of early streptozotocin-induced diabetic rats. Exp Biol Med 231:925–931
Johnstone MT, Creager SJ, Scales KM, Cusco JA, Lee BK, Creager MA (1993) Impaired endothelium-dependent vasodilation in patients with insulin-dependent diabetes mellitus. Circ 88:2510–2516
Karasu Ç (2000) Time course of changes in endothelium-dependent and -independent relaxation of chronically diabetic aorta: role of reactive oxygen species. Eur J Pharmacol 392:163–173
Kim-Shapiro DB, Schechter AN, Gladwin MT (2006) Unraveling the reactions of nitric oxide, nitrite, and hemoglobin in physiology and therapeutics. Arterioscler Thromb Vasc Biol 26:697–705
Komers R, Schutzer WE, Reed JF, Lindsley JN, Oyama TT, Buck DC, Mader SL, Anderson S (2006) Altered endothelial nitric oxide synthase targeting and conformation and caveolin-1 expression in the diabetic kidney. Diabetes 55:1651–1659
Lima B, Forrester MT, Hess DT, Stamler JS (2010) S-nitrosylation in cardiovascular signaling. Circ Res 106:633–646
Lopes-Virella MF, Carter RE, Gilbert GE, Klein RL, Jaffa M, Jenkins AJ, Lyons TJ, Garvey WT, Virella G (2008) Risk factors related to inflammation and endothelial dysfunction in the DCCT/EDIC cohort and their relationship with nephropathy and macrovascular complications. Diabetes Care 31:2006–2012
Malakul W, Thirawarapan S, Suvitayavat W, Woodman OL (2008) Type 1 diabetes and hypercholesterolaemia reveal the contribution of endothelium-derived hyperpolarizing factor to endothelium-dependent relaxation of the rat aorta. Clin Exp Pharmacol Physiol 35:192–200
Myers PR, Minor RL Jr, Guerra R Jr, Bates JN, Harrison DG (1990) Vasorelaxant properties of the endothelium-derived relaxing factor more closely resemble S-nitrosocysteine than nitric oxide. Nature 345:161–163
Nacci C, Tarquinio M, De Benedictis L, Mauro A, Zigrino A, Carratu MR, Quon MJ, Montagnani M (2009) Endothelial dysfunction in mice with streptozotocin-induced type 1 diabetes is opposed by compensatory overexpression of cyclooxygenase-2 in the vasculature. Endocrinology 150:849–861
Ng ESM, Cheng Z-J, Ellis A, Ding H, Jiang Y, Li Y, Hollenberg MD, Triggle CR (2007) Nitrosothiol stores in vascular tissue: modulation by ultraviolet light, acetylcholine and ionomycin. Eur J Pharmacol 560:183–192
Orie NN, Aloamaka CP, Iyawe VI (1993) Duration-dependent attenuation of acetylcholine—but not histamine—induced relaxation of the aorta in diabetes mellitus. Gen Pharmacol 24:329–332
Oyama Y, Kawasaki H, Hattori Y, Kanno M (1986) Attenuation of endothelium-dependent relaxation in aorta from diabetic rats. Eur J Pharmacol 132:75–78
Peredo HA, Rodríguez R, Susemihl MC, Villarreal I, Filinger E (2006) Long-term streptozotocin-induced diabetes alters prostanoid production in rat aorta and mesenteric bed. Auton Autocoid Pharmacol 26:355–360
Pieper GM (1999) Enhanced, unaltered and impaired nitric oxide-mediated endothelium-dependent relaxation in experimental diabetes mellitus: importance of disease duration. Diabetology 42:204–213
Pieper GM, Dembny K, Siebeneich W (1998) Long-term treatment in vivo with NOX-101, a scavenger of nitric oxide, prevents diabetes-induced endothelial dysfunction. Diabetol 41:1220–1226
Riad A, Westermann D, Van Linthout S, Mohr Z, Uyulmaz S, Becher PM, Rutten H, Wohlfart P, Peters H, Schultheiss HP, Tschope C (2008) Enhancement of endothelial nitric oxide synthase production reverses vascular dysfunction and inflammation in the hindlimbs of a rat model of diabetes. Diabetol 51:2325–2332
Rusche KM, Spiering MM, Marletta MA (1998) Reactions catalyzed by tetrahydrobiopterin-free nitric oxide synthase. Biochemistry 37:15503–15512
Satoh M, Fujimoto S, Haruna Y, Arakawa S, Horike H, Komai N, Sasaki T, Tsujioka K, Makino H, Kashihara N (2005) NAD(P)H oxidase and uncoupled nitric oxide synthase are major sources of glomerular superoxide in rats with experimental diabetic nephropathy. Am J Physiol Renal Physiol 288:F1144–F1152
Shen B, Ye C-L, Ye K-H, Liu J-J, Sun P, Jiang J-H (2003) Mechanism underlying enhanced endothelium-dependent vasodilatation in thoracic aorta of early stage streptozotocin-induced diabetic mice. Acta Pharmacol Sin 24:422–428
Sheng J-Z, Braun AP (2007) Small- and intermediate-conductance Ca2+-activated K+ channels directly control agonist-evoked nitric oxide synthesis in human vascular endothelial cells. Am J Physiol Cell Physiol 293:C458–C467
Sheng JZ, Ella S, Davis MJ, Hill MA, Braun AP (2009) Openers of SKCa and IKCa channels enhance agonist-evoked endothelial nitric oxide synthesis and arteriolar vasodilation. FASEB J 23:1138–1145
Shi Y, Ku DD, Man RYK, Vanhoutte PM (2006) Augmented endothelium-derived hyperpolarizing factor-mediated relaxations attenuate endothelial dysfunction in femoral and mesenteric, but not in carotid arteries from type I diabetic rats. J Pharmacol Exp Ther 318:276–281
Sobey CG, Weiler JM, Boujaoude M, Woodman OL (2004) Effect of short-term phytoestrogen treatment in male rats on nitric oxide-mediated responses of carotid and cerebral arteries: comparison with 17beta-estradiol. J Pharmacol Exp Ther 310:135–140
Stadler K, Jenei V, von Bolcshazy G, Somogyi A, Jakus J (2003) Increased nitric oxide levels as an early sign of premature aging in diabetes. Free Radic Biol Med 35:1240–1251
Stankevicius E, Lopez-Valverde V, Rivera L, Hughes AD, Mulvany MJ, Simonsen U (2006) Combination of Ca2+-activated K+ channel blockers inhibits acetylcholine-evoked nitric oxide release in rat superior mesenteric artery. Br J Pharmacol 149:560–572
Stankevicius E, Dalsgaard T, Kroigaard C, Beck L, Boedtkjer E, Misfeldt MW, Nielsen G, Schjorring O, Hughes A, Simonsen U (2011) Opening of small and intermediate calcium-activated potassium channels induces relaxation mainly mediated by nitric-oxide release in large arteries and endothelium-derived hyperpolarizing factor in small arteries from rat. J Pharmacol Exp Ther 339:842–850
Stockklauser-Färber K, Ballhausen T, Laufer A, Rösen P (2000) Influence of diabetes on cardiac nitric oxide synthase expression and activity. Biochim Biophys Acta (BBA) - Mol Basis Dis 1535:10–20
Sullivan JC, Pollock JS (2006) Coupled and Uncoupled NOS: Separate But Equal? Circ Res 98:717–719
Takahashi S, Mendelsohn ME (2003) Calmodulin-dependent and -independent activation of endothelial nitric-oxide synthase by heat shock protein 90. J Biol Chem 278:9339–9344
Vera R, Sanchez M, Galisteo M, Villar IC, Jimenez R, Zarzuelo A, Perez-Vizcaino F, Duarte J (2007) Chronic administration of genistein improves endothelial dysfunction in spontaneously hypertensive rats: involvement of eNOS, caveolin and calmodulin expression and NADPH oxidase activity. Clin Sci (Lond) 112:183–191
Wendt MC, Daiber A, Kleschyov AL, Mulsch A, Sydow K, Schulz E, Chen K, Keaney JJF, Lassegue B, Walter U, Griendling KK, Munzel T (2005) Differential effects of diabetes on the expression of the gp91phox homologues nox1 and nox4. Free Radic Biol Med 39:381–391
Woodman OL, Missen MA, Boujaoude M (2004) Daidzein and 17 beta-estradiol enhance nitric oxide synthase activity associated with an increase in calmodulin and a decrease in caveolin-1. J Cardiovasc Pharmacol 44:155–163
Yuill KH, Yarova P, Kemp-Harper BK, Garland CJ, Dora KA (2011) A novel role for HNO in local and spreading vasodilatation in rat mesenteric resistance arteries. Antioxid Redox Signal 14:1625–1635
Acknowledgments
The authors would like to acknowledge the help from Mr C.H. Leo during the course of the study. Anjali Joshi was supported by a Melbourne University International Research Scholarship.
Conflict of interest
The authors declare that they do not have any competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Joshi, A., Woodman, O.L. Increased nitric oxide activity compensates for increased oxidative stress to maintain endothelial function in rat aorta in early type 1 diabetes. Naunyn-Schmiedeberg's Arch Pharmacol 385, 1083–1094 (2012). https://doi.org/10.1007/s00210-012-0794-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-012-0794-3