Abstract
Purpose
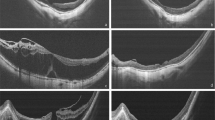
To investigate the vitreoretinal relationship in eyes with full-thickness macular hole (FTMH) without retinal schisis or detachment. Eyes with and without high myopia were compared using slit-lamp biomicroscopy, optical coherence tomography (OCT), and intraoperative observations.
Methods
Clinical records of 34 consecutive cases of FTMH without schisis or detachment in highly myopic eyes (refractive error larger than −6.0 diopters or axial length >26 mm) were retrospectively reviewed. All eyes underwent pars plana vitrectomy between 2006 and 2013. An additional 43 consecutive cases of FTMH in eyes without high myopia were also reviewed to serve as controls. All control patients underwent surgery during the same period. Ophthalmological, OCT, and intraoperative findings, and vitreoretinal interface features were documented in both groups. Anatomical closure rate and final best-corrected visual acuity (BCVA) were compared between groups.
Results
Premacular tissue was identified during surgery in 21 of 34 high myopia patients (61.8 %) and three of 43 control patients (7.0 %). The high myopia group showed two layers of premacular membranes. Two cases had a shiny, loose inner membrane, 13 cases had a tightly adherent outer membrane, and six cases had both. Only a tightly adherent membrane was found in controls. In the high myopia group, 11 of 21 eyes (52.4 %) did not have a preretinal membrane identified preoperatively. Anatomical closure was achieved in 91.2 and 95.3 % of high myopia and control patients respectively (p = 0.65). No significant intergroup difference in final BCVA was observed.
Conclusion
Premacular tissue was found in 61.8 % of eyes with high myopia and FTMH without retinal schisis or detachment. Anatomically successful surgical closure in high myopia patients was achieved at a rate comparable to their idiopathic counterparts.



Similar content being viewed by others
References
Bainbridge J, Herbert E, Gregor Z (2008) Macular holes: vitreoretinal relationships and surgical approaches. Eye 22:1301–1309
Wu TT, Kung YH (2012) Comparison of anatomical and visual outcomes of macular hole surgery in patients with high myopia vs non-high myopia: a case–control study using optical coherence tomography. Graefes Arch Clin Exp Ophthalmol 250:327–331
Mester V, Kuhn F (2000) Internal limiting membrane removal in the management of full-thickness macular holes. Am J Ophthalmol 129:769–777
Freeman WR, Azen SP, Kim JW et al (1997) Vitrectomy for the treatment of full-thickness stage 3 or 4 macular holes: results of a multicentered randomized clinical trial. Arch Ophthalmol 115(1):11–21
Ezra E, Gregor ZJ, Moorfields Macular Hole Study Group (2004) Surgery for idiopathic full-thickness macular hole: two-year results of a randomized clinical trial comparing natural history, vitrectomy, and vitrectomy plus autologous serum: Moorfields Macular Hole Study Group Report No. 1. Arch Ophthalmol 122(2):224–236
Abdelkader E, Lois N (2008) Internal limiting membrane peeling in vitreo-retinal surgery. Surv Ophthalmol 53:368–396
Tanaka Y, Shimada N, Moriyama M et al (2011) Natural history of lamellar macular holes in highly myopic eyes. Am J Ophthalmol 15:96–99.e1
Fang X, Zheng X, Weng Y et al (2009) Anatomical and visual outcome after vitrectomy with triamcinolone acedonide-assisted epiretinal membrane removal in highly myopic eyes with retinal detachment due to macular hole. Eye 23:248–254
Jo Y, Ikuno Y, Nishida K (2012) Retinoschisis: a predictive factor in vitrectomy for macular holes without retinal detachment in highly myopic eyes. Br J Ophthalmol 96:197–200
Kuo HK, Lin JW, Kao ML, Liu CC (2004) Clinicopathological study of the idiopathic macular hole: comparison of epiretinal membrane peeling and internal limiting membrane peeling. Ophthalmologica 218:31–35
Sakaguchi H, Ikuno Y, Choi JS, Ohji M, Tano T (2004) Multiple components of epiretinal tissues detected by triamcinolone and indocyanine green in macular hole and retinal detachment as a result of high myopia. Am J Ophthalmol 138:1079–1081
Chen YP, Chen TL, Yang KR et al (2006) Treatment of retinal detachment resulting from posterior staphyloma-associated macular hole in highly myopic eyes. Retina 26:25–31
Kao TY, Yang CM, Yeh PT (2013) The value of combining autofluorescence and optical coherence tomography in predicting the visual prognosis of sealed macular holes. Am J Ophthalmol 156(1):149–156
Garcia-Arumi J, Boixadera A, Martinez-Castillo V et al (2012) Surgery for myopic macular hole without retinal detachment. European Ophthalmic Review 4(6):204–207
Liu HY, Zou HD, Liu K et al (2011) Posterior vitreous cortex contributes to macular hole in highly myopic eyes with retinal detachment. Chin Med J 124(16):2474–2479
Worst JG (1977) Cisternal systems of the fully developed vitreous body in the young adult. Trans Ophthalmol Soc U K 97:550–554
Kishi S, Hagimura N, Shimizu K (1996) The role of the premacular liquefied pocket and premacular vitreous cortex in idiopathic macular hole development. Am J Ophthalmol 122:622–628
Alkabes M, Padilla L, Salinas C et al (2013) Assessment of OCT measurements as prognostic factors in myopic macular hole surgery without foveoschisis. Graefes Arch Clin Exp Ophthalmol 251:2521–2527
Qu J, Zhao M, Jiang Y et al (2012) Vitrectomy outcomes in eyes with high myopic macular hole without retinal detachment. Retina 32(2):275–280
Alkabes M, Pichi F, Nucci P et al (2014) Anatomical and visual outcomes in high myopic macular hole (HM-MH) without retinal detachment: a review. Graefes Arch Clin Exp Ophthalmol 252(2):191–199
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wu, LL., Ho, TC., Yang, CH. et al. Vitreo-retinal relationship and post-operative outcome of macular hole repair in eyes with high myopia. Graefes Arch Clin Exp Ophthalmol 254, 7–14 (2016). https://doi.org/10.1007/s00417-015-2986-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-015-2986-2