Abstract
Purpose
Two main techniques are commonly used during laparoscopic right hemicolectomy in order to perform the ileocolic anastomosis: intracorporeal (IA) and extracorporeal (EA). The aim of this study was to evaluate the safety of the two techniques.
Methods
A systematic review was carried out to identify studies comparing IA and EA. The primary endpoint was anastomotic leakage. The secondary endpoints were intra- and postoperative results. A meta-analysis was carried out using the random-effects model.
Results
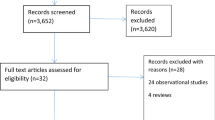
Fourteen studies matched the selection criteria, enrolling 1717 patients (50.3 % IA, 49.7 % EA). The anastomotic leakage was similar in the IA and the EA groups (3.4 vs. 4.6 %, respectively) with a risk difference (RD) of −0.01 (95 % CI = −0.03 to 0.01; P = 0.120). IA group had lower overall complication rate (27.6 vs. 38.4 %; RD = −0.15; 95 % CI = 0.27 to −0.04; P = 0.009) and wound infection rate (4.9 vs. 8.9 %; RD = 0.52; −0.03; 95 % CI = −0.06 to −0.01; P = 0.030). Time to first oral intake (weighted mean difference (WMD) = −1; 95 % CI = −1.59 to −0.41; P < 0.001), length of hospital stay (WMD = −1.13; 95 % CI = −1.90 to −0.35; P = 0.004) and minilaparotomy size (WMD = −26; 95 % CI = −38 to −13; P < 0.001) were shorter in IA patients. The incisional hernia rate was lower in the IA group (2.3 vs. 13.7 %) with an RD of −0.09 (95 % CI = −0.17 to −0.02; P = 0.020). There were no differences in operative time, blood loss, conversion, internal hernia, reoperation, mortality, time to first flatus and defecation, analgesic required, number of lymph nodes harvested and length of distal margin.
Conclusions
Laparoscopic right hemicolectomy with IA is a safe alternative to EA. Additional well-structured, prospective randomised trials are needed to confirm all the advantages regarding postoperative results which were pointed out in our study.





Similar content being viewed by others
References
Colon Cancer Laparoscopic or Open Resection Study Group, Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, Påhlman L, Cuesta MA, Msika S, Morino M, Lacy A, Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10(1):44–52
Chaves JA, Idoate CP, Fons JB et al (2011) A case–control study of extracorporeal versus intracorporeal anastomosis in patients subjected to right laparoscopic hemicolectomy. Cir Esp 89:24–30
Fabozzi M, Allieta R, Contul RB et al (2010) Comparison of short- and medium-term results between laparoscopically assisted and totally laparoscopic right hemicolectomy: a case–control study. Surg Endosc Interv Tech 24:2085–2091
Scatizzi M, Kroening KC, Borrelli A et al (2010) Extracorporeal versus intracorporeal anastomosis after laparoscopic right colectomy for cancer: a case–control study. World J Surg 34:2902–2908
Anania G, Santini M, Scagliarini L et al (2012) A totally mini-invasive approach for colorectal laparoscopic surgery. World J Gastroenterol 18(29):3869–3874
Erguner I, Aytac E, Baca B et al (2013) Total laparoscopic approach for the treatment of right colon cancer: a technical critique. Asian J Surg 36:58–63
Roscio F, Bertoglio C, De Luca A et al (2012) Totally laparoscopic versus laparoscopic assisted right colectomy for cancer. Int J Surg 10:290–295
Lee KH, Ho J, Akmal Y et al (2013) Short- and long-term outcomes of intracorporeal versus extracorporeal ileocolic anastomosis in laparoscopic right hemicolectomy for colon cancer. Surg Endosc Interv Tech 27:1986–1990
Magistro C, Di Lernia S, Ferrari G et al (2013) Totally laparoscopic versus laparoscopic-assisted right colectomy for colon cancer: is there any advantage in short-term outcomes? A prospective comparative assessment in our center. Surg Endosc Interv Tech 27:2613–2618
Marchesi F, Pinna F, Percalli L et al (2013) Totally laparoscopic right colectomy: theoretical and practical advantages over the laparo-assisted approach. J Laparoendosc Adv Surg Tech 23:418–424
Milone M, Elmore U, Di Salvo E et al (2015) Intracorporeal versus extracorporeal anastomosis. Results from a multicentre comparative study on 512 right-sided colorectal cancers. Surg Endosc 29(8):2314–2320
Trastulli S, Coratti A, Guarino S et al (2015) Robotic right colectomy with intracorporeal anastomosis compared with laparoscopic right colectomy with extracorporeal and intracorporeal anastomosis: a retrospective multicentre study. Surg Endosc 29:1512–1521
Vergis AS, Steigerwald SN, Bhojani FD et al (2015) Laparoscopic right hemicolectomy with intracorporeal versus extracorporeal anastamosis: a comparison of short-term outcomes. Can J Surg 58:63–68
Hanna MH, Hwang GS, Phelan MJ et al (2015) Laparoscopic right hemicolectomy: short- and long-term outcomes of intracorporeal versus extracorporeal anastomosis. Surg Endosc
Shapiro R, Keler U, Segev L et al (2015) Laparoscopic right hemicolectomy with intracorporeal anastomosis: short- and long-term benefits in comparison with extracorporeal anastomosis. Surg Endosc
Carnuccio P, Jimeno J, Parés D (2014) Laparoscopic right colectomy: a systematic review and meta-analysis of observational studies comparing two types of anastomosis. Tech Coloproctol 18:5–12
Cirocchi R, Trastulli S, Farinella E et al (2013) Intracorporeal versus extracorporeal anastomosis during laparoscopic right hemicolectomy - systematic review and meta-analysis. Surg Oncol 22:1–13
Feroci F, Lenzi E, Garzi A et al (2013) Intracorporeal versus extracorporeal anastomosis after laparoscopic right hemicolectomy for cancer: a systematic review and meta-analysis. Int J Color Dis 28:1177–1186
van Oostendorp S, Elfrink A, Borstlap W et al (2016) Intracorporeal versus extracorporeal anastomosis in right hemicolectomy: a systematic review and meta-analysis. Surg Endosc
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700
Rahbari NN, Weitz J, Hohenberger W et al (2010) Definition and grading of anastomotic leakage following anterior resection of the rectum: a proposal by the International Study Group of Rectal Cancer. Surgery 147:339–351
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Clarke M, Horton R (2001) Bringing it all together: Lancet-Cochrane collaborate on systematic reviews. Lancet 357:1728
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. JAMA 283:2008–2012
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13
Messori A, Maratea D, Fadda V, Trippoli S (2013) Using risk difference as opposed to odds-ratio in meta-analysis. Int J Cardiol 164(1):127
Zapletal E, LeMaitre D, Menard J et al (1996) The number needed to treat: a clinically useful nomogram in its proper context. BMJ 312:426–429
Mantel N, Haenszel W (1959) Statistical aspects of the analysis of data from retrospective studies of disease. J Natl Cancer Inst 22:719–748
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Egger M, Davey Smith G, Schneider M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56:455–463
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558
Sakpal TV (2010) Sample size estimation in clinical trial. Perspect Clin Res 1:67–69
Hellan M, Anderson C, Pigazzi A (2009) Extracorporeal versus intracorporeal anastomosis for laparoscopic right hemicolectomy. JSLS 13:312–317
Grams J, Tong W, Greenstein AJ et al (2010) Comparison of intracorporeal versus extracorporeal anastomosis in laparoscopic-assisted hemicolectomy. Surg Endosc 24(8):1886–1891
Makino T, Trencheva K, Shukla PJ et al (2014) The influence of obesity on short- and long-term outcomes after laparoscopic surgery for colon cancer: a case-matched study of 152 patients. Surgery 156:661–668
Aytac E, Stocchi L, Ozdemir Y et al (2013) Factors affecting morbidity after conversion of laparoscopic colorectal resections. Br J Surg 100:1641–1648
Melich G, Jeong DH, Hur H et al (2014) Laparoscopic right hemicolectomy with complete mesocolic excision provides acceptable perioperative outcomes but is lengthy—analysis of learning curves for a novice minimally invasive surgeon. Can J Surg 57:331–336
Vlug MS, Wind J, Hollmann MW et al (2011) Laparoscopy in combination with fast track multimodal management is the best perioperative strategy in patients undergoing colonic surgery: a randomized clinical trial (LAFA-study). Ann Surg 254:868–875
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Claudio Ricci declares that he did not receive any funding for this manuscript.
Riccardo Casadei declares that he did not receive any funding for this manuscript.
Vincenzo Alagna declares that he did not receive any funding for this manuscript.
Elia Zani declares that he did not receive any funding for this manuscript.
Giovanni Taffurelli declares that he did not receive any funding for this manuscript.
Carlo Alberto Pacilio declares that he did not receive any funding for this manuscript.
Francesco Minni declares that he did not receive any funding for this manuscript.
Conflicts of interest
The authors declare that they no conflict of interest.
Ethical approval
This article does not contain any studies with human participants carried out by any of the authors.
Rights and permissions
About this article
Cite this article
Ricci, C., Casadei, R., Alagna, V. et al. A critical and comprehensive systematic review and meta-analysis of studies comparing intracorporeal and extracorporeal anastomosis in laparoscopic right hemicolectomy. Langenbecks Arch Surg 402, 417–427 (2017). https://doi.org/10.1007/s00423-016-1509-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-016-1509-x