Abstract
Purpose
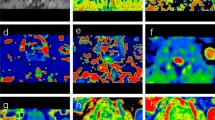
To explore the diagnostic value of monoexponential diffusion-weighted imaging (DWI), diffusion kurtosis imaging (DKI), and dynamic contrast-enhanced (DCE)-MRI for differentiating between spinal malignant and non-malignant tumors lacking typical imaging signs and correlation between the parameters of the three models.
Methods
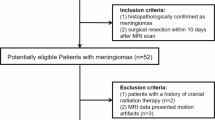
DWI, DKI, and DCE-MRI examinations were performed in 39 and 27 cases of spinal malignant and non-malignant tumors, respectively. Two radiologists independently evaluated apparent diffusion coefficient (ADC), mean diffusivity (MD), and mean kurtosis (MK) of the DWI and DKI models, and volume transfer constant (Ktrans), rate constant (kep), and extracellular extravascular volume ratio (ve) of the DCE-MRI model for post-processing analyses. Statistical differences of parameters were compared using an independent sample t test. The sensitivity, specificity, and the area under the receiver operating characteristic (ROC) curve were determined. Pearson correlation analysis was used to evaluate the correlation between these parameters.
Results
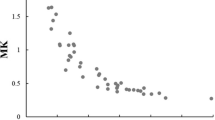
ADC, MD, and ve were significantly lower, while MK and kep were significantly higher for spinal malignant tumors than for non-malignant tumors. The MK had the highest area under the ROC curve of 0.940 and sensitivity (96.3%). Ve was weakly positively correlated with ADC (r = 0.468) and MD (r = 0.363) and weakly negatively correlated with MK (r = −0.469). kep was weakly positively correlated with MK (r = 0.375). Ktrans was weakly positively correlated with ADC (r = 0.325).
Conclusions
Monoexponential DWI, DKI, and DCE-MRI have potential value in the differentiation of spinal malignant from non-malignant tumors lacking typical imaging signs, and there is a certain correlation between the parameters of the three models.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.





Similar content being viewed by others
Abbreviations
- ADC:
-
Apparent diffusion coefficient
- AUC:
-
Area under curve
- DCE-MRI:
-
Dynamic contrast-enhanced-MRI
- DKI:
-
Diffusion kurtosis imaging
- DWI:
-
Diffusion-weighted imaging
- FA:
-
Flip angle
- FOV:
-
Field of view
- ICC:
-
Intraclass correlation coefficient
- K trans :
-
Volume transfer constant
- k ep :
-
Rate constant
- MD:
-
Mean diffusivity
- MK:
-
Mean kurtosis
- ROC:
-
Receiver operating characteristic curve
- ROI:
-
Region of interest
- v e :
-
Extracellular extravascular volume ratio
References
Zambo I, Veselý K (2014) WHO classification of tumours of soft tissue and bone 2013: the main changes compared to the 3rd edition. Cesk Patol 50(2):64–70
Wang Fengxian, Chu Chen, Zhao Cheng et al (2019) Diffusion kurtosis imaging in sacroiliitis to evaluate the activity of ankylosing spondylitis. J Magn Reson Imaging 49(1):101–108
Hui ES, Cheung MM, Qi L et al (2008) Towards better MR characterization of neural tissues using directional diffusion kurtosis analysis. Neurimage 42(1):122–134
Surov A, Nagata S, Razek AA, Tirumani SH, Wienke A, Kahn T (2015) Comparison of ADC values in different malignancies of the skeletal musculature: a multicentric analysis. Skelet Radiol 44(7):995–1000
Ahlawat S, Khandheria P, Subhawong TK, Fayad LM (2015) Differentiation of benign and malignant skeletal lesions with quantitative diffusion weighted MRI at 3T. Eur J Radiol 84(6):1091–1097
Surov A, Behrmann C (2014) Diffusion-weighted imaging of skeletal muscle lymphoma. Skelet Radiol 43(7):899–903
Jenson JH, Helpern JA, Ramani A et al (2005) Diffusional kurtosis imaging: the quantification of non-gaussian water diffusion by means of magnetic resonance imaging. Magn Reson Med 53(6):1432–1440
Bai Y, Lin YS, Tian J (2016) Grading of gliomas by using monoexponential, biexponential, and stretched exponential diffusion weighted MR imaging and diffusion kurtosis MR imaging. Radiology 278(2):496–504
Zhu L, Pan ZL, Ma Q et al (2017) Diffusion kurtosis imaging study of rectal adenocarcinoma associated with histopathologic prognostic factors: preliminary findings. Radiology 284(1):66–76
Sun K, Chen X, Chai W et al (2015) Breast cancer: diffusion kurtosis MR imaging-diagnostic accuracy and correlation with clinical-pathologic factors. Radiology 277(1):46–55
Nogueira L, Brandao S, Matos E et al (2014) Application of the diffusion kurtosis model for the study of breast lesions. Eur Radiol 24(6):1197–1203
Ogawa Masaki, Kan Hirohito, Arai Nobuyuki et al (2019) Differentiation between malignant and benign musculoskeletal tumors using diffusion kurtosis imaging. Skelet Radiol 48(2):285–292
Zheng D, Chen Y, Chen Y et al (2014) Dynamic contrast-enhanced MRI of nasopharyngeal carcinoma: a preliminary study of the correlations between quantitative parameters and clinical stage. J Magn Reson Imaging 39(4):940–948
Saha A, Peck KK, Lis E et al (2014) Magnetic resonance perfusion characteristics of hypervascular renal and hypovascular prostate spinal metastases: clinical utilities and implications. Spine 39(24):E1433–E1440
Khadem NR, Karimi S, Peck KK et al (2012) Characterizing hypervascular and hypovascular metastases and normal bone marrow of the spine using dynamic contrast enhanced MR imaging. AJNR Am J Neuroradiol 33(11):2178–2185
Lang N, Su MY, Yu HJ et al (2013) Differentiation of myeloma and metastatic cancer in the spine using dynamic contrast-enhanced MRI. Magn Reson Imaging 31(8):1285–1291
Lang N, Su MY, Xing X et al (2017) Morphological and dynamic contrast enhanced MR imaging features for the differentiation of chordoma and giant cell tumors in the axial skeleton. J Magn Reson Imaging 45(4):1068–1075
Lang N, Su MY, Yu HJ et al (2015) Differentiation of tuberculosis and metastatic cancer in the spine using dynamic contrast-enhanced MRI. Eur Spine J 24(8):1729–1737
Tofts PS (1997) Modeling tracer kinetics in dynamic Gd-DTPA MR imaging. J Magn Reson Imaging 7(1):91–101
Hatakenaka M, Soeda H, Yabuuchi H et al (2008) Apparent diffusion coefficients of breast tumors: clinical application. Magn Reson Med Sci 7(1):23–29
Hui ES, Cheung MM, Qi L et al (2008) Advanced MR diffusion characterization of neural tissue using directional diffusion kurtosis analysis. Conf Proc IEEE Eng Med Biol Soc 2008:3941–3944
Huang W, Chen YY, Fedorov A et al (2016) The impact of arterial input function determination variations on prostate dynamic contrast-enhanced magnetic resonance imaging pharmacokinetic modeling: a multicenter data analysis challenge. Tomography 2(1):56–66
Hu H, Xu XQ, Liu H et al (2017) Orbital benign and malignant lymphoproliferative disorders: differentiation using semi-quantitative and quantitative analysis of dynamic contrast-enhanced magnetic resonance imaging. Eur J Radiol 88:88–94
Park M, Kim J, Choi YS et al (2016) Application of dynamic contrast-enhanced MRI parameters for differentiating squamous cell carcinoma and malignant lymphoma of the oropharynx. AJR Am J Roentgenol 206(2):401–407
Haradome K, Haradome H, Usui Y et al (2014) Orbital lymphoproliferative disorders (OLPDs): value of MR imaging for differentiating orbital lymphoma from benign OPLDs. AJNR Am J Neuroradiol 35(10):1976–1982
Li Ting, Tao Yu, Li Lyu et al (2018) Use of diffusion kurtosis imaging and quantitative dynamic contrast-enhanced MRI for the differentiation of breast tumors. J Magn Reson Imaging 48(5):1358–1366
Acknowledgements
This study has received funding by National Natural Science Foundation of China (81701648, 81971578) and Clinical key project of Peking University Third Hospital (BYSY2018007).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, J., Chen, Y., Zhang, E. et al. Use of monoexponential diffusion-weighted imaging and diffusion kurtosis imaging and dynamic contrast-enhanced-MRI for the differentiation of spinal tumors. Eur Spine J 29, 1112–1120 (2020). https://doi.org/10.1007/s00586-020-06330-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06330-w