Abstract
Identification of cytotoxic T lymphocyte (CTL) epitopes from tumor antigens is essential for the development of peptide vaccines against tumor immunotherapy. Among all the tumor antigens, the caner-testis (CT) antigens are the most widely studied and promising targets. PLAC1 (placenta-specific 1, CT92) was considered as a novel member of caner-testis antigen, which expressed in a wide range of human malignancies, most frequently in breast cancer. In this study, three native peptides and their analogues derived from PLAC1 were predicted by T cell epitope prediction programs including SYFPEITHI, BIMAS and NetCTL 1.2. Binding affinity and stability assays in T2 cells showed that two native peptides, p28 and p31, and their analogues (p28-1Y9 V, p31-1Y2L) had more potent binding activity towards HLA-A*0201 molecule. In ELISPOT assay, the CTLs induced by these four peptides could release IFN-γ. The CTLs induced by these four peptides from the peripheral blood mononuclear cells (PBMCs) of HLA-A*02+ healthy donor could lyse MCF-7 breast cancer cells (HLA-A*0201+, PLAC1+) in vitro. When immunized in HLA-A2.1/Kb transgenic mice, the peptide p28 could induce the most potent peptide-specific CTLs among these peptides. Therefore, our results indicated that the peptide p28 (VLCSIDWFM) could serve as a novel candidate epitope for the development of peptide vaccines against PLAC1-positive breast cancer.
Similar content being viewed by others
Introduction
The immune system has been implicated in controlling tumors. The evidence collected in the last decade indicated that CD8+ T cells which recognize peptide fragments (epitopes) derived from tumor antigens in a human leukocyte antigen (HLA)-restricted manner could play an important role in this process (Roth et al. 1994; Boon and van der Bruggen 1996). The cytotoxic T lymphocytes (CTLs) could not only directly lyse tumor cells but also secrete cytokines, such as tumor necrosis factor (TNF) and interferon (IFN)-γ, which could kill tumor cells indirectly. Therefore, peptide vaccine therapy based on epitopes from tumor antigens is a promising way to tumor immunotherapy and the identification of epitopes is the bottleneck in peptide vaccine development. Cancer testis (CT) antigens are the most widely studied and promising tumor antigens for tumor immunotherapy. They are expressed in various tumors but not in normal tissues with the exception of immune privileged organs, such as testis and placenta (Coulie et al. 1994). The epitopes derived from CT antigens such as MAGE-1 (Salgaller et al. 1994), MAGE-3 (Sadanaga et al. 2001), and NY-ESO-1 (Jager et al. 1998) have been proven to elicit CTL response. Furthermore, more evidence suggested that the development of specific immunotherapy based on multiple antigens might be clinically beneficial (Sadanaga et al. 2001).
The trophoblast-specific protein PLAC1 (placenta-specific 1) has been recently considered as a member of CT antigens. PLAC1 is from a human X-linked gene with placenta-specific expression, ectopically expressed in a wide range of human malignancies, most frequently in breast cancer, and is involved in the proliferation, migration and invasion of the breast cancer (Cocchia et al. 2000). The PLAC1 gene encodes a membrane-associated protein which is speculated to serve as a receptor-like function modulating specific cell–cell or ligand–receptor interactions unique to the maternal placental interface (Fant et al. 2002). Knockdown of PLAC1 is associated with decreased expression of cyclin D1 and reduced phosphorylation of AKT kinase. PLAC1 is frequently activated and highly expressed in a variety of tumors, particularly in breast cancer. Fifty-one of 62 (82%) primary breast cancer samples scored positive for PLAC1 expression, with 24% (15 of 62) showing low, 40% (25 of 62) showing intermediate, and 17% (11 of 62) showing high expression (Koslowski et al. 2007). RNAi mediated silencing of PLAC1 in breast cancer cells MCF-7 and BT-549 profoundly impaired their motility, migration and invasion, and induced G1-S cell cycle block with nearly complete abrogation of proliferation (Koslowski et al. 2007). HLA-A*0201 is the most widely expressed HLA-I molecule in Chinese population. Therefore, identification of HLA-A*0201-restricted CTL epitopes derived from PLAC1 would be very important to the immunotherapy of breast cancer.
Many studies reported that two aliphatic hydrophobic anchor residues located at position 2 and 9 of the epitopes could be essential for their binding to HLA-A*0201 molecule. Ruppert et al. found that leucine (L) and methione (M) at position 2, and valine (V), isoleucine (I), and leucine (L) at position 9 were associated with the optimal binding capacity (Ruppert et al. 1993; Lazoura and Apostolopoulos 2005). Tourdot et al. described that the immunogenicity of the HLA-A*0201-binding peptides could be enhanced by introducing a tyrosine at the first position (1Y) (Tourdot et al. 2000). Therefore, the analogues of candidate epitopes were usually designed by introducing a tyrosine at position 1, a leucine at position 2 and/or a valine at position 9.
In the present study, HLA-A2-restricted candidate epitopes were predicted from PLAC1 by using three prediction programs. Native peptides and their analogues with higher scores were selected to synthesize. Binding assay in T2 cells was performed to determine their capacity of binding affinity and stability toward HLA-A*0201 molecule. Then, the immunogenicity of these peptides was investigated in vitro (in PBMCs from healthy donors) and in vivo (in HLA-A2.1/Kb transgenic mice).
Materials and methods
Cell lines, mice and blood samples
The TAP-deficient T2 cell line (HLA-A*0201+, PLAC1−) was kindly supplied by Professor Yu-zhang Wu (Third Military Medical University, China). The breast cancer cell line MCF-7 (HLA-A*0201+,PLAC1+)was purchased from the American Type Culture Collection (ATCC, USA). The T2 and MCF-7 cell lines were cultured in RPMI 1640 (Gibco, US) medium supplemented with 10% fetal bovine serum, 100 units/mL penicillin, and 100 μg/mL streptomycin in an incubator with a humidified atmosphere containing 5% CO2.
HLA-A2.1/Kb transgenic mice (Vitiello et al. 1991) were kindly supplied by Professor Xue-tao Cao (Second Military Medical University, China). Mice were bred and maintained in specific pathogen-free facilities. For experimental purposes, mice were used at 6–8 weeks of age.
Peripheral blood samples were obtained from HLA-A*02+ healthy donors. The sample collection was approved by the ethics committee of Zhengzhou University.
Peptide prediction and synthesis
The prediction of HLA-A*0201 epitopes in PLAC1 protein (NCBI NP_068568.1) was carried out using computer-based T cell epitope prediction programs including BIMAS (http://bimas.dcrt.nih.gov/molbio/hla_bind), SYFPEITHI (http://www.syfpeithi.de/Scripts/MHC Server.dll/EpitopePrediction.htm) and NetCTL 1.2 (http://www.cbs.dtu.dk/services/NetCTL) (Wang et al. 2009; Mommaas et al. 2002; Kesmir et al. 2002). Native peptides with prediction scores among the top ten by all the three programs were selected, their solubility was also considered. The analogues were designed by altering the native peptides with tyrosine at position 1 (1Y), leucine at position 2 (2L) or position 9 (9 V) according to the literature mentioned above. Peptides were synthesized by standard solid phase Fmoc strategy and were purified to more than 95% purity by reverse phase high performance liquid chromatography (RP-HPLC). Their molecular weights were confirmed by electrospray ionization mass spectrometry (ESI–MS). COX-2321 (p321, ILIGETIKI) were used as a positive control in HLA-A*0201 binding assay (Gao et al. 2009). Peptides were dissolved in DMSO at a concentration of 10 mM, and stored at −20°C.
T2 binding assay
To determine the binding properties of the candidate peptides toward HLA-A*0201 molecule, up-regulation of peptide-induced HLA-A*0201 molecules on T2 cells was examined according to the protocol described previously. Briefly, T2 cells (1 × 106 cells/mL) were incubated with peptide (50 μM) in serum-free RPMI 1640 medium supplemented with 3 μg/mL human β2-microglobulin (β2-M, Merck, Germany) at 37°C for 18 h. Cells were then washed twice and incubated with the anti-HLA-A2 mAb, BB7.2 (Santa Cruz, US), followed by treatment with FITC-labeled goat IgG anti-mouse immunoglobulin (Tang et al. 2007; Li et al. 2009). Cells were harvested and analyzed by flow cytometry (FACSCalibur, Becton–Dickinson, US). The fluorescence index (FI) was calculated as follows: FI = (mean FITC fluorescence with the given peptide − mean FITC fluorescence without peptide)/(mean FITC fluorescence without peptide).
Measurement of the peptide/HLA-A*0201 complex stability
T2 cells (1 × 106 cells/mL) were incubated with peptide (100 μM) and β2-M (100 ng/mL) for 18 h at 37°C in serum-free RPMI 1640 medium. Cells were washed twice to remove free peptides, then incubated with brefeldin A (10 μg/mL, Sigma, US) for 1 h, washed, and incubated at 37°C for 0, 2, 4, and 6 h. Cells were then washed twice, stained and analyzed by flow cytometry (Han et al. 2006; He et al. 2008). The dissociation complex 50 (DC50) was defined as the time required for the loss of 50% of the stabilized peptide/HLA-A*0201 complexes at time 0 h.
Analysis of PLAC1 expression by RT-PCR
RT-PCR was used to analyze the expression of PLAC1 mRNA in three breast cancer cell lines involving MCF-7 (Wang et al. 2002). Briefly, total RNA was extracted and reverse-transcribed with Avian myoblastosis virus (AMV) reverse transcriptase and oligo dT (Clontech, US). Quality of the cDNA was confirmed by polymerase chain reaction (PCR) of GAPDH. Gene-specific PCR primers used to amplify PLAC1 and GAPDH were designed (PLAC1 sense: 5′-CTG GAC GGC TTC CTG TTT-3′, antisense: 5′-CAC CTC GTA GCA TTT CTC ATC-3′, size: 496 bp; GAPDH sense: 5′-GAA GGT GAA GGT CGG AGT C-3′, antisense: 5′-GAA GAT GGT GAT GGG ATT TC-3′, size: 226 bp). PCR was performed with the Taq polymerase (Clontech, US) for 30 cycles in an Eppendorf GA PCR system (Germany) at an annealing temperature of 72°C. Products were analyzed on 1% agarose gel containing 0.01 mg/mL ethidium bromide.
Generation of CTLs from PBMCs of healthy donors
CTLs induction in vitro was performed in accordance with the procedures previously described. Briefly, PBMCs of the HLA-A*02+ healthy donor were obtained with centrifugation at a Ficoll–Paque density gradient and then cultured in RPMI 1640 supplemented with 10% FCS, 100 units/mL penicillin, and 100 units/mL streptomycin (Han et al. 2006). Then these cells were stimulated once a week with the synthetic peptides and the β2-M at the final concentration of 10 μg/mL. Human recombinant IL-2 was added to the culture medium at a concentration of 50 units/mL on day 3 and the day after each stimulation. The enzyme linked immunospot (ELISPOT) assay and cytotoxic assay were performed on day 21.
IFN-γ release enzyme-linked immunospot (ELISPOT) assay
ELISPOT assay was performed using a commercial kit (Dakewe, China). T2 cells, pulsed with the indicated concentration of synthetic peptides, were used as stimulator cells. Effector cells (1 × 105) and Peptide-pulsed T2 cells (1 × 105) were seeded into 96-well microplates coated with antibody specific for human IFN-γ (Lv et al. 2010; Bernhard et al. 1988). After incubation at 37°C for 16 h, cells were removed and plates were processed. The number of spots was determined automatically by using a computer-assisted spot analyzer (Dakewe, China).
Generation of CTLs from HLA-A2.1/Kb transgenic mice
HLA-A2.1/Kb transgenic mice were immunized with 100 μg of various peptides and 140 μg of the IAb-restricted HBVcore antigen-derived T helper epitope (sequence 128–140: TPPAYRPPNAPIL) prepared in incomplete Freund’s adjuvant (IFA) on days 0, 5 and 10 (Eguchi et al. 2006; Tourdot et al. 2000). Group of mice received IFA containing PBS or T-helper peptide was used as negative control. After 11 days, spleen lymphocytes (5 × 107 cells in 10 mL) were stimulated in vitro with peptide (10 μM). At day 6 of culture, cytotoxic activity was tested based on the measurement of LDH release using the non-radioactive cytotoxicity assay kit (Promega, US) at E:T ratios, 20:1, 40:1 and 80:1.
Cytotoxicity assay
Cytotoxic activity was tested based on the measurement of lactate dehydrogenase (LDH) release using the non-radioactive cytotoxicity assay kit (Promega, US) at various E:T ratios (10:1, 20:1 and 40:1, CTLs from the PBMCs of healthy donors; 20:1, 40:1 and 80:1, CTLs from the spleen lymphocytes of transgenic mice) (Ding et al. 2009). For CTLs generated form PBMCs of healthy donors, target cells were T2 cells loaded with or without selected peptides and tumor cells MCF-7. For CTLs generated form HLA-A2.1/Kb transgenic mice, tumor cells MCF-7 were served as target cells. Target cells (1 × 104/well) were co-cultured with various number of effector cells at 37°C for 5 h. The percentage of specific lysis of the target cells was determined as: percentage of specific lysis = [(experimental release − effector spontaneous release − target spontaneous release)/(target maximum release − target spontaneous release)] × 100. For inhibition of CTL activity, 10 μg/mL of anti-HLA-A2 monoclonal antibody (BB7.2) was used as reported previously (Han et al. 2006; Gomi et al. 1999).
Results
Selection of potential HLA-A*0201 epitopes in PLAC1
Based on the three prediction programs, SYFPEITHI, BIMAS and NetCTL, five native peptides (p8, p11, p28, p31, and p42) scored among the top 10 by all the programs were preliminarily selected. Because of the poor solubility of p8 and p42, only three native peptides (p11, p28, and p31) and their analogues (p11-1Y9 V, p28-1Y9 V, and p31-1Y2L) were selected and synthesized with a purity of over 95% (Table 1). The molecular weights of all the peptides were confirmed by ESI–MS (Table 2).
Binding affinity of candidate peptides to HLA-A*0201
To evaluate the binding affinity of these peptides to HLA-A*0201 molecule in vitro, a binding assay in T2 cells was used. As shown in Table 2, all of the peptides synthesized could bind to HLA-A*0201 molecules with different affinities. Among the six candidate peptides (Table 2), the native peptides p28 and p31 and their analogues p28-1Y9 V and p31-1Y2L, showed potent binding affinity to HLA-A*0201 (FI values were 0.75, 0.89, 1.01 and 1.05, respectively). The binding affinities of other peptides were not very high (FI < 0.5). Each analogue showed stronger affinity than the relative native peptide. By comparison with the p11 peptide and its analogue, p28 and p31 and their analogues were selected for the further assay.
Measurement of the peptide/HLA-A*0201 complex stability
The peptides which showed potent binding affinity to HLA-A*0201 were tested for the peptide/HLA-A*0201 complex stability. T2 cells were used to evaluate the stability of the peptide/HLA-A*0201 complexes in vitro. The binding stability of these peptides was shown as DC50. The DC50 of the four peptides was longer than 2 h (Table 2). The DC50 of p28-1Y9 V/HLA-A*0201 and p31-1Y2L/HLA-A*0201 complexes was longer than 4 h. In concordance with the binding affinities, the analogues showed more potent binding stabilities than their native peptides.
Expression of PLAC1 in tumor cell lines
The expression of PLAC1 mRNA in three breast cancer cell lines was analyzed by RT-PCR. Expression of positive control GAPDH (226 bp) gene was observed in all the three cell lines (Fig. 1), suggesting that mRNA isolation and RT-PCR were all successful. PLAC1 gene was also expressed in all the three cell lines involving MCF-7 cells (HLA-A*0201+).
IFN-γ release ELISPOT assay
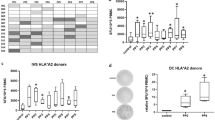
Based on the result of the T2 binding assay and peptide/HLA-A*0201 stability assay, p28, p28-1Y9 V, p31 and p31-1Y2L were selected to investigate their ability to induce T cell response. IFN-γ release ELISPOT assay were employed to test their ability to induced CTL response in vitro. The CTLs were induced from the PBMCs of the HLA-A*02+ healthy donors. The data showed that the CTLs induced by all the four peptides could produce IFN-γ, while p28, p31, and p31-1Y2L showed more potent activity which could induce more amounts of IFN-γ in at least two of three donors (Fig. 2).
ELISPOT assay to measure IFN-γ release by CTLs induced from PBMCs of healthy donors. PBMCs from healthy donors were separated routinely and stimulated with synthetic peptides and IL-2 in RPMI 1640 supplemented with 10% FCS for 21 days. Then, these PBMCs were collected and ELISPOT assay was performed to determine the IFN-γ production by these cells. PBMCs induced by PBS were used as negative control
In vitro cytotoxic activity of peptide-specific CTLs
To investigate whether IFN-γ-producing CTLs could lyse target cells, a LDH cytotoxicity assay was performed. PBMCs from healthy donor 1 were stimulated with synthetic peptides according to previously described method for CTLs induction. MCF-7 cells (HLA-A*0201+, PLAC1+) were used as target cells. All of the four peptides tested were able to elicit PLAC1-specific CTLs which could lyse MCF-7 cells at E: T ratio of 40:1 (Fig. 3a, b). As a control, the PBMCs could not lyse MCF-7 without peptides pulsed. We further examined the cytolytic activity of p28-specific CTLs (Fig. 4). The p28-specific CTLs could lyse MCF-7 cells and T2 cells loaded with peptide p28, but could not lyse T2 cells without peptide-loaded. After incubating with anti-HLA-A2 monoclonal antibody, p28-specific CTLs could not lyse MCF-7 cells even at higher E: T ratio. Our results indicating that p28 could be naturally processed and presented to the tumor cell surface in association with the HLA-A*0201.
Specific lysis of MCF-7 cell lines by the CTLs generated from PBMCs of healthy donor 1. CTLs were induced by PLAC1-derived peptides and their analogues, respectively. a p28 and p28-1Y9 V, b p31 and p31-1Y2L. The effector/target (E:T) ratios were 10:1, 20:1 and 40:1. Levels of LDH release were detected. CTLs induced by PBS were used as negative control
Specific lysis of various cell lines by the CTLs induced by p28. T2 cells loaded with or without p28, and tumor cells MCF-7 incubated with or without Anti-HLA-A2 antibody served as target cells. The cytotoxic activity of the p28 induced CTLs was determined against these cells at various E:T ratios by LDH assay
In vivo induction of peptide-specific CTLs in HLA-A2.1/Kb transgenic mice
After showing that all the four peptides could elicit CTLs in vitro, we addressed the question whether the peptide could be naturally processed and presented, and then induce peptide-specific CTLs in vivo. HLA-A2.1/Kb transgenic mice were immunized with peptides emulsified in IFA in the presence of HBVcore128 T helper epitope. Spleen lymphocytes were pooled and re-stimulated in vitro with peptides, respectively. Then the CTLs were tested for their ability of cytotoxic activity. MCF-7 cells (HLA-A*0201+, PLAC1+) were used as target cells. Our result showed that 29.6%, 39.8%, and 29.4% of MCF-7 cells were lysed by p28-induced CTLs at E:T ratio of 20:1, 40:1 and 80:1, respectively (Fig. 5a). The other peptides did not show very potent cytotoxic activities (Fig. 5a, b). These results suggested that peptide p28 could be naturally processed and presented, and induce potent peptide-specific CTL response in vivo.
Specific lysis of MCF-7 by the CTLs generated from immunized HLA-A2.1/Kb transgenic mice (n = 4). HLA-A2.1/Kb mice were immunized with 100 μg of various peptides and 140 μg of the IAb-restricted HBVcore antigen-derived T helper epitope (sequence 128–140: TPPAYRPPNAPIL) prepared in IFA on days 0, 5 and 10. Eleven days after the first immunization, the animals were sacrificed, and spleen lymphocytes were re-stimulated in vitro with the same peptide for an additional 6 days. The effector/target (E:T) ratios were 20:1, 40:1 and 80:1. a p28 and p28-1Y9 V, b p31 and p31-1Y2L. Group of mice received IFA containing PBS or T-helper peptide was used as negative control
Discussion
Over the past few years, the analysis of spontaneous immune responses to autologous tumors in patients has allowed the identification of several kinds of tumor-associated antigens that can be the targets for tumor specific immune responses based on the recognition of tumor antigen by CTLs in an MHC-class I/peptide complex-restricted manner (Coulie et al. 1994; Cheever et al. 1995). Therefore, cancer-specific immunotherapy has become an attractive fourth-therapeutic approach against carcinomas. Cancer-testis (CT) genes, normally expressed in germ line cells but also activated in a wide range of cancer types, often encode antigens that are immunogenic in cancer patients and present potential for use as biomarkers and targets for immunotherapy. Thus, the identification of T cell epitopes from these antigens becomes a critical step in the development of peptide-based immunotherapy for cancer.
The trophoblast-specific gene PLAC1 (placenta-specific 1) is a newly considered CT genes, a human X-linked gene with placenta-specific expression, ectopically expressed in a wide range of human malignancies, most frequently in breast cancer, and is essentially involved in cancer cell proliferation, migration and invasion (Cocchia et al. 2000). PLAC1 was localized to the plasma membrane of the breast cancer cell line, MCF-7 (Koslowski et al. 2007). PLAC1 expression has been demonstrated in a variety of human cancers. PLAC1 was identified highly expressed in hepatocellular carcinoma (HCC) tissues but not in corresponding non-cancerous tissues. Among HCC samples tested, 32% (22/69) showed PLAC1 mRNA expression while the protein was detected in 23.3% (7/30). A serological survey revealed that 3.8% (4/101) of HCC patients had anti- PLAC1 antibody response, suggesting the immunogenicity of PLAC1 in HCC patients (Dong et al. 2008). PLAC1 also could be potential targets for immunotherapy in colorectal cancer and epithelial ovarian cancer (Liu et al. 2008; Tchabo et al. 2009). Although functional insight into PLAC1 in the normal trophoblast is lacking, preliminary studies suggest that cancer-derived PLAC1 has the potential to promote tumor growth. In addition, it also appears to elicit a specific immunologic response that may influence survival in some cancer patients, suggesting that it may provide a therapeutic target for the treatment of some cancers (Fant et al. 2010). If CTL epitopes derived from PLAC1 were identified, they will be useful for the peptide-based immunotherapy of tumors that express PLAC1.
In this study, we identified PLAC1 derived epitope based on the widely used epitope prediction programs, the candidate native peptides and their analogues modified with P1 (Y), P2 (L) or P9 (V) were selected and synthesized. Then, the Peptide-MHC affinity assay and peptide/HLA-A*0201 complex stability assay were performed to determine their capacity of binding affinity and stability to HLA-A*0201 molecule. Results showed that p28 and p31 and their analogues are the high-affinity peptide, with potent binding affinity and stability to HLA-A*0201 molecule. Subsequent IFN-γ release and LDH release assays by using PBMCs from HLA-A*02+ healthy donors showed that the native peptide p28 and p31 and their analogues could induce potent T cell response. The CTLs induced by p28 and p31 and their analogues could specifically lyse the MCF-7 (HLA-A*0201+, PLAC1+) cells. We further examined the cytolytic activity of p28-specific CTLs. The lack of reactivity against MCF-7 incubated with anti-HLA-A2 monoclonal antibody (HLA-A*0201 blocked, PLAC1+) and T2 cells without peptide loaded (HLA-A*0201+, PLAC1−) clearly demonstrate that the generated CTLs exhibited the cytotoxic reactivity against human breast cancer cells in a PLAC1 specific and HLA-A2-restricted manner. The peptide is further characterized by being immunogenic in vivo in HLA-A2.1/Kb transgenic mice. The results showed that the p28-induced CTLs in HLA-A2.1/Kb transgenic mice could lyse the MCF-7 cells which is in a PLAC1-specific and HLA-A*0201-restricted manner. p28 showed more potent cytotoxic activities than other candidate peptides especially at the lower E:T ratios which indicated that it was a very potent candidate peptide. The in vivo assay indicated that p28 could be naturally processed and presented which have good immunogenicity in vivo, too.
The most widely used method to increase both HLA-A2.1-binding affinity and stability of antigenic peptides is to introduce MHC-binding favorable amino acids in positions, P1, P2 and P9. However, even when peptide modifications are selected very cautiously, by maximally avoiding changes in antigenic structure, peptide analogs may also trigger T cells bearing TCRs, which are unable to recognize tumor cells (Dutoit et al. 2002; Stuge et al. 2004). Speiser and colleagues reported that vaccination with natural tumor/self antigen resulted in vigorous T cell responses easily detectable directly in peripheral blood of 6/6 melanoma patients. Detailed studies revealed that responding T cells expressed TCRs with high functional avidity for the natural antigen, conferring efficient tumor recognition. Tumor cell killing was further enhanced because of unexpected high levels of T cell activation, which was significantly superior compared with T cells from patients vaccinated with analog peptide (Speiser et al. 2008). In our results, the analogues showed more potent binding affinity and stability than their native peptides. However, the activities of the analogues of p28 and p31 were not more potent than the relative native peptides in cytotoxicity assays in vitro and in vivo. The reason might be that the substitutions changed the conformation of the native peptide which affected its recognition by the TCR. The results described here suggested that the binding properties of peptides to MHC molecules might be essential to their T cell response activities, but not all the peptides with good binding activities are immunodominant epitopes.
In conclusion, a novel HLA-A*0201-restricted T cell epitope, p28 (VLCSIDWFM), was identified from PLAC1. Our results indicated that p28 could serve as a good candidate to develop peptide vaccines against PLAC1-positive breast cancer. Further, the identified peptide sequences could be used in future epitope-specific vaccine strategies including peptide vaccine strategies, single chain trimer DNA vaccine strategies, and for developing immune-monitoring reagents.
References
Bernhard EJ, Le AX, Barbosa JA, Lacy E, Engelhard VH (1988) Cytotoxic T lymphocytes from HLA-A2 transgenic mice specific for HLA-A2 expressed on human cells. J Exp Med 168(3):1157–1162
Boon T, van der Bruggen P (1996) Human tumor antigens recognized by T lymphocytes. J Exp Med 183(3):725–729
Cheever MA, Disis ML, Bernhard H, Gralow JR, Hand SL, Huseby ES, Qin HL, Takahashi M, Chen W (1995) Immunity to oncogenic proteins. Immunol Rev 145:33–59
Cocchia M, Huber R, Pantano S, Chen EY, Ma P, Forabosco A, Ko MS, Schlessinger D (2000) PLAC1, an Xq26 gene with placenta-specific expression. Genomics 68(3):305–312
Coulie PG, Brichard V, Van Pel A, Wolfel T, Schneider J, Traversari C, Mattei S, De Plaen E, Lurquin C, Szikora JP, Renauld JC, Boon T (1994) A new gene coding for a differentiation antigen recognized by autologous cytolytic T lymphocytes on HLA-A2 melanomas. J Exp Med 180(1):35–42
Ding FX, Wang F, Lu YM, Li K, Wang KH, He XW, Sun SH (2009) Multiepitope peptide-loaded virus-like particles as a vaccine against hepatitis B virus-related hepatocellular carcinoma. Hepatology 49(5):1492–1502
Dong XY, Peng JR, Ye YJ, Chen HS, Zhang LJ, Pang XW, Li Y, Zhang Y, Wang S, Fant ME, Yin YH, Chen WF (2008) Plac1 is a tumor-specific antigen capable of eliciting spontaneous antibody responses in human cancer patients. Int J Cancer 122(9):2038–2043
Dutoit V, Rubio-Godoy V, Pittet MJ, Zippelius A, Dietrich PY, Legal FA, Guillaume P, Romero P, Cerottini JC, Houghten RA, Pinilla C, Valmori D (2002) Degeneracy of antigen recognition as the molecular basis for the high frequency of naive A2/Melan-a peptide multimer(+) CD8(+) T cells in humans. J Exp Med 196(2):207–216
Eguchi J, Hatano M, Nishimura F, Zhu X, Dusak JE, Sato H, Pollack IF, Storkus WJ, Okada H (2006) Identification of interleukin-13 receptor alpha2 peptide analogues capable of inducing improved antiglioma CTL responses. Cancer Res 66(11):5883–5891
Fant M, Weisoly DL, Cocchia M, Huber R, Khan S, Lunt T, Schlessinger D (2002) PLAC1, a trophoblast-specific gene, is expressed throughout pregnancy in the human placenta and modulated by keratinocyte growth factor. Mol Reprod Dev 63(4):430–436
Fant M, Farina A, Nagaraja R, Schlessinger D (2010) PLAC1 (Placenta-specific 1): a novel, X-linked gene with roles in reproductive and cancer biology. Prenat Diagn 30(6):497–502
Gao YF, Sun ZQ, Qi F, Qi YM, Zhai MX, Lou HP, Chen LX, Li YX, Wang XY (2009) Identification of a new broad-spectrum CD8 + T cell epitope from over-expressed antigen COX-2 in esophageal carcinoma. Cancer Lett 284(1):55–61
Gomi S, Nakao M, Niiya F, Imamura Y, Kawano K, Nishizaka S, Hayashi A, Sobao Y, Oizumi K, Itoh K (1999) A cyclophilin B gene encodes antigenic epitopes recognized by HLA-A24-restricted and tumor-specific CTLs. J Immunol 163(9):4994–5004
Han JF, Zhao TT, Liu HL, Lin ZH, Wang HM, Ruan ZH, Zou LY, Wu YZ (2006) Identification of a new HLA-A*0201-restricted cytotoxic T lymphocyte epitope from CML28. Cancer Immunol Immunother 55(12):1575–1583
He Y, Mao L, Lin Z, Deng Y, Tang Y, Jiang M, Li W, Jia Z, Wang J, Ni B, Wu Y (2008) Identification of a common HLA-A*0201-restricted epitope among SSX family members by mimicking altered peptide ligands strategy. Mol Immunol 45(9):2455–2464
Jager E, Chen YT, Drijfhout JW, Karbach J, Ringhoffer M, Jager D, Arand M, Wada H, Noguchi Y, Stockert E, Old LJ, Knuth A (1998) Simultaneous humoral and cellular immune response against cancer-testis antigen NY-ESO-1: definition of human histocompatibility leukocyte antigen (HLA)-A2-binding peptide epitopes. J Exp Med 187(2):265–270
Kesmir C, Nussbaum AK, Schild H, Detours V, Brunak S (2002) Prediction of proteasome cleavage motifs by neural networks. Protein Eng 15(4):287–296
Koslowski M, Sahin U, Mitnacht-Kraus R, Seitz G, Huber C, Tureci O (2007) A placenta-specific gene ectopically activated in many human cancers is essentially involved in malignant cell processes. Cancer Res 67(19):9528–9534
Lazoura E, Apostolopoulos V (2005) Rational Peptide-based vaccine design for cancer immunotherapeutic applications. Curr Med Chem 12(6):629–639
Li F, Yang D, Wang Y, Liu B, Deng Y, Wang L, Shang X, Tong W, Ni B, Wu Y (2009) Identification and modification of an HLA-A*0201-restricted cytotoxic T lymphocyte epitope from Ran antigen. Cancer Immunol Immunother 58(12):2039–2049
Liu FF, Dong XY, Pang XW, Xing Q, Wang HC, Zhang HG, Li Y, Yin YH, Fant M, Ye YJ, Shen DH, Zhang Y, Wang S, Chen WF (2008) The specific immune response to tumor antigen CP1 and its correlation with improved survival in colon cancer patients. Gastroenterology 134(4):998–1006
Lv H, Gao Y, Wu Y, Zhai M, Li L, Zhu Y, Liu W, Wu Z, Chen F, Qi Y (2010) Identification of a novel cytotoxic T lymphocyte epitope from CFP21, a secreted protein of Mycobacterium tuberculosis. Immunol Lett 133(2):94–98
Mommaas B, Kamp J, Drijfhout JW, Beekman N, Ossendorp F, Van Veelen P, Den Haan J, Goulmy E, Mutis T (2002) Identification of a novel HLA-B60-restricted T cell epitope of the minor histocompatibility antigen HA-1 locus. J Immunol 169(6):3131–3136
Roth C, Rochlitz C, Kourilsky P (1994) Immune response against tumors. Adv Immunol 57:281–351
Ruppert J, Sidney J, Celis E, Kubo RT, Grey HM, Sette A (1993) Prominent role of secondary anchor residues in peptide binding to HLA-A2.1 molecules. Cell 74(5):929–937
Sadanaga N, Nagashima H, Mashino K, Tahara K, Yamaguchi H, Ohta M, Fujie T, Tanaka F, Inoue H, Takesako K, Akiyoshi T, Mori M (2001) Dendritic cell vaccination with MAGE peptide is a novel therapeutic approach for gastrointestinal carcinomas. Clin Cancer Res 7(8):2277–2284
Salgaller ML, Weber JS, Koenig S, Yannelli JR, Rosenberg SA (1994) Generation of specific anti-melanoma reactivity by stimulation of human tumor-infiltrating lymphocytes with MAGE-1 synthetic peptide. Cancer Immunol Immunother 39(2):105–116
Speiser DE, Baumgaertner P, Voelter V, Devevre E, Barbey C, Rufer N, Romero P (2008) Unmodified self antigen triggers human CD8 T cells with stronger tumor reactivity than altered antigen. Proc Natl Acad Sci U S A 105(10):3849–3854
Stuge TB, Holmes SP, Saharan S, Tuettenberg A, Roederer M, Weber JS, Lee PP (2004) Diversity and recognition efficiency of T cell responses to cancer. PLoS Med 1(2):e28
Tang Y, Lin Z, Ni B, Wei J, Han J, Wang H, Wu Y (2007) An altered peptide ligand for naive cytotoxic T lymphocyte epitope of TRP-2(180–188) enhanced immunogenicity. Cancer Immunol Immunother 56(3):319–329
Tchabo NE, Mhawech-Fauceglia P, Caballero OL, Villella J, Beck AF, Miliotto AJ, Liao J, Andrews C, Lele S, Old LJ, Odunsi K (2009) Expression and serum immunoreactivity of developmentally restricted differentiation antigens in epithelial ovarian cancer. Cancer Immun 9:6
Tourdot S, Scardino A, Saloustrou E, Gross DA, Pascolo S, Cordopatis P, Lemonnier FA, Kosmatopoulos K (2000) A general strategy to enhance immunogenicity of low-affinity HLA-A2. 1-associated peptides: implication in the identification of cryptic tumor epitopes. Eur J Immunol 30(12):3411–3421
Vitiello A, Marchesini D, Furze J, Sherman LA, Chesnut RW (1991) Analysis of the HLA-restricted influenza-specific cytotoxic T lymphocyte response in transgenic mice carrying a chimeric human-mouse class I major histocompatibility complex. J Exp Med 173(4):1007–1015
Wang Y, Han KJ, Pang XW, Vaughan HA, Qu W, Dong XY, Peng JR, Zhao HT, Rui JA, Leng XS, Cebon J, Burgess AW, Chen WF (2002) Large scale identification of human hepatocellular carcinoma-associated antigens by autoantibodies. J Immunol 169(2):1102–1109
Wang B, Yao K, Liu G, Xie F, Zhou F, Chen Y (2009) Computational prediction and identification of Epstein-Barr virus latent membrane protein 2A antigen-specific CD8 + T-cell epitopes. Cell Mol Immunol 6(2):97–103
Acknowledgments
This work was supported by grants from the National Natural Science Foundation of China (Nos. 30901362, 30872381).
Conflicts of interests
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, W., Zhai, M., Wu, Z. et al. Identification of a novel HLA-A2-restricted cytotoxic T lymphocyte epitope from cancer-testis antigen PLAC1 in breast cancer. Amino Acids 42, 2257–2265 (2012). https://doi.org/10.1007/s00726-011-0966-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-011-0966-3