Abstract
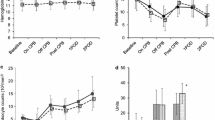
Surface-coated cardiopulmonary bypass (CPB) has been shown to have excellent biocompatibility during cardiac surgery in adults, but there have been only a few reports demonstrating the efficacy of this coating for congenital cardiac surgery. We tested the efficacy of poly-2-methoxyethylacrylate (PMEA) coating for CPB circuits in congenital cardiac surgery. Eleven operative cases of ventricular septal defect were studied: group C (control: no coating, n = 5) and group P (PMEA coating, n = 6). The platelet count and β-thromboglobulin (βTG), fibrinogen (FBG), thrombin-antithrombin complex (TAT), and neutrophil elastase levels were measured during the operation. Postoperative chest tube drainage was analyzed and the surface of the artificial lung was observed with an electron microscope. Elevation of TAT and neutrophil elastase was suppressed in group P (P < 0.05). Observation of the artificial lung surface using an electron microscope clearly revealed fewer blood cells were adherent to the surface in group P. The FBG level and postoperative bleeding were relatively lower in group P, but there were no significant differences between groups. The platelet count and βTG level were the same in both groups. We concluded that the PMEA-coated circuit reduces activation of the coagulation system and the inflammatory reaction in pediatric cardiac surgery.
Similar content being viewed by others
References
Asimakopoulos G, Smith PLC, Patnatunga CP, Taylor KM. Lung injury and acute respiratory distress syndrome after cardiopulmonary bypass. Ann Thorac Surg 1999;68:1107–1115
Paparella D, Yau TM, Young E. Cardiopulmonary bypass-induced inflammation: pathophysiology and treatment. An update. Eur J Cardiothorac Surg 2002;21:232–244
Tonz M, Mihaljevic T, von Segesser LK, Fehr J, Schmid ER, Turina MI. Acute lung injury during cardiopulmonary bypass. Chest 1995;108:1551–1556
Heter EJ, Lee KS, Manspeizer HE, Mongero L, Spanier TB, Caliste X, Esrig B, Smith C. Heparin-bonded cardiopulmonary bypass circuits reduce cognitive dysfunction. J Cardiothorac Vasc Anesth 2002;16:37–42
Pappalardo F, Valle PD, Crescenzi G, Corno C, Franco A, Torracca L, Alfieri O, Galli L, Zangrillo A, D’Angelo A. Phosphorycholine coating may limit thrombin formation during high-risk cardiac surgery: a randomized controlled trial. Ann Thorac Surg 2006;81:886–891
Rubens FD, Nathan H, Labow R, Williams KS, Wonzy D, Karsh J, Ruel M, Mesana T. Effects of methylprednisolone and biocompatible copolymer circuit on blood activation during cardiopulmonary bypass. Ann Thorac Surg 2005;79:655–665
Wimmer-Greinecker G, Matheis G, Matens S, Oremek G, Adbel-Rahman U, Moritz A. Synthetic protein-treated versus heparincoated cardiopulmonary bypass surfaces: similar clinical results and minor biochemical differences. Eur J Cardiothorac Surg 1999; 16:211–217
Boning A, Scheewe J, Ivers T, Friedrich C, Stieh J, Freitag S, Cremer JT. Phosphorylcholine or heparin coating for pediatric extracorporeal circulation causes similar biologic effects in neonates and infants. J Thorac Cardiovasc Surg 2004;127:1458–1465
Tanaka M, Motomura T, Kawada M, Anzai T, Kasori Y, Shiroya T, Shimura K, Onishi M, Mochizuki A. Blood compatible aspects of poly(2-methoxyethylacrylate) (PMEA)-relationship between protein adsorption and platelet adhesion on PMEA surface. Biomaterials 2000;21:1471–1481
Baykut D, Wehrle BJ, Weichelt K, Schwartz P, Zerkowski HR. New surface biopolymers for oxygenators: an in vitro hemocompatibility test of poly(2-methoxyethylacrylate). Eur J Med Res 2001;6:297–305
Saito N, Motoyama S, Sawamoto J. Effects of new polymer-coated extracorporeal circuits on biocompatibility during cardiopulmonary bypass. Artif Organs 2000;24:547–554
Suhara H, Sawa Y, Nishimura M, Oshiyama H, Yokoyama K, Saito N, Matsuda H. Efficacy of a new coating material, PMEA, for cardiopulmonary bypass circuits in a porcine model. Ann Thorac Surg 2001;71:1603–1608
Ninomiya M, Miyaji K, Takamoto S. Influence of PMEA-coated bypass circuits on perioperative inflammatory response. Ann Thorac Surg 2003;75:913–917, discussion 7-8
Gunaydin S, Farsak B, Kocakulak M, Sari T, Yorgancioglu C, Zorlutuna Y. Clinical performance and biocompatibility of poly (2-methoxyethylacrylate)-coated extracorporeal circuits. Ann Thorac Surg 2002;74:819–824
Ikuta T, Fujii H, Shibata T, Hattori K, Hirai H, Kumano H, Suehiro S. A new poly-2-methoxyethylacrylate-coated cardiopulmonary bypass circuit possesses superior platelet preservation and inflammatory suppression efficacy. Ann Thorac Surg 2004;77:1678–1683
Eisses MJ, Geiduschek JM, Jonmarker C, Cohen GA, Chandler WL. Effect of polymer coating (poly-2-methoxyethylacrylate) of the oxygenator on hemostatic markers during cardiopulmonary bypass in children. J Cardiothorac Vasc Anesth 2007;21:28–34
Kirshbom PM, Miller BE, Spitzer K, Easley KA, Spainhour CE, Kogon BE, Kanter KR. Failure of surface-modified bypass circuits to improve platelet function during pediatric cardiac surgery J Thorac Cardiovasc Surg 2006;132:675–680
Yoshimura K, Nakagawa S, Koyama S, Kobayashi T, Homma T. Roles of neutrophil elastase and superoxide anion in leukotriene B4-induced lung injury in rabbit. J Appl Physiol 1994;76:91–96
Ilton MK, Langton PE, Taylor ML, Misso NLA, Newman M, Thompson PJ, Hung J. Differential expression of neutrophil adhesion molecules during coronary artery surgery with cardiopulmonary bypass. J Thorac Cardiovasc Surg 1999;118:930–937
Jordan JE, Zhao ZQ, Vinten-Johansen J. The role of neutrophils in myocardial ischemia-reperfusion injury. Cardiovasc Res 1999;43: 860–878
Grossi EA, Kallenbach K, Chau S, Derivaux CC, Aguinaga MG, Steinberg BM, Kim D, Iyer S, Tayyarah M, Artman M, Galloway AC, Colvin SB. Impact of heparin bonding on pediatric cardiopulmonary bypass: a prospective randomized study. Ann Thorac Surg 2000;70:191–196
Olsson C, Siegban A, Halden E, Nilsson B, Venge P, Thelin S. No benefit of reduced heparinization in thoracic aortic operation with heparin-coated bypass circuit. Ann Thorac Surg 2000;69:743–749
Gorman RC, Ziats NP, Rao AK, Gikakis N, Sun L, Khan MMH, Stenach N, Sapatnekar S, Chouhan V, Gorman III JH, Niewiarowski S, Colman RW, Anderson JM, Edmunds Jr LH. Surface-bound heparin fails to reduce thrombin formation during clinical cardiopulmonary bypass. J Thorac Cardiovasc Surg 1996; 111:1–12
Wakayama F, Fukuda I, Suzuki Y, Kondo N. Neutrophil elastase inhibitor, Sivelestat, attenuates acute lung injury after cardiopulmonary bypass in the rabbit endotoxemia model. Ann Thorac Surg 2007;83:153–160
Edmunds LH Jr, Colman RC. Thrombin during cardiopulmonary bypass. Ann Thorac Surg 2006;82:2315–2322
Aldea GS, Soltow LO, Chandler WL, Triggs CM, Vocelka CR, Crockett GI, Shin YT, Curits WE, Verrier ED. Limitation of thrombin generation, platelet activation, and inflammation by elimination of cardiotomy suction in patients undergoing coronary artery bypass grafting treated with heparin-bonded circuits. J Thorac Cardiovasc Surg 2002;123:742–755
De Somer F, Van Belleghem Y, Caes F, Francois K, Overbeke HV, Arnout J, Taeymans Y, Nooten GV. Tissue factor as the main activator of the coagulation system during cardiopulmonary bypass. J Thorac Cardiovasc Surg 2002;123:951–958
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Suzuki, Y., Daitoku, K., Minakawa, M. et al. Poly-2-methoxyethylacrylate-coated bypass circuits reduce activation of coagulation system and inflammatory response in congenital cardiac surgery. J Artif Organs 11, 111–116 (2008). https://doi.org/10.1007/s10047-008-0415-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-008-0415-6