Abstract
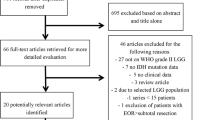
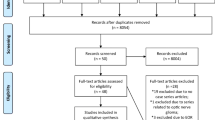
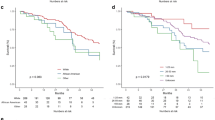
Multiple high-grade gliomas (M-HGGs) are well--separated tumors, differentiated as multifocal (MF) and multicentric (MC) by their MRI features. The authors performed a systematic review and meta-analysis of literature examining epidemiology, clinical and radiological characteristics, management, and the overall survival from M-HGGs. According to PRISMA guidelines, a comprehensive review of studies published between January 1990 and January 2017 was carried out. The authors identified studies that examined the prevalence rate, clinical and radiological characteristics, treatment, and overall survival from M-HGGs in patients with HGG. Data were analyzed using a random-effects meta-analysis model. Finally, we systematically reviewed demographic characteristics, lesion location, and surgical and adjuvant treatments. Twenty-three studies were included in this systematic review. The M-HGGs prevalence rate was 19% (95% CI 13–26%) and the hazard ratio of death from M-HGGs in the HGGs population was 1.71 (95% CI 1.49–1.95, p < 0.0001). The MC prevalence rate was 6% (CI 95% 4–10%), whereas MF prevalence rate was 11% (CI 95% 6–20%) (p < 0.0001). There were no statistically significant differences between MF and MC HGGs in gender, lesion location, histological type, and surgical treatment. Survival analysis of MC tumors showed that surgical resection (gross total resection or subtotal resection) is an independent predictor of improved outcome (HR 7.61 for biopsy subgroup, 95% CI 1.94–29.78, p = 0.004). The prevalence of M-HGGs is approximately 20% of HGGs. The clinical relevance of separating M-HGGs in MF and MC tumors remains questionable and its prognostic significance is unclear. When patient status and lesion characteristics make it safe and feasible, cytoreduction should be attempted in patients with M-HGGs because it improves overall survival.





Similar content being viewed by others
References
Akimoto J, Sasaki H, Haraoka R, Nakajima N, Fukami S, Kohno M (2014) A case of radiologically multicentric but genetically identical multiple glioblastomas. Brain Tumor Pathol 31:113–117. https://doi.org/10.1007/s10014-013-0157-x
Arcos A, Romero L, Serramito R, Santín JM, Prieto A, Gelabert M, Arráez MÁ, Ángel M (2012) Multicentric glioblastoma multiforme. Report of 3 cases, clinical and pathological study and literature review. Neurocirugia (Astur) 23:211–215. https://doi.org/10.1016/j.neucir.2012.06.004
Arvold ND, Tanguturi SK, Aizer AA, Wen PY, Reardon DA, Lee EQ, Nayak L, Christianson LW, Horvath MC, Dunn IF, Golby AJ, Johnson MD, Claus EB, Chiocca EA, Ligon KL, Alexander BM (2015) Hypofractionated versus standard radiation therapy with or without temozolomide for older glioblastoma patients. Int J Radiat Oncol Biol Phys 92:384–389. https://doi.org/10.1016/j.ijrobp.2015.01.017
Banan R, Hartmann C (2017) The new WHO 2016 classification of brain tumors—what neurosurgeons need to know. Acta Neurochir (Wien) 1–16. doi: https://doi.org/10.1007/s00701-016-3062-3
Batzdorf U, Malamud N (1963) The problem of multicentric gliomas. J Neurosurg 20:122–136. https://doi.org/10.3171/jns.1963.20.2.0122
Bloch O, Han SJ, Cha S, Sun MZ, Aghi MK, McDermott MW, Berger MS, Parsa AT (2012) Impact of extent of resection for recurrent glioblastoma on overall survival: clinical article. J Neurosurg 117:1032–1038. https://doi.org/10.3171/2012.9.JNS12504
Bradley W (1880) Case of gliosarcomatous tumors of the brain. Proc Conn Med Soc
Cuddapah VA, Robel S, Watkins S, Sontheimer H (2014) A neurocentric perspective on glioma invasion. Nat Publ Gr 15:455–465. https://doi.org/10.1038/nrn3765
Djalilian HR, Shah MV, Hall WA (1999) Radiographic incidence of multicentric malignant gliomas. Surg Neurol 51:554–558. https://doi.org/10.1016/S0090-3019(98)00054-8
Fares Y, Younes M, Kanj A, Ruiz Barnes P, Muñiz J (2009) Multicentric glioma. P R Health Sci J 28:75–79
Giese A, Bjerkvig R, Berens ME, Westphal M (2003) Cost of migration: invasion of malignant gliomas and implications for treatment. J Clin Oncol 21:1624–1636. https://doi.org/10.1200/JCO.2003.05.063
Globus J, Kuhlenbeck H (1944) The subependymal cell plate (matrix) and its relationship to brain tumors of the ependymal type. J. Neuropathol
Gulati S, Jakola AS, Nerland US, Weber C, Solheim O (2011) The risk of getting worse: surgically acquired deficits, perioperative complications, and functional outcomes after primary resection of glioblastoma. World Neurosurg 76:572–579. https://doi.org/10.1016/j.wneu.2011.06.014
Hartmann C, Hentschel B, Simon M, Westphal M, Schackert G, Tonn JC, Loeffler M, Reifenberger G, Pietsch T, Von Deimling A, Weller M (2013) Long-term survival in primary glioblastoma with versus without isocitrate dehydrogenase mutations. Clin Cancer Res 19:5146–5157. https://doi.org/10.1158/1078-0432.CCR-13-0017
Hassaneen W, Levine NB, Suki D, Salaskar AL, de Moura LA, McCutcheon IE, Prabhu SS, Lang FF, DeMonte F, Rao G, Weinberg JS, Wildrick DM, Aldape KD, Sawaya R (2011) Multiple craniotomies in the management of multifocal and multicentric glioblastoma. Clinical article. J Neurosurg 114:576–584. https://doi.org/10.3171/2010.6.JNS091326
Hefti M, Von Campe G, Schneider C, Roelcke U, Landolt H, Article O, Hefti M, Von Campe G, Schneider C, Roelcke U, Landolt H (2010) Multicentric tumor manifestations of high grade gliomas: Independent proliferation or hallmark of extensive disease? Zentralbl Neurochir 71:103. https://doi.org/10.1055/s-0029-1241190
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ Br Med J 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Karlowee V, Amatya VJ, Hirano H, Takayasu T, Nosaka R, Kolakshyapati M, Yoshihiro M, Takeshima Y, Sugiyama K, Arita K, Kurisu K, Yamasaki F (2016) Multicentric glioma develops via a mutant IDH1-independent pathway: immunohistochemical study of multicentric glioma. Pathobiology:4–8. https://doi.org/10.1159/000447951
Karnofsky DA, Abelmann WH, Craver LF, Burchenal JH (1948) The use of the nitrogen mustards in the palliative treatment of carcinoma. Cancer 1:634–656. https://doi.org/10.1002/1097-0142(194811)1:4<634::AID-CNCR2820010410>3.0.CO;2-L
Kato T, Aida T, Abe H, Ogata A, Nakamura N, Nagashima K, Kitaoka K (1990) Clinicopathological study of multiple gliomas—report of three cases. Neurol Med Chir (Tokyo) 30:604–609
Khan MB, Chakraborty S, Boockvar JA (2016) Gross total resection of glioblastoma improves overall survival and progression-free survival compared to subtotal resection or biopsy alone. Neurosurgery 79:N12–N13. https://doi.org/10.1227/01.neu.0000508600.08200.c1
Kong D-S, Kim J, Lee I-H, Kim ST, Seol HJ, Lee J-I, Park W-Y, Ryu G, Wang Z, Ma’ayan A, Nam D-H (2016) Integrative radiogenomic analysis for multicentric radiophenotype in glioblastoma. Oncotarget 7:11526–11538. 10.18632/oncotarget.7115
Kreth FW, Thon N, Simon M, Westphal M, Schackert G, Nikkhah G, Hentschel B, Reifenberger G, Pietsch T, Weller M, Tonn JC (2013) Gross total but not incomplete resection of glioblastoma prolongs survival in the era of radiochemotherapy. Ann Oncol 24:3117–3123. https://doi.org/10.1093/annonc/mdt388
Krex D, Mohr B, Appelt H, Schackert HK, Schackert G, Waziri AE, Bruce JN, Ph D, Schackert G, Al ET, Appelt H, Schackert HK, Schackert G, Waziri AE, Bruce JN (2003) Genetic analysis of a multifocal glioblastoma multiforme: a suitable tool to gain new aspects in glioma development. Neurosurgery 53:1377–1384. https://doi.org/10.1227/01.NEU.0000093426.29236.86
Kuhnt D, Becker A, Ganslandt O, Bauer M, Buchfelder M, Nimsky C (2011) Correlation of the extent of tumor volume resection and patient survival in surgery of glioblastoma multiforme with high-field intraoperative MRI guidance. Neuro-Oncology 13:1339–1348. https://doi.org/10.1093/neuonc/nor133
Kyritsis AP, Levin VA, Alfred Yung WK, Leeds NE (1993) Imaging patterns of multifocal gliomas. Eur J Radiol 16:163–170. https://doi.org/10.1016/0720-048X(93)90063-S
Lacroix M, Abi-Said D, Fourney DR, Gokaslan ZL, Shi W, DeMonte F, Lang FF, McCutcheon IE, Hassenbusch SJ, Holland E, Hess K, Michael C, Miller D, Sawaya R (2001) A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg 95:190–198. https://doi.org/10.3171/jns.2001.95.2.0190
Lasocki A, Gaillard F, Tacey MA, Drummond KJ, Stuckey SL (2016) The incidence and significance of multicentric noncontrast-enhancing lesions distant from a histologically-proven glioblastoma. J Neuro-Oncol 129:471–478. https://doi.org/10.1007/s11060-016-2193-y
Lasocki A, Gaillard F, Tacey M, Drummond K, Stuckey S (2016) Multifocal and multicentric glioblastoma: improved characterisation with FLAIR imaging and prognostic implications. J Clin Neurosci 31:92–98. https://doi.org/10.1016/j.jocn.2016.02.022
Laws ER, Parney IF, Huang W, Anderson F, Morris AM, Asher A, Lillehei KO, Bernstein M, Brem H, Sloan A, Berger MS, Chang S, Tumor B (2003) Survival following surgery and prognostic factors for recently diagnosed malignant glioma: data from the glioma outcomes project. J Neurosurg 99:467–473. https://doi.org/10.3171/jns.2003.99.3.0467
Lim DA, Cha S, Mayo MC, Chen M-HH, Keles E, Vanden Berg S, Berger MS (2007) Relationship of glioblastoma multiforme to neural stem cell regions predicts invasive and multifocal tumor phenotype. Neuro-Oncology 9:424–429. https://doi.org/10.1215/15228517-2007-023
Liu Q, Liu Y, Li W, Wang X, Sawaya R, Lang FF, Yung WKA, Chen K, Fuller GN, Zhang W (2015) Genetic, epigenetic, and molecular landscapes of multifocal and multicentric glioblastoma. Acta Neuropathol 130:587–597. https://doi.org/10.1007/s00401-015-1470-8
Moher D, Liberati A, Tetzlaff J, Altman DG, Grp P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement (reprinted from annals of internal medicine). Phys Ther 89:873–880. https://doi.org/10.1371/journal.pmed.1000097
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET, Carbone PP (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Orringer D, Lau D, Khatri S, Zamora-Berridi GJ, Zhang K, Wu C, Chaudhary N, Sagher O (2012) Extent of resection in patients with glioblastoma: limiting factors, perception of resectability, and effect on survival. J Neurosurg 117:851–859. https://doi.org/10.3171/2012.8.JNS12234
Parsa AT, Wachhorst S, Lamborn KR, Prados MD, McDermott MW, Berger MS, Chang SM, Francisco S (2005) Prognostic significance of intracranial dissemination of glioblastoma multiforme in adults. J Neurosurg 102:622–628. https://doi.org/10.3171/jns.2005.102.4.0622
Patil CG, Eboli P, Hu J (2012) Management of multifocal and multicentric gliomas. Neurosurg Clin N Am 23:343–350. https://doi.org/10.1016/j.nec.2012.01.012
Patil CG, Yi A, Elramsisy A, Hu J, Mukherjee D, Irvin DK, Yu JS, Bannykh SI, Black KL, Nuño M, Angeles L (2012) Prognosis of patients with multifocal glioblastoma: a case-control study. J Neurosurg 117:705–711. https://doi.org/10.3171/2012.7.JNS12147
Paulsson AK, Holmes JA, Peiffer AM, Miller LD, Liu W, Xu J, Hinson WH, Lesser GJ, Laxton AW, Tatter SB, Debinski W, Chan MD (2014) Comparison of clinical outcomes and genomic characteristics of single focus and multifocal glioblastoma. J Neuro-Oncol 119:429–435. https://doi.org/10.1007/s11060-014-1515-1
R. Stupp, W. P. Mason MJ van den B et al. (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma, N Engl J Med vol 352, no 10 987–996.
Russel D, Rubinstein S (1989) Pathol Tumours Nerv Syst 702:145–147. https://doi.org/10.1136/pgmj.35.410.702
di Russo P, Perrini P, Pasqualetti F, Meola A, Vannozzi R (2013) Management and outcome of high-grade multicentric gliomas: a contemporary single-institution series and review of the literature. Acta Neurochir 155:2245–2251. https://doi.org/10.1007/s00701-013-1892-9
Salvati M, Caroli E, Orlando ER, Frati A, Artizzu S, Ferrante L (2003) Multicentric glioma: our experience in 25 patients and critical review of the literature. Neurosurg Rev 26:275–279. https://doi.org/10.1007/s10143-003-0276-7
Sanai N, Berger MS (2008) Glioma extent of resection and its impact on patient outcome. Neurosurgery 62:753–764. https://doi.org/10.1227/01.neu.0000318159.21731.cf
Scott JG, Suh JH, Elson P, Barnett GH, Vogelbaum MA, Peereboom DM, Stevens GHJ, Elinzano H, Chao ST (2011) Aggressive treatment is appropriate for glioblastoma multiforme patients 70 years old or older: a retrospective review of 206 cases. Neuro-Oncology 13:428–436. https://doi.org/10.1093/neuonc/nor005
Selbekk T, Jakola AS, Solheim O, Johansen TF, Lindseth F, Reinertsen I, Unsgård G (2013) Ultrasound imaging in neurosurgery: approaches to minimize surgically induced image artefacts for improved resection control. Acta Neurochir 155:973–980. https://doi.org/10.1007/s00701-013-1647-7
Showalter TN, Andrel J, Andrews DW, Curran WJ, Daskalakis C, Werner-Wasik M (2007) Multifocal glioblastoma multiforme: prognostic factors and patterns of progression. Int J Radiat Oncol Biol Phys 69:820–824. https://doi.org/10.1016/j.ijrobp.2007.03.045
Stark AM, Van De Bergh J, Hedderich J, Mehdorn HM, Nabavi A (2012) Glioblastoma: clinical characteristics, prognostic factors and survival in 492 patients. Clin Neurol Neurosurg 114:840–845. https://doi.org/10.1016/j.clineuro.2012.01.026
Tanaka S, Meyer FB, Buckner JC, Uhm JH, Yan ES, Parney IF, Clinic M (2013) Presentation, management, and outcome of newly diagnosed glioblastoma in elderly patients. J Neurosurg 118:786–798. https://doi.org/10.3171/2012.10.JNS112268
Taylor MD, Bernstein M (1999) Awake craniotomy with brain mapping as the routine surgical approach to treating patients with supratentorial intraaxial tumors: a prospective trial of 200 cases. J Neurosurg 90:35–41. https://doi.org/10.3171/jns.1999.90.1.0035
Thomas RP, Xu LW, Lober RM, Li G, Nagpal S (2013) The incidence and significance of multiple lesions in glioblastoma. J Neuro-Oncol 112:91–97. https://doi.org/10.1007/s11060-012-1030-1
Verger E, Salamero M, Conill C (1992) Can Karnofsky performance status be transformed to the eastern cooperative oncology group scoring scale and vice versa? Eur J Cancer 28:1328–1330. https://doi.org/10.1016/0959-8049(92)90510-9
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2013) The Newcastle-Ottawa scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses. Ottawa Hosp Res Inst 1–4. doi: https://doi.org/10.2307/632432
Wen PY, Macdonald DR, Reardon DA, Cloughesy TF, Sorensen AG, Galanis E, DeGroot J, Wick W, Gilbert MR, Lassman AB, Tsien C, Mikkelsen T, Wong ET, Chamberlain MC, Stupp R, Lamborn KR, Vogelbaum MA, Van Den Bent MJ, Chang SM (2010) Updated response assessment criteria for high-grade gliomas: Response assessment in neuro-oncology working group. J Clin Oncol 28:1963–1972. https://doi.org/10.1200/JCO.2009.26.3541
Acknowledgements
We thank Ms. Juliet Strachan and Ms. Anne-Marie Peduto for English revision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure of potential conflicts of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Ethical approval
For this type of study, formal consent is not required.
Informed consent
The nature of this article did not require informed consent.
Electronic supplementary material
Online Resource 1
Literature search syntax (PDF 100 kb)
Online Resource 2
Discrepancies between authors in systematic review process (PDF 342 kb)
Online Resource 3
Discrepancies between authors in quality score assignment (PDF 328 kb)
Online Resource 5
Multifocal versus multicentric tumors: demographics data and lesion location (PDF 114 kb)
Online Resource 6
Comparison of surgical treatment rates in M-HGGs population (PDF 331 kb)
Online Resource 7
Surgical and adjuvant treatments of multifocal and multicentric HGGs (PDF 109 kb)
Rights and permissions
About this article
Cite this article
Di Carlo, D.T., Cagnazzo, F., Benedetto, N. et al. Multiple high-grade gliomas: epidemiology, management, and outcome. A systematic review and meta-analysis. Neurosurg Rev 42, 263–275 (2019). https://doi.org/10.1007/s10143-017-0928-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-017-0928-7