Abstract
Background
Various systemic inflammatory and nutritional scores have been reported to predict postoperative outcomes. This study aimed to investigate the best systemic inflammatory and nutritional scores in colorectal cancer (CRC) patients who underwent potentially curative resection.
Method
We evaluated 468 consecutive CRC patients in this study. Comparisons of systemic inflammatory and nutritional scores, including the neutrophil to lymphocyte ratio (NLR), platelet to lymphocyte ratio (PLR), prognostic index (PI), prognostic nutritional index (PNI), and modified Glasgow prognostic score (mGPS), were performed using univariate/multivariate analyses for patient survival.
Results
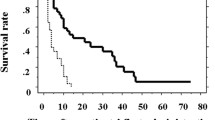
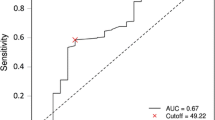
The PNI and mGPS, but not the NLR, PLR, and PI, were significantly associated with overall and relapse-free survival. The mGPS, but not the PNI, was strongly correlated with TNM stage (P < 0.001). Cox multivariate analysis showed that both the PNI and mGPS were exclusive independent prognostic factors for both overall and relapse-free survival (P < 0.001). Furthermore, the PNI status predicted patient survival more clearly than the mGPS in combination with TNM stage.
Conclusions
This study suggests that the PNI and mGPS are useful predictive scores in CRC patients who undergo potentially curative resection, especially the PNI in combination with TNM stage. Routine evaluation of the host status using the scores may be useful in CRC treatment.


Similar content being viewed by others
Abbreviations
- CRC:
-
Colorectal cancer
- mGPS:
-
Modified Glasgow prognostic score
- CRP:
-
C-reactive protein
- NLR:
-
Neutrophil to lymphocyte ratio
- PLR:
-
Platelet to lymphocyte ratio
- PI:
-
Prognostic index
- PNI:
-
Prognostic nutritional index
- BMI:
-
Body mass index
- CEA:
-
Carcinoembryonic antigen
- HR:
-
Hazard ratio
- CI:
-
Confidence interval
- OS:
-
Overall survival
- DFS:
-
Disease-free survival
References
Oshima H, Nakayama M, Han TS et al (2015) Suppressing TGFbeta signaling in regenerating epithelia in an inflammatory microenvironment is sufficient to cause invasive intestinal cancer. Cancer Res 75:766–776
Bozzetti F (2002) Rationale and indications for preoperative feeding of malnourished surgical cancer patients. Nutrition 18:953–959
Meguid MM, Mughal MM, Debonis D et al (1986) Influence of nutritional status on the resumption of adequate food intake in patients recovering from colorectal cancer operations. Surg Clin North Am 66:1167–1176
Onodera T, Goseki N, Kosaki G (2014) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai Zasshi 10:1–7
Onodera T, Goseki N, Kosaki G (1984) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai Zasshi 85:1001–1005
Gomes de Lima KV, Maio R (2012) Nutritional status, systemic inflammation and prognosis of patients with gastrointestinal cancer. Nutr Hosp 27:707–714
Park JH, Watt DG, Roxburgh CS et al. (2015) colorectal cancer, systemic inflammation, and outcome: staging the tumor and staging the host. Ann Surg. 236(2): 326−36
The Japanese society for cancer of the colon and rectum (2005) JSCCR guidelines 2005 for the treatment of colorectal cancer. Kanehara and Co., Ltd, Tokyo
The Japanese society for cancer of the colon and rectum (2010) JSCCR Guidelines 2010 for the treatment of colorectal cancer. Kanehara and Co., Ltd, Tokyo
Watanabe T, Itabashi M, Shimada Y et al (2012) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol 17:1–29
Sobin LHGMWC (2009) TNM classification of malignant tumours, 7th edn. Wiley-Blackwell, New York
Mallappa S, Sinha A, Gupta S et al (2013) Preoperative neutrophil to lymphocyte ratio >5 is a prognostic factor for recurrent colorectal cancer. Colorectal Dis 15:323–328
Smith RA, Bosonnet L, Raraty M et al (2009) Preoperative platelet-lymphocyte ratio is an independent significant prognostic marker in resected pancreatic ductal adenocarcinoma. Am J Surg 197:466–472
Proctor MJ, Morrison DS, Talwar D et al (2011) A comparison of inflammation-based prognostic scores in patients with cancer. A Glasgow Inflammation Outcome Study. Eur J Cancer 47:2633–2641
Mohri Y, Inoue Y, Tanaka K et al (2013) Prognostic nutritional index predicts postoperative outcome in colorectal cancer. World J Surg 37:2688–2692
Tarantino I, Warschkow R, Worni M et al (2012) Elevated preoperative CEA is associated with worse survival in stage I-III rectal cancer patients. Br J Cancer 107:266–274
Stiksma J, Grootendorst DC, van der Linden PW (2014) CA 19-9 as a marker in addition to CEA to monitor colorectal cancer. Clin Colorectal Cancer 13:239–244
Mantovani A, Allavena P, Sica A et al (2008) Cancer-related inflammation. Nature 454:436–444
Heys SD, Walker LG, Deehan DJ et al (1998) Serum albumin: a prognostic indicator in patients with colorectal cancer. J R Coll Surg Edinb 43:163–168
Kinoshita A, Onoda H, Imai N et al (2012) Comparison of the prognostic value of inflammation-based prognostic scores in patients with hepatocellular carcinoma. Br J Cancer 107:988–993
Guthrie GJ, Roxburgh CS, Farhan-Alanie OM et al (2013) Comparison of the prognostic value of longitudinal measurements of systemic inflammation in patients undergoing curative resection of colorectal cancer. Br J Cancer 109:24–28
Cedres S, Torrejon D, Martinez A et al (2012) Neutrophil to lymphocyte ratio (NLR) as an indicator of poor prognosis in stage IV non-small cell lung cancer. Clin Transl Oncol 14:864–869
Jin H, Zhang G, Liu X et al (2013) Blood neutrophil-lymphocyte ratio predicts survival for stages III-IV gastric cancer treated with neoadjuvant chemotherapy. World J Surg Oncol 11:112
Lee S, Oh SY, Kim SH et al (2013) Prognostic significance of neutrophil lymphocyte ratio and platelet lymphocyte ratio in advanced gastric cancer patients treated with FOLFOX chemotherapy. BMC Cancer 13:350
Yao Y, Yuan D, Liu H et al (2013) Pretreatment neutrophil to lymphocyte ratio is associated with response to therapy and prognosis of advanced non-small cell lung cancer patients treated with first-line platinum-based chemotherapy. Cancer Immunol Immunother 62:471–479
Tokunaga R, Sakamoto Y, Nakagawa S et al (2015) Prognostic nutritional index predicts severe complications, recurrence, and poor prognosis in patients with colorectal cancer undergoing primary tumor resection. Dis Colon Rectum 58:1048–1057
Dutta S, Crumley AB, Fullarton GM et al (2012) Comparison of the prognostic value of tumour and patient related factors in patients undergoing potentially curative resection of gastric cancer. Am J Surg 204:294–299
Miyamoto Y, Baba Y, Sakamoto Y et al (2015) Sarcopenia is a negative prognostic factor after curative resection of colorectal cancer. Ann Surg Oncol 22:2663–2668
Moon HG, Ju YT, Jeong CY et al (2008) Visceral obesity may affect oncologic outcome in patients with colorectal cancer. Ann Surg Oncol 15:1918–1922
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Tokunaga, R., Sakamoto, Y., Nakagawa, S. et al. Comparison of systemic inflammatory and nutritional scores in colorectal cancer patients who underwent potentially curative resection . Int J Clin Oncol 22, 740–748 (2017). https://doi.org/10.1007/s10147-017-1102-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-017-1102-5