Abstract
Purpose
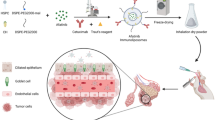
Despite an increasing interest in the use of inhalation for local delivery of molecules for respiratory diseases and systemic disorders, methods to deliver therapy through airways has received little attention for lung cancer treatment. However, inhalation of anticancer drugs is an attractive alternative route to systemic administration which results in limited concentration of the medication in the lungs, and triggers whole-body toxicity. In this study, we investigated the feasibility of nebulization for therapeutic antibodies, a new class of fully-approved anticancer drugs in oncology medicine.
Materials and methods
Cetuximab, a chimeric IgG1 targeting the epidermal growth factor receptor (EGFR), was nebulized using three types of delivery devices: a jet nebulizer PARI LC+®, a mesh nebulizer AeronebPro® and an ultrasonic nebulizer SYST’AM® LS290. Aerosol size distribution was measured using a cascade impactor and aerosol droplets were observed under optical microscopy. The immunological and pharmacological properties of cetuximab were evaluated following nebulization using A431 cells.
Results
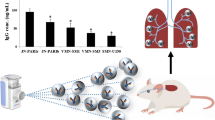
The aerosol particle clouds generated with the three nebulizers displayed similar aerodynamical characteristics, but the IgG formed aggregates in liquid phase following nebulization with both the jet and ultrasonic devices. Flow cytometry analyses and assays of EGFR-phosphorylation and cell growth inhibitions on A431 demonstrated that both the mesh and the jet nebulizers preserved the binding affinity to EGFR and the inhibitory activities of cetuximab.
Conclusions
Altogether, our results indicate that cetuximab resists the physical constraints of nebulization. Thus, airway delivery represents a promising alternative to systemic administration for local delivery of therapeutic antibodies in lung cancer treatment.





Similar content being viewed by others
References
L. G. Collins, C. Haines, R. Perkel, and R. E. Enck. Lung cancer: diagnosis and management. Am. Fam. Phys. 75:56–63 (2007).
G. Scheuch, M. J. Kohlhaeufl, P. Brand, and R. Siekmeier. Clinical perspectives on pulmonary systemic and macromolecular delivery. Adv. Drug Deliv. Rev. 58:996–1008 (2006).
J. S. Patton, and P. R. Byron. Inhaling medicines: delivering drugs to the body through the lungs. Nat. Rev. Drug Discov. 6:67–74 (2007).
A. J. Bitonti, and J. A. Dumont. Pulmonary administration of therapeutic proteins using an immunoglobulin transport pathway. Adv. Drug Deliv. Rev. 58:1106–1118 (2006).
J. S. Patton, C. S. Fishburn, and J. G. Weers. The lungs as a portal of entry for systemic drug delivery. Proc. Am. Thorac. Soc. 1:338–344 (2004).
R. U. Agu, M. I. Ugwoke, M. Armand, R. Kinget, and N. Verbeke. The lung as a route for systemic delivery of therapeutic proteins and peptides. Respir. Res. 2:198–209 (2001).
L. Fabbri. Pulmonary safety of inhaled insulins: a review of the current data. Curr. Med. Res. Opin. 22(Suppl 3):21–28 (2006).
F. Gagnadoux, A. Le Pape, E. Lemarie, S. Lerondel, I. Valo, V. Leblond, J. Racineux, and T. Urban. Aerosol delivery of chemotherapy in an orthotopic model of lung cancer. Eur. Respir. J. 26:657–661 (2005).
A. E. Hershey, I. D. Kurzman, L. J. Forrest, C. A. Bohling, M. Stonerook, M. E. Placke, A. R. Imondi, and D. M. Vail. Inhalation chemotherapy for macroscopic primary or metastatic lung tumors: proof of principle using dogs with spontaneously occurring tumors as a model. Clin. Cancer Res. 5:2653–2659 (1999).
N. V. Koshkina, J. C. Waldrep, L. E. Roberts, E. Golunski, S. Melton, and V. Knight. Paclitaxel liposome aerosol treatment induces inhibition of pulmonary metastases in murine renal carcinoma model. Clin. Cancer Res. 7:3258–3262 (2001).
N. V. Koshkina, and E. S. Kleinerman. Aerosol gemcitabine inhibits the growth of primary osteosarcoma and osteosarcoma lung metastases. Int. J. Cancer 116:458–463 (2005).
V. Knight, N. V. Koshkina, J. C. Waldrep, B. C. Giovanella, and B. E. Gilbert. Anticancer effect of 9-nitrocamptothecin liposome aerosol on human cancer xenografts in nude mice. Cancer Chemother. Pharmacol. 44:177–186 (1999).
P. M. Anderson, S. N. Markovic, J. A. Sloan, M. L. Clawson, M. Wylam, C. A. Arndt, W. A. Smithson, P. Burch, M. Gornet, and E. Rahman. Aerosol granulocyte macrophage-colony stimulating factor: a low toxicity, lung-specific biological therapy in patients with lung metastases. Clin. Cancer Res. 5:2316–2323 (1999).
C. F. Verschraegen, B. E. Gilbert, E. Loyer, A. Huaringa, G. Walsh, R. A. Newman, and V. Knight. Clinical evaluation of the delivery and safety of aerosolized liposomal 9-nitro-20(s)-camptothecin in patients with advanced pulmonary malignancies. Clin. Cancer Res. 10:2319–2326 (2004).
G. A. Otterson, M. A. Villalona-Calero, S. Sharma, M. G. Kris, A. Imondi, M. Gerber, D. A. White, M. J. Ratain, J. H. Schiller, A. Sandler, M. Kraut, S. Mani, and J. R. Murren. Phase I study of inhaled doxorubicin for patients with metastatic tumors to the lungs. Clin. Cancer Res. 13:1246–1252 (2007).
B. P. H. Wittgen, P. W. A. Kunst, K. van der Born, A. W. van Wijk, W. Perkins, F. G. Pilkiewicz, R. Perez-Soler, S. Nicholson, G. J. Peters, and P. E. Postmus. Phase I study of aerosolized slit cisplatin in the treatment of patients with carcinoma of the lung. Clin. Cancer Res. 13:2414–2421 (2007).
M. Z. Lin, M. A. Teitell, and G. J. Schiller. The evolution of antibodies into versatile tumor-targeting agents. Clin. Cancer Res. 11:129–138 (2005).
M. S. Nayeem, and R. H. Khan. Recombinant antibodies in cancer therapy. Curr. Protein Pept. Sci. 7:165–170 (2006).
L. Dellamary, D. J. Smith, A. Bloom, S. Bot, G. Guo, H. Deshmuk, M. Costello, and A. Bot. Rational design of solid aerosols for immunoglobulin delivery by modulation of aerodynamic and release characteristics. J. Control. Release 95:489–500 (2004).
S. Schule, W. Friess, K. Bechtold-Peters, and P. Garidel. Conformational analysis of protein secondary structure during spray-drying of antibody/mannitol formulations. Eur. J. Pharm. Biopharm. 65:1–9 (2007).
M. Maury, K. Murphy, S. Kumar, A. Mauerer, and G. Lee. Spray-drying of proteins: effects of sorbitol and trehalose on aggregation and FT-IR amide I spectrum of an immunoglobulin G. Eur. J. Pharm. Biopharm. 59:251–261 (2005).
A. J. Bitonti, J. A. Dumont, S. C. Low, R. T. Peters, K. E. Kropp, V. J. Palombella, J. M. Stattel, Y. Lu, C. A. Tan, J. J. Song, A. M. Garcia, N. E. Simister, G. M. Spiekermann, W. I. Lencer, and R. S. Blumberg. Pulmonary delivery of an erythropoietin Fc fusion protein in non-human primates through an immunoglobulin transport pathway. Proc. Natl. Acad. Sci. U S A. 101:9763–9768 (2004).
S. C. Low, S. L. Nunes, A. J. Bitonti, and J. A. Dumont. Oral and pulmonary delivery of fsh-Fc fusion proteins via neonatal Fc receptor-mediated transcytosis. Hum. Reprod. 20:1805–1813 (2005).
N. Hanna, R. Lilenbaum, R. Ansari, T. Lynch, R. Govindan, P. A. Janne, and P. Bonomi. Phase II trial of cetuximab in patients with previously treated non-small-cell lung cancer. J. Clin. Oncol. 24:5253–5258 (2006).
J. V. Heymach, M. Nilsson, G. Blumenschein, V. Papadimitrakopoulou, and R. Herbst. Epidermal growth factor receptor inhibitors in development for the treatment of non-small cell lung cancer. Clin. Cancer Res. 12:4441s–4445s (2006).
R. C. Lilenbaum. The evolving role of cetuximab in non-small cell lung cancer. Clin. Cancer Res. 12:4432s–4435s (2006).
D. D. Miller, M. M. Amin, L. B. Palmer, A. R. Shah, and G. C. Smaldone. Aerosol delivery and modern mechanical ventilation: in vitro/in vivo evaluation. Am. J. Respir. Crit. Care Med. 168:1205–1209 (2003).
L. Vecellio None, D. Grimbert, M. H. Becquemin, E. Boissinot, A. Le Pape, E. Lemarie, and P. Diot. Validation of laser diffraction method as a substitute for cascade impaction in the European project for a nebulizer standard. J. Aerosol Med. 14:107–114 (2001).
D. S. Salomon, R. Brandt, F. Ciardiello, and N. Normanno. Epidermal growth factor-related peptides and their receptors in human malignancies. Crit. Rev. Oncol. Hematol. 19:183–232 (1995).
M. L. Janmaat, F. A. E. Kruyt, J. A. Rodriguez, and G. Giaccone. Response to epidermal growth factor receptor inhibitors in non-small cell lung cancer cells: limited antiproliferative effects and absence of apoptosis associated with persistent activity of extracellular signal-regulated kinase or akt kinase pathways. Clin. Cancer Res. 9:2316–2326 (2003).
G. N. Gill, T. Kawamoto, C. Cochet, A. Le, J. D. Sato, H. Masui, C. McLeod, and J. Mendelsohn. Monoclonal anti-epidermal growth factor receptor antibodies which are inhibitors of epidermal growth factor binding and antagonists of epidermal growth factor binding and antagonists of epidermal growth factor-stimulated tyrosine protein kinase activity. J. Biol. Chem. 259:7755–7760 (1984).
W. K. Bleeker, J. J. Lammerts van Bueren, H. H. van Ojik, A. F. Gerritsen, M. Pluyter, M. Houtkamp, E. Halk, J. Goldstein, J. Schuurman, M. A. van Dijk, J. G. J. van de Winkel, and P. W. H. I. Parren. Dual mode of action of a human anti-epidermal growth factor receptor monoclonal antibody for cancer therapy. J. Immunol. 173:4699–4707 (2004).
J. Baselga. The EGFR as a target for anticancer therapy-focus on cetuximab. Eur. J. Cancer. 37(Suppl 4):16–22 (2001).
R. U. Agu, S. Valiveti, K. S. Paudel, M. Klausner, P. J. Hayden, and A. L. Stinchcomb. Permeation of win 55,212-2, a potent cannabinoid receptor agonist, across human tracheo-bronchial tissue in vitro and rat nasal epithelium vivo. J. Pharm. Pharmacol. 58:1459–1465 (2006).
H. Steckel, and F. Eskandar. Factors affecting aerosol performance during nebulization with jet and ultrasonic nebulizers. Eur. J. Pharm. Sci. 19:443–455 (2003).
I. Fangmark, and J. C. Carpin. Protein nebulization. J. Aerosol. Sci. 27:231–232 (1996).
H. C. Mahler, R. Müller, W. Frieß, A. Delille, and S. Matheus. Induction and analysis of aggregates in a liquid IgG1-antibody formulation. Eur. J. Pharm. Biopharm. 59(3):407–417 (2005).
H. Schellekens. Factors influencing the immunogenicity of therapeutic proteins.Nephrol. Dial. Transplant. 6:3–9 (2005).
Acknowledgements
We thank Michèle De Monte for helpful suggestions in statistical analysis. This work was supported by grants from Cancéropôle Grand Ouest, IFR135 (Institut Fédératif de Recherche), la Ligue contre le Cancer. Agnès Maillet’s fellowships were donated by SPLF (Société de Pneumologie de Langue Française) and Pneumologie Dévelopement.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maillet, A., Congy-Jolivet, N., Le Guellec, S. et al. Aerodynamical, Immunological and Pharmacological Properties of the Anticancer Antibody Cetuximab Following Nebulization. Pharm Res 25, 1318–1326 (2008). https://doi.org/10.1007/s11095-007-9481-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-007-9481-3