Abstract
Purpose
Due to inconsistent definitions used in the literature, the prevalence of rapid eye movement (REM)-related sleep-disordered breathing (SDB) has been quite variable and its clinical significance remains unclear. This study aimed to compare the prevalence of and clinical characteristics between various criteria for defining REM-related SDB. We also investigated how frequently CPAP therapy was recommended in patients with REM-related SDB and if they had lower CPAP adherence compared to non-stage-specific SDB.
Methods
In this cross-sectional study, we evaluated 1,019 consecutive adults referred for a polysomnogram for suspicion of SDB. The prevalence of REM-related SDB was calculated based on “traditional criteria” commonly reported in the literature and a “strict criteria” that minimized the contribution of SDB during non-REM sleep.
Results
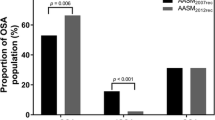
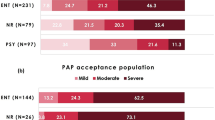
The prevalence of REM-related SDB ranged from 13.5% to 36.7%. There were no clinically significant differences between the strict definition and the traditional definition of REM-related SDB. REM-related SDB was more prevalent in women, younger individuals and African Americans. Compared to non-stage-specific obstructive sleep apnea (OSA), patients with REM-related SDB were equally symptomatic and hypersomnolent. CPAP titration was recommended in 88% of patients with REM-related SDB vs. 94% of patients with non-stage-specific OSA (p < 0.001). There was no significant difference in CPAP adherence between the two groups.
Conclusions
Regardless of how REM-related SDB is defined, it was highly prevalent in our large clinical cohort. Compared to non-stage-specific OSA, these patients were equally hypersomnolent and adherent to CPAP therapy despite having overall significantly milder OSA. Further research is needed to better establish whether these patients will derive any benefit from long-term CPAP therapy.
Similar content being viewed by others
References
Haba-Rubio J, Janssens JP, Rochat T, Sforza E (2005) Rapid eye movement-related disordered breathing: clinical and polysomnographic features. Chest 128(5):3350–3357
Koo BB, Dostal J, Ioachimescu O, Budur K (2008) The effects of gender and age on REM-related sleep-disordered breathing. Sleep Breath 12(3):259–264
Koo BB, Patel SR, Strohl K, Hoffstein V (2008) Rapid eye movement-related sleep-disordered breathing: influence of age and gender. Chest 134(6):1156–1161
Resta O, Carpanano GE, Lacedonia D, Di Gioia G, Giliberti T, Stefano A, Bonfitto P (2005) Gender difference in sleep profile of severely obese patients with obstructive sleep apnea (OSA). Respir Med 99(1):91–96
Chami HA, Baldwin CM, Silverman A, Zhang Y, Rapoport D, Punjabi N, Gottlieb DJ (2010) Sleepiness, quality of life, and sleep maintenance in REM versus non-REM sleep-disordered breathing. Am J Respir Crit Care Med 181(9):997–1002
Goh DY, Galster P, Marcus CL (2000) Sleep architecture and respiratory disturbances in children with obstructive sleep apnea. Am J Respir Crit Care Med 162(2 Pt 1):682–686
O’Connor C, Thornley KS, Hanly PJ (2000) Gender differences in the polysomnographic features of obstructive sleep apnea. Am J Respir Crit Care Med 161(5):1465–1472
Punjabi NM, Caffo BS, Goodwin JL, Gottlieb DJ, Newman AB, O’Connor GT, Rapoport DM, Redline S, Resnick HE, Robbins JA, Shahar E, Unruh ML, Samet JM (2009) Sleep-disordered breathing and mortality: a prospective cohort study. PLoS Med 6(8):e1000132
Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla KM (2008) Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep 31(8):1071–1078
Peppard PE, Ward NR, Morrell MJ (2009) The impact of obesity on oxygen desaturation during sleep-disordered breathing. Am J Respir Crit Care Med 180(8):788–793
Findley LJ, Wilhoit SC, Suratt PM (1985) Apnea duration and hypoxemia during REM sleep in patients with obstructive sleep apnea. Chest 87(4):432–436
Somers VK, Dyken ME, Clary MP, Abboud FM (1995) Sympathetic neural mechanisms in obstructive sleep apnea. J Clin Invest 96(4):1897–1904
Chervin RD, Aldrich MS (1998) The relation between multiple sleep latency test findings and the frequency of apneic events in REM and non-REM sleep. Chest 113(4):980–984
Punjabi NM, Bandeen-Roche K, Marx JJ, Neubauer DN, Smith PL, Schwartz AR (2002) The association between daytime sleepiness and sleep-disordered breathing in NREM and REM sleep. Sleep 25(3):307–314
Kass JE, Akers SM, Bartter TC, Pratter MR (1996) Rapid-eye-movement-specific sleep-disordered breathing: a possible cause of excessive daytime sleepiness. Am J Respir Crit Care Med 154(1):167–169
Iber C, Ancoli-Israel S, Chesson A, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications, 1st ed. American Academy of Sleep Medicine, Westchester
Kushida CA, Littner MR, Hirshkowitz M, Morgenthaler TI, Alessi CA, Bailey D, Boehlecke B, Brown TM, Coleman J Jr, Friedman L, Kapen S, Kapur VK, Kramer M, Lee-Chiong T, Owens J, Pancer JP, Swick TJ, Wise MS (2006) Practice parameters for the use of continuous and bilevel positive airway pressure devices to treat adult patients with sleep-related breathing disorders. Sleep 29(3):375–380
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep 14(6):540–545
Radloff LS (1977) The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1(3):385–401
Conflicts of interest
None of the authors have a conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Conwell, W., Patel, B., Doeing, D. et al. Prevalence, clinical features, and CPAP adherence in REM-related sleep-disordered breathing: a cross-sectional analysis of a large clinical population. Sleep Breath 16, 519–526 (2012). https://doi.org/10.1007/s11325-011-0537-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-011-0537-6