Abstract
Background
Sleep apnea (SA) may be linked to coronary artery disease (CAD). Both conditions have similar risk factors, confounding the analyses. Investigation of the lipid profile is routine in the adult population, even without symptoms or suspected cardiac ailment. SA, however, remains underdiagnosed even in the presence of unambiguous clinical manifestations.
Purpose
The aim of this study was to verify the association between SA and CAD, adjusting for usual CAD risk factors.
Methods
Patients who underwent diagnostic or therapeutic coronariography and portable type III polysomnography were studied. The severity of SA was determined by the apnea–hypopnea index (AHI). We measured classic CAD risk factors: fasting glucose; total, HDL, and LDL cholesterols; triglycerides; uric acid, and high-sensitivity C-reactive protein. We excluded patients older than 65 years, with body mass index higher than 40 kg/m2, with diabetes, and with history of smoking in the last year.
Results
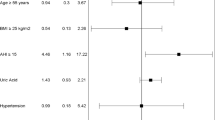
Of 55 included patients, 28 had AHI > 14, showing an odds ratio of 8.7 for CAD. Patients without (n = 29) and with CAD (n = 26), showed AHI of, respectively, 11 ± 11 and 23 ± 14 per hour (P = 0.001). In a binary logistic regression to predict CAD, controlling for all the above risk factors, the only variables entered in the stepwise model were AHI (either as continuous or categorical variable) and uric acid.
Conclusion
In a sample without smokers, morbidly obese, or diabetic patients, AHI is the main predictor of CAD. SA should integrate the set of risk factors routinely assessed in clinical investigation for coronary disease risk stratification.


Similar content being viewed by others
References
Somers VK, White DP, Amin R, Abraham WT, Costa F, Culebras A, Daniels S, Floras JS, Hunt CE, Olson LJ, Pickering TG, Russell R, Woo M, Young T (2008) Sleep apnea and cardiovascular disease: an American Heart Association/American College of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council on Cardiovascular Nursing. J Am Coll Cardiol 8:686–717
Crummy F, Piper AJ, Naughton MT (2008) Obesity and the lung: 2. Obesity and sleep-disordered breathing. Thorax 8:738–746
Devulapally K, Pongonis R Jr, Khayat R (2009) OSA: the new cardiovascular disease: part II: overview of cardiovascular diseases associated with obstructive sleep apnea. Heart Fail Rev 3:155–164
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, Jones DW, Materson BJ, Oparil S, Wright JT Jr, Roccella EJ, Heart N, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure, National High Blood Pressure Education Program Coordinating Committee (2003) The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC VII). J Am Med Assoc 289:2560–2572
Lüthje L, Andreas S (2008) Obstructive sleep apnea and coronary artery disease. Sleep Med Rev 1:19–31
Nelson CA, Wolk R, Somers VK (2005) Sleep-disordered breathing: implications for the pathophysiology and management of cardiovascular disease. Compr Ther 1:21–27
Leung RS (2009) Sleep-disordered breathing: autonomic mechanisms and arrhythmias. Prog Cardiovasc Dis 4:324–338
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V (2005) Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med 19:2034–2041
Gami AS, Howard DE, Olson EJ, Somers VK (2005) Day-night pattern of sudden death in obstructive sleep apnea. N Engl J Med 12:1206–1214
McNicholas WT, Bonsigore MR (2007) Management Committee of EU COST ACTION B26. Sleep apnoea as an independent risk factor for cardiovascular disease: current evidence, basic mechanisms and research priorities. Eur Respir J 1:156–178
Butt M, Dwivedi G, Khair O, Lip GY (2010) Obstructive sleep apnea and cardiovascular disease. Int J Cardiol 1:7–16
Gottlieb DJ, Yenokyan G, Newman AB, O'Connor GT, Punjabi NM, Quan SF, Redline S, Resnick HE, Tong EK, Diener-West M, Shahar E (2010) Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure. The Sleep Heart Health Study. Circulation 4:352–360
Peker Y, Kraiczi H, Hedner J, Löth S, Johansson A, Bende M (1999) An independent association between obstructive sleep apnoea and coronary artery disease. Eur Respir J 1:179–184
Klein C, Martinez D, Hackenhaar FS, Medeiros TM, Marcolin ML, Silveira FS, Wainstein MV, Gonçalvez SC, Benfato MS (2010) Carbonyl groups: bridging the gap between sleep disordered breathing and coronary artery disease. Free Radic Res 8:907–912
Tonelli de Oliveira AC, Martinez D, Vasconcelos LF, Gonçalves SC, Lenz MC, Fuchs SC, Gus M, Abreu-Silva EO, Moreira LB, Fuchs FD (2009) Diagnosis of obstructive sleep apnea syndrome and its outcomes with home portable monitoring. Chest 2:330–336
American Academy of Sleep Medicine (2005) International classification of sleep disorders. Diagnostic and coding manual (ICSD-2). 2nd ed. Westchester, IL
Punjabi NM, Sorkin JD, Katzel LI, Goldberg AP, Schwartz AR, Smith PL (2002) Sleep-disordered breathing and insulin resistance in middle-aged and overweight men. Am J Respir Crit Care Med 5:677–682
Lear SA, Chen MM, Birmingham CL, Frohlich JJ (2003) The relationship between simple anthropometric indices and C-reactive protein: ethnic and gender differences. Metabolism 12:1542–1546
Ryan S, Taylor CT, McNicholas WT (2009) Systemic inflammation: a key factor in the pathogenesis of cardiovascular complications in obstructive sleep apnoea syndrome? Thorax 7:631–636
Steiropoulos P, Kotsianidis I, Nena E, Tsara V, Gounari E, Hatzizisi O, Kyriazis G, Christaki P, Froudarakis M, Bouros D (2009) Long-term effect of continuous positive airway pressure therapy on inflammation markers of patients with obstructive sleep apnea syndrome. Sleep 4:537–543
Taheri S, Austin D, Lin L, Nieto FJ, Young T, Mignot E (2007) Correlates of serum C-reactive protein (CRP) -no association with sleep duration or sleep disordered breathing. Sleep 8:991–996
Kao TW, Lu IS, Liao KC, Lai HY, Loh CH, Kuo HK (2009) Associations between body mass index and serum levels of C-reactive protein. S Afr Med J 5:326–330
Kono M, Tatsumi K, Saibara T, Nakamura A, Tanabe N, Takiguchi Y, Kuriyama T (2007) Obstructive sleep apnea syndrome is associated with some components of metabolic syndrome. Chest 5:1387–1392
Drager LF, Bortolotto LA, Maki-Nunes C, Trombetta IC, Alves MJ, Fraga RF, Negrão CE, Krieger EM, Lorenzi-Filho G (2010) The incremental role of obstructive sleep apnoea on markers of atherosclerosis in patients with metabolic syndrome. Atherosclerosis 2:490–495
Roche F, Sforza E, Pichot V, Maudoux D, Garcin A, Celle S, Picard-Kossovsky M, Gaspoz JM, Barthélémy JC, PROOF Study Group (2009) Obstructive sleep apnoea/hypopnea influences high-density lipoprotein cholesterol in the elderly. Sleep Med 8:882–886
Gonçalves SC, Martinez D, Gus M, de Abreu-Silva EO, Bertoluci C, Dutra I, Branchi T, Moreira LB, Fuchs SC, de Oliveira AC, Fuchs FD (2007) Obstructive sleep apnea and resistant hypertension: a case–control study. Chest 6:1858–1862
Lopez-Jimenez F, Sert Kuniyoshi FH, Gami A, Somers VK (2008) Obstructive sleep apnea: implications for cardiac and vascular disease. Chest 3:793–804
Kim SY, Guevara JP, Kim KM, Choi HK, Heitjan DF, Albert DA (2010) Hyperuricemia and coronary heart disease: a systematic review and meta-analysis. Arthritis Care Res 2:170–180
Lavie L, Hefetz A, Luboshitzky R, Lavie P (2003) Plasma levels of nitric oxide and L-arginine in sleep apnea patients: effects of nCPAP treatment. J Mol Neurosci 1:57–63
Gagliardi AC, Miname MH, Santos RD (2009) Uric acid: a marker of increased cardiovascular risk. Atherosclerosis 1:11–17
Tsai WC, Huang YY, Lin CC, Li WT, Lee CH, Chen JY, Chen JH (2009) Uric acid is an independent predictor of arterial stiffness in hypertensive patients. Heart Vess 5:371–375. doi:10.1007/s00380-008-1127-9
Drager LF, Bortolotto LA, Figueiredo AC, Krieger EM, Lorenzi GF (2007) Effects of continuous positive airway pressure on early signs of atherosclerosis in obstructive sleep apnea. Am J Respir Crit Care Med 7:706–712
De Luis DA, González Sagrado M, Conde R, Aller R, Izaola O (2010) Resistin levels and inflammatory markers in patients with morbid obesity. Nutr Hosp 4:630–634
Chami HA, Resnick HE, Quan SF, Gottlieb DJ (2011) Association of incident cardiovascular disease with progression of sleep-disordered breathing. Circulation 12:1280–1286
Martinez D, da Silva RP, Klein C, Fiori CZ, Massierer D, Cassol CM, Bos AJ, Gus M (2011) High risk for sleep apnea in the Berlin questionnaire and coronary artery disease. Sleep and Breathing 6. doi:10.1007/s11325-010-0460-2
Dempsey JA, Veasey SC, Morgan BJ, O'Donnell CP (2010) Pathophysiology of sleep apnea. Physiol Rev 1:47–112
Kohli P, Balachandran JS, Malhotra A (2011) Obstructive sleep apnea and the risk for cardiovascular disease. Curr Atheroscler Rep 2:138–146
Hui DS, Ko FW, Fok JP, Chan MC, Li TS, Tomlinson B, Cheng G (2004) The effects of nasal continuous positive airway pressure on platelet activation in obstructive sleep apnea syndrome. Chest 5:1768–1775
Yumino D, Redolfi S, Ruttanaumpawan P, Su MC, Smith S, Newton GE, Mak S, Bradley TD (2010) Nocturnal rostral fluid shift: a unifying concept for the pathogenesis of obstructive and central sleep apnea in men with heart failure. Circulation 14:1598–1605
Acknowledgments
Drs. Jorge Pinto Ribeiro and Marco Vugman Wainstein are thanked for their valuable contribution in providing data from the cineangiocoronariography.
Financial support
Students received grants from the Brazilian government through CAPES and CNPq. The main support was offered by the Research Incentive Fund (FIPE) of the Hospital de Clínicas de Porto Alegre (Porto Alegre, Rio Grande do Sul, Brazil).
Conflict of interest
The authors declare that they have no conflict of interest regarding the present study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martinez, D., Klein, C., Rahmeier, L. et al. Sleep apnea is a stronger predictor for coronary heart disease than traditional risk factors. Sleep Breath 16, 695–701 (2012). https://doi.org/10.1007/s11325-011-0559-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-011-0559-0