Abstract
Background
Sleep bruxism (SB) is a movement described as an involuntary mastication movement during sleep, also defined as rhythmic masticatory muscle activity (RMMA). It is observed in 2–40 % of the pediatric population. A link was suggested between respiratory events and RMMA. Rapid palatal expansion (RPE) is an effective orthopedic treatment for correcting maxillary transverse deficiency and sleep-disordered breathing (SDB) in children. The aim was to evaluate the possible reduction of SB after rapid palatal expansion (RPE) therapy.
Methods
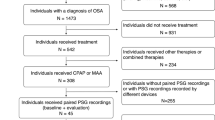
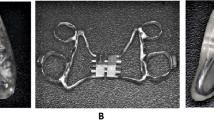
A total of 32 patients (8–14 years old; 22 girls and 10 boys) received an orthodontic treatment for transverse maxillary deficiency (5 mm or more) at the orthodontics department of the Université de Montréal. They underwent an ambulatory polysomnography (PSG) before, after expansion with the expander, and at the end of the study without the expander. They were classified into three subgroups based on sleep electromyography (EMG) data.
Results
Total sleep time and stage NREM 3 presented significant differences between the types of appliances. Moreover, there was a time effect observed for total sleep time, sleep cycles, stage NREM 2, and stage REM, while only a trend suggested for stage NREM 3. Significant differences were observed between subgroups for both RMMA episodes and burst indexes, similarly, for the oxygen desaturation index (ODI). A total of 50 % of the patients were classified as responders when RMMA episodes index decreased by more than 25 % when comparing treatment efficacy at baseline night.
Conclusion
Most bruxers (65 %) reduced their RMMA episode index after expansion, but sleep and respiratory variables remained unchanged.

Similar content being viewed by others
Abbreviations
- AHI:
-
Apnea-hypopnea index
- ECG:
-
Electrocardiography
- EEG:
-
Electroencephalography
- EMG:
-
Electromyography
- EOG:
-
Electrooculography
- NREM:
-
Non rapid eye movement
- ODI:
-
Oxygen desaturation index
- OSA:
-
Obstructive sleep apnea
- PSG:
-
Polysomnography
- RMMA:
-
Rhythmic activity of masticatory muscles
- REM:
-
Rapid eye movement
- RME:
-
Rapid maxillary expansion
- RPE:
-
Rapid palatal expansion
- SB:
-
Sleep bruxism
- SDB:
-
Sleep-disordered breathing
- SEM:
-
Standard error mean
References
Lobbezoo F, Ahlberg JA, Glaros G, Kato T, Koyano K, Lavigne GJ, de Leeuw R, Manfredini D, Svensson P, Winocur E (2013) Bruxism defined and graded: an international consensus. J Oral Rehabil 40(1):2–4. doi:10.1111/joor.12011
Carra MC, Huynh NT, El-Khatib H, Remise C, Lavigne GJ (2013) Sleep bruxism, snoring, and headaches in adolescents: short-term effects of a mandibular advancement appliance. Sleep Med 14(7):656–661. doi:10.1016/j.sleep.2013.03.009
Garde JB, Suryavanshi RK, Jawale BA, Deshmukh V, Dadhe DP, Suryavanshi MK (2014) An epidemiological study to know the prevalence of deleterious oral habits among 6 to 12 year old children. J Int Oral Health 6(1):39–43
Itani O, Kaneita Y, Ikeda M, Kondo S, Yamamoto R, Osaki Y, Kanda H, Suzuki K, Higuchi S, Ohida T (2013) Disorders of arousal and sleep-related bruxism among Japanese adolescents: a nationwide representative survey. Sleep Med 14(6):532–541. doi:10.1016/j.sleep.2013.03.005
Cheifetz AT, Osganian SK, Allred EN, Needleman HL (2005) Prevalence of bruxism and associated correlates in children as reported by parents. J Dent Child (Chic) 72(2):67–73
Maluly M, Andersen ML, Dal-Fabbro C, Garbuio S, Bittencourt L, de Siqueira JT, Tufik S (2013) Polysomnographic study of the prevalence of sleep bruxism in a population sample. J Dent Res 9(7 Suppl):97S–103S. doi:10.1177/0022034513484328
Manfredini D, Restrepo C, Diaz-Serrano K, Winocur E, Lobbezoo F (2013) Prevalence of sleep bruxism in children: a systematic review of the literature. J Oral Rehabil 40(8):631–642. doi:10.1111/joor.12069
Ohayon MM, Li KK, Guilleminault C (2001) Risk factors for sleep bruxism in the general population. Chest 119(1):53–61. doi:10.1378/chest.119.1.53
Rossi D, Manfredini D (2013) Family and school environmental predictors of sleep bruxism in children. J Orofacial Pain 27(2):135–141. doi:10.11607/jop.1057
Simoes-Zenari M, Bitar ML (2010) Factors associated to bruxism in children from 4–6 years. Pro-Fono Revista de Atualizacao Cientifica 22(4):465–472
Restrepo CC (2010) Bruxism in children. In: Paesani DA (ed) Bruxism: theory and practice. Quintessence, Berlin, pp 111–120
Lavigne GJ, Rompré PH, Montplaisir JY (1996) Sleep bruxism: validity of clinical research diagnostic criteria in a controlled polysomnographic study. J Dent Res 75(1):546–552. doi:10.1177/00220345960750010601
Macaluso GM, Guerra P, Di Giovanni G, Boselli M, Parrino L, Terzano MG (1998) Sleep bruxism is a disorder related to periodic arousals during sleep. J Dent Res 77(4):565–573. doi:10.1177/00220345980770040901
Reding GR, Zepelin H, Robinson JE Jr, Zimmerman SO, Smith VH (1968) Nocturnal teeth-grinding: all-night psychophysiologic studies. J Dent Res 47(5):786–797. doi:10.1177/00220345680470052001
Sjöholm T, Lehtinen II, Helenius H (1995) Masseter muscle activity in diagnosed sleep bruxists compared with non-symptomatic controls. J Sleep Res 4(1):48–55. doi:10.1111/j.1365-2869.1995.tb00150.x
Lavigne GJ, Manzini C (2000) Sleep bruxism and concomitant motor activity. In: Kryger MH, Roth T, Dement WC (eds) Principles and practice of sleep medicine Philadelphia, W.B. Saunders, pp 773–85
Lavigne GJ, Khoury S, Abe S, Yamaguchi T, Raphael K (2008) Bruxism physiology and pathology: an overview for clinicians. J Oral Rehabil 35(7):476–494. doi:10.1111/j.1365-2842.2008.01881.x
Rompré PH, Daigle-Landry D, Guitard F, Montplaisir JY, Lavigne GJ (2007) Identification of a sleep bruxism subgroup with a higher risk of pain. J Dent Res 86(9):837–842. doi:10.1177/154405910708600906
Thorpy MJ (1990) International classification of sleep disorders: diagnostic and coding manual diagnostic. American Sleep Disorders Association Rochester, MN
Fallone G, Owens JA, Deane J (2002) Sleepiness in children and adolescents: clinical implications. Sleep Med Rev 6(4):287–306. doi:10.1053/smrv.2001.0192
Mindell JA, Owens JA (2010) A clinical guide to pediatric sleep: diagnosis and management of sleep problems, 2nd edn. Wolters Kluwer Health/Lippincott Williams and Wilkins, Philadelphia
Sheldon SH, Ferber R, Kryger MH (2005) Principles and practice of pediatric sleep medicine, 1st edn. Elsevier Saunders, USA
Sherrington CS (1946) Man of his nature. doi.:10.1017/CBO9780511694196
Barbosa TS, Miyakoda LS, Pocztaruk RL, Rocha CP, Gaviao MB (2008) Temporomandibular disorders and bruxism in childhood and adolescence: review of the literature. Int J Pediatr Otorhinolaryngol 72(3):299–314. doi:10.1016/j.ijporl.2007.11.006
Lavigne G, Manzini C, Huynh NT (2011) Sleep bruxism. In: Kryger MH, Roth T, Dement WC (eds) Principles and practice of sleep medicine, 5th edn. Elservier Saunders, St-Louis, pp 1129–1139
Miyawaki S, Lavigne GJ, Pierre M, Guitard F, Montplaisir JY, Kato T (2003) Association between sleep bruxism, swallowing-related laryngeal movement, and sleep positions. Sleep 26(4):461–465
Thie NM, Kato T, Bader G, Montplaisir JY, Lavigne GJ (2002) The significance of saliva during sleep and the relevance of oromotor movements. Sleep Med Rev 6(3):213–227. doi:10.1053/smrv.2001.0183
Lavigne GJ, Rompré PH, Guitard F, Sessle BJ, Kato T, Montplaisir JY (2002) Lower number of K-complexes and K-alphas in sleep bruxism: a controlled quantitative study. Clin Neurophysiol 113(5):686–693. doi:10.1016/S1388-2457(02)00037-8
Restrepo CC, Sforza C, Colombo A, Peláez-Vargas A, Ferrario VF (2008) Palate morphology of bruxist children with mixed dentition. A pilot study. J Oral Rehabil 35(5):353–360. doi:10.1111/j.1365-2842.2008.01848.x
AASM (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications, 1st edn. American Academy of Sleep Medicine, Westchester)
Brunner E, Domhof S, Langer F (2002) Nonparametric analysis of longitudinal data in factorial experiments. Wiley, New York
Hasegawa Y, Lavigne G, Rompré P, Kato T, Urade M, Huynh N (2013) Is there a first night effect on sleep bruxism? A sleep laboratory study. J Clin Sleep Med 9(11):1139–1145. doi:10.5664/jcsm.3152
Cistulli PA, Palmisano RG, Poole MD (1998) Treatment of obstructive sleep apnea syndrome by rapid maxillary expansion. Sleep 21(8):831–835
Guilleminault C, Quo S, Huynh NT, Li K (2008) Orthodontic expansion treatment and adenotonsillectomy in the treatment of obstructive sleep apnea in prepubertal children. Sleep 31(7):953–957
Pirelli P, Saponara M, Guilleminault C (2004) Rapid maxillary expansion in children with obstructive sleep apnea syndrome. Sleep 27(4):761–766
Villa MP, Rizzoli A, Miano S, Malagola C (2011) Efficacy of rapid maxillary expansion in children with obstructive sleep apnea syndrome: 36 months of follow-up. Sleep Breathing Schlaf Atmung 15(2):179–184. doi:10.1007/s11325-011-0505-1
Schutz TC, Dominguez GC, Hallinan MP, Cunha TC, Tufik S (2011) Class II correction improves nocturnal breathing in adolescents. Angle Orthod 81(2):222–228. doi:10.2319/052710-233.1
Acknowledgments
The authors would like to thank Dr. Gilles Lavigne, Pierre Rompré, and the participants for their input and support. The ambulatory devices were graciously provided by Dr. Gilles Lavigne.
Conflict of interest
The authors declare that they have no conflict of interest.
Sources of funding
This study was funded by the GramDENT scholarship, Geoffrion fund project both at the Université de Montréal, as well as the FRQ–S (RSBO) subvention.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bellerive, A., Montpetit, A., El-Khatib, H. et al. The effect of rapid palatal expansion on sleep bruxism in children. Sleep Breath 19, 1265–1271 (2015). https://doi.org/10.1007/s11325-015-1156-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1156-4