Abstract
Background
Reducing the need for diagnostic sleep studies for obstructive sleep apnea (OSA) would reduce direct and opportunity costs while expediting time to treatment for this common and morbid disorder. We sought to determine if an established sleep apnea screening questionnaire (STOP-BANG) and wrist-worn overnight oximetry data could provide high positive predictive value for the presence of OSA.
Methods
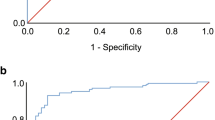
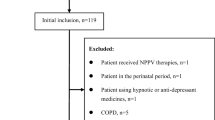
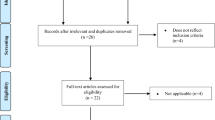
We conducted a prospective observational study of consecutive unattended sleep study patients at a single facility. Patients were referred for sleep testing after chart review by a sleep physician. We assessed area under the receiver-operating characteristic curve (ROC AUC) and positive predictive value (PPV) of STOP-BANG score and oxygen desaturation index (ODI) for a respiratory disturbance index (RDI) ≥15/h.
Results
Among 234 test patients, 65 % had an RDI ≥15/h. STOP-BANG had poor ability to discriminate these patients (ROC AUC 0.62). ODI added significant diagnostic information to the STOP-BANG score, increasing the ROC AUC to 0.86. Having the ODI, the STOP-BANG score no longer contributed significant diagnostic information, and the ODI alone discriminated as well as the combination (ROC AUC 0.86). Forty nine percent had an ODI ≥7/h, which had PPV of 92 % (95 % confidence interval (CI), 86 to 96 %). In the validation sample of 1,196 consecutive patients, ODI ≥ 7/h had a PPV of 97 % (95 % CI, 95 to 97 %).
Conclusions
Among patients with a high prevalence of OSA, high ODI is common and its presence has high PPV for OSA. These data suggest that overnight oximetry prior to sleep testing could significantly reduce the number of patients requiring sleep studies, thereby reducing costs and time to treatment.

Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- CPAP:
-
Continuous positive airway pressure
- HST:
-
Home sleep test
- ODI:
-
Oxygen desaturation index
- OSA:
-
Obstructive sleep apnea
- PAT:
-
Peripheral arterial tonometry
- PPV:
-
Positive predictive value
- PSG:
-
Polysomnogram
- RDI:
-
Respiratory disturbance index
- ROC AUC:
-
Receiver-operating characteristic area under curve
- VA:
-
Veterans Affairs
References
Giles TL, Lasserson TJ, Smith BH, White J, Wright J, Cates CJ (2006) Continuous positive airways pressure for obstructive sleep apnoea in adults. Cochrane Database Syst Rev 19, CD001106
Tregear S, Reston J, Schoelles K, Phillips B (2010) Continuous positive airway pressure reduces risk of motor vehicle crash among drivers with obstructive sleep apnea: systematic review and meta-analysis. Sleep 33:1373–1380
Fava C, Dorigoni S, Dalle Vedove F, Danese E, Montagnana M, Guidi GC, Narkiewicz K, Minuz P (2014) Effect of CPAP on blood pressure in patients with OSA/hypopnea a systematic review and meta-analysis. Chest 145:762–771
Chung F, Yegneswaran B, Liao P, Chung SA, Vairavanathan S, Islam S, Khajehdehi A, Shapiro CM (2008) STOP Questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology 108:812–821
Kunisaki KM, Brown KE, Fabbrini AE, Wetherbee EE, Rector TS (2014) STOP-BANG questionnaire performance in a Veterans Affairs unattended sleep study program. Ann Am Thorac Soc 11:192–197
Pittman SD, Ayas NT, MacDonald MM, Malhotra A, Fogel RB, White DP (2004) Using a wrist-worn device based on peripheral arterial tonometry to diagnose obstructive sleep apnea: in-laboratory and ambulatory validation. Sleep 27:923–933
Choi JH, Kim EJ, Kim YS, Choi J, Kim TH, Kwon SY, Lee HM, Lee SH, Shin C, Lee SH (2010) Validation study of portable device for the diagnosis of obstructive sleep apnea according to the new AASM scoring criteria: Watch-PAT 100. Acta Otolaryngol 130:838–843
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845
Chiner E, Signes-Costa J, Arriero JM, Marco J, Fuentes I, Sergado A (1999) Nocturnal oximetry for the diagnosis of the sleep apnoea hypopnoea syndrome: a method to reduce the number of polysomnographies? Thorax 54:968–971
Sériès F, Marc I, Cormier Y, La Forge J (1993) Utility of nocturnal home oximetry for case finding in patients with suspected sleep apnea hypopnea syndrome. Ann Intern Med 119:449–453
Lévy P, Pépin JL, Deschaux-Blanc C, Paramelle B, Brambilla C (1996) Accuracy of oximetry for detection of respiratory disturbances in sleep apnea syndrome. Chest 109:395–399
Magalang UJ, Dmochowski J, Veeramachaneni S, Draw A, Mador MJ, El-Solh A, Grant BJ (2003) Prediction of the apnea-hypopnea index from overnight pulse oximetry. Chest 124:1694–1701
Chung F, Liao P, Elsaid H, Islam S, Shapiro CM, Sun Y (2012) Oxygen desaturation index from nocturnal oximetry: a sensitive and specific tool to detect sleep-disordered breathing in surgical patients. Anesth Analg 114:993–1000
Kuna ST, Gurubhagavatula I, Maislin G, Hin S, Hartwig KC, McCloskey S, Hachadoorian R, Hurley S, Gupta R, Staley B, Atwood CW (2011) Noninferiority of functional outcome in ambulatory management of obstructive sleep apnea. Am J Respir Crit Care Med 183:1238–1244
Rosen CL, Auckley D, Benca R, Foldvary-Schaefer N, Iber C, Kapur V, Rueschman M, Zee P, Redline S (2012) A multisite randomized trial of portable sleep studies and positive airway pressure autotitration versus laboratory-based polysomnography for the diagnosis and treatment of obstructive sleep apnea: the home PAP study. Sleep 35:757–767
Acknowledgments
This study supported by an Upper Midwest Veterans Integrated Service Network 23 Strategic Initiative Award. The funding agency had no role in design or conduct of the study; collection, management, analysis, or interpretation of the data; preparation, review, or approval of the manuscript; nor decision to submit the manuscript for publication. We thank the Veterans Integrated Service Network (VISN) 23 for supporting this project. We thank the Minneapolis VA Sleep Clinic staff for assistance with data collection, logistic support for this study, and for their dedication to the sleep health of veterans.
Conflict of interest
The authors declare that they have no competing interests.
Guarantor
KMK and TSR had full access to the data and take responsibility for the integrity of the data and the accuracy of the data analysis. The lead author KMK affirms that the manuscript is an honest, accurate, and transparent account of the study being reported; that no important aspects of the study have been omitted; and that any discrepancies from the study as planned have been explained.
Disclaimer
The views expressed in this article are those of the authors and do not necessarily represent the views of VISN 23, the Minneapolis VA Health Care System, the U.S. Department of Veterans Affairs, the U.S. Government, or the University of Minnesota.
Author contributions
KMK conceived and designed the study, directed the statistical analyses, interpreted the data, drafted the manuscript, and approved the final version.
OG contributed to collection and interpretation of the data, revised the manuscript critically for important intellectual content, and approved the final version.
EEW contributed to the conception and design of the study, contributed to interpretation of the data, revised the manuscript critically for important intellectual content, and approved the final version.
TSR contributed to the conception and design of the study, performed the statistical analyses, interpreted the data, revised the manuscript critically for important intellectual content, and approved the final version.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kunisaki, K.M., Bohn, O.A., Wetherbee, E.E. et al. High-resolution wrist-worn overnight oximetry has high positive predictive value for obstructive sleep apnea in a sleep study referral population. Sleep Breath 20, 583–587 (2016). https://doi.org/10.1007/s11325-015-1251-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1251-6