Abstract
Purpose
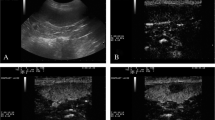
Microwave ablation is used for the treatment of hypersplenism. Image guidance and ablation volume assessment is important to ensure that the ablation is successful. The accuracy of 3D ultrasound (US) and magnetic resonance imaging (MRI) in determining the parameters for microwave ablation were compared in a canine splenomegaly model.
Methods
Microwave ablation of the spleen was performed on 13 dogs with congestive splenomegaly. Several combinations of power output and ablation time were used: 60 W for 300 s, 50 W for 360 s and 40 W for 450 s. The ablation zone volume was measured by 3D US and 3D MRI immediately after microwave ablation, and at 1, 2 and 8 weeks thereafter.
Results
Compared with 3D MRI, the ablation zone reconstruction rate was lower with 3D US (92 vs. 100 %). However, there was no significant difference was found in the ablation volume calculated soon after the treatment and 1 week and 2 months later.
Conclusion
3D US may be useful for quantifying the volume of microwave ablation zones in the spleens of experimental animals and appears promising as an alterative modality to MRI for clinical examinations.




Similar content being viewed by others
References
Runyan BL, Smith RS, Osland JS (2008) Progressive splenomegaly following splenic artery embolization. Am Surg 74(5):437–439
Liu Q, Ma K, He Z, Dong J, Hua X, Huang X, Qiao L (2005) Radiofrequency ablation for hypersplenism in patients with liver cirrhosis: a pilot study. J Gastrointest Surg 9(5):648–657
Hashemieh M, Akhlaghpoor S, Azarkeivan A, Azizahari A, Shirkavand A, Sheibani K (2012) Partial radiofrequency ablation of the spleen in thalassemia. Diagn Interv Radiol 18(4):397–402
Liu QD, Ma KS, He ZP, Ding J, Huang XQ, Dong JH (2003) Experimental study on the feasibility and safety of radiofrequency ablation for secondary splenomagely and hypersplenism. World J Gastroenterol 9(4):813–817
Liang P, Gao Y, Zhang H, Yu X, Wang Y, Duan Y, Shi W (2011) Microwave ablation in the spleen for treatment of secondary hypersplenism: a preliminary study. AJR Am J Roentgenol 196(3):692–696
Xu HX, Lu MD, Xie XY, Yin XY, Kuang M, Chen JW, Xu ZF, Liu GJ (2005) Prognostic factors for long-term outcome after percutaneous thermal ablation for hepatocellular carcinoma: a survival analysis of 137 consecutive patients. Clin Radiol 60(9):1018–1025
Liang P, Dong B, Yu X, Yang Y, Yu D, Su L, Xiao Q, Sheng L (2003) Prognostic factors for percutaneous microwave coagulation therapy of hepatic metastases. AJR Am J Roentgenol 181(5):1319–1325
Ward RC, Healey TT, Dupuy DE (2013) Microwave ablation devices for interventional oncology. Exp Rev Med Devices 10(2):225–238
Lubner MG, Brace CL, Hinshaw JL, Lee FT Jr (2010) Microwave tumor ablation: mechanism of action, clinical results, and devices. J Vasc Interv Radiol 21(8 Suppl):S192–203
Groeschl RT, Pilgrim CH, Hanna EM, Simo KA, Swan RZ, Sindram D, Martinie JB, Iannitti DA, Bloomston M, Schmidt C, Khabiri H, Shirley LA, Martin RC, Tsai S, Turaga KK, Christians KK, Rilling WS, Gamblin TC (2014) Microwave ablation for hepatic malignancies: a multiinstitutional analysis. Ann Surg 259(6):1195–1200
Chiang J, Wang P, Brace CL (2013) Computational modelling of microwave tumour ablations. Int J Hyperth 29(4):308–317
Lubner MG, Brace CL, Ziemlewicz TJ, Hinshaw JL, Lee FT Jr (2013) Microwave ablation of hepatic malignancy. Semin Intervent Radiol 30(1):56–66
Brace CL (2009) Radiofrequency and microwave ablation of the liver, lung, kidney, and bone: what are the differences? Curr Probl Diagn Radiol 38(3):135–143
Liang P, Yu J, Lu MD, Dong BW, Yu XL, Zhou XD, Hu B, Xie MX, Cheng W, He W, Jia JW, Lu GR (2013) Practice guidelines for ultrasound-guided percutaneous microwave ablation for hepatic malignancy. World J Gastroenterol 19(33):5430–5438
Gao Y, Wang Y, Duan Y, Li C, Sun Y, Zhang D, Lu T, Liang P (2010) 915MHz microwave ablation with high output power in in vivo porcine spleens. Eur J Radiol 75(1):87–90
Duan YQ, Gao YY, Ni XX, Wang Y, Feng L, Liang P (2007) Changes in peripheral lymphocyte subsets in patients after partial microwave ablation of the spleen for secondary splenomegaly and hypersplenism: a preliminary study. Int J Hyperth 23(5):467–472
McKeown MJ, Makeig S, Brown GG, Jung TP, Kindermann SS, Bell AJ, Sejnowski TJ (1998) Analysis of fMRI data by blind separation into independent spatial components. Hum Brain Mapp 6(3):160–188
Chang CH, Yu CH, Ko HC, Chen CL, Chang FM (2005) Fetal upper arm volume in predicting intrauterine growth restriction: a three-dimensional ultrasound study. Ultrasound Med Biol 31(11):1435–1439
Leung KY, Ngai CS, Chan BC, Leung WC, Lee CP, Tang MH (2005) Three-dimensional extended imaging: a new display modality for three-dimensional ultrasound examination. Ultrasound Obstet Gynecol 26(3):244–251
Babinszki A, Nyari T, Jordan S, Nasseri A, Mukherjee T, Copperman AB (2001) Three-dimensional measurement of gestational and yolk sac volumes as predictors of pregnancy outcome in the first trimester. Am J Perinatol 18(4):203–211
Landry A, Spence JD, Fenster A (2005) Quantification of carotid plaque volume measurements using 3D ultrasound imaging. Ultrasound Med Biol 31(6):751–762
Bu L, Munns S, Zhang H, Disterhoft M, Dixon M, Stolpen A, Sonka M, Scholz TD, Mahoney LT, Ge S (2005) Rapid full volume data acquisition by real-time 3-dimensional echocardiography for assessment of left ventricular indexes in children: a validation study compared with magnetic resonance imaging. J Am Soc Echocardiogr 18(4):299–305
Ohto M, Kato H, Tsujii H, Maruyama H, Matsutani S, Yamagata H (2005) Vascular flow patterns of hepatic tumors in contrast-enhanced 3-dimensional fusion ultrasonography using plane shift and opacity control modes. J Ultrasound Med 24(1):49–57
Neshat H, Cool DW, Barker K, Gardi L, Kakani N, Fenster A (2013) A 3D ultrasound scanning system for image guided liver interventions. Med Phys 40(11):112903
Zotz RJ, Trabold T, Bock A, Kollmann C (2001) In vitro measurement accuracy of three-dimensional ultrasound. Echocardiography 18(2):149–156
Liang P, Dong B, Yu X, Yu D, Cheng Z, Su L, Peng J, Nan Q, Wang H (2001) Computer-aided dynamic simulation of microwave-induced thermal distribution in coagulation of liver cancer. IEEE Trans Biomed Eng 48(7):821–829
Conflict of interest
None to declare.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by the National Natural Science Foundation of People’s Republic of China (No. 30371367), and the Ministry of Science and Technology of People’s Republic of China (No. 2004BA714B10).
Rights and permissions
About this article
Cite this article
Sheng, L., Li, J., Chen, J. et al. Comparison of 3D ultrasound and magnetic resonance imaging for microwave ablation in the canine splenomegaly model. Int J CARS 10, 459–464 (2015). https://doi.org/10.1007/s11548-014-1095-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-014-1095-8