Abstract
BACKGROUND
Few studies have explored the association between neighborhood characteristics and adherence to diabetes self-management behaviors, and none have examined the influence of neighborhood safety on adherence to treatment regimens among patients with diabetes.
OBJECTIVE
To assess whether neighborhood safety is associated with self-reports of technical quality of care and with nonadherence to diabetes treatment regimens.
DESIGN
A cross-sectional analysis of a population-based sample of California adults responding to the 2007 California Health Interview Survey. Multivariable logistic regression models were used to examine the association of self-reported neighborhood safety with technical quality of care and treatment nonadherence, adjusted for sociodemographic characteristics, barriers to access to care, and health status.
PARTICIPANTS
Adults with type 2 diabetes currently receiving medical treatment.
MAIN MEASURES
Patient-reported neighborhood safety, performance of recommended processes of care by provider, treatment nonadherence (patient delays in filling prescriptions and obtaining needed medical care).
KEY RESULTS
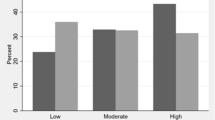
Self-reported neighborhood safety was not associated with process measures of technical quality of care, but was associated with treatment nonadherence. Specifically, compared to those who report living in a safe neighborhood, a higher proportion of patients living in unsafe neighborhoods reported delays in filling a prescription for any reason (21.9% vs. 12.8%, aOR = 1.69, 95%CI 1.19, 2.40) and delays in filling a prescription due to cost (12.2% vs. 6.8%, aOR = 1.63, 95%CI 1.02, 2.62).
CONCLUSIONS
Contextual factors, such as neighborhood safety, may contribute to treatment nonadherence in daily life, even when the technical quality of care delivered in the clinic is not diminished.
Similar content being viewed by others
References
Brown AF, Ettner SL, Piette J, et al. Socioeconomic position and health among persons with diabetes mellitus: a conceptual framework and review of the literature. Epidemiol Rev. 2004;26(1):63–77.
McBean AM, Huang Z, Virnig BA, Lurie N, Musgrave D. Racial variation in the control of diabetes among elderly medicare managed care beneficiaries. Diabetes Care. 2003;26(12):3250–6.
Peek ME, Cargill A, Huang ES. Diabetes health disparities: a systematic review of health care interventions. Med Care Res Rev. 2007;64(5 Suppl):101S–56.
Harris MI. Racial and ethnic differences in health care access and health outcomes for adults with type 2 diabetes. Diabetes Care. 2001;24(3):454–9.
Heisler M, Faul J, Hayward R, Langa K, Blaum C, Weir D. Mechanisms for racial and ethnic disparities in glycemic control in middle-aged and older Americans in the health and retirement study. Arch Intern Med. 2007;167:1853–60.
Brown AF, Ang A, Pebley AR. The relationship between neighborhood characteristics and self-rated health for adults with chronic conditions. Am J Public Health. 2007;97(5):926–32.
Karter AJ, Ferrara A, Liu JY, Moffet HH, Ackerson LM, Selby JV. Ethnic disparities in diabetic complications in an insured population. JAMA. 2002;287(19):2519–27.
Morenoff JD, Lynch JW. What makes a place healthy? Neighborhood influences on racial/ethnic disparities in health over the life course. In: Anderson NB, Bulatao RA, Cohen B, eds. Critical Perspectives on Racial and Ethnic Differences in Health in Late Life. Washington (DC): National Academies Press; 2004.
Moskowitz D, Bodenheimer T. Moving from evidence-based medicine to evidence-based health. J Gen Intern Med. 2011:1–3.
Trinacty C, Adams A, Soumerai S, et al. Racial differences in long-term self-monitoring practice among newly drug-treated diabetes patients in an HMO. J Gen Intern Med. 2007;22:1506–13.
Diez Roux AV, Merkin SS, Arnett D, et al. Neighborhood of residence and incidence of coronary heart disease. N Engl J Med. 2001;345(2):99–106.
Fish JS, Ettner S, Ang A, Brown AF. Association of perceived neighborhood safety on body mass index. Am J Public Health. 2010;100(11):2296–303.
Frank LD, Kerr J, Sallis JF, Miles R, Chapman J. A hierarchy of sociodemographic and environmental correlates of walking and obesity. Prev Med. 2008;47(2):172–8.
Dubowitz T, Heron M, Basurto-Davila R, Bird CE, Lurie N, Escarce JJ. Racial/ethnic differences in US health behaviors: a decomposition analysis. Am J Health Behav. 2011;35(3):290–304.
Nelson K, Taylor L, Lurie N, Escarce J, McFarland L, Fihn SD. Neighborhood environment and health status and mortality among veterans. J Gen Intern Med. 2011.
Odgers CL, Moffitt TE, Tach LM, et al. The protective effects of neighborhood collective efficacy on British children growing up in deprivation: a developmental analysis. Dev Psychol. 2009;45(4):942–57.
Pickett KE, Pearl M. Multilevel analyses of neighbourhood socioeconomic context and health outcomes: a critical review. J Epidemiol Commun Health. 2001;55(2):111–22.
Ross CE, Mirowsky J. Neighborhood disadvantage, disorder, and health. J Health Soc Behav. 2001;42(3):258–76.
Sampson RJ. The neighborhood context of well-being. Perspect Biol Med. 2003;46(3 Suppl):S53–64.
Sampson RJ, Raudenbush SW, Earls F. Neighborhoods and violent crime: a multilevel study of collective efficacy. Science. 1997;277(5328):918–24.
Bennett GG, McNeill LH, Wolin KY, Duncan DT, Puleo E, Emmons KM. Safe to walk? Neighborhood safety and physical activity among public housing residents. PLoS Med. 2007;4(10):e306.
Gary TL, Safford MM, Gerzoff RB, et al. Perception of neighborhood problems, health behaviors, and diabetes outcomes among adults with diabetes in managed care: the Translating Research Into Action for Diabetes (TRIAD) study. Diabetes Care. 2008;31(2):273–8.
Kendzor D, Businelle M, Mazas C, et al. Pathways between socioeconomic status and modifiable risk factors among African American smokers. J Behav Med. 2009;32(6):545–57.
Horowitz CR, Colson KA, Hebert PL, Lancaster K. Barriers to buying healthy foods for people with diabetes: evidence of environmental disparities. Am J Public Health. 2004;94(9):1549–54.
Edwards R, Burns J, McElduff P, Young R, New J. Variations in process and outcomes of diabetes care by socio-economic status in Salford, UK. Diabetologia. 2003;46(6):750–9.
Kelly WF, Mahmood R, Kelly MJ, Turner S, Elliott K. Influence of social deprivation on illness in diabetic patients. BMJ. 1993;307(6912):1115–6.
California Health Interview Survey. CHIS 2007 Methodology Report 1--Sample Design. 2009; Available at: http://www.chis.ucla.edu/methodology.html. Accessed April 15, 2011.
California Health Interview Survey. CHIS 2007 Methodology Report 2--Data Processing Procedures. 2009; Available at: http://www.chis.ucla.edu/methodology.html. Accessed April 15, 2011.
California Health Interview Survey. CHIS 2007 Methodology Report 3--Response Rates. 2009; Available at: http://www.chis.ucla.edu/methodology.html. Accessed April 15, 2011.
National Committee for Quality Assurance. Diabetes Recognition Program. 2009; http://www.ncqa.org/tabid/1023/Default.aspx.
Kessler RC, Andrews G, Colpe LJ, et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol Med. 2002;32:959–76.
Platt A, Field S, Asch D, et al. Neighborhood of residence is associated with daily adherence to CPAP therapy. Sleep. 2009;32(6):799–806.
Steptoe A, Feldman P. Neighborhood problems as sources of chronic stress: development of a measure of neighborhood problems, and associations with socioeconomic status and health. Ann Behav Med. 2001;23(3):177–85.
Taylor SE, Repetti RL, Seeman T. Health psychology: what is an unhealthy environment and how does it get under the skin? Annu Rev Psychol. 1997;48(1):411–47.
Weiner SJ, Schwartz A, Weaver F, et al. Contextual errors and failures in individualizing patient care: a multicenter study. Ann Intern Med. 2010;153(2):69–75.
Haskard-Zolnierek KB, DiMatteo MR. Physician communication and patient adherence to treatment: a meta-analysis. Med Care. 2009:826–834.
Piette JD, Heisler M, Horne R, Caleb AG. A conceptually based approach to understanding chronically ill patients' responses to medication cost pressures. Soc Sci Med. 2006;62(4):846–57.
Greenfield S, Kaplan S, Ware JE Jr. Expanding patient involvement in care. Effects on patient outcomes. Ann Intern Med. 1985;102(4):520–8.
Cramer JS, Sibley RF, Bartlett DP, Kahn LS, Loffredo L. An adaptation of the diabetes prevention program for use with high-risk, minority patients with type 2 diabetes. Diabetes Educ. 2007;33(3):503–8.
Mayer-Davis EJ, D'Antonio AM, Smith SM, et al. Pounds off with empowerment (POWER): a clinical trial of weight management strategies for black and white adults with diabetes who live in medically underserved rural communities. Am J Public Health. 2004;94(10):1736–42.
Piette JD, Heisler M, Krein S, Kerr EA. The role of patient-physician trust in moderating medication nonadherence due to cost pressures. Arch Intern Med. 2005;165(15):1749–55.
Piette JD, Heisler M, Wagner TH. Cost-related medication underuse: do patients with chronic illnesses tell their doctors? Arch Intern Med. 2004;164(16):1749–55.
Norris SL, Lau J, Smith SJ, Schmid CH, Engelgau MM. Self-management education for adults with type 2 diabetes: a meta-analysis of the effect on glycemic control. Diabetes Care. 2002;25(7):1159–71.
DiMatteo M. Variations in patients' adherence to medical recommendations: a quantitative review of 50 years of research. Med Care. 2004;42(3):200–9.
Acknowledgements
This work was supported by the National Institute of Diabetes, Digestive and Kidney Diseases (R18DK69846 and K01DK078939).
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Billimek, J., Sorkin, D.H. Self-reported Neighborhood Safety and Nonadherence to Treatment Regimens Among Patients with Type 2 Diabetes. J GEN INTERN MED 27, 292–296 (2012). https://doi.org/10.1007/s11606-011-1882-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-011-1882-7