Abstract
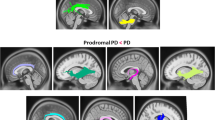
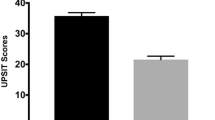
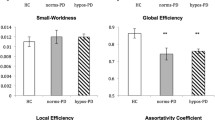
Olfaction dysfunction is considered as a robust marker of prodromal Parkinson disease (PD). Measurement of olfaction function as a screening test is unsatisfactory due to long lead time interval and low specificity for detection of PD. Use of imaging markers might yield more accurate predictive values and provide bases for combined use of imaging and clinical markers for early PD. Diffusion MRI connectometry was conducted on 85 de novo PD patients in and 36 healthy controls to find: first, white matter tracts with significant difference in quantitative anisotropy between PD groups with various degrees of olfaction dysfunction and second, second fibers with correlation with University of Pennsylvania Smell Identification Test (UPSIT) score in each group using a multiple regression analysis considering age, sex, GDS and MoCA score. Local connectomes were determined in seven of all the possible comparisons, correcting for false discovery rate (FDR). PD patients with anosmia and normal olfaction had the highest number of fibers with decreased connectivity in left inferior longitudinal fasciculus, bilateral fornix, bilateral middle cerebellar peduncle (MCP), bilateral cingulum, bilateral corticospinal tract (CST) and body, genu and splenium of corpus callosum (CC) (FDR = 0.0013). In multiple regression analysis, connectivity in the body, genu and splenium of CC and bilateral fornix had significant negative correlation (FDR between 0.019 and 0.083), and bilateral cingulum and MCP had significant positive correlation (FDR between 0.022 and 0.092) with UPSIT score. White matter connectivity in healthy controls could not be predicted by UPSIT score using the same model. The results of this study provide compelling evidence that microstructural degenerative changes in these areas underlie the clinical phenotype of prodromal olfaction dysfunction in PD and that diffusion parameters of these areas might be able to serve as signature markers for early detection of PD. This is the first report that confirms a discriminative role for UPSIT score in identifying PD specific changes in white matter microstructure. Our results open a window to identify microstructural signatures of prodromal PD in white matter.
Similar content being viewed by others
References
Ansari, M., Rahmani, F., Dolatshahi, M., Pooyan, A., & Aarabi, M. H. (2016). Brain pathway differences between Parkinson’s disease patients with and without REM sleep behavior disorder. Sleep & breathing = Schlaf & Atmung.
Berg, D., Marek, K., Ross, G. W., & Poewe, W. (2012). Defining at-risk populations for Parkinson’s disease: lessons from ongoing studies. Movement disorders : Official Journal of the Movement Disorder Society, 27(5), 656 – 65.
Braak, H., Del Tredici, K., Rüb, U., de Vos, R. A., Steur, E. N. J., & Braak, E. (2003). Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiology of Aging, 24(2), 197–211.
Braak, H., Ghebremedhin, E., Rüb, U., Bratzke, H., & Del Tredici, K. (2004). Stages in the development of Parkinson’s disease-related pathology. Cell and Tissue Research, 318(1), 121 – 34.
Del Tredici, K., Rüb, U., de Vos, R. A., Bohl, J. R., & Braak, H. (2002). Where does parkinson disease pathology begin in the brain? Journal of Neuropathology & Experimental Neurology, 61(5), 413 – 26.
Doty, R. (1994). Studies of olfactory dysfunction in major neurological disorders. Advances in the Biosciences, 93, 593–602.
Doty, R. L., Shaman, P., Kimmelman, C. P., & Dann, M. S. (1984). University of Pennsylvania Smell Identification Test: a rapid quantitative olfactory function test for the clinic. The Laryngoscope, 94(2 Pt 1), 176–178.
Fullard, M. E., Tran, B., Xie, S. X., Toledo, J. B., Scordia, C., Linder, C., et al. (2016). Olfactory impairment predicts cognitive decline in early Parkinson’s disease. Parkinsonism & Related Disorders, 25, 45–51.
Haehner, A., Hummel, T., Hummel, C., Sommer, U., Junghanns, S., & Reichmann, H. (2007). Olfactory loss may be a first sign of idiopathic Parkinson’s disease. Movement Disorders: Official Journal of the Movement Disorder Society, 22(6), 839 – 42.
Hall, J. M., Ehgoetz Martens, K. A., Walton, C. C., O’Callaghan, C., Keller, P. E., Lewis, S. J., et al. (2016). Diffusion alterations associated with Parkinson’s disease symptomatology: A review of the literature. Parkinsonism & Related Disorders, 33, 12–26.
Ham, J. H., Lee, J. J., Sunwoo, M. K., Hong, J. Y., Sohn, Y. H., & Lee, P. H. (2016). Effect of olfactory impairment and white matter hyperintensities on cognition in Parkinson’s disease. Parkinsonism & Related Disorders, 24, 95 – 9.
Ibarretxe-Bilbao, N., Junque, C., Marti, M. J., Valldeoriola, F., Vendrell, P., Bargallo, N., et al. (2010). Olfactory impairment in Parkinson’s disease and white matter abnormalities in central olfactory areas: A voxel-based diffusion tensor imaging study. Movement Disorders: Official Journal of the Movement Disorder Society, 25(12), 1888–1894.
Jennings, D., Siderowf, A., Stern, M., Seibyl, J., Eberly, S., Oakes, D., et al. (2014). Imaging prodromal Parkinson disease: The Parkinson Associated Risk Syndrome Study. Neurology, 83(19), 1739–1746.
Jennings, D., Siderowf, A., Stern, M., Seibyl, J., Eberly, S., Oakes, D., et al. (2017). Conversion to Parkinson disease in the PARS Hyposmic and dopamine transporter-deficit prodromal cohort. JAMA Neurology.
Leemans, A., Jeurissen, B., Sijbers, J., & Jones, D. (2009). ExploreDTI: a graphical toolbox for processing, analyzing, and visualizing diffusion MR data. 17th Annual Meeting of International Society for Magnetic Resonance in Medicine. 209:3537.
Luo, C., Song, W., Chen, Q., Yang, J., Gong, Q., & Shang, H. F. (2016). Cortical thinning in drug-naive Parkinson’s disease patients with depression. Journal of Neurology, 263(10), 2114–2119.
Mahlknecht, P., Iranzo, A., Hogl, B., Frauscher, B., Muller, C., Santamaria, J., et al. (2015). Olfactory dysfunction predicts early transition to a Lewy body disease in idiopathic RBD. Neurology, 84(7), 654–658.
Marek, K., Jennings, D., Lasch, S., Siderowf, A., Tanner, C., Simuni, T., et al. (2011). The parkinson progression marker initiative (PPMI). Progress in Neurobiology, 95(4), 629 – 35.
Mole, J. P., Subramanian, L., Bracht, T., Morris, H., Metzler-Baddeley, C., & Linden, D. E. (2016). Increased fractional anisotropy in the motor tracts of Parkinson’s disease suggests compensatory neuroplasticity or selective neurodegeneration. European Radiology, 26(10), 3327–3335.
Munhoz, R. P., Moro, A., Silveira-Moriyama, L., & Teive, H. A. (2015). Non-motor signs in Parkinson’s disease: a review. Arquivos De Neuro-psiquiatria, 73(5), 454 – 62.
Murphy, C., Cain, W. S., Gilmore, M. M., & Skinner, R. B. (1991). Sensory and semantic factors in recognition memory for odors and graphic stimuli: elderly versus young persons. The American Journal of Pssychology. 161–92.
Nigro, S., Riccelli, R., Passamonti, L., Arabia, G., Morelli, M., Nistico, R., et al. (2016). Characterizing structural neural networks in de novo Parkinson disease patients using diffusion tensor imaging. Human Brain Mapping.
Pellicano, C., Benincasa, D., Pisani, V., Buttarelli, F. R., Giovannelli, M., & Pontieri, F. E. (2007). Prodromal non-motor symptoms of Parkinson’s disease. Neuropsychiatric Disease and Treatment, 3(1), 145 – 52.
Postuma, R. B., & Berg, D. (2016). Advances in markers of prodromal Parkinson disease. Nature Reviews Neurology, 12(11), 622 – 34.
Rahmani, F., & Aarabi, M. H. (2017). Does apolipoprotein A1 predict microstructural changes in subgenual cingulum in early Parkinson? Journal of Neurology.
Ressler, K. J., Sullivan, S. L., & Buck, L. B. (1994). Information coding in the olfactory system: evidence for a stereotyped and highly organized epitope map in the olfactory bulb. Cell, 79(7), 1245–1255.
Rodriguez-Violante, M., Gonzalez-Latapi, P., Camacho-Ordonez, A., Martinez-Ramirez, D., Morales-Briceno, H., & Cervantes-Arriaga, A. (2014). Comparing the accuracy of different smell identification tests in Parkinson’s disease: relevance of cultural aspects. Clinical Neurology and Neurosurgery, 123, 9–14.
Ross, G. W., Petrovitch, H., Abbott, R. D., Tanner, C. M., Popper, J., Masaki, K., et al. (2008). Association of olfactory dysfunction with risk for future Parkinson’s disease. Annals of Neurology, 63(2), 167 – 73.
Schapira, A. H. V., Chaudhuri, K. R., & Jenner, P. (2017). Non-motor features of Parkinson disease. Nature Reviews Neuroscience, 18(7), 435 – 50.
Scherfler, C., Schocke, M. F., Seppi, K., Esterhammer, R., Brenneis, C., Jaschke, W., et al. (2006). Voxel-wise analysis of diffusion weighted imaging reveals disruption of the olfactory tract in Parkinson’s disease. Brain: A Journal of Neurology, 129(Pt 2), 538 – 42.
Schmahmann, J. D., Smith, E. E., Eichler, F. S., & Filley, C. M. (2008). Cerebral White Matter: Neuroanatomy, Clinical Neurology, and Neurobehavioral Correlates. Annals of the New York Academy of Sciences, 1142, 266–309.
Tessa, C., Lucetti, C., Giannelli, M., Diciotti, S., Poletti, M., Danti, S., et al. (2014). Progression of brain atrophy in the early stages of Parkinson’s disease: a longitudinal tensor-based morphometry study in de novo patients without cognitive impairment. Human Brain Mapping, 35(8), 3932–3944.
The Parkinson Progression Marker Initiative (PPMI). (2011). Progress in Neurobiology.95(4):629 – 35.
Visanji, N., & Marras, C. (2015). The relevance of pre-motor symptoms in Parkinson’s disease. Expert review of Neurotherapeutics, 15(10), 1205–1217.
Wang, J., You, H., Liu, J.-F., Ni, D.-F., Zhang, Z.-X., & Guan, J. (2011). Association of Olfactory Bulb Volume and Olfactory Sulcus Depth with Olfactory Function in Patients with Parkinson Disease. American Journal of Neuroradiology, 32(4), 677 – 81.
Wilson, R. S., Yu, L., Schneider, J. A., Arnold, S. E., Buchman, A. S., & Bennett, D. A. (2011). Lewy Bodies and Olfactory Dysfunction in Old Age. Chemical Senses, 36(4), 367 – 73.
Wiltshire, K., Concha, L., Gee, M., Bouchard, T., Beaulieu, C., & Camicioli, R. (2010). Corpus callosum and cingulum tractography in Parkinson’s disease. The Canadian Journal of Neurological Sciences Le Journal Canadien des Sciences Neurologiques, 37(5), 595–600.
Yeh, F. C., Badre, D., Verstynen, T. (2015). Connectometry: A statistical approach harnessing the analytical potential of the local connectome. NeuroImage.
Yeh, F. C., & Tseng, W. Y. (2011). NTU-90: a high angular resolution brain atlas constructed by q-space diffeomorphic reconstruction. NeuroImage, 58(1), 91 – 9.
Yeh, F.-C., Tang, P.-F., & Tseng, W.-Y.I. (2013). Diffusion MRI connectometry automatically reveals affected fiber pathways in individuals with chronic stroke. NeuroImage: Clinical, 2, 912 – 21.
Yeh, F.-C., Verstynen, T. D., Wang, Y., Fernández-Miranda, J. C., & Tseng, W.-Y.I. (2013). Deterministic Diffusion Fiber Tracking Improved by Quantitative Anisotropy. PloS One, 8(11), e80713.
Zhang, Y., Wu, I. W., Tosun, D., Foster, E., & Schuff, N. (2016). Progression of Regional Microstructural Degeneration in Parkinson’s Disease: A Multicenter Diffusion Tensor Imaging Study. PloS One, 11(10), e0165540.
Acknowledgements
The database of this work was funded by grants from the Michael J Fox Foundation for Parkinson’s Research, the W Garfield Weston Foundation, and the Alzheimer’s Association, the Canadian Institutes for Health Research, and the Natural Sciences and Engineering Research Council of Canada. We thank Christian Beckmann and Simon Eickhoff for their advice on data analysis. Data used in this article were obtained from the Parkinson Progression Markers Initiative (PPMI) database (www.ppmi-info.org/data). For up-to-date information on the study, visit www.ppmi-info.org. PPMI is sponsored and partially funded by the Michael J Fox Foundation for Parkinson Research and funding partners, including AbbVie, Avid Radiopharmaceuticals, Biogen, Bristol-Myers Squibb, Covance, GE Healthcare, Genentech, GlaxoSmithKline (GSK), Eli Lilly and Company, Lundbeck, Merck, Meso Scale Discovery (MSD), Pfizer, Piramal Imaging, Roche, Servier, and UCB (www.ppmi-info.org/fundingpartners).
Authors’ Contribution statements
All the authors agreed on the current list of authors as it appears on the first page. Soheila Sobhani, Farzaneh Rahmani and Mohammad Hadi Aarabi contributed equally to this paper as first authors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest, nor have they received any funding from any organization or granting bodies which might pose any conflict of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study, by the Parkinson’s Disease Progression Marker Initiative (PPMI).
Electronic supplementary material
Below is the link to the electronic supplementary material.



Rights and permissions
About this article
Cite this article
Sobhani, S., Rahmani, F., Aarabi, M.H. et al. Exploring white matter microstructure and olfaction dysfunction in early parkinson disease: diffusion MRI reveals new insight. Brain Imaging and Behavior 13, 210–219 (2019). https://doi.org/10.1007/s11682-017-9781-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-017-9781-0