Abstract
Background
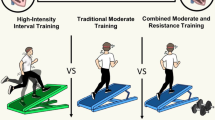
Exercise training improves exercise capacity (peakVO2), which is closely related to long-term survival in cardiac patients. However, it remains unclear which type and intensity of exercise is most effective for improving exercise tolerance and body weight. Individual studies suggest that aerobic interval training (AIT) might increase peakVO2 more in this population.
Objective
We conducted a meta-analysis to summarize the effects of AIT compared with moderate continuous training (MCT) on peakVO2, submaximal exercise capacity, and body weight in patients with coronary artery disease (CAD) with preserved and/or reduced left ventricular ejection fraction (LVEF).
Data sources and study selection
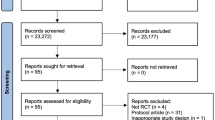
A systematic search was conducted and we included randomized trials comparing AIT and MCT in CAD patients lasting at least 4 weeks, reporting peakVO2 results, and published in a peer-reviewed journal up to May 2013. The primary outcome measure was peakVO2. Secondary outcomes were submaximal exercise capacity parameters and body weight.
Synthesis methods
Random- and fixed-effects models were used and data were reported as weighted means and 95 % confidence intervals (CIs).
Results
Nine study groups were included, involving 206 patients (100 AIT, 106 MCT). Overall, AIT resulted in a significantly larger increase in peakVO2 [+1.60 mL/kg/min (95 % CI 0.18–3.02; p = 0.03)] compared with MCT. MCT seemed to be more effective in reducing body weight (−0.78 kg; 95 % CI −0.01 to 1.58; p = 0.05).
Limitations
The small number of studies might have affected the power to reach significance for the secondary outcomes.
Conclusion
In CAD patients with preserved and/or reduced LVEF, AIT is superior to MCT for improving peakVO2, while MCT seems to be more effective in reducing body weight. However, large, well-designed, randomized controlled trials are warranted to confirm these findings.






Similar content being viewed by others
References
Nichols M, Townsend N, Scarborough P, et al. European cardiovascular disease statistics: Edition 2012. http://www.ehnheart.org/cvd-statistics/cvd-statistics-2012.html. Accessed 1 Nov 2012.
Taylor RS, Brown A, Ebrahim S, et al. Exercise-based rehabilitation for patients with coronary heart disease: systematic review and meta-analysis of randomized controlled trials. Am J Med. 2004;116(10):682–92.
Vanhees L, Fagard R, Thijs L, et al. Prognostic significance of peak exercise capacity in patients with coronary artery disease. J Am Coll Cardiol. 1994;23(2):358–63.
Myers J, Prakash M, Froelicher V, et al. Exercise capacity and mortality among men referred for exercise testing. N Engl J Med. 2002;346(11):793–801.
Shephard CW, While AE. Cardiac rehabilitation and quality of life: a systematic review. Int J Nurs Stud. 2012;49(6):755–71.
Oldridge N. Exercise-based cardiac rehabilitation in patients with coronary heart disease: meta-analysis outcomes revisited. Future Cardiol. 2012;8(5):729–51.
Cornelissen VA, Fagard RH. Effects of endurance training on blood pressure, blood pressure-regulating mechanisms, and cardiovascular risk factors. Hypertension. 2005;46(4):667–75.
Vanhees L, Rauch B, Piepoli M, on behalf of the writing group of the EACPR, et al. Importance of characteristics and modalities of physical activity and exercise in the management of cardiovascular health in individuals with cardiovascular disease (part III). Eur J Prev Cardiol. 2012;19(6):1333–56.
Vanhees L, Stevens A, Schepers D, et al. Determinants of the effects of physical training and of the complications requiring resuscitation during exercise in patients with cardiovascular disease. Eur J Cardiovasc Prev Rehabil. 2004;11(4):304–12.
Rankin AJ, Rankin AC, MacIntyre P, et al. Walk or run? Is high-intensity exercise more effective than moderate-intensity exercise at reducing cardiovascular risk? Scott Med J. 2012;57(2):99–102.
Arena R, Myers J, Forman DE, et al. Should high-intensity-aerobic interval training become the clinical standard in heart failure. Heart Fail Rev. 2013;18(1):95–105.
Cornish AK, Broadbent S, Cheema BS. Interval training for patients with coronary artery disease: a systematic review. Eur J Appl Physiol. 2011;111(4):579–89.
O’Donovan G, Owen A, Bird SR, et al. Changes in cardiorespiratory fitness and coronary heart disease risk factors following 24 wk of moderate- or high-intensity exercise of equal energy cost. J Appl Physiol. 2005;98(5):1619–25.
Guiraud T, Nigam A, Gremeaux V, et al. High-intensity interval training in cardiac rehabilitation. Sports Med. 2012;42(7):587–605.
Wisløff U, Støylen A, Loennechen JP, et al. Superior cardiovascular effect of aerobic interval training versus moderate continuous training in heart failure patients: a randomized study. Circulation. 2007;115(24):3086–94.
Smart NA, Dieberg G, Giallauria F. Intermittent versus continuous exercise training in chronic heart failure: a meta-analysis. Int J Cardiol. 2013;166(2):352–8.
Haykowsky MJ, Timmons MP, Kruger C, et al. Meta-analysis of aerobic interval training on exercise capacity and systolic function in patients with heart failure and reduced ejection fractions. Am J Cardiol. 2013;111(10):1466–9.
Rognmo Ø, Hetland E, Helgerud J, et al. High intensity aerobic interval exercise is superior to moderate intensity exercise for increasing aerobic capacity in patients with coronary artery disease. Eur J Cardiovasc Prev Rehabil. 2004;11(3):216–22.
Warburton DE, McKenzie DC, Haykowsky MJ, et al. Effectiveness of high-intensity interval training for the rehabilitation of patients with coronary artery disease. Am J Cardiol. 2005;95(9):1080–4.
Rocco EA, Prado DM, Silva AG, et al. Effect of continuous and interval exercise training on the PETCO2 response during a graded exercise test in patients with coronary artery disease. Clinics. 2012;67(6):623–7.
Moholdt TT, Amundsen BH, Rustad LA, et al. Aerobic interval training versus continuous moderate exercise after coronary artery bypass surgery: a randomized study of cardiovascular effects and quality of life. Am Heart J. 2009;158(6):1031–7.
Dimopoulos S, Anastatiou-Nana M, Sakellariou D, et al. Effects of exercise rehabilitation program on heart rate recovery in patients with chronic heart failure. Eur J Cardiovasc Prev Rehabil. 2006;13(1):67–73.
Vanhees L, Geladas N, Hansen D, on behalf of the writing group of the EACPR, et al. Importance of characteristics and modalities of physical activity and exercise in the management of cardiovascular health in individuals with cardiovascular risk factors: recommendations from the EACPR (part II). Eur J Prev Cardiol. 2012;19(5):1005–33.
The George Institute for Global Health and the University of Sydney. Physiotherapy Evidence Database; 2012. http://www.pedro.org.au/english/downloads/pedro-scale/. Accessed 18 Oct 2012.
De Morton NA. The PEDro scale is a valid measure of the methodological quality of clinical trials: a demographic study. Aust J Physiother. 2009;55(2):129–33.
Maher CG, Sherrington C, Herbert RD, et al. Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys Ther. 2003;83(8):713–21.
Follman D, Elliott P, Suh I, et al. Variance imputation for overviews of clinical trials with continuous response. Clin Epidemiol. 1992;45(7):769–73.
Moholdt T, Aamot IL, Granøien I, et al. Aerobic interval training increases peak oxygen uptake more than usual care exercise training in myocardial infarction patients: a randomized controlled study. Clin Rehabil. 2012;26(1):33–44.
Dersimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177–88.
Hunter JE, Schmidt FL. Fixed effects vs. random effects meta-analysis models: implications for cumulative research knowledge. Int J Sel Assess. 2000;8(4):275–92.
Roditis P, Dimopoulos S, Sakellariou D, et al. The effects of exercise training on the kinetics of oxygen uptake in patients with chronic heart failure. Eur J Cardiovasc Prev Rehabil. 2007;14(2):304–11.
Amundsen BH, Rognmo Ø, Hatlen-Rebhan G, et al. High-intensity aerobic exercise improves diastolic function in coronary artery disease. Scand Cardiovasc J. 2008;42(2):110–7.
Fu TC, Wang CH, Lin PS, et al. Aerobic interval training improves oxygen uptake efficiency by enhancing cerebral and muscular hemodynamics in patients with heart failure. Int J Cardiol. 2013;167(1):41–50.
Iellamo F, Manzi V, Caminiti G, et al. Dose–response relationship of baroreflex sensitivity and heart rate variability to individually-tailored exercise training in patients with heart failure. Int J Cardiol. 2013;166(2):334–9.
Freyssin C, Verkindt C, Prieur F, et al. Cardiac rehabilitation in chronic heart failure: effect of an 8-week, high intensity interval training versus continuous training. Arch Phys Med Rehabil. 2012;93(8):1359–64.
Iellamo F, Manzi V, Caminiti G, et al. Matched dose interval and continuous exercise training induce similar cardiorespiratory and metabolic adaptations in patients with heart failure. Int J Cardiol. 2013;167(6):2561–5.
Moholdt T, Aamot IL, Granøien I, et al. Long-term follow-up after cardiac rehabilitation: a randomized study of usual care exercise training versus aerobic interval training after myocardial infarction. Int J Cardiol. 2011;152(3):388–90.
Smart NA, Steele M. A comparison of 16 weeks of continuous vs intermittent exercise training in chronic heart failure patients. Congest Heart Fail. 2012;18(4):205–11.
Currie KD, Dubberley JB, McKelvie RS, et al. Low-volume, high-intensity interval training in patients with coronary artery disease. Med Sci Sports Exerc. 2013;45(8):1436–42.
Fletcher GF, Balady GJ, Amsterdam EA, et al. Exercise standards for testing and training: a statement for healthcare professionals from the American Heart Association. Circulation. 2001;104(14):1694–740.
Mezzani A, Agostoni P, Cohen-Solal A, et al. Standards for the use of cardiopulmonary exercise testing for the functional evaluation of cardiac patients: a report from the Exercise Physiology Section of the European Association for Cardiovascular Prevention and Rehabilitation. Eur J Cardiovasc Prev Rehabil. 2009;16(3):249–67.
Keteyian SJ, Brawner CA, Savage PD, et al. Peak aerobic capacity predicts prognosis in patients with coronary heart disease. Am Heart J. 2008;156(2):292–300.
Hwang CL, Wu YT, Chou CH. Effect of aerobic interval training on exercise capacity and metabolic risk factors in people with cardiometabolic disorders: a meta-analysis. J Cardiopulm Rehabil Prev. 2011;31(6):378–85.
Tomczak CR, Thompson RB, Paterson I, et al. Effect of acute high-intensity interval exercise on postexercise biventricular function in mild heart failure. J Appl Physiol. 2011;110(2):398–406.
Nechwatal RM, Duck C, Gruber G. Physical training as interval or continuous training in chronic heart failure for improving functional capacity, hemodynamics and quality of life: a controlled study. Z Kardiol. 2002;91(4):328–37.
Tjønna AE, Lee SJ, Rognmo Ø, et al. Aerobic interval training versus continuous moderate exercise as a treatment for the metabolic syndrome: a pilot study. Circulation. 2008;118(4):346–54.
Guazzi M, Vitelli A, Arena R. The effect of exercise training on plasma NT-pro-BNP levels and its correlation with improved exercise ventilator efficiency in patients with heart failure. Int J Cardiol. 2012;158(2):290–1.
Van de Veire NR, Van Laethem C, Philippé J, et al. VE/VCO2 slope and oxygen uptake efficiency slope in patients with coronary artery disease and intermediate peakVO2. Eur J Cardiovasc Prev Rehabil. 2006;13(6):916–23.
Sarullo FM, Fazio G, Brusca I, et al. Cardiopulmonary exercise testing in patients with chronic heart failure: prognostic comparison from peak VO2 and VE/VCO2 slope. Open Cardiovasc Med J. 2010;26(4):127–34.
Cahalin LP, Chase P, Arena R, et al. A meta-analysis of the prognostic significance of cardiopulmonary exercise testing in patients with heart failure. Heart Fail Rev. 2013;18(1):79–94.
Guazzi M, Adams V, Conraads V, et al. EACPR/AHA Scientific Statement: clinical recommendations for cardiopulmonary exercise testing data assessment in specific patient populations. Eur Heart J. 2012;33(12):2917–27.
Hansen D, Dendale P, van Loon LJ, Meeusen R. The impact of training modalities on the clinical benefits of exercise intervention in patients with cardiovascular disease or type 2 diabetes mellitus. Sports Med. 2010;40(11):921–40.
Thompson PD, Franklin BA, Balady GJ, et al. Exercise and acute cardiovascular events placing the risks into perspective: a scientific statement from the American Heart Association Council on Nutrition, Physical Activity, and Metabolism and the Council on Clinical Cardiology. Circulation. 2007;115(17):2358–68.
Rognmo Ø, Moholdt T, Bakken H, et al. Cardiovascular risk of high- versus moderate intensity aerobic exercise in coronary heart disease patients. Circulation. 2012;126(12):1436–40.
Fagard RH, Staessen JA, Thijs L. Advantages and disadvantages of the meta-analysis approach. J Hypertens Suppl. 1996;14(2):S9–12.
Acknowledgments
L.V. is the holder of the faculty chair ‘Lifestyle and Health’ at the University of Applied Sciences, Utrecht, the Netherlands. V.A.C. is supported as a postdoctoral fellow by Research Foundation Flanders (FWO). However, no specific sources of funding were used to assist in the preparation of this review.
The authors have no potential conflicts of interest that are directly relevant to the content of this review. All authors also take responsibility for all aspects of the reliability and freedom from bias of the data presented and their discussed interpretation.
The abstract of this manuscript was accepted for oral presentation at the Congress of the European Society of Hypertension (ESH; Milan, 14–18 June 2013) and at the Congress of the European Society of Cardiology (ESC; Amsterdam, 31 August–4 September 2013).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
N. Pattyn and E. Coeckelberghs contributed equally.
Rights and permissions
About this article
Cite this article
Pattyn, N., Coeckelberghs, E., Buys, R. et al. Aerobic Interval Training vs. Moderate Continuous Training in Coronary Artery Disease Patients: A Systematic Review and Meta-Analysis. Sports Med 44, 687–700 (2014). https://doi.org/10.1007/s40279-014-0158-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-014-0158-x