Abstract
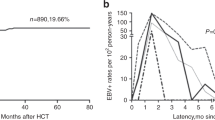
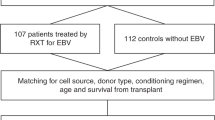
We monitored 133 high-risk allo-SCT recipients for 6 months after transplant for EBV reactivation by quantitative real-time PCR. Rituximab was given as pre-emptive therapy for viremia >1000 copies/mL. The 1-year cumulative incidence of EBV reactivation was 29.4% (95% confidence interval (CI): 18–40) in patients monitored due to initial high-risk characteristics (n=93) and 31.8% (95% CI: 19.7–44) in those followed because of the development of refractory GVHD (n=40). Overall response rate to Rituximab was 83%. Nine patients (9.6%) developed post-transplant lymphoproliferative disorder (PTLD) at a median of +62 days after SCT. Eight of them showed a concomitant CMV reactivation. Second SCT was the only risk factor associated with EBV infection and PTLD in multivariate analysis (hazard ratio (HR) 2.6 (95% CI: 1.1–6.4; P=0.04) and HR 6.4 (95%CI: 1.3–32; P=0.02)). The development of EBV reactivation was not associated with non-relapse mortality or OS (P=0.97 and P=0.84, respectively).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Curtis RE, Travis LB, Rowlings PA, Socié G, Kingma DW, Banks PM et al. Risk of lymphoproliferative disorders after bone marrow transplantation: a multiinstitutional study. Blood 1999; 94: 2208–2216.
Landgren O, Gilbert ES, Rizzo JD, Socié G, Banks PM, Sobocinski KA et al. Risk factors for lymphoproliferative disorders after allogeneic hematopoietic cell transplantation. Blood 2009; 113: 4992–5001.
Reddy N, Rezvani K, Barrett AJ, Savani BN . Strategies to prevent EBV reactivation and posttransplant lymphoproliferative disorders after allogeneic stem cell transplantation in high-risk patients. Biol Blood Marrow Transplant 2011; 17: 591–597.
Styczynski J, Reusser P, Einsele H, de la Camara R, Cordonnier C, Ward KN et al. Management of HSV, VZV and EBV infections in patients with hematological malignancies and after SCT: guidelines from the Second European Conference on Infections in Leukemia. Bone Marrow Transplant 2009; 43: 757–770.
Blaes AH, Cao Q, Wagner JE, Young JA, Weisdorf DJ, Brunstein CG et al. Monitoring and preemptive rituximab therapy for Epstein-Barr virus reactivation after antithymocyte globulin containing nonmyeloablative conditioning for umbilical cord blood transplantation. Biol Blood Marrow Transplant 2010; 16: 287–291.
Styczynski J, Gil L, Tridello G, Ljungman P, Donnelly JP, van der Velden W et al. Response to rituximab-based therapy and risk factor analysis in epstein barr virus-related lymphoproliferative disorder after hematopoietic stem cell transplant in children and adults: a study from the Infectious Diseases Working Party of the European Group for Blood and Marrow Transplantation. Clin Infect Dis 2013; 57: 794–802.
Coppoletta S, Tedone E, Galano B, Soracco M, Raiola AM, Lamparelli T et al. Rituximab treatment for Epstein-Barr virus DNAemia after alternative-donor hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2011; 17: 901–907.
Sanz J, Boluda JC, Martín C, González M, Ferrá C, Serrano D et al. Single-unit umbilical cord blood transplantation from unrelated donors in patients with hematological malignancy using busulfan, thiotepa, fludarabine and ATG as myeloablative conditioning regimen. Bone Marrow Transplant 2012; 47: 1287–1293.
Piñana JL, Martino R, Barba P, Margall N, Roig MC, Valcárcel D et al. Cytomegalovirus infection and disease after reduced intensity conditioning allogeneic stem ce ll transplantation: single-center experience. Bone Marrow Transplant 2010; 45: 534–542.
Martino R, Subirà M . Invasive fungal infections in hematology: new trends. Ann Hematol 2002; 81: 233–243.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J et al. 1994 Consensus Conference on Acute GVHD Grading. Bone Marrow Transplant 1995; 15: 825.
Martin PJ, Rizzo JD, Wingard JR, Ballen K, Curtin PT, Cutler C et al. First- and second-line systemic treatment of acute graft-versus-host disease: recommendations of the American Society of Blood and Marrow Transplantation. Biol Blood Marrow Transplant 2012; 18: 1150–1163.
Cheson BD, Pfistner B, Juweid ME, Gascoyne RD, Specht L, Horning SJ et al. Revised response criteria for malignant lymphoma. J Clin Oncol 2007; 25: 579–586.
Klein JP, Rizzo JD, Zhang MJ, Keiding N . Statistical methods for the analysis and presentation of the results of bone marrow transplants. Part I: unadjusted analysis. Bone Marrow Transplant 2001; 28: 909–915.
Klein JP, Rizzo JD, Zhang MJ, Keiding N . Statistical methods for the analysis and presentation of the results of bone marrow transplants. Part 2: Regression modeling. Bone Marrow Transplant 2001; 28: 1001–1011.
Kaplan EL, Meier P . Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958; 53: 457–481.
Zallio F, Primon V, Tamiazzo S, Pini M, Baraldi A, Corsetti MT et al. Epstein-Barr virus reactivation in allogeneic stem cell transplantation is highly related to cytomegalovirus reactivation. Clin Transplant 2013; 27: E491–E497.
van der Velden WJ, Mori T, Stevens WB, de Haan AF, Stelma FF, Blijlevens NM et al. Reduced PTLD-related mortality in patients experiencing EBV infection following allo-SCT after the introduction of a protocol incorporating pre-emptive rituximab. Bone Marrow Transplant 2013; 48: 1465–1471.
Hoegh-Petersen M, Goodyear D, Geddes MN, Liu S, Ugarte-Torres A, Liu Y et al. High incidence of post transplant lymphoproliferative disorder after antithymocyte globulin-based conditioning and ineffective prediction by day 28 EBV-specific T lymphocyte counts. Bone Marrow Transplant 2011; 46: 1104–1112.
Fox CP, Burns D, Parker AN, Peggs KS, Harvey CM, Natarajan S et al. EBV-associated post-transplant lymphoproliferative disorder following in vivo T-cell-depleted allogeneic transplantation: clinical features, viral load correlates and prognostic factors in the rituximab era. Bone Marrow Transplant 2014; 49: 280–286.
Majewski M, Korecka M, Joergensen J, Fields L, Kossev P, Schuler W et al. Immunosuppressive TOR kinase inhibitor everolimus (RAD) suppresses growth of cells derived from posttransplant lymphoproliferative disorder at allograft-protecting doses. Transplantation 2003; 75: 1710–1717.
Patriarca F, Medeot M, Isola M, Battista ML, Sperotto A, Pipan C et al. Prognostic factors and outcome of Epstein-Barr virus DNAemia in high-risk recipients of allogeneic stem cell transplantation treated with preemptive rituximab. Transpl Infect Dis 2013; 15: 259–267.
Heslop HE . How I treat EBV lymphoproliferation. Blood 2009; 114: 4002–4008.
Worth A, Conyers R, Cohen J, Jagani M, Chiesa R, Rao K et al. Pre-emptive rituximab based on viraemia and T cell reconstituion: a highly effective strategy for the prevention of EBV-associated lymphoproliferative following stem cell transplantation. Br J Haematol 2011; 155: 377–385.
Uhlin M, Wikell H, Sundin M, Blennow O, Maeurer M, Ringden O et al. Risk factors for EBV related post-trasplant lymphoproliferative disease after allogeneic stem cell transplantation. Haematologica 2014; 99: 346–352.
Petropoulou A, Porcher R, Peffault R, Xhaard A, Weisdorf D, Ribaud P et al. Increased infection rate after preemptive rituximab treatment for epstein-barr virus reactivation after allogeneic stem cell transplantation. Transplantation 2012; 94: 879–883.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Bone Marrow Transplantation website
Supplementary information
Rights and permissions
About this article
Cite this article
García-Cadenas, I., Castillo, N., Martino, R. et al. Impact of Epstein Barr virus-related complications after high-risk allo-SCT in the era of pre-emptive rituximab. Bone Marrow Transplant 50, 579–584 (2015). https://doi.org/10.1038/bmt.2014.298
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2014.298
This article is cited by
-
Rituximab for posttransplant lymphoproliferative disorder – therapeutic, preemptive, or prophylactic?
Bone Marrow Transplantation (2024)
-
Post-transplantation lymphoproliferative disorder after haematopoietic stem cell transplantation
Annals of Hematology (2021)
-
Pre-emptive rituximab treatment for Epstein–Barr virus reactivation after allogeneic hematopoietic stem cell transplantation is a worthwhile strategy in high-risk recipients: a comparative study for immune recovery and clinical outcomes
Bone Marrow Transplantation (2020)
-
Epstein–Barr virus reactivation after allogeneic hematopoietic stem cell transplantation: multifactorial impact on transplant outcomes
Bone Marrow Transplantation (2020)
-
A retrospective analysis on anti-CD20 antibody–treated Epstein–Barr virus–related posttransplantation lymphoproliferative disorder following ATG-based haploidentical T-replete hematopoietic stem cell transplantation
Annals of Hematology (2020)