Abstract
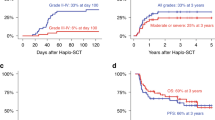
Emerging data demonstrate promising results of related haploidentical allogeneic hematopoietic stem cell transplantation (haplo-HCT) for the treatment of hematologic malignancies. Data about G-CSF primed PBSC as reliable source of graft with myeloablative conditioning are lacking. We updated the outcomes in 130 adult patients with high-risk hematologic malignancies who received haplo-PBSC transplantation consecutively under busulfan-based conditioning. PBSC were freshly isolated and infused without ex vivo T-cell depletion into the recipients. Myeloid recovery was achieved in 99.2% patients with full donor chimerism. The cumulative incidence of acute grade 3–4 GvHD, overall and extensive chronic GvHD was 14.9%, 38.6% and 16.5%, respectively. The 3-year non-relapse mortality rate was 24.1%. Non-remission prior to transplant was associated with higher incidence of relapse (P=0.006), inferior overall survival (P=0.017) and leukemia-free survival (P=0.024). These data suggest that PBSC is a reliable graft source in haploidentical, unmanipulated transplant settings under myeloablative conditioning in patients with high-risk hematologic malignancies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Aversa F, Terenzi A, Tabilio A, Falzetti F, Carotti A, Ballanti S et al. Full haplotype-mismatched hematopoietic stem-cell transplantation: a phase II study in patients with acute leukemia at high risk of relapse. J Clin Oncol 2005; 23: 3447–3454.
Federmann B, Bornhauser M, Meisner C, Kordelas L, Beelen DW, Stuhler G et al. Haploidentical allogeneic hematopoietic cell transplantation in adults using CD3/CD19 depletion and reduced intensity conditioning: a phase II study. Haematologica 2012; 97: 1523–1531.
Wang Y, Liu DH, Liu KY, Xu LP, Zhang XH, Han W et al. Long-term follow-up of haploidentical hematopoietic stem cell transplantation without in-vitro T-cell-depletion for the treatment of leukemia: nine years of experience at a single center. Cancer 2013; 119: 978–985.
Luznik L, O'Donnell PV, Symons HJ, Chen AR, Leffell MS, Zahurak M et al. HLA-haploidentical bone marrow transplantation for hematologic malignancies using nonmyeloablative conditioning and high-dose, posttransplantation cyclophosphamide. Biol Blood Marrow Transplant 2008; 14: 641–650.
Powles R, Mehta J, Kulkarni S, Treleaven J, Millar B, Marsden J et al. Allogeneic blood and bone marrow stem cell transplantation in haematological malignant diseases: a randomized trial. Lancet 2000; 355: 1231–1237.
Schmitz N, Beksac M, Bacigalupo A, Ruutu T, Nagler A, Gluckman E et al. Filgrastim-mobilized peripheral blood progenitor cells versus bone marrow transplantation for treating leukemia: 3-year results from the EBMT randomized trial. Haematologica 2005; 90: 643–648.
Mohty M, Kuentz M, Michallet M, Bourhis JH, Milpied N, Sutton L et al. Chronic graft-versus-host disease after allogeneic blood stem cell transplantation: long-term results of a randomized study. Blood 2002; 100: 3128–3134.
Meisel R, Klingebiel T, Dilloo D . Peripheral blood stem cells versus bone marrow in pediatric unrelated donor stem cell transplantation. Blood 2013; 121: 863–865.
Di Bartolomeo P, Santarone S, De Angelis G, Picardi A, Cudillo L, Cerretti R et al. Haploidentical, unmanipulated, G-CSF-primed bone marrow transplantation for patients with high-risk hematologic malignancies. Blood 2013; 121: 849–857.
Xu LP, Liu KY, Liu DH, Chen H, Han W, Chen YH et al. The inferiority of G-PB to rhG-CSF-mobilized blood and marrow grafts as a stem cell source in patients with high-risk acute leukemia who underwent unmanipulated HLA-mismatched/ haploidentical transplantation: a comparative analysis. Bone Marrow Transplant 2010; 45: 985–992.
Wenrong H, Honghua L, Gao C, Bo J, Wang Q, Yu Z et al. Unmanipulated HLA-mismatched/ haploidentical peripheral blood stem cell transplantation for high-risk hematologic malignancies. Transfusion 2012; 52: 1354–1362.
Luo Y, Hanwen X, Lai X, Shi J, Tan Y, Jingsong H et al. T-cell-replete haploidentical HSCT with low-dose anti-T-lymphocyte globulin compared with matched sibling HSCT and unrelated HSCT. Blood 2014; 124: 2735–2743.
Lu DP, Dong L, Wu T, Huang XJ, Zhang MJ, Han W et al. Conditioning including antithymocyte globulin followed by unmanipulated HLA mismatched/haploidentical blood and marrow transplantation can achieve comparable outcomes with HLA-identical sibling transplantation. Blood 2006; 107: 3065–3073.
Rowlings PA, Przepiorka D, Klein JP, GaLE RP, Passweg JR, henslee-Downey PJ et al. IBMTR Severity Index for grading acute graft-versus-host disease: retrospective comparison with Glucksberg grade. Br J Haematol 1997; 97: 855–864.
Castagna L, Crocchiolo R, Furst S, Bramanti S, EI Cheikh J, Sarina B et al. Bone marrow compared with peripheral blood stem cells for haploidentical transplantation with a nonmyeloablative conditioning regimen and post-transplantation cyclophosphamide. Biol Blood Marrow Transplant 2014; 20: 724–729.
Raj K, Pagliuca A, Bradstock K, Noriega V, Potter V, Streetly M et al. Peripheral blood hematopoietic stem cells for transplantation of hematological diseases from related, haploidentical donors after reduced-intensity conditioning. Biol Blood Marrow Transplant 2014; 20: 890–895.
Solomon SR, Sizemore CA, Sanacore M, Zhang X, Brown S, Holland HK et al. Haploidentical transplantation using T cell replete peripheral blood stem cells and myeloablative conditioning in patients with high-risk hematologic malignancies who lack conventional donors is well tolerated and produces excellent relapse-free survival: results of a prospective phase II trial. Biol Blood Marrow transplant 2012; 18: 1859–1866.
Chang YJ, Xu LP, Liu DH, Liu KY, Han W, Chen YH et al. Platelet engraftment in patients with hematologic malignancies following unmanipulated haploidentical blood and marrow transplantation: effects of CD34+ cell dose and disease status. Biol Blood Marrow Transplant 2009; 15: 632–638.
Kong Y, Hu Y, Zhang XH, Wang YZ, Mo XD, Zhang YY et al. Association between an impaired bone marrow vascular microenvironment and prolonged isolated thrombocytopenia after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2014; 20: 1190–1197.
Wang Y, Chang YJ, Xu LP, Liu KY, Liu DH, Zhang XH et al. Who is the best donor for a related HLA haplotype-mismatched transplant? Blood 2014; 124: 843–850.
Friedrichs B, Tichelli A, Bacigalupo A, Russell NH, Ruutu T, Shapira MY et al. Long-term outcome and late effects in patients transplanted with mobilized blood or bone marrow: a randomized trial. Lancet Oncol 2010; 11: 331–338.
Anasetti C, Logan BR, Lee SJ, Waller EK, Weisdorf DJ, Wingard JR et al. Peripheral-blood stem cells versus bone marrow from unrelated donors. N Engl J Med 2012; 367: 1487–1496.
Wang Y, Liu DH, Xu LP, Liu KY, Chen H, Zhang XH et al. Prevention of relapse using granulocyte CSF-primed PBPCs following HLA-mismatched/haploidentical, T-cell-replete hematopoietic SCT in patients with advanced-stage acute leukemia: a retrospective risk-factor analysis. Bone Marrow Transplant 2012; 47: 1099–1104.
Acknowledgements
We thank the laboratory teams and the nurses for their support to clinical work.
Author contributions
LY and D-HL were responsible for the conception and design of the study; W-RH, D-HL, FL, L-PD and LW collected, analyzed and interpreted the data; D-HL drafted the manuscript; W-RH, H-HL, C-JG, JB, FL, L-PD and YJ provided study material or patients; L-LW provided laboratory work.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Huang, WR., Li, HH., Gao, CJ. et al. Haploidentical, unmanipulated G-CSF-primed peripheral blood stem cell transplantation for high-risk hematologic malignancies: an update. Bone Marrow Transplant 51, 1464–1469 (2016). https://doi.org/10.1038/bmt.2016.166
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2016.166
This article is cited by
-
Antithymocyte globulin plus post-transplant cyclophosphamide combination as graft-versus-host disease prophylaxis in haploidentical peripheral blood stem cell transplantation for hematological malignancies
International Journal of Hematology (2022)
-
Outcomes of myeloablative peripheral blood stem cell transplantation for non-complete remission patients with relapsed/refractory peripheral T cell lymphomas
Annals of Hematology (2019)
-
Everyone has a donor: contribution of the Chinese experience to global practice of haploidentical hematopoietic stem cell transplantation
Frontiers of Medicine (2019)
-
The consensus on indications, conditioning regimen, and donor selection of allogeneic hematopoietic cell transplantation for hematological diseases in China—recommendations from the Chinese Society of Hematology
Journal of Hematology & Oncology (2018)