Abstract
Purpose
To evaluate the tear film osmolarity (TFO) and ocular surface clinical signs and symptoms in chronically medicated glaucoma patients and post-trabeculectomy patients.
Methods
This is a single-center, prospective case-controlled study. One-hundred and thirty eyes of 130 participants aged ≥45 years were included (49 normal controls, 50 glaucoma patients on chronic preserved anti-glaucoma medication ≥6 months, and 31 post-trabeculectomy patients not on medication ≥6 months). TFO, tear break-up time (TBUT), Schirmer’s test I and dry eye symptoms were evaluated. Data from both groups of glaucoma patients were compared with age and sex-matched controls. Logistic regression was performed to calculate the odds ratios.
Results
Mean TFO in the three groups were 301.4±7.7, 307.0±9.3, and 307.4±11.6 mOsm/l, respectively. Compared with normal controls, chronically medicated glaucoma patients and post-trabeculectomy patients were more likely to have a raised TFO, with odds ratios (95% CI) of 4.43 (1.74–11.32) and 2.76 (1.02–7.94), respectively. Both groups of glaucoma patients were also more likely to experience dry eye symptoms, with ORs of 4.72 (1.92–11.59) and 4.24 (1.54–11.72). There was no significant difference in TFO and symptoms between both groups of glaucoma patients, and in TBUT and Schirmer’s test across all three groups.
Conclusions
Patients on chronic topical anti-glaucoma medication and post-trabeculectomy patients were more likely to have raised TFO and dry eye symptoms, suggesting significant ocular surface disease. Glaucoma practitioners should be aware that dry eye symptoms and raised TFO may occur in the absence of TBUT and Schirmer’s test abnormality.
Similar content being viewed by others
Introduction
Glaucoma is a major cause of blindness worldwide, second only to cataract.1, 2 The estimated prevalence of 0.8–7.0% globally3, 4, 5, 6 is predicted to increase by up to 50% by the year 2020,2 with 11.2 million of these patients projected to suffer from bilateral blindness.2 Treatment for glaucoma is usually targeted at reducing the intraocular pressure (IOP), which, when increased, is the main cause of irreversible optic nerve damage. This is usually achieved by topical medications.7
Unfortunately, ocular surface disease (OSD) is common in patients chronically treated for glaucoma.8 One of the reasons for this adverse effect is the presence of preservatives in the medication. The detrimental effects on the ocular surface could even decrease quality of life.9, 10 These preservatives, the most common being benzalkonium chloride (BAK), inhibit microbial growth in the medication and minimize the risk of ocular infection. In the form of cationic surfactants, preservatives cause microbial cell destruction by disrupting the cell membrane lipids and cytoplasmic contents.11 The lipid-destruction properties in BAK extend to the lipids in the tear film, which solubilizes during interaction with BAK.12 Tear lipids are responsible for the stabilization and evaporation control of the tear film. Its disturbance is a major cause of dry eye13—a common condition among patients being treated for glaucoma.14 The International Dry Eye Workshop has classified the use of anti-glaucoma medication as an extrinsic cause of evaporative dry eye.13
Surgical intervention is warranted when topical medications are inadequate in achieving the target IOP (eg, in advanced glaucoma), or there are significant contraindications for medication use (eg, medical side effects such as arrhythmia or allergic response).7 The current first line surgical procedure for glaucoma treatment is trabeculectomy with antimetabolites. After trabeculectomy, approximately 40% patients no longer require the use of anti-glaucoma medication.15 The prospect of anti-glaucoma medication cessation after surgery may be an advantageous outcome because the eye will no longer be subjected to the side effects of the contained preservatives. It is not known if the dry eye effect induced by previously instilled preservative containing medications can be reversed after their cessation. On the other hand, trabeculectomy has been suggested to have deleterious effects on the ocular surface, for example, conjunctival epithelial spongiosis and reduced number of conjunctival goblet cells.16
Previous researchers have analyzed the tear function in patients using topical anti-glaucoma medications. Tear break-up time (TBUT) and Schirmer’s test are examples of the common tests used. Another parameter that can be used to evaluate dry eye is tear film osmolarity (TFO). Measurements of TFO have been demonstrated to be suitable, and even superior to other forms of tests, in terms of dry eye diagnosis.17, 18, 19 Sullivan et al.20 found that TFO measurements are the best indication of dry eye severity, with a correlation coefficient of 0.55, as compared with other clinical tests.
In dry eye patients, TFO is increased. This moreover causes osmolarity of the ocular surface epithelial cells to elevate. The hyperosmolarity of the cells prompts the production of a cascade of proinflammatory cytokines.21 Conjunctival hyperemia, superficial punctate keratitis and symptoms of ocular discomfort are just a few of the clinical manifestations of tear cytokine upregulation.21 In patients topically medicated for glaucoma, TFO have been demonstrated to be elevated compared with normal values.22, 23 However, the previous studies did not compare these TFO values to a group of normal patients as controls. Januleviciene et al23 evaluated the change in TFO as patients switched from preserved anti-glaucoma medications to its preservative-free variants, whereas Labbe et al22 did a cross-sectional study to evaluate the effect of preserved topical anti-glaucoma medications on TFO.
Despite the numerous studies conducted on anti-glaucoma medication and OSD, the tear function test (TBUT and Schirmer’s test) profiles of these patients have not been well reported. The far majority of studies only reported symptoms24 or the tear function tests with preset thresholds.22, 25, 26 Another study reported that only 4.8% and 33.8% of patients on anti-glaucoma medications had TBUT and Schirmer’s test values of >10 s and >10 mm, respectively, as compared with a healthy population of 100% above these thresholds.27
We hypothesize that TFO may be raised in glaucoma patients, both on topical therapy and post trabeculectomy, compared with normal controls. This study is therefore aimed to compare TFO in chronically medicated glaucoma patients and post-trabeculectomy patients to controls without glaucoma or dry eyes.
As a secondary aim, we will compare clinical tear function tests between glaucoma patients and controls and explore the relationships between these dry eye test results and glaucoma treatment variables (ie, duration and number of topical anti-glaucoma medications).
Materials and methods
A prospectively conducted case-controlled study was performed at the Singapore National Eye Centre, from February 2012 to July 2012. This study complied with the tenets of the Declaration of Helsinki on human research and was approved by the SingHealth Institutional Review Board. All study participants have read and signed an informed consent form.
Eligible patients above the age of 45 years were recruited and segregated into three groups. The first group consisted of normal patients without prior history of glaucoma, dry eye, or other ocular surface disorder. Only patients who did not have any dry eye symptoms or use of lubricants within the last 3 months were included. The second group consisted of patients with glaucoma, have been using ≥1 topical preserved anti-glaucoma medication for ≥6 months, and had no history of trabeculectomy. The third group consisted of patients with glaucoma who have undergone trabeculectomy ≥6 months ago and were not on any anti-glaucoma medications or topical steroids. Patients with any other history of significant ocular or systemic disease, ocular or systemic conditions associated with dry eye, use of topical steroids, and contact lens wear were excluded from the study.
Clinical evaluation
Dry eye symptoms and clinical signs were evaluated. The severity and frequency of dry eye symptoms experienced by patients were determined using the ‘Symptom Assessment iN Dry Eye’ (SANDE) scale as previously described.28 In short, the subject marks an ‘X’ on two separate 10 cm line; one representing the severity and the other representing the frequency of symptoms. These parameters were then quantified by measuring the distance between the left-end of the line to the ‘X’, with a range of 0–100 mm. A symptom global score was than computed using these measurements.
Clinical tests include TFO measurement, TBUT, and Schirmer’s test I (without anesthesia). TFO was measured using the TearLab Osmolarity System (TearLab Corp, San Diego, CA, USA). The lab-on-a-chip system of the instrument consists of a one-time-use test card, which collects 50 ηl of tear sample and analyses it immediately to provide an osmolarity reading.29 In accordance to the recommendation of the manufacturer and a previous report,30 three measurements per eye were taken and averaged for analysis. However, only the eye eligible for the study was evaluated.
Another recommendation of the manufacturer was to obtain measurements from both eyes and use the higher of the two measurements for analysis.20, 31 However, because not all glaucoma patients would be treated on both eyes, only the treated eye was included in the study. In patients where both eyes were eligible, both eyes were included in the study. In the control group, only the right eye was included in the analysis. To ensure that the TFO is not affected by reflex tearing or the instillation of fluorescein dye, measurements were done before any other clinical tests.
For TBUT evaluation, fluorescein was instilled with a fluorescein strip (Fluorets; Chauvin Pharmaceuticals, Aubenas, France) moistened with non-preserved saline. A single observer evaluated this parameter to avoid inter-observer discrepancies. TBUT was measured three times with a stopwatch and averaged for analysis. Schirmer’s test I recorded (in millimeters) the length of wetting on the Schirmer’s strip (Sno strips; Bausch & Lomb, Rochester, NY, USA) after 5 min.
Data analysis
To maintain independence of data points, only one eye was included in the analysis. The right eyes of normal controls were used for analysis. For patients in the glaucoma treatment groups, if both eyes are eligible for the study, only the right eye of each patient was used for analysis.
Statistical analysis was performed using SPSS (version 20; SPSS statistics, Chicago, IL, USA). For comparisons of continuous variables (eg, TFO and SANDE scores) between the three groups, if analysis of variance (ANOVA) showed a significant trend (P<0.05), post hoc multiple comparisons were used, with statistical significance set at the level of 0.05/6 or 0.008. Differences in clinical features between each group were first determined with one-way MANOVA. Where there is a significant result in one-way MANOVA, logistic regression was performed to calculate odds ratios, corrected for age and gender. Values from the control group were used as the indicator to which the medicated and post-trabeculectomy group were compared. Spearmen’s correlation was used to identify correlations between each clinical test. To establish dichotomous-dependent variables, the cut-off value for TFO was ≤308 mOsm/l as determined from previous reports.20, 22 The threshold for coding the other parameters was the median values of those parameters among all patients. For example, severe dry eye symptom was defined as having a SANDE score above the median of 10. To examine associations between the dry eye parameters and variables of medication use (ie, the duration and number of drops used), logistic regression was performed with the dry eye parameters as dependent variable and the medication variables as independent variables.
Results
One-hundred and thirty patients were recruited in total: 49 normal controls; 50 in the medicated group; and 31 in the post-trabeculectomy group. Mean age of patients in the three groups were 63.2±9.3, 65.9±10.1, and 71.1±7.5 years, respectively. There was no statistical difference in patient demographics between the control and the medicated group. However, patients in the post-trabeculectomy group were significantly older than the other two groups (P≤0.005). Racial differences between groups were minimal, with the majority made up of Chinese patients. Patient demographics, duration and number of topical anti-glaucoma medication used, and duration between trabeculectomy and study entry are shown in Table 1.
Of the 50 patients (50 eyes) in the medicated group, the most common glaucoma type was primary open-angle glaucoma (24 patients), followed by primary angle-closure glaucoma (20 patients). Five patients were being treated for ocular hypertension, and two patients had neovascular glaucoma secondary to uveitis. For each patient, the mean number of medications currently used was 3, their duration of medication use varied widely, ranging from 6 to 195 months, with a mean of 63.2 months (Table 1).
In the post-trabeculectomy group, majority of diagnoses were similarly primary open-angle glaucoma (16 patients), followed by primary angle-closure glaucoma (15 patients). One patient had ocular hypertension and two had secondary glaucoma (one due to pigment dispersion and the other due to post-penetrating keratoplasty). All patients have discontinued medication use for a duration ranging 11–166 months since the trabeculectomy procedure, with a mean of 56.7 months (Table 1). Before trabeculectomy, patients in group 3 used a mean of three different types of topical anti-glaucoma medication for a duration ranging 6–138 months, with a mean of 42.7 months.
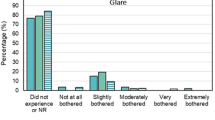
The severity of dry eye symptoms (Table 1) is the main discriminating feature between the glaucoma groups compared with control. In addition, we found TFO correlated moderately with the SANDE score (r=0.317, P<0.001). There was a trend for lower TBUT in the medicated group compared with controls, and a lower Schirmer’s test in the post-trabeculectomy group compared with controls, but these were not statistically significant (Table 1).
TFO was significantly higher in the medicated and post-trabeculectomy groups as compared with normal controls (P=0.01, Table 1). Patients on chronic anti-glaucoma medication were approximately three times more likely to have an increased TFO, whereas post-trabeculectomy patients were up to four times more likely (Table 2). There was, however, no significant difference in TFO between these two groups of glaucoma patients (P=0.41).
When the results were recalculated including only the eye with worse osmolarity in glaucoma patients where both eyes were eligible, similar conclusions were obtained except with higher odds ratios (data not shown). We did not present this formally as we did not have osmolarity values for both eyes of the control group.
Similarly, with symptom scores, both groups of glaucoma patients experienced more symptoms of dry eye than controls (P<0.001, Table 1), but no difference between glaucoma groups (P=0.91). Both groups of glaucoma patients were five times more likely to develop severe dry eye symptoms than controls (Table 2).
Age, gender, number and duration of topical anti-glaucoma medication use, and duration since trabeculectomy did not significantly contribute to the severity of TFO and dry eye symptoms and signs (Table 3).
Discussion
This study found TFO to be elevated significantly in both chronically medicated glaucoma patients as well as in post-trabculectomy patients as compared with controls. Glaucoma patients on treatment have also experienced more symptoms of dry eye than normal controls. However, tear function tests (TBUT and Schirmer’s test) were not significantly different between glaucoma-treated patients and normal controls.
TFO has been suggested to be the ‘gold standard’ for dry eye diagnosis.32 Studies have demonstrated the agreement of TFO measurements with other clinical signs of dry eye17, 22 and even exhibited a linear correlationship with the overall severity of dry eye across the entire clinical spectrum.20
Although tear film hyperosmolarity have been demonstrated previously in glaucoma-medicated patients (n=40),22 the lack of a control group may have rendered the study less conclusive. In the current study, we found that patients chronically medicated for glaucoma have significantly higher TFOs than normal controls. In another longitudinal study of 30 patients, the TFO had decreased significantly within 2 weeks after the patients had switched from preserved to preservative-free topical anti-glaucoma medication.23
The discontinuation of preserved medications supported the widely accepted notion of the adverse effects of preservatives on the ocular surface. In an animal study, Chen et al33 have demonstrated that the application of BAK alone onto the cornea can be extremely detrimental to the ocular surface. The disturbances of preservatives on tear lipids may have increased evaporation of the aqueous tear component, and consequently increased the relative solute concentration (TFO). Elevation of TFO may lead to an inflammatory response,21 which damages the ocular surface and its afferent nerves and may result in a reduction of tear aqueous secretion and an even further increase in TFO. In other words, the TFO may then be a cause as well as effect of the dry eye.
We also found that TFO is elevated in post-trabeculectomy patients, even after a long period with no anti-glaucoma medication. To the best of our knowledge and literature search, TFO has not been reported in post-trabeculectomy patients. An association between development or exacerbation of dry eye and presence of trabeculectomy blebs has been suggested.34 Ocular discomfort, tearing, foreign body sensation, and burning sensation had been reported in patients after trabeculectomy in an observational study of 97 patients.35 These symptoms are similar to that of dry eye.13 We found agreeing data in the current study, where post-trabeculectomy patients were five times more likely to experience symptoms of dry eye. It is important to note that the symptoms and clinical signs of dry eye may not always concord.36, 37 In a study of 344 subjects, only 57% of patients with clear objective signs of dry eye were symptomatic.29 On the other hand, patients may experience symptoms of dry eye in the absence of any clinical signs.38 The disagreement between symptoms and signs may be an additional support for the use of TFO measurements to determine the severity of dry eye.
Neves Mendes et al39 conducted a case-controlled study to evaluate ocular surface changes in post-trabeculectomy patients. By comparing a group of post-trabeculectomy patients (at least 6 months after surgery) against normal controls (40 eyes of 40 participants in each group), they found that TBUT, corneal fluorescein staining, and Rose Bengal staining were worse in post-trabeculectomy patients.39 In that study, TBUT was lower in post-trabeculectomy patients (9.3±4.5 vs 12.5±2.1 s in the control group), but the difference may not be clinically meaningful. Although the racial composition of their study population and site(s) of data collection were not mentioned, it is likely to be made up of at least a majority of Brazilian because the authors’ affiliations were in Brazil. Differences between TBUT and Schirmer’s test of these studies may be because of differences in ethnicity. The tear parameters may be more normal in non-Asian controls compared with Asian controls. In addition, it should be noted that in Neves Mendes et al’s study, their post-trabeculectomy patients discontinued topical medications for ≥3 months as compared with ≥11 months in the current study. Some residual effect from the medication may have manifest in their data.
The mechanism of dry eye in post-trabeculectomy patients is not well understood. It is likely that the bleb morphology, which can be elevated, especially cystic blebs, interferes with the spreading of the tear film as the upper lid passes over this elevation. In 1983, Soong and Quigley40 noticed dellen formations proximate to the blebs in 10% of the trabeculectomy cases reviewed. They associated the dellen formations to compromised tear film, which have a tendency to break up at the corneal area adjacent to the bleb.
There are several other reasons why trabeculectomy itself may compromise tear function; the use of antimetabolites may have compromised corneal epithelium. For example, mitomycin C used during surgery to minimize post-operative scarring has reported to cause corneal epitheliopathy41, 42 and limbal stem cell deficiency.43 Irregular corneal surface and increased inflammatory cells result from the corneal epithelial abnormalities,45, 46 and this may be related to the poor quality of the tear film.
Alternatively, the raised TFO in trabeculectomy may be related to prior medication use. If this were true, the fact that patients’ TFO were still elevated even after more than 11 months of discontinuation of anti-glaucoma medication is quite remarkable and significant. This prolonged effect of medications may be related to profibrotic and chronic inflammatory changes in the ocular surface after instillation of anti-glaucoma medications. Our results also seem to suggest that TFO and dry eye symptoms tend not to reverse after trabeculectomy surgery in previously chronically medicated glaucoma eyes.
In our study, glaucoma patients experienced more symptoms of dry eye than the controls. In the profiling of our glaucoma patients, unlike Baudouin8 who reported a lower mean TBUT and Schirmer’s compared with our studies, our controls and glaucoma patients essential show similar TBUT and Schirmer’s test.
In the profiling of our glaucoma patients, dry eye symptoms were more severe in glaucoma patients than controls. On the other hand, our controls and glaucoma patients showed similar TBUT and Schirmer’s test results. One possible explanation for this is the way we defined the control group, that is, we defined control participants to be those with absence of dry eye symptoms. Later on, we explored the scenario of controls having stringent criteria for TBUT and Schirmer’s test. However, there was no difference in the mean TFO (P>0.05) with exactly the same mean of 301 mOsm/l, comparing controls with TBUT above and below 5 s. Similarly, the mean TFO in controls with Schirmer’s test less or more than 10 mm was also not different at 301 mOsm/l. This suggests that more stringent classifications for controls will not result in a lower or different TFO.
We found that the number of topical anti-glaucoma medications use, duration of use, and duration post trabeculectomy did not influence the osmolarity and dry eye symptoms (Table 3). In contrast, Labbe et al22 reported that the number instillations of anti-glaucoma medications correlated positively with the TFO (r=0.629). The apparent discrepancy may be due to a smaller range or spread of our variables. The TFO ranged from 290 to 339 mOsm/l in the current study compared with 280–343 mOsm/l in Labbe et al’s study. TBUT in our glaucoma patients was also spread within a smaller range (0.8–10.8 s), compared with the seconds reported in the study by Labbe et al.
The current study has several strengths. We calculated odds ratios of glaucoma treatment contributing to increased TFO and dry eye symptoms. The incorporation of a control group eliminated any bias in the data collection process. To the best of our knowledge, this is the first study that reported the tear function tests values in glaucoma-medicated and post-trabeculectomy patients with a control group.
In addition, clinical tests were performed in a standardized sequence that ensured that measurements were not affected by a previous procedure. Repeated measurements of TFO and TBUT also ascertained their accuracy.
However, the drawbacks of our study must also be considered. First, corneal and conjunctival fluorescein staining was not evaluated, although this has been extensively studied in the past.25, 35, 39, 46, 47, 48
Second, our study did not consider the possibility that glaucoma patients’ (in the medicated and post-trabeculectomy groups) tear function may be due to dry eye that was independent of their glaucoma treatment. Glaucoma patients on concomitant systemic (eg, hormonal pills)49 or ocular medications (eg, artificial tear lubricants),50 which can affect dry eye test parameters, were also not considered. A controlled longitudinal study of TFO may be needed to ascertain ocular surface changes that may take place after the commencement of glaucoma treatment.
Third, the effect of different kinds of topical anti-glaucoma medications on TFO was not evaluated in detail here. For example, differences in ocular surface side effects of latanoprost and timolol have been reported, although this is controversial among different studies.51, 52 Future studies may be warranted to evaluate TFO variances with different types of anti-glaucoma medication use. In addition, we did not evaluate number of instillations of medications per day or the time of last use. A longitudinal prospective study would also be good to evaluate the same eye on medication and postoperatively. This may be difficult to analyze because of variation of use during the long period of treatment.
In glaucoma, medical compliance is crucial in controlling the IOP. Unfortunately, the preservatives present in these medications cause the development of, or exacerbates, OSD. Preservative-induced OSD causes ocular discomfort and dryness and may account for non-compliance to glaucoma treatment53 (up to 64% in one study).54 The development of preservative-free topical anti-glaucoma medications such as Timabak (Théa, Paris, France) and Zioptan (Merck, Whitehouse Station, NJ, USA) has provided a solution to avoid the adverse effects of preservatives.14, 55 The decrement of TFO and improvement of symptoms is even possible when patients switch from preserved prostaglandin analogue (latanoprost) drops to its preservative-free form (tafluprost).23
Glaucoma practitioners should be aware that the presence of dry eye symptoms may occur with a raised TFO to indicate OSD in their patients, without an associated abnormality of TBUT and Schirmer’s testing. This emphasizes the importance of ocular surface symptom assessment in glaucoma patients.
In conclusion, our study reports that TFO is increased in glaucoma patients on chronic topical medications and remains elevated after trabeculectomy surgery. Further studies may be warranted to determine whether dry eye is merely aggravated by or can be caused by trabeculectomy surgery.

References
Quigley HA . Number of people with glaucoma worldwide. Br J Ophthalmol 1996; 80 (5): 389–393.
Quigley HA, Broman AT . The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol 2006; 90 (3): 262–267.
Dielemans I, Vingerling JR, Wolfs RC, Hofman A, Grobbee DE, de Jong PT . The prevalence of primary open-angle glaucoma in a population-based study in the Netherlands. The Rotterdam Study. Ophthalmology 1994; 101 (11): 1851–1855.
Friedman DS, Wolfs RC, O'Colmain BJ, Klein BE, Taylor HR, West S et al. Prevalence of open-angle glaucoma among adults in the United States. Arch Ophthalmol 2004; 122 (4): 532–538.
Rudnicka AR, Mt-Isa S, Owen CG, Cook DG, Ashby D . Variations in primary open-angle glaucoma prevalence by age, gender, and race: a Bayesian meta-analysis. Invest Ophthalmol Vis Sci 2006; 47 (10): 4254–4261.
Leske MC, Connell AM, Schachat AP, Hyman L . The Barbados Eye Study. Prevalence of open angle glaucoma. Arch Ophthalmol 1994; 112 (6): 821–829.
Lee DA, Higginbotham EJ . Glaucoma and its treatment: a review. Am J Health Syst Pharm 2005; 62 (7): 691–699.
Baudouin C, Renard JP, Nordmann JP, Denis P, Lachkar Y, Sellem E et al. Prevalence and risk factors for ocular surface disease among patients treated over the long term for glaucoma or ocular hypertension. Eur J Ophthalmol 2013; 23 (1): 47–54.
Skalicky SE, Goldberg I, McCluskey P . Ocular surface disease and quality of life in patients with glaucoma. Am J Ophthalmol 2012; 153 (1): 1–9 e2.
Paletta Guedes RA, Paletta Guedes VM, Freitas SM, Chaoubah A . Quality of life of medically versus surgically treated glaucoma patients. J Glaucoma 2012; 22: 369–373.
Noecker R . Effects of common ophthalmic preservatives on ocular health. Adv Ther 2001; 18 (5): 205–215.
Wilson WS, Duncan AJ, Jay JL . Effect of benzalkonium chloride on the stability of the precorneal tear film in rabbit and man. Br J Ophthalmol 1975; 59 (11): 667–669.
Lemp MA, Baudouin C, Baum J, Dogru M, Foulks GN, Kinoshita S et al. The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007; 5 (2): 75–92.
Pisella PJ, Pouliquen P, Baudouin C . Prevalence of ocular symptoms and signs with preserved and preservative free glaucoma medication. Br J Ophthalmol 2002; 86 (4): 418–423.
Gayton JL, Van Der Karr M, Sanders V . Combined cataract and glaucoma surgery: trabeculectomy versus endoscopic laser cycloablation. J Cataract Refract Surg 1999; 25 (9): 1214–1219.
Baudouin C . Ocular surface and external filtration surgery: mutual relationships. Dev Ophthalmol 2012; 50: 64–78.
Versura P, Profazio V, Campos EC . Performance of tear osmolarity compared to previous diagnostic tests for dry eye diseases. Curr Eye Res 2010; 35 (7): 553–564.
Tomlinson A, Khanal S, Ramaesh K, Diaper C, McFadyen A . Tear film osmolarity: determination of a referent for dry eye diagnosis. Invest Ophthalmol Vis Sci 2006; 47 (10): 4309–4315.
Lemp MA, Bron AJ, Baudouin C, Benitez Del Castillo JM, Geffen D, Tauber J et al. Tear osmolarity in the diagnosis and management of dry eye disease. Am J Ophthalmol 2011; 151 (5): 792–798 e1.
Sullivan BD, Whitmer D, Nichols KK, Tomlinson A, Foulks GN, Geerling G et al. An objective approach to dry eye disease severity. Invest Ophthalmol Vis Sci 2010; 51 (12): 6125–6130.
Li DQ, Chen Z, Song XJ, Luo L, Pflugfelder SC . Stimulation of matrix metalloproteinases by hyperosmolarity via a JNK pathway in human corneal epithelial cells. Invest Ophthalmol Vis Sci 2004; 45 (12): 4302–4311.
Labbe A, Terry O, Brasnu E, Van Went C, Baudouin C . Tear film osmolarity in patients treated for glaucoma or ocular hypertension. Cornea 2012; 31 (9): 994–999.
Januleviciene I, Derkac I, Grybauskiene L, Paulauskaite R, Gromnickaite R, Kuzmiene L . Effects of preservative-free tafluprost on tear film osmolarity, tolerability, and intraocular pressure in previously treated patients with open-angle glaucoma. Clin Ophthalmol 2012; 6: 103–109.
Fechtner RD, Godfrey DG, Budenz D, Stewart JA, Stewart WC, Jasek MC . Prevalence of ocular surface complaints in patients with glaucoma using topical intraocular pressure-lowering medications. Cornea 2010; 29 (6): 618–621.
Arici MK, Arici DS, Topalkara A, Guler C . Adverse effects of topical antiglaucoma drugs on the ocular surface. Clin Experiment Ophthalmol 2000; 28 (2): 113–117.
Kuppens EV, Stolwijk TR, de Keizer RJ, van Best JA . Basal tear turnover and topical timolol in glaucoma patients and healthy controls by fluorophotometry. Invest Ophthalmol Vis Sci 1992; 33 (12): 3442–3448.
Herreras JM, Pastor JC, Calonge M, Asensio VM . Ocular surface alteration after long-term treatment with an antiglaucomatous drug. Ophthalmology 1992; 99 (7): 1082–1088.
Schaumberg DA, Gulati A, Mathers WD, Clinch T, Lemp MA, Nelson JD et al. Development and validation of a short global dry eye symptom index. Ocul Surf 2007; 5 (1): 50–57.
Sullivan BD, Crews LA, Messmer EM, Foulks GN, Nichols KK, Baenninger P et al. Correlations between commonly used objective signs and symptoms for the diagnosis of dry eye disease: clinical implications. Acta Ophthalmol 2012 epub ahead of print 28 December 2012; doi:10.1111/aos.12012.
Khanal S, Millar TJ . Barriers to clinical uptake of tear osmolarity measurements. Br J Ophthalmol 2012; 96 (3): 341–344.
Sullivan BD, Crews LA, Sonmez B, de la Paz MF, Comert E, Charoenrook V et al. Clinical utility of objective tests for dry eye disease: variability over time and implications for clinical trials and disease management. Cornea 2012; 31 (9): 1000–1008.
Farris RL . Tear osmolarity—a new gold standard? Adv Exp Med Biol 1994; 350: 495–503.
Chen W, Li Z, Hu J, Zhang Z, Chen L, Chen Y et al. Corneal alternations induced by topical application of benzalkonium chloride in rabbit. PLoS One 2011; 6 (10): e26103.
Palmberg P . Surgery for complications. In Albert DM (eds) Ophthalmic Surgery: Principles and Techniques. Blackwell Science: Malden, MA, 1999 pp 176–191.
Budenz DL, Hoffman K, Zacchei A . Glaucoma filtering bleb dysesthesia. Am J Ophthalmol 2001; 131 (5): 626–630.
Fuentes-Paez G, Herreras JM, Cordero Y, Almaraz A, Gonzalez MJ, Calonge M . Lack of concordance between dry eye syndrome questionnaires and diagnostic tests. Arch Soc Esp Oftalmol 2011; 86 (1): 3–7.
Moore JE, Graham JE, Goodall EA, Dartt DA, Leccisotti A, McGilligan VE et al. Concordance between common dry eye diagnostic tests. Br J Ophthalmol 2009; 93 (1): 66–72.
Viso E, Rodriguez-Ares MT, Abelenda D, Oubina B, Gude F . Prevalence of asymptomatic and symptomatic meibomian gland dysfunction in the general population of Spain. Invest Ophthalmol Vis Sci 2012; 53 (6): 2601–2606.
Neves Mendes CR, Hida RY, Kasahara N . Ocular surface changes in eyes with glaucoma filtering blebs. Curr Eye Res 2012; 37 (4): 309–311.
Soong HK, Quigley HA . Dellen associated with filtering blebs. Arch Ophthalmol 1983; 101 (3): 385–387.
Coppens G, Maudgal P . Corneal complications of intraoperative mitomycin C in glaucoma surgery. Bull Soc Belge Ophtalmol 2010; 314: 19–23.
Hau S, Barton K . Corneal complications of glaucoma surgery. Curr Opin Ophthalmol 2009; 20 (2): 131–136.
Sauder G, Jonas JB . Limbal stem cell deficiency after subconjunctival mitomycin C injection for trabeculectomy. Am J Ophthalmol 2006; 141 (6): 1129–1130.
Dua HS, Saini JS, Azuara-Blanco A, Gupta P . Limbal stem cell deficiency: concept, aetiology, clinical presentation, diagnosis and management. Indian J Ophthalmol 2000; 48 (2): 83–92.
Wilson SE, Netto M, Ambrosio R Jr. . Corneal cells: chatty in development, homeostasis, wound healing, and disease. Am J Ophthalmol 2003; 136 (3): 530–536.
Shimazaki J, Hanada K, Yagi Y, Yamagami J, Ishioka M, Shimmura S et al. Changes in ocular surface caused by antiglaucomatous eyedrops: prospective, randomised study for the comparison of 0.5% timolol v 0. 12% unoprostone. Br J Ophthalmol 2000; 84 (11): 1250–1254.
Leung EW, Medeiros FA, Weinreb RN . Prevalence of ocular surface disease in glaucoma patients. J Glaucoma 2008; 17 (5): 350–355.
Yalvac IS, Gedikoglu G, Karagoz Y, Akgun U, Nurozler A, Koc F et al. Effects of antiglaucoma drugs on ocular surface. Acta Ophthalmol Scand 1995; 73 (3): 246–248.
Smith JA, Albeitz J, Begley C, Caffery B, Nichols K, Schaumberg D, Schein O . The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007; 5 (2): 93–107.
Pflugfelder SC, Geerling G, Kinoshita S, Lemp MA, McCulley J, Nelson D et al. Management and therapy of dry eye disease: report of the Management and Therapy Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007 5 (2): 163–178.
Thygesen J, Aaen K, Theodorsen F, Kessing SV, Prause JU . Short-term effect of latanoprost and timolol eye drops on tear fluid and the ocular surface in patients with primary open-angle glaucoma and ocular hypertension. Acta Ophthalmol Scand 2000; 78 (1): 37–44.
Costagliola C, Prete AD, Incorvaia C, Fusco R, Parmeggiani F, Di Giovanni A . Ocular surface changes induced by topical application of latanoprost and timolol: a short-term study in glaucomatous patients with and without allergic conjunctivitis. Graefes Arch Clin Exp Ophthalmol 2001; 239 (11): 809–814.
Kulkarni SV, Damji KF, Buys YM . Medical management of primary open-angle glaucoma: Best practices associated with enhanced patient compliance and persistency. Patient Prefer Adherence 2008; 2: 303–314.
Bloch S, Rosenthal AR, Friedman L, Caldarolla P . Patient compliance in glaucoma. Br J Ophthalmol 1977; 61 (8): 531–534.
Pisella PJ, Fillacier K, Elena PP, Debbasch C, Baudouin C . Comparison of the effects of preserved and unpreserved formulations of timolol on the ocular surface of albino rabbits. Ophthalmic Res 2000; 32 (1): 3–8.
Acknowledgements
Grant support was provided by NMRC/1206/2009, NMRC/CSA/013/2009, NMRC/TCR/002-SERI/2008, and NMRC/CG/SERI/2010 from National Medical Research Council (NMRC), Singapore, BMRC 10/1/35/19/670 from Biomedical Research Council (BMRC), Singapore, and the SNEC research endowment funds from the Singapore National Eye Centre, Singapore.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Lee, SY., Wong, T., Chua, J. et al. Effect of chronic anti-glaucoma medications and trabeculectomy on tear osmolarity. Eye 27, 1142–1150 (2013). https://doi.org/10.1038/eye.2013.144
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2013.144
Keywords
This article is cited by
-
Changing from preserved, to preservative-free cyclosporine 0.1% enhanced triple glaucoma therapy: impact on ocular surface disease—a randomized controlled trial
Eye (2023)
-
Managing the ocular surface after glaucoma filtration surgery: an orphan topic
Graefe's Archive for Clinical and Experimental Ophthalmology (2023)
-
Optimization of the Ocular Surface Through Treatment of Ocular Surface Disease Before Ophthalmic Surgery: A Narrative Review
Ophthalmology and Therapy (2022)
-
Präoperatives Management bei subkonjunktivalen/subtenonalen glaukomchirurgischen Operationen unter besonderer Berücksichtigung des Gelimplantats (XEN®)
Der Ophthalmologe (2021)
-
Das postoperative trockene Auge nach ophthalmochirurgischen Eingriffen
Spektrum der Augenheilkunde (2021)