Abstract
Iron accumulation is associated with the pathophysiology of chronic kidney disease (CKD). Renal fibrosis is a final common feature that contributes to the progression of CKD; however, little is known about the association between renal iron accumulation and renal interstitial fibrosis in CKD. Here we investigate the effects of iron chelation on renal interstitial fibrosis in a rat model of CKD. CKD was induced by 5/6 nephrectomy in Sprague–Dawley rats. At 8 weeks after operation, 5/6 nephrectomized rats were administered an oral iron chelator, deferasirox (DFX), in chow for 8 weeks. Other CKD rats were given a normal diet. Sham-operative rats given a normal diet served as a control. CKD rats exhibited hypertension, glomerulosclerosis and renal interstitial fibrosis. Iron chelation with DFX did not change hypertension and glomerulosclerosis; however, renal interstitial fibrosis was attenuated in CKD rats. Consistent with these findings, renal gene expression of collagen type III and transforming growth factor-β was increased in CKD rats compared with the controls, while iron chelation suppressed these increments. In addition, a decrease in vimentin along an increase in E-cadherin in renal gene expression was observed in CKD rats with iron chelation. CKD rats also showed increased CD68-positive cells in the kidney, whereas its increase was attenuated by iron deprivation. Similarly, increased renal gene expression of CD68, tumor necrosis factor-α and monocyte chemoattractant protein-1 was suppressed in CKD rats with iron chelation. Renal iron accumulation seems to be associated with renal interstitial fibrosis in a rat model of CKD.
Similar content being viewed by others
Introduction
Chronic kidney disease (CKD) represents a public health epidemic that leads to end-stage renal disease.1 Renal fibrosis is a final common feature that contributes to the progression of CKD.2 Thus, prevention of renal fibrosis is critical for suppressing the progression of CKD.
Iron is an essential element for life and has an important role in a number of metabolic processes. Excessive iron, however, produces oxidative stress, which may lead to tissue damage. Thus, iron is considered to be implicated in the pathophysiology of several cardiovascular and renal diseases. Importantly, renal iron accumulation is observed in patients with chronic renal disease3, 4 and animal models of nephropathy.5, 6, 7, 8 In this regard, iron reduction might be effective against these diseases. In fact, the effects of iron chelation with deferoxamine against several cardiovascular and renal diseases have been reported. For instance, experimental studies have shown that iron chelation with deferoxamine leads to greater recovery of myocardial function and reduced myocardial infarct size.9, 10 Furthermore, deferoxamine has protective effects on carbon tetrachloride-induced acute hepatic failure,11 and renal dysfunction induced by adriamycin12 and chromium13 in experimental studies. In addition, recent clinical studies have shown the safety and efficacy of iron chelation with deferiprone in patients with glomerulonephritis and diabetic nephropathy.14
Renal fibrosis is a final feature that is related to the progression of CKD; however, little is known about the association between renal iron accumulation and renal interstitial fibrosis in CKD. In the current study, we investigate the effects of iron chelation on renal interstitial fibrosis in a rat model of CKD.
Methods
Animals and experimental design
All animal care and experimental procedures were approved by the Animal Research Committee of Hyogo College of Medicine (protocol #13-060). Six-week-old male Sprague–Dawley (SD) rats were purchased from Oriental Yeast Inc., Chiba, Japan and housed in the Hyogo College of Medicine Animal Care Facility. Rats were fed on a normal diet for 1week. Afterward, rats were anesthetized with ketamine HCl and xylazine HCl, and underwent a surgery to remove 5/6 of total renal mass by cauterizing the upper and lower poles of the right kidney followed by resecting the left kidney, as previously described.15
Protocol 1: At 3 weeks after 5/6 nephrectomy, rats were randomly divided into three groups and were administered several doses of an oral iron chelator, deferasirox (DFX), in chow (low dose (15 mg kg−1 day−1), moderate dose (30 mg kg−1 day−1) and high dose (60 mg kg−1 day−1) (n=4 in each group)) for 3 weeks. Other CKD rats were given a normal diet (n=4) for 3 weeks. Sham-operative rats given a normal diet served as a control (n=4). DFX was a gift from Novartis Pharma K.K. (Basel, Switzerland). Rats were maintained on a 12 h light/dark cycle and had free access to food and water. Systolic blood pressure (SBP) was measured, and urine samples were collected for 24 h in metabolic cages at 5 weeks surgery. At 6 weeks after surgery, rats were killed by intraperitoneal injection of ketamine HCl and xylazine HCl. Their blood was quickly withdrawn by abdominal aorta puncture, and serum was stored at −80°C before analysis. The tissues were excised and washed in phosphate-buffered saline. Afterward, the tissues were quickly snap-frozen in liquid nitrogen and stored at −80 °C. A part of each sample was fixed with buffered 4% paraformaldehyde.
Protocol 2: At 8 weeks after 5/6 nephrectomy, rats were randomly divided into two groups and were given DFX (30 mg kg−1 day−1) in chow (n=8) or a normal diet (n=8) for 8 weeks. Sham-operative rats given a normal diet served as a control (n=6). SBP and body weight were monitored every 1 week and behavior was assessed every day during the experiments. Urine samples were collected for 24 h in metabolic cages every 4 weeks. At 16 weeks after surgery, rats were collected blood samples and tissues.
Blood pressure, blood and urine measurements
SBP was measured by a noninvasive computerized tail-cuff system (MK-2000, Muromachi Kikai, Tokyo, Japan).16, 17 Blood cell count, serum iron, blood urea nitrogen (BUN) and creatinine levels were measured as previously reported.8, 18 Urinary concentrations of total protein and iron were determined by the pyrogallol red method and atomic absorption method, respectively.15
RNA extraction and real-time quantitative RT-PCR
Total RNA was extracted from the kidney using TRIzol reagent (Invitrogen, Carlsbad, CA, USA) as previously reported.19 Total RNA was treated with DNase and reverse transcribed into cDNA using random primers (Applied Biosystems, Alameda, CA, USA). Real-time PCR reactions were performed using the ABI PRISM 7900 with TaqMan Universal PCR Master Mix and TaqMan Gene Expression Assays (Applied Biosystems).15 TaqMan Gene Expression Assays were used as probes and primers for each gene as follows: collagen type III (assay ID no. Rn01437683_m1), plasminogen activator inhibitor type 1 (PAI-1) (assay ID Rn01481341_m1), vimentin (assay ID Rn00579738_m1), E-cadherin (assay ID Rn00580109_m1), transforming growth factor-β (TGF-β) (assay ID no. Rn00572010_m1), p22phox (assay ID no. Rn00577357_m1), gp91phox (assay ID no. Rn00576710_m1), CD68 (assay ID Rn01495634_g1), tumor necrosis factor-α (TNF-α) (assay ID no. Rn99999017_m1), monocyte chemoattractant protein-1 (MCP-1) (assay ID Rn00580555_m1), lipocalin 2 (LCN2) (assay ID Rn00590612_m1) and glyceraldehyde-3-phosphatedehydrogenase (GAPDH) (assay ID no. Rn99999916_m1). Relative gene expression levels were normalized to GAPDH gene expression.
Western blot analysis
The total protein homogenate (30 μg) from the kidney was separated by sodium dodecyl sulfate–PAGE (SDS–PAGE) and transferred onto polyvinylidene difluoride membranes. Renal tissues were homogenized with ice-cold lysis buffer (mmol l−1: Tris-HCl 20 (pH 7.5), EGTA 1, NaCl 150, β-glycerophosphate 1, sodium orthovanadate 1, Na2EDTA 1, PMSF 1, and sodium pyrophosphate 2.5, plus 1% Triton-X-100 and 1 μg ml–1 leupeptin). The signals were detected using enhanced chemiluminescence kit (Thermo Scientific, Rockford, IL, USA), and the images were analyzed using Image Quant LAS 4000 mini (GE Healthcare UK Ltd, Little Chalfont, UK). Here, the antibodies used were against rabbit anti-Smad3 (Cell Signaling Technology, Inc., Danvers, MA, USA; dilution 1:1000), rabbit anti-GAPDH (Cell Signaling Technology; dilution 1:1000), goat anti-LCN2 (R and D Systems, Minneapolis, MN, USA; dilution 1:1000) and mouse anti-β-actin (Sigma-Aldrich, St Louis, MO, USA; dilution 1:1000).
Assessments of tissue iron content
Tissue iron content of the kidney was measured by Metallo assay kit according to the manufacturer’s instructions (AKJ Global Technology, Chiba, Japan). Iron content was then corrected to kidney weight for each sample.
Histological analysis
Kidney tissues were fixed with buffered 4% paraformaldehyde, embedded in paraffin and cut into 4-μm-thick sections. Periodic acid-Schiff and Masson’s trichrome staining were performed using serial sections. Ferric iron deposits were stained using berlin blue staining. Glomerular and tubular lesions were evaluated by a semiquantitative score using the method as previously described.20 The extent of iron deposits was evaluated by semiquantitative score; 0, 1 and 2 correspond to 0, 1–10 and 10–20% of the microscopic field. Thirty randamly selected fields were counted. Renal sections were immunohistochemically stained with a primary mouse anti-CD68 antibody (AbD Serotec, Raleigh, NC, USA; dilution 1:1000), a primary mouse anti-desmin antibody (Dako, Glostrup, Denmark; dilution 1:50). Immunostains were visualized with the use of EnVision+ System-HRP (DAB) (Dako). Every section was counterstained with hematoxylin. Quantification of CD68-positive cells and desmin staining was evaluated as previously described.15 All of the histological scoring was performed in a blinded manner.
Transmission electron microscopy
For electron microscopy analysis, fresh kidney tissues were fixed with ice-cold buffer containing 4% paraformaldehyde, 5% glutaraldehyde and 0.2 M Phosphate buffer (pH 7.4). The tissues were visualized as described previously.15
Statistical analysis
Values are reported as the means±s.e.m. Statistical analysis was performed using one-way analysis of variance. Analysis of variance (Kruskal–Wallis test, followed by Mann–Whitney U-test) was used for statistical comparisons. We considered that the differences were significant when the probability value was <0.05.
Results
Short-term effects of iron chelation with DFX in CKD rats
Initially, to examine the safety and renal effects of iron chelation with DFX in CKD rats, we administered three doses of DFX in chow (low dose (15 mg kg−1 day−1), moderate dose (30 mg kg−1 day−1) and high dose (60 mg kg−1 day−1)) for 3 weeks to CKD rats. At 6 weeks after surgery, body weight was not different among the groups (Figure 1a). CKD rats exhibited increase in SBP, and all doses of DFX administration did not change this increase in SBP (Figure 1b). Increased proteinuria, serum BUN and creatinine levels were observed in CKD rats compared with the control group, and all doses of DFX did not affect these changes in CKD rats (Figures 1c and e). Histological analysis showed that glomerulosclerosis and increased renal interstitial fibrosis were observed in CKD rats and all doses of DFX did not change glomerulosclerosis in CKD rats (Figures 1f and g). Moderate and high dose of DFX tended to attenuate renal interstitial fibrosis in CKD rats (Figures 1f and g). As shown in Table 1, blood hemoglobin content and hematocrit value were decreased in CKD rats compared with the control group, but the differences were not statistically significant. All doses of DFX administration did not worsen these parameters. Serum iron levels were not different among the groups.
Short-term effects of several doses of DFX in CKD Rats. (a) Body weight, (b) systolic blood pressure, (c) urinary protein excretion, (d) serum BUN levels and (e) serum creatinine levels in the control, CKD, CKD+DFX (15 mg kg−1 day−1), CKD+DFX (30 mg kg−1 day−1) and CKD+DFX (60 mg kg−1 day−1) groups (n=4 in each group). (f) Representative images of PAS and MT staining of the kidney sections. Upper panels show PAS staining (Scale bar, 50 μm). Middle panels show low magnification view of MT staining (Scale bar, 200 μm). Lower panels show high magnification view of MT staining (Scale bar, 100 μm). (g) Quantitative analysis of glomerular sclerosis score and tubular lesion score in the control, CKD, CKD+DFX (15 mg kg−1 day−1), CKD+DFX (30 mg kg−1 day−1), and CKD+DFX (60 mg kg−1 day−1) groups (n=4 in each group). PAS, periodic acid-Schiff; MT, Masson’s trichrome; Control, Sham-operated rats fed a normal diet; CKD, 5/6 nephrectomized rats fed a normal diet; CKD+DFX15, 5/6 nephrectomized rats administered DFX (15 mg kg−1 day−1); CKD+DFX30, 5/6 nephrectomized rats administered DFX (30 mg kg−1 day−1); CKD+DFX60, 5/6 nephrectomized rats administered DFX (60 mg kg−1 day−1). *P<0.05 vs. the control group. A full color version of this figure is available at Hypertension Research online.
Long-term effects of iron chelation on physiological parameters and proteinuria in CKD rats
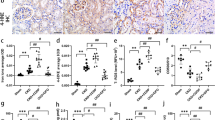
Next, to investigate the association between renal iron accumulation and renal interstitial fibrosis in CKD, we administered moderate dose (30 mg kg−1 day−1) of DFX for 8 weeks to CKD rats. At 16 weeks after surgery, body weight did not differ among the three groups (Figure 2a). DFX administration did not affect the increase in SBP of CKD rats (Figure 2b). CKD rats showed increase in urinary volume compared with the control group, and iron chelation did not change this increment in urinary volume (Figure 2c). Meanwhile, urinary iron excretion was increased in CKD rats compared with the control group, and iron chelation led to further increase of urinary iron excretion in CKD rats (Figure 2d). In addition, iron accumulation was increased in the tubules of CKD rats compared with the control group, whereas iron chelation reduced iron accumulation in the tubules of CKD rats (Figures 2e and f). Renal iron content was increased in CKD rats, and it was decreased in CKD+DFX rats (Figure 2g). In contrast, as shown in Table 2, normocytic normochromic anemia was observed in CKD and CKD+DFX rats. Serum iron levels were not different among the groups.
Long-term effects of iron chelation with DFX on physiological parameters in CKD Rats. (a) Body weight, (b) systolic blood pressure, (c) urinary volume and (d) urinary iron excretion in the control, CKD and CKD+DFX groups (n=6 in each group). (e) Representative images of berlin blue staining of the kidney sections. Scale bar, 200 μm. (f) Quantitative analysis of renal iron deposits score and (g) renal iron content in the control, CKD and CKD+DFX groups (n=4–6 in each group). Control, Sham-operated rats fed a normal diet; CKD, 5/6 nephrectomized rats fed a normal diet; CKD+DFX, 5/6 nephrectomized rats administered DFX (30 mg kg− 1 day−1). *P<0.05 vs. the control group, †P<0.05 vs. the CKD group. A full color version of this figure is available at Hypertension Research online.
Proteinuria was progressively increased in CKD rats after surgery, and iron chelation with DFX did not suppress the increment of proteinuria (Figure 3a). Serum BUN and creatinine levels were also increased in CKD rats, and DFX administration did not affect these increments (Figure 3b). Periodic acid-Schiff staining demonstrated that iron chelation did not change glomerulosclerosis in the CKD kidney (Figures 4a and b). Moreover, desmin staining and transmission electron microscopy revealed that iron chelation did not attenuate the progression of glomerular podocyte injury in CKD rats (Figures 4a and b). Collectively, these data indicate that iron chelation with DFX does not affect hypertension, proteinuria, glomerulosclerosis and podocyte injury in CKD rats.
Long-term effects of iron chelation with DFX on proteinuria in CKD Rats. (a) Time course of urinary total protein excretion in the control (white circle), CKD (black square) and CKD+DFX (white triangle) groups (n=6 in each group). (b) Serum BUN and creatinine levels in the control, CKD and CKD+DFX groups (n=6 in each group). Control, Sham-operated rats fed a normal diet; CKD, 5/6 nephrectomized rats fed a normal diet; CKD+DFX, 5/6 nephrectomized rats administered DFX (30 mg kg− 1 day−1). *P<0.05 vs. the control group.
Long-term effects of iron chelation with DFX on renal structure in CKD Rats. (a) Representative images of PAS, desmin staining and electron microscopy of the kidney sections. (Box area in EM is showing high-magnification view of dashed square area in low-magnification view.) Scale bar, 50 μm. (b) Quantitative analysis of glomerular sclerosis score and desmin-positive cells in the control, CKD and CKD+DFX groups (n=6 in each group). PAS, periodic acid-Schiff staining; EM, electron microscopy. Control, Sham-operated rats fed a normal diet; CKD, 5/6 nephrectomized rats fed a normal diet; CKD+DFX, 5/6 nephrectomized rats administered DFX (30 mg kg− 1 day−1). *P<0.05 vs. the control group. A full color version of this figure is available at Hypertension Research online.
Long-term effects of iron chelation on renal interstitial fibrosis in CKD rats
Next, we evaluated long-term effects of iron chelation with DFX on renal interstitial fibrosis and inflammation in CKD rats. Masson’s trichrome staining showed that renal interstitial fibrosis was increased in CKD rats; however, it was attenuated by iron chelation with DFX (Figures 5a and b). Consistently, iron chelation suppressed the increased gene expression levels of collagen type III and PAI-1 in the kidney of CKD rats (Figure 5c). Moreover, we found a decrease in vimentin along an increase in E-cadherin in renal gene expression of CKD rats with iron chelation, as compared with CKD rats (Figure 5c).
Long-term effects of iron chelation with DFX on renal interstitial fibrosis in CKD Rats. (a) Representative images of Masson’s trichrome staining of the kidney sections. Upper panels show low-magnification view (Scale bar, 200 μm). Lower panels show high-magnification view (Scale bar, 100 μm). (b) Quantitative analysis of tubular lesion score and (c) renal gene expression of Collagen III, PAI-1, Vimentin and E-cadherin in the Control, CKD and CKD+DFX groups (n=4–6 in each group). (d) Renal expression of TGF-β gene and Smad3 protein, and (e) renal gene expression of p22phox and gp91phox in the control, CKD and CKD+DFX groups (n=4–6 in each group). Gene expression of Collagen III, PAI-1, Vimentin, E-cadherin, TGF-β, p22phox and gp91phox was normalized with GAPDH gene expression, and relative levels of gene expression are shown in the graph. Protein expression of Smad3 was standardized on the basis of GAPDH expression, and the relative levels of expression are plotted in the graphs. Control, Sham-operated rats fed a normal diet; CKD, 5/6 nephrectomized rats fed a normal diet; CKD+DFX, 5/6 nephrectomized rats administered DFX (30 mg kg− 1 day−1). *P<0.05 vs. the control group, †P<0.05 vs. the CKD group. A full color version of this figure is available at Hypertension Research online.
TGF-β pathway (TGF-β and Smad3) and oxidative stress pathway (nicotinamide adenine dinucleotide phosphate (NADPH) oxidase) are known to be involved in the pathogenesis of fibrosis in the kidney.21, 22 Renal expression of TGF-β gene and Smad3 protein was increased in CKD rats, while it was attenuated by iron chelation (Figure 5d). In addition, renal gene expression of p22phox and gp91phox was increased in CKD rats. Iron chelation did not affect increased p22phox gene expression, while it attenuated increased gp91phox gene expression in the kidney of CKD rats (Figure 5e).
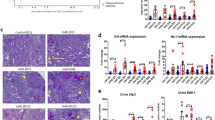
Inflammation also has a role in the development of renal fibrosis.23 CKD rats showed increased CD68-positive cells in the kidney, whereas its increase was attenuated by iron chelation with DFX (Figures 6a and b). Consistent with these findings, iron chelation suppressed the increased gene expression levels of CD68, TNF-α and MCP-1 in the kidney of CKD rats (Figure 6c).
Long-term effects of iron chelation with DFX on renal inflammation in CKD rats. (a) Representative images of CD68 staining of the kidney sections. Upper panels show low-magnification view (Scale bar, 200 μm). Lower panels show high-magnification view (Scale bar, 100 μm). (b) Quantitative analysis of CD68-positive cells score and renal gene expression of (c) CD68, TNF-α and MCP-1 in the control, CKD and CKD+DFX groups (n=4–6 in each group). Renal (d) LCN2 gene and (e) LCN2 protein expression in the control, CKD and CKD+DFX groups (n=4–6 in each group). Gene expression of CD68, TNF-α, MCP-1 and LCN2 was normalized with GAPDH gene expression, and relative levels of gene expression are shown in the graph. Protein expression of LCN2 was standardized on the basis of β-actin expression, and the relative levels of expression are plotted in the graphs. Control, Sham-operated rats fed a normal diet; CKD, 5/6 nephrectomized rats fed a normal diet; CKD+DFX, 5/6 nephrectomized rats administered DFX (30 mg kg− 1 day−1). *P<0.05 vs. the control group, †P<0.05 vs. the CKD group. A full color version of this figure is available at Hypertension Research online.
To further investigate the effects of iron chelation on renal intestinal fibrosis in CKD rats, we assessed renal LCN2 expression in these groups. LCN2 is one of the key effectors of renal damage and one of the biomarkers of CKD progression.24 Renal LCN2 gene and protein expression levels were increased in CKD rats as compared with the control group, whereas these increments were suppressed by iron chelation with DFX (Figures 6d and e).
Discussion
This study showed that iron chelation with DFX attenuated the progression of renal intestinal fibrosis in a rat model of CKD. Iron chelation did not affect hypertension, proteinuria, glomerulosclerosis and podocyte injury in CKD rats, while iron chelation suppressed the progression of renal interstitial fibrosis in CKD rats.
Iron is essential for many biological reactions; however, excess iron makes toxic by generating free radicals. Therefore, it is important to consider the role of iron in the pathophysiology of various diseases. In this study, we showed increased renal iron accumulation and urinary iron excretion in CKD rats. Similarly to our study, increased renal iron accumulation and urinary iron excretion have been reported in patients with chronic renal disease3, 4, 25 and animal models of renal diseases.5, 6, 7, 8 Under physiological conditions, circulating iron enters the renal tubular lumen through the glomerulus. Once filtered by the glomerulus, iron is almost completely reabsorbed in the renal tubules to minimize urinary iron loss. In CKD rats, the glomerular barrier and renal tubules are damaged, resulting in increased filtration of iron through the glomerulus, decreased reabsorption of iron from the renal tubules and increased urinary iron excretion.26 Of interest, we have recently reported that dietary iron restriction prevents further deterioration of renal damage in CKD rats.18 In the present study, we found that iron chelation with DFX attenuated the progression of renal interstitial fibrosis in a rat model of CKD. In addition, while this manuscript was in preparation, it was reported that iron chelation with deferoxamine alleviated renal interstitial fibrosis in mice with unilateral ureteral obstruction.27 About the difference between dietary iron restriction and iron chelation by the drugs to reduce iron accumulation in the kidney, the effect of dietary iron restriction is to prevent further iron accumulation in the kidney, while that of iron chelation by the drugs is to deprive iron accumulation in the kidney. Although the effects on renal function were not completely same between dietary iron restriction and iron chelation by the drugs, these findings suggest that renal iron accumulation seems to be associated with the development of renal intestinal fibrosis in CKD.
Renal interstitial fibrosis is a final common feature for various types of end-stage renal diseases.28 The TGF-β and oxidative stress pathways are known to be involved in the pathogenesis of fibrosis in the kidney.21, 22 Increased renal expression of TGF-β gene and Smad3 protein was attenuated by iron chelation. Meanwhile, iron chelation with DFX attenuated increased renal gene expression of gp91phox but not p22phox in CKD rats. Renal cells differentially express NADPH oxidase components: gp91phox is expressed in mesangial cells, podocytes and endothelium; p22phox in mesangial cells, podocytes, endothelial cells, vascular smooth muscle cells and fibroblasts.29 As we extracted total RNA from the whole kidney, this method may affect these results. Inflammation is also considered to have a role in renal interstitial fibrosis.23 In the current study, iron chelation with DFX suppressed renal inflammation in CKD rats. Collectively, these results suggest that iron chelation with DFX might attenuate renal interstitial fibrosis by inhibiting the TGF-β pathway, inflammation and partly oxidative stress in CKD rats. However, iron chelation with DFX did not affect proteinuria, glomerulosclerosis and podocyte injury with decreased renal intestinal fibrosis in CKD rats. Therefore, attenuation of renal interstitial fibrosis by iron chelation may be a secondarily occurring effect that does not contribute to renal damage in itself.
In this study, we could not observe significant effects of DFX on SBP in CKD rats. As we measured blood pressure by the tail-cuff method, this method for measuring blood pressure may partly affect the results. It might be still possible that there would be difference in directly measured telemetric blood pressure, which should be more sensitive than tail-cuff-measured blood pressure.
DFX is developed as an oral iron chelator. Single-center, prospective and open-labeled studies showed the safety and efficacy of another oral iron chelator, deferiprone, in patients with glomerulonephritis and diabetic nephropathy.14 In addition, safety of DFX is reported in patients with CKD undergoing hemodialysis30 and myelodysplastic syndrome;31 however, it is noteworthy that side effect of DFX is mild and reversible increases in serum creatinine levels.31, 32 Fanconi syndrome is also reported as a rare complication (complication rate is 0.1–1%) in both adult and pediatric patients treated with DFX.33 In other words, the effects of DFX on renal function remain controversial. Although DFX administration did not affect serum creatinine levels in CKD rats in the current study, our results could provide a balanced account on the risk/benefit assessment for the use of this iron chelating drug in CKD. As we assessed the effects of DFX on renal function only in a rat model of CKD, further studies are necessary to investigate the effects of DFX on renal function. In this regard, our observations differ from a previous report that DFX led to increased urinary protein and glucose excretion, and increased tubular damage markers in Wistar rats.34 The differences between these results may depend on differences in the experimental protocol. Sánchez-González et al.34 provided high dose of DFX intraperitoneally in normal rats for 1 week, whereas we gave CKD rats three doses of DFX in chow for 3 weeks and moderate dose of DFX in chow for 8 weeks. Since they evaluated renal toxicological effects of DFX in normal rats, the dose of DFX in their experiments (75 mg kg−1 day−1) was higher than the current experiments (15, 30 and 60 mg kg−1 day−1) and the usual doses in patients (20 mg kg−1 day−1). Taken together, these results could provide a careful assessment on the excess dose of DFX.
In conclusion, iron chelation with DFX attenuates the progression of renal interstitial fibrosis in CKD rats. Renal iron accumulation seems to be associated with renal interstitial fibrosis in a rat model of CKD.
References
Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY . Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med 2004; 351: 1296–1305.
Quaggin SE, Kapus A . Scar wars: mapping the fate of epithelial-mesenchymal-myofibroblast transition. Kidney Int 2011; 80: 41–50.
Nankivell BJ, Boadle RA, Harris DC . Iron accumulation in human chronic renal disease. Am J Kidney Dis 1992; 20: 580–584.
Wang H, Nishiya K, Ito H, Hosokawa T, Hashimoto K, Moriki T . Iron deposition in renal biopsy specimens from patients with kidney diseases. Am J Kidney Dis 2001; 38: 1038–1044.
Izuhara Y, Nangaku M, Inagi R, Tominaga N, Aizawa T, Kurokawa K, van Ypersele de Strihou C, Miyata T . Renoprotective properties of angiotensin receptor blockers beyond blood pressure lowering. J Am Soc Nephrol 2005; 16: 3631–3641.
Nankivell BJ, Chen J, Boadle RA, Harris DC . The role of tubular iron accumulation in the remnant kidney. J Am Soc Nephrol 1994; 4: 1598–1607.
Harris DC, Tay C, Nankivell BJ . Lysosomal iron accumulation and tubular damage in rat puromycin nephrosis and ageing. Clin Exp Pharmacol Physiol 1994; 21: 73–81.
Naito Y, Sawada H, Oboshi M, Fujii A, Hirotani S, Iwasaku T, Okuhara Y, Eguchi A, Morisawa D, Ohyanagi M, Tsujino T, Masuyama T . Increased renal iron accumulation in hypertensive nephropathy of salt-loaded hypertensive rats. PLoS ONE 2013; 8: e75906.
Bolli R, Patel BS, Jeroudi MO, Li XY, Triana JF, Lai EK, McCay PB . Iron-mediated radical reactions upon reperfusion contribute to myocardial "stunning". Am J Physiol 1990; 259: H1901–H1911.
Reddy BR, Kloner RA, Przyklenk K . Early treatment with deferoxamine limits myocardial ischemic/reperfusion injury. Free Radic Biol Med 1989; 7: 45–52.
Ritter C, Reinke A, Andrades M, Martins MR, Rocha J, Menna-Barreto S, Quevedo J, Moreira JC, Dal-Pizzol F . Protective effect of N-acetylcysteine and deferoxamine on carbon tetrachloride-induced acute hepatic failure in rats. Crit Care Med 2004; 32: 2079–2083.
Bulucu F, Oktenli C, Kenar L, Ocal R, Koc B, Inal V, Yamanel L, Yaman H, Sanisoglu YS, Aydin A . Efficacy of deferoxamine, N-acetylcysteine and selenium treatments in rats with adriamycin-induced nephrotic syndrome. J Nephrol 2008; 21: 576–583.
Molina-Jijón E, Zarco-Márquez G, Medina-Campos ON, Zataraín-Barrón ZL, Hernández-Pando R, Pinzón E, Zavaleta RM, Tapia E, Pedraza-Chaverri J . Deferoxamine pretreatment prevents Cr(VI)-induced nephrotoxicity and oxidant stress: role of Cr(VI) chelation. Toxicology 2012; 291: 93–101.
Rajapurkar MM, Hegde U, Bhattacharya A, Alam MG, Shah SV . Effect of deferiprone, an oral iron chelator, in diabetic and non-diabetic glomerular disease. Toxicol Mech Methods 2013; 23: 5–10.
Naito Y, Fujii A, Sawada H, Hirotani S, Iwasaku T, Eguchi A, Ohyanagi M, Tsujino T, Masuyama T . Effect of iron restriction on renal damage and mineralocorticoid receptor signaling in a rat model of chronic kidney disease. J Hypetens 2012; 30: 2192–2201.
Naito Y, Hirotani S, Sawada H, Akahori H, Tsujino T, Masuyama T . Dietary iron restriction prevents hypertensive cardiovascular remodeling in Dahl salt-sensitive rats. Hypertension 2011; 57: 497–504.
Chen X, Mori T, Guo Q, Hu C, Ohsaki Y, Yoneki Y, Zhu W, Jiang Y, Endo S, Nakayama K, Ogawa S, Nakayama M, Miyata T, Ito S . Carbonyl stress induces hypertension and cardio-renal vascular injury in Dahl salt-sensitive rats. Hypertens Res 2013; 36: 361–367.
Naito Y, Fujii A, Sawada H, Hirotani S, Iwasaku T, Okuhara Y, Eguchi A, Ohyanagi M, Tsujino T, Masuyama T . Dietary iron restriction prevents further deterioration of renal damage in a chronic kidney disease rat model. J Hypetens 2013; 31: 1203–1213.
Hošková L, Málek I, Kautzner J, Honsová E, van Dokkum RP, Husková Z, Vojtíšková A, Varcabová S, Cervenka L, Kopkan L . Tacrolimus-induced hypertension and nephrotoxicity in Fawn-Hooded rats are attenuated by dual inhibition of renin-angiotensin system. Hypertens Res 2014; 37: 724–732.
Pillebout E, Weitzman JB, Burtin M, Martino C, Federici P, Yaniv M, Friedlander G, Terzi F . JunD protects against chronic kidney disease by regulating paracrine mitogens. J Clin Invest 2003; 112: 843–852.
Sato M, Muragaki Y, Saika S, Roberts AB, Ooshima A . Targeted disruption of TGF-beta1/Smad3 signaling protects against renal tubulointerstitial fibrosis induced by unilateral ureteral obstruction. J Clin Invest 2003; 112: 1486–1494.
Oberg BP, McMenamin E, Lucas FL, McMonagle E, Morrow J, Ikizler TA, Himmelfarb J . Increased prevalence of oxidant stress and inflammation in patients with moderate to severe chronic kidney disease. Kidney Int 2004; 65: 1009–1016.
Rodríguez-Iturbe B, García García G . The role of tubulointerstitial inflammation in the progression of chronic renal failure. Nephron Clin Pract 2010; 116: c81–c88.
Viau A, El Karoui K, Laouari D, Burtin M, Nguyen C, Mori K, Pillebout E, Berger T, Mak TW, Knebelmann B, Friedlander G, Barasch J, Terzi F . Lipocalin 2 is essential for chronic kidney disease progression in mice and humans. J Clin Invest 2010; 120: 4065–4076.
Goraya N, Simoni J, Jo C, Wesson DE . Dietary acid reduction with fruits and vegetables or bicarbonate attenuates kidney injury in patients with a moderately reduced glomerular filtration rate due to hypertensive nephropathy. Kidney Int 2012; 81: 86–93.
Martines AM, Masereeuw R, Tjalsma H, Hoenderop JG, Wetzels JF, Swinkels DW . Iron metabolism in the pathogenesis of iron-induced kidney injury. Nat Rev Nephrol 2013; 9: 385–398.
Ikeda Y, Ozono I, Tajima S, Imao M, Horinouchi Y, Izawa-Ishizawa Y, Kihira Y, Miyamoto L, Ishizawa K, Tsuchiya K, Tamaki T . Iron chelation by deferoxamine prevents renal interstitial fibrosis in mice with unilateral ureteral obstruction. PLoS ONE 2014; 9: e89355.
Nath KA . Tubulointerstitial changes as a major determinant in the progression of renal damage. Am J Kidney Dis 1992; 20: 1–7.
Gill PS, Wilcox CS . NADPH oxidases in the kidney. Antioxid Redox Signal 2006; 8: 1597–1607.
Maker GL, Siva B, Batty KT, Trengove RD, Ferrari P, Olynyk JK . Pharmacokinetics and safety of deferasirox in subjects with chronic kidney disease undergoing haemodialysis. Nephrology (Carlton) 2013; 18: 188–193.
Breccia M, Alimena G . Efficacy and safety of deferasirox in myelodysplastic syndromes. Ann Hematol 2013; 92: 863–870.
Kontoghiorghes GJ . Introduction of higher doses of deferasirox: better efficacy but not effective iron removal from the heart and increased risks of serious toxicities. Expert Opin Drug Saf 2010; 9: 633–641.
Murphy N, Elramah M, Vats H, Zhong W, Chan MR . A case report of deferasirox-induced kidney injury and Fanconi syndrome. WMJ 2013; 112: 177–180.
Sánchez-González PD, López-Hernandez FJ, Morales AI, Macías-Nuñez JF, López-Novoa JM . Effects of deferasirox on renal function and renal epithelial cell death. Toxicol Lett 2011; 203: 154–161.
Acknowledgements
We thank Noriko Kumon, Sachi Ito and Manami Hosokawa for their technical assistance. This study was supported by a grant from Hyogo Science and Technology Association (to Y. Naito).
Disclaimer
The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
There authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Naito, Y., Fujii, A., Sawada, H. et al. Association between renal iron accumulation and renal interstitial fibrosis in a rat model of chronic kidney disease. Hypertens Res 38, 463–470 (2015). https://doi.org/10.1038/hr.2015.14
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2015.14
Keywords
This article is cited by
-
Ferroptosis and cuproptposis in kidney Diseases: dysfunction of cell metabolism
Apoptosis (2024)
-
Vitexin attenuates chronic kidney disease by inhibiting renal tubular epithelial cell ferroptosis via NRF2 activation
Molecular Medicine (2023)
-
Impact of iron status on kidney outcomes in kidney transplant recipients
Scientific Reports (2023)
-
Angiotensin II type-1 receptor-associated protein interacts with transferrin receptor-1 and promotes its internalization
Scientific Reports (2022)
-
Kidney tubule iron loading in experimental focal segmental glomerulosclerosis
Scientific Reports (2022)