Abstract
Hypertensive disorders in pregnancy (HDP) represent some of the most important problems faced by public health because HDP is a major cause of maternal and prenatal morbidity and mortality. Several epidemiological studies have been performed to determine the prevalence and risk factors of HDP as well as its subtypes. The prevalences of HDP, gestational hypertension and preeclampsia are 5.2–8.2%, 1.8–4.4% and 0.2–9.2%, respectively. Body mass index, anemia and lower education appear to be modifiable risk factors for HDP. Maternal age, primiparous, multiple pregnancy, HDP in previous pregnancy, gestational diabetes mellitus, preexisting hypertension, preexisting type 2 diabetes mellitus, preexisting urinary tract infection and a family history of hypertension, type 2 diabetes mellitus and preeclampsia appear to be nonmodifiable risk factors. Genetic variants including a single-nucleotide polymorphism in the angiotensinogen gene have also been reported to be nonmodifiable risk factors. Epidemiological studies have recently examined the associations between a history of HDP and its subtypes and future risks of other diseases. These studies have reported associations between a history of HDP and a risk of coronary heart disease, heart failure, dysrhythmia, stroke, hypertension, diabetes mellitus, end-stage renal dysfunction and cardiomyopathy. HDP is not associated with the future incidence of total cancer. In conclusion, HDP is not a rare complication of pregnancy and the influence of HDP remains for an extended duration. Physicians should consider the effects of HDP when treating chronic diseases in women.
Similar content being viewed by others
Introduction
Hypertensive disorders in pregnancy (HDP) remain one of the most important problems in public health as well as perinatal medicine. HDP is a major cause of maternal and prenatal morbidity and mortality.1, 2, 3 HDP is thought to be a kind of syndrome, composed of some types of diseases that are respectively caused by confluence of both genetic and acquired factors.4 HDP has previously been defined as a subtype of toxemia of pregnancy that consists of one or more symptoms of hypertension, proteinuria and edema during pregnancy. There has been little consensus regarding international classifications; however, various classifications have been described.5, 6, 7 A Japanese consensus for pregnancy-induced hypertension (PIH), proposed in 2004, consists of 4 subtypes according to symptoms and onset: gestational hypertension (GH), preeclampsia (PE), superimposed preeclampsia and eclampsia.8 GH is defined as hypertension (systolic blood pressure (SBP) of ⩾140 mm Hg and/or diastolic blood pressure (DBP) of ⩾90 mm Hg) at ⩾20 weeks of gestation and recover ⩽12 weeks after delivery. PE is defined as hypertension with proteinuria (excretion of ⩾300 mg protein per day) at ⩾20 weeks of gestation and recovery ⩽12 weeks after delivery. Superimposed preeclampsia is defined as: (1) proteinuria at ⩾20 weeks of gestation superimposed on chronic hypertension present at <20 weeks of gestation and /or before pregnancy, or (2) the deterioration of hypertension and/or proteinuria at ⩾20 weeks of gestation in patients with chronic hypertension with proteinuria at <20 weeks of gestation or (3) GH occurring in renal disease only with proteinuria at <20 weeks of gestation and/or before pregnancy. Eclampsia is defined as the onset of seizures at ⩾20 weeks of gestation without convulsion or secondary seizures.8 Effective treatment is needed for women with severe HDP because worsening of HDP may cause maternal cardiovascular events and death9, 10, 11 as well as placental dysfunction.
Several epidemiological studies have examined the prevalence,12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30 risk factors13, 14, 21, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52 and predictors53, 54, 55, 56, 57, 58, 59 of HDP and its subtypes. Many epidemiological studies examined the associations between the history of HDP and its subtypes and future risks of other diseases.60, 61, 62, 63, 64, 65, 66, 67, 68, 69, 70, 71, 72, 73, 74
In this review, we provide information regarding the prevalence, risk factors, predictors and future risks of other diseases of HDP and its subtypes; we primarily focus on GH and PE because they are major HDP subtypes.
Prevalence
Prevalence
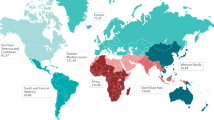
Table 1 shows the prevalence of HDP and its subtypes from epidemiological studies. The prevalences of HDP, PIH, GH and PE are 5.2–8.2%, 4.1–19.4%, 1.8–4.4% and 0.2–9.2%, respectively, in all pregnancies.12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30 According to region, the prevalence of PE is 0.5–2.3% in Africa, 0.2–6.7% in Asia, 2.8–9.2% in Oceania, 2.8–5.2% in Europe, 2.6–4.0% in North America and 1.8–7.7% in South America and the Caribbean.
Seasonal effects
Several studies have examined the seasonal variation in the prevalence of HDP and its subtypes. The prevalence of HDP and PIH is high for delivery in winter or early spring among Japanese, Chinese and Australian subjects.12, 14, 18 For Kuwaiti subjects, the prevalence of PIH is high in June; however, the prevalence of PE is high in November.16 The prevalence of PE is high for delivery in winter in Norwegian, Swedish and American subjects.20, 21, 22, 23 For Australian subjects, the prevalence of PE is high in spring to summer.18 A study of Indian subjects has examined the difference in the prevalence of PE between the monsoon season and the dry season and has found no differences in prevalence.15
Risk factors of HDP
Modifiable factors
Body mass index
A positive association between higher prepregnancy body mass index (BMI) and the prevalence of HDP has been reported in Chinese subjects.13 Compared with subjects with a prepregnancy BMI of <24.0 kg m−2, subjects with a prepregnancy BMI of 24.0–27.9 and ⩾28.0 kg m−2 showed a 1.79- and 3.11-fold higher prevalence of HDP, respectively.13 A study of Pakistani and White British women has shown that a 5 kg m−2 increase in BMI is associated with a 1.54- and 1.60-fold higher prevalence of HDP.19 The association between higher prepregnancy BMI and the prevalence of PE has also been examined. A retrospective study of Taiwanese has found that subjects with a BMI of >24.2 and <19.8 kg m−2 were at a 2.4- and 0.6-fold higher risk of PE compared with subjects with a BMI of 19.8–24.2 kg m−2.26 A meta-analysis of 29 prospective cohort studies has reported that subjects with a BMI of <20.0, 25.0–29.9, 30.0–34.9 and ⩾35.0 kg m−2 had a 0.77-, 1.70-, 2.93- and 4.14-fold higher risk of PE compared with subjects with a BMI of 20.0–24.9 kg m−2, respectively.40
Anemia
A cross-sectional study using the database of the World Health Organization Multicountry Survey (WHOMCS) on maternal and newborn health has reported that subjects with anemia had a 4.06-fold times higher risk of PE than subjects who were anemic.28
Smoking
A population-based cohort study of Swedish subjects has reported a lower risk of GH and PE among subjects who smoked cigarettes compared with those who did not smoke.21 The odds ratios of subjects who smoked 1–9 and ⩾10 cigarettes per day were 0.86 and 0.48 for GH and 0.64 and 0.55 for PE, respectively, compared with subjects who did not.21 A retrospective study of Australian subjects has also shown 1.57-fold higher risk of GH among subjects with habitual smoking compared with subjects who were not habitual smokers.39 Systematic reviews and a meta-analysis have shown an inverse association between cigarette smoking and the risk of PE.41, 42 Subjects who habitually smoked during pregnancy showed a 0.67-fold lower risk of PE compared with subjects who were not habitual smokers.42 However, for PIH, a recent study based on a Japanese perinatal registry has shown that subjects who smoked during pregnancy had a 1.20-fold higher risk for PIH compared with subjects who did not smoke during pregnancy.29 Our case–control study of Japanese subjects has also shown that in a subgroup with a prepregnancy BMI of ⩾24.0 kg m−2, the frequency of smoking before pregnancy was significantly higher in women with PE than in controls.43
Alcohol intake
A cross-sectional study of Chinese subjects had shown a positive association between alcohol intake and the risk of HDP.13 Subjects with alcohol intake showed a 1.75-fold higher risk of HDP compared with subjects without alcohol intake.13 A prospective study of Americans has shown that subjects who were habitual drinkers had a 0.55-fold lower risk of PE compared with subjects who did not drink habitually.34
Education
A cross-sectional study of Chinese subjects has shown that those who graduated from university or college had ∼35% lower PIH prevalence compared with subjects who completed elementary school.14 The study based on the WHOMCS database has shown that subjects who went to school for 0 years and 5–8 years has shown 1.20- and 1.21-fold higher risk of PE than subjects who went to school for ⩾11 years;28 however, in this study, the risk of PE among subjects who went to school for 1–4 years, 9–11 years and ⩾11 years was not significantly different.28 Notably, cross-sectional studies of Latin Americans and Taiwanese subjects have shown no association between educational status and the risk of PE.24, 26
Nonmodifiable factors
Maternal age
A positive association between higher maternal age and the risk of HDP has been shown in Chinese subjects.13 Compared with subjects aged 25–29 years, those aged 35–39 and ⩾40 years had a 1.84- and 2.39-fold higher risk of HDP, respectively.13 Higher maternal age was also positively associated with the prevalence of PIH in Chinese subjects.14 Compared with subjects aged 20–34 years, those aged ⩾35 years had an ∼60% higher prevalence of PIH.14 For GH, Australian subjects aged ⩾40 years had a 1.45-fold higher risk of GH compared with subjects aged 30–34 years.39 A higher maternal age was also positively associated with the risk of PE.24, 25, 26, 28 Latin American, Caribbean and Taiwanese women aged ⩾35 years showed 1.67- and 1.8-fold higher risks of PE compared with similar subjects aged 20–34 years.24, 26 The study based on the WHOMCS database has shown that subjects aged >35 years had a 1.78-fold higher risk of PE compared with subjects aged 20–35 years.28 A cross-sectional study of Americans has examined the association between age groups of mothers and the risk of PE stratified by race.25 Subjects of Black and other races aged ⩾35 years showed a 1.7-fold higher risk of PE than those aged 30–34 years. However, this association was not observed among White subjects.25 An epidemiological study of Americans has shown no association between higher maternal age and the risk of PE.31
A positive association between lower maternal age and the prevalence of PE has been shown in both White and non-White American subjects.25 White subjects aged 20–24, 18–19 and 15–17 years had a 1.4-, 1.8- and 2.6-fold higher risk of PE compared with those aged 30–34 years, respectively. Subjects from Black and other races aged 18–19 and 15–17 years had a 2.0- and 2.4-fold higher risk of PE, respectively, compared with subjects aged 30–34 years.25 However, the study based on WHOMCS database has shown an inverse association between lower maternal age and the risk of PE.28 Subjects aged 17–19 years had a 0.72-fold lower risk of PE compared with subjects aged 20–35 years.28 Other epidemiological studies have shown no association between lower maternal age and the prevalence of HDP, PIH or PE.13, 14, 24, 26, 31
Primipara
Women who are primiparous show a higher risk of HDP and PE.13, 24, 26, 28, 31, 34, 39 The study in Chinese subjects has shown that primiparous subjects had a 1.5-fold higher risk of HDP compared with subjects who were not primiparous.13 For PE, primiparous subjects showed a 2.38-, 3.9-, 4.75- and 2.9-fold higher risk of PE in Latin Americans,24 Americans31, 34 and Australians39 compared with multiparous subjects. Studies of Taiwanese subjects have also shown that primiparous subjects had a 1.3-fold higher risk of PE.26 A study based on the WHOMCS database has shown that the number of previous births is inversely associated with the risk of PE. Subjects with 0 and ⩾4 previous births had a 1.42- and 0.83-fold risk of PE compared with subjects with 1–3 births.28
Multiple pregnancy
Multiple pregnancy is associated with a higher risk of HDP, PIH and PE compared with singleton pregnancy.13, 14, 21, 24, 26, 28, 31, 38 Multiple pregnancy has been reported to have a 3.68-fold higher risk of HDP compared with singletons in a study on Chinese subjects.13 The prevalence of PIH is 3.31-fold higher in multiple pregnancy compared with singleton pregnancy.14 For PE, studies of Swedish, Taiwanese, Latin American and Danish populations have shown a 4.17-, 3.6-, 2.10- and 2.3-fold higher risk of PE, respectively, in multiple pregnancy compared with singleton pregnancy.21, 24, 26, 38 The study based on the WHOMCS database has also shown a 2.55-fold higher risk of PE in multiple pregnancy compared with single pregnancy.28
Previous experience of pregnant complications
Studies of Americans have shown a positive association between hypertensive disorders in the first pregnancy and the risk of hypertensive disorders in the second pregnancy.35, 36 A study of Americans has shown that subjects with mild GH (DBP 90–109 mm Hg), severe GH (DBP ⩾110 mm Hg) and PE/eclampsia in the first pregnancy had a 3.0-, 3.4- and 6.3-fold higher risk of hypertension in the second pregnancy, respectively.35 Another study has shown that subjects with borderline hypertension (SBP 130–139 mm Hg and/or DBP 85–89 mm Hg) and hypertension (SBP ⩾140 mm Hg and/or DBP ⩾90 mm Hg) at admission of the first pregnancy had a higher risk of GH and PE in the second pregnancy.36 Subjects who were not GH but were borderline hypertensive at admission of the first pregnancy had a 2.07-fold higher risk of GH and a 2.02-fold higher risk of PE in the second pregnancy. Subjects who were not GH but were hypertensive at admission of the first pregnancy had a 3.42-fold higher risk of GH and a 3.81-fold higher risk of PE in the second pregnancy. The associations were evident among subjects who were GH in the first pregnancy.36 For PE, a systematic review has examined the unadjusted relative risk of previous cohort studies and case–control studies.52 Compared with subjects without PE in previous pregnancy, those with PE in a previous pregnancy had a 7.19-fold higher risk of PE in cohort studies and 7.61-fold higher risk of PE in case–control studies.52
Gestational diabetes mellitus (GDM)
GDM often occurs together with HDP. GDM is associated with a 2.48-fold higher risk of HDP in Chinese population,13 1.87-fold higher risk of GH in Australian population39 and 3.11- and 1.93-fold higher risk of PE in Swedish, Latin American, and Caribbean populations.21, 24
Preexisting disease
Diabetes mellitus (DM) appears to be an important risk factor for HDP. Type 2 DM has been associated with a 2.48-fold higher risk of HDP in Chinese subjects,13 a 3.25-fold higher risk of GH in Australian subjects39 and a 1.93-fold higher risk of PE in Latin American subjects.24 Type 1 DM is also associated with a 5.58-fold higher risk of PE.21 The incidence of HDP is similar in type 1 DM and type 2 DM.37 A study of Danish subjects has shown a negative association between DM and the risk of PE.38 DM is associated with a 0.4- and 0.2-fold lower risk of severe PE in primiparous and multiparous mothers, respectively.38
Chronic hypertension also appears to be an important risk factor for HDP. Subjects with a history of chronic hypertension also had a 1.99- and 8.32-fold higher risk of PE compared with subjects who did not in Latin Americans and in subjects of the WHOMCS database.24, 28 Danish subjects with probable chronic hypertension have been found to shown a 2.2-fold higher risk of PE compared with subjects with no risk factors. Subjects with definite hypertension have also been found to have a 3.4-fold higher risk of PE.38
Urinary tract infection has been reported to be a risk factor of HDP.26, 28 Urinary tract infection during pregnancy has been associated with a 4.8-fold higher risk of PE in Taiwanese subjects.26 A history of pyelonephritis has also been associated with a 1.64-fold higher risk of PE among subjects of the WHOMCS.28 However, another study of Australians has shown no association between urinary tract infection and the risk of GH.39
The study based on the WHOMCS database has shown that histories of heart disease, renal disease and hepatic disease are positively associated with the risk of PE.28 The odds ratios of a history of these diseases are 2.12, 4.52 and 4.07, respectively.
Family history
A family history of hypertension and type 2 DM are reported risk factors of HDP. In Chinese subjects, family history of hypertension and type 2 DM have been associated with a 3.17- and 2.67-fold higher risk of HDP compared with subjects without these conditions.13
A family history of PE has also been reported to be a risk factor of PE. A systematic review has shown that subjects with a family history of PE had a 2.9-fold higher risk of PE compared with subjects without a family history of PE.52
Genetic variants
Many studies have investigated the associations between genetic variants, including single-nucleotide polymorphisms, and HDP. An association with the M235T variant of the angiotensinogen (AGT) gene has been shown in many subjects; however, there are racial differences among these associations. In Caucasian subjects, Ward et al.44 have shown that the frequency of the TT genotype of AGT is significantly higher in primigravid PE (65%) than in primigravid controls (40%). In Japanese subjects, we have found that the frequency of the TT genotype is significantly higher in primigravid PIH 93–94% (93% in PE and 94% in GH) than in primigravid controls (77%).45 Zafarmand et al.46 have performed a questionnaire study of middle-aged Dutch women in a large prospective cohort study. Under both dominant and additive genetic models, the M235T polymorphism has been found to be associated with a history of elevated blood pressure during pregnancy with odds ratios of 1.29 (95% confidence interval, 1.01–1.64; P=0.04) and 1.20 (95% confidence interval, 1.02–1.42; P=0.03), respectively.46 Furthermore, our association studies for Japanese subjects have revealed that the TT genotype of AGT, the heterozygosity of the Glu298Asp variant and homozygosity of the Glu298 genotype of the endothelial nitric oxide synthase 3 (NOS3) gene and prepregnancy BMI of ⩾24 kg m−2 are independently associated with HDP;47 additionally, the TT genotype of AGT and a mentally stressful condition during pregnancy are synergistically associated with HDP.48 Recent studies have reported new candidate genes associated with HDP. An association study including 208 women with PE and 212 healthy pregnant women in Brazil has reported that the T allele of the rs1319501 of the nicotinamide phosphoribosyl transferase (NAMPT) gene is associated with PE (82% in PE vs. 73% in controls, odds ratio=1.626, 95% confidence interval, 1.170–2.257).49 A study of a Chinese Han population including 402 women with PE and 554 healthy pregnant women has reported that the G allele of rs 2228570 of the Vitamin D receptor (VDR) gene is a risk factor for PE (62% in PE vs. 55% in controls, odds ratios=1.137, 95% confidence interval, 1.111–1.610).50 Notably, genome-wide association studies have been carried out; however, the lack of statistical power may have affected the results.51 Further studies with larger sample sizes are expected.
Predictors of HDP
Several epidemiological studies have attempted to determine predictors of HDP, especially with regard to PE.
A meta-analysis has examined the utility of blood pressure in predicting PE during the first or second trimester of pregnancy.54 The mean value of arterial blood pressure is a better predictor of PE than SBP, DBP or an increment in blood pressure during pregnancy for low-risk women.54 A study of Nigerian subjects has shown microalbuminuria appears to be a predictor of PE. However, the sensitivity and specificity of the criteria (urinary albumin excretion ⩾30 mg per 24 h at booking) were 88.9% and 67.9%, respectively.57 In addition, proteinuria does not predict complications of PE.56 Prepregnant BMI and BMI at booking appears to be predictors of PE. However, a meta-analysis has found that BMI is a fairly weak predictor of PE.53 A meta-analysis has shown that hypertriglyceridemia is associated with and precedes the onset of PE.55
Several first-trimester risk prediction models for PE have been developed. However, a systematic review has concluded that the reliability and validity of these models is limited.58
Prognosis of HDP
Cardiovascular disease
A study of Canadians has shown that GH and PE are associated with a 1.8- and 2.1-fold higher risk of future cardiovascular disease.68 A study of Norwegian subjects has shown that PE is associated with a 1.9-fold higher risk of death from cardiovascular disease.69
Coronary heart disease
A study of Finnish subjects has shown that GH is associated with a 1.44-fold higher risk of ischemic heart disease, 1.75-fold higher risk of myocardial infarction and 3.00-fold higher risk of myocardial infarct death60 in the future. A study of Danish subjects has also shown that GH, mild PE and severe PE are associated with a 1.48-, 1.57- and 1.61-fold higher risk of ischemic heart disease, respectively.62 A meta-analysis has shown that PE is associated with a 2.16-fold higher risk of ischemic heart disease.73
Heart failure
A study of Canadian subjects has shown that GH and PE are associated with a 1.83- and 1.56-fold higher risk of heart failure or an atrial or ventricular dysrhythmia in the future.70 A study of Finnish subjects has shown that GH is associated with a 1.78-fold higher risk of heart failure.60 A study of Danish subjects has shown that mild PE and severe PE are associated with a 1.67- and 1.71-fold higher risk of heart failure.62
Stroke
An association between HDP and a future risk of stroke has been reported.60, 62, 71
A prospective study of Finnish subjects has shown that GH is associated with a 1.59-fold higher risk of ischemic stroke.60 A registry-based cohort study of Danish subjects has also shown that GH, mild PE and severe PE are associated with a 1.51-, 1.43- and 1.58-fold higher risk of stroke, respectively.62 A cohort study of Scottish subjects has also shown that GH and PE/eclampsia are associated with a 2.42- and 3.39-fold higher risk of stroke.71 A meta-analysis has shown that PE is associated with a 1.81-fold higher risk of stroke.73
Cancer
A prospective study of Norwegian subjects has shown an inverse association between GH or PE and the risk of breast cancer.61 In this study, subjects with GH or PE in the first pregnancy had a 0.83-fold lower risk of breast cancer compared with subjects without them.61 A registry-based cohort study of Danish subjects has shown that a history of HDP is inversely associated with the risk of lung and breast cancer but that it is positively associated with the risk of endometrial and urinary tract cancer.66 This study has found no association between a history of HDP and the risk of all cancers. A meta-analysis has also reported no association between PE and the risk of any cancer.73
Hypertension
A cohort study of UK subjects has shown that GH and PE/eclampsia are associated with a 2.47- and 3.98-fold higher future risk of hypertension, as diagnosed by a medical doctor.71 The registry-based cohort study of Danish subjects has also shown that GH, mild PE and severe PE are associated with a 5.31-, 3.61- and 6.07-fold higher risk of hypertension, respectively.62 A meta-analysis including the UK study described above has also shown that PE is associated with a 3.70-fold higher risk of hypertension.73
Diabetes mellitus
The prospective study of Finnish subjects has shown that GH is associated with a 1.52-fold higher risk of future DM.60 The registry-based cohort study of Danish subjects has also shown that GH, mild PE and severe PE are associated with a 3.12-, 3.53- and 3.68-fold higher risk of DM, respectively.62
Other diseases
For kidney disease, a prospective study of Taiwanese subjects has shown that a history of HDP is positively associated with a risk of end-stage renal disease in the future.63 HDP and PE are associated with a 1.91- and 2.17-fold higher risk of end-stage renal disease. GH is not significantly associated with the risk of end-stage renal disease.63 PE increases the future risk of microalbuminuria.74 A meta-analysis has reported that PE is associated with a 4.31-fold higher risk of microalbuminuria.74
An association between HDP and a risk of cardiomyopathy has recently been reported.64 In this registry-based cohort study, severe and moderate PE have been found to be positively associated with a risk of cardiomyopathy but not PIH. Severe and moderate PE are associated with a 3.17- and 2.56-fold higher risk of cardiomyopathy.64
Comment
In the present review, we have discussed the prevalence, risk factors, predictors and prognosis of HDP from epidemiological studies.
The prevalence of HDP and its subtypes varies among regions and races, possibly because of differences in genetic factors, lifestyles and social and medical environments among races and countries. A seasonal effect on HDP has been shown in several studies.12, 14, 15, 16, 18, 20, 21, 22, 23 Nearly all studies have shown that the prevalence of HDP is high for delivery in the cold season, whereas the study in Kuwait has shown that the prevalence of PIH is high for delivery in the hot season. The reason for this association is not clear, because these studies have not provided information regarding when HDP occurred. However, according to the definition of PIH, GH and PE, the prevalence of HDP may be high in autumn to winter. For Kuwaiti subjects, the prevalence of PIH may be high in spring to summer. These results suggest that the prevalence of HDP may be associated with burdens following temperature and humidity changes.
The modifiable risk factors of HDP, BMI, anemia and lower education levels are positively associated with the risk of HDP. Of these, anemia is a severe health problem; the WHO (World Health Organization) has reported that ∼30% of women of reproductive age have anemia worldwide.75 Smoking during pregnancy may be inversely associated with the risk of HDP; however, there are positive associations in some populations. Plausible biological mechanisms for the effect of smoking on the pathogenesis of PE have been studied.42 In short, the effects of toxic chemicals in cigarettes on the circulation and placental systems reduce the plasma volume and oxidative stress.42 In addition, smoking during pregnancy appears to be associated with other unfavorable outcomes. For example, a meta-analysis has shown that smoking during pregnancy is associated with a 1.23-fold higher risk of miscarriage.76 Therefore, expecting mothers should avoid smoking. The effect of alcohol intake on HDP is unclear. More evidence is needed to determine the association between alcohol intake and the risk of HDP.
For the nonmodifiable risk factors of HDP, maternal age, primiparous, multiple pregnancy, a history of HDP in a previous pregnancy, GDM, preexisting hypertension, preexisting type 2 DM, preexisting urinary tract infection and a family history of hypertension, type 2 DM and PE are positively associated with the risk of HDP. These results suggest that a precise interview history is important in differentiating women with a high risk of HDP.
Duckitt and Harrington52 have created a list of identified risk factors of PE at antenatal booking visits. The list consists of 10 items: age, parity, previous PE, a family history of PE, multiple pregnancy, preexisting medical conditions (DM, chronic hypertension, renal disease, autoimmune disease and antiphospholipid syndrome), time between pregnancies, BMI, blood pressure level and proteinuria. We suggest that the presence of anemia and urinary tract infection should be added to the 10 items stated above. In addition, complications including HDP and GDM in previous pregnancy should be recorded instead of a history of previous PE.
It is important to notice signs of HDP, especially PE, because early HDP treatment is beneficial for expectant mothers and fetuses. A meta-analysis has shown that the mean values of arterial blood pressure are a better predictor of PE in low-risk women. According to the results of the study, an increase in mean arterial pressure by ⩾90 mm Hg in the second trimester allows detection of high-risk expectant mothers of PE. Microalbuminuria also appears to predict PE. However, 24 h urine collection is not easily performed in a routine maternal health checkup. Therefore, this examination should be performed only in mothers who have several of the above risk factors.
Epidemiological studies have revealed that HDP is associated with future chronic disease risk. HDP is positively associated with the risk of CHD, heart failure, dysrhythmia, stroke, hypertension, DM, end-stage renal disease and cardiomyopathy. HDP is not associated with an incidence of total cancer. However, an association between HDP and the risk of specific cancers has been reported. Breast and lung cancer may be inversely associated with a history of HDP, whereas endometrial and urinary tract cancer may positively associate with a history of HDP.
HDP is thought to be composed of various diseases that occur through the confluence of both genetic and acquired factors. A genetic variant, M235T of AGT, is strongly linked to the G-6A variant in the promoter region; however, the possession of -6A leads to lower promoter activity than -6G.77 Furthermore, the variant contributes to an inadequate trophoblastic invasion of the uterine spiral artery and a narrowing of the spiral arteries in early pregnancy.78 Our previous results indicating that the TT genotype of AGT and a mentally stressful condition during pregnancy are synergistically associated with HDP are consistent with the pathophysiology described above. These results suggest that early prediction using genetic factors and performing appropriate intervention for individuals may be effective for HDP prevention, as well as in preventing future chronic diseases; however, associating genetic factors with diseases differs according to race.
Conclusion
HDP is not a rare complication in pregnancy. The influence of HDP remains for an extended duration after pregnancy. Epidemiological studies have revealed that a history of HDP is associated with a risk of chronic disease, particularly cardiovascular disease. HDP should be treated not only as a maternal and perinatal health problem but also a health problem affecting later life. Early prediction using various risk factors, prevention through appropriate interventions and a long follow-up for women with a history of HDP are important.
References
Khan KS, Wojdyla D, Say L, Gülmezoglu AM, Van Look PF . WHO analysis of causes of maternal death: a systematic review. Lancet 2006; 367: 1066–1074.
Say L, Chou D, Gemmill A, Tunçalp Ö, Moller AB, Daniels J, Gülmezoglu AM, Temmerman M, Alkema L . Global causes of maternal death: a WHO systematic analysis. Lancet Glob Health 2014; 2: e323–e333.
Vogel JP, Souza JP, Mori R, Morisaki N, Lumbiganon P, Laopaiboon M, Ortiz-Panozo E, Hernandez B, Pérez-Cuevas R, Roy M, Mittal S, Cecatti JG, Tunçalp Ö, Gülmezoglu AM WHO Multicountry Survey on Maternal and Newborn Health Research Network. Maternal complications and perinatal mortality: findings of the World Health Organization Multicountry Survey on Maternal and Newborn Health. BJOG 2014; 121 (Suppl 1): 76–88.
Kobashi G . Genetic and environmental factors associated with the development of hypertension in pregnancy. J Epidemiol 2006; 16: 1–8.
Report of the National High Blood Pressure Education Program Working Group on High Blood Pressure in Pregnancy. Am J Obstet Gynecol 2000; 183: S1–S22.
Grown MA, Hague WH, Higgins J, Lowe S, McCowan L, Oats J, Peek MJ, Rowan JA, Walters BN The Australasian Society of the Study of Hypertension in Pregnancy. The detection, investigation and management of hypertension in pregnancy: full consensus statement. Aust N Z J Obstet Gynecol 2000; 40: 133–155.
Brown MA, Lindheimer MD, de Swiet M, Van Assche A, Moutquin JM . The classification and diagnosis of the hypertensive disorders of pregnancy: statement from the International Society for the Study of Hypertension in Pregnancy (ISSHP). Hypertens Pregnancy 2001; 20: ix–xiv.
Ito M . Newly defined/classified pregnancy-induced hypertension: comparison of pregnancy-induced hypertension with previously recognized toxemia of pregnancy. Acta Obst Gynaec Jpn 2006; 58: 1295–1301 (in Japanese).
Sharshar T, Lamy C, Mas JL . Incidence and causes of strokes associated with pregnancy and puerperium. A study in public hospitals of Ile de France. Stroke in Pregnancy Study Group. Stroke 1995; 26: 930–936.
Mongraw-Chaffin ML, Cirillo PM, Cohn BA . Preeclampsia and cardiovascular disease death: prospective evidence from the child health and development studies cohort. Hypertension 2010; 56: 166–171.
Cantwell R, Clutton-Brock T, Cooper G, Dawson A, Drife J, Garrod D, Harper A, Hulbert D, Lucas S, McClure J, Millward-Sadler H, Neilson J, Nelson-Piercy C, Norman J, O’Herlihy C, Oates M, Shakespeare J, de Swiet M, Williamson C, Beale V, Knight M, Lennox C, Miller A, Parmar D, Rogers J, Springett A . Saving mothers’ lives: reviewing maternal deaths to make motherhood safer: 2006–2008. The Eighth Report of the Confidential Enquiries into Maternal Deaths in the United Kingdom. BJOG 2011; 118 (Suppl 1): 1–203.
Morikawa M, Yamada T, Yamada T, Cho K, Sato S, Minakami H . Seasonal variation in the prevalence of pregnancy-induced hypertension in Japanese women. J Obstet Gynaecol Res 2014; 40: 926–931.
Ye C, Ruan Y, Zou L, Li G, Li C, Chen Y, Jia C, Megson IL, Wei J, Zhang W . The 2011 survey on hypertensive disorders of pregnancy (HDP) in China: prevalence, risk factors, complications, pregnancy and perinatal outcomes. PLoS ONE 2014; 9: e100180.
Ma R, Liu JM, Li S, Ye RW, Chen H, Xue MJ, Wang TM, Cheng LC, Zheng JC, Wu LM, Pan YJ, Chen H, Li Z . Study on the descriptive epidemiology of pregnancy-induced hypertension from 1995–2000 in Jiaxing of Zhejiang province, China. Zhonghua Liu Xing Bing Xue Za Zhi 2005; 26: 960–963 (in Chinese).
Subramaniam V . Seasonal variation in the incidence of preeclampsia and eclampsia in tropical climatic conditions. BMC Womens Health 2007; 7: 18.
Makhseed M, Musini VM, Ahmed MA, Monem RA . Influence of seasonal variation on pregnancy-induced hypertension and/or preeclampsia. Aust N Z J Obstet Gynaecol 1999; 39: 196–199.
Muti M, Tshimanga M, Notion GT, Bangure D, Chonzi P . Prevalence of pregnancy induced hypertension and pregnancy outcomes among women seeking maternity services in Harare, Zimbabwe. BMC Cardiovasc Disord 2015; 15: 111.
Algert CS, Roberts CL, Shand AW, Morris JM, Ford JB . Seasonal variation in pregnancy hypertension is correlated with sunlight intensity. Am J Obstet Gynecol 2010; 203: 215.e1–5.
Bryant M, Santorelli G, Lawlor DA, Farrar D, Tuffnell D, Bhopal R, Wright J . A comparison of South Asian specific and established BMI thresholds for determining obesity prevalence in pregnancy and predicting pregnancy complications: findings from the Born in Bradford cohort. Int J Obes (Lond) 2014; 38: 444–450.
Magnus P, Eskild A . Seasonal variation in the occurrence of pre-eclampsia. BJOG 2001; 108: 1116–1119.
Ros HS, Cnattingius S, Lipworth L . Comparison of risk factors for preeclampsia and gestational hypertension in a population-based cohort study. Am J Epidemiol 1998; 147: 1062–1070.
Wellington K, Mulla ZD . Seasonal trend in the occurrence of preeclampsia and eclampsia in Texas. Am J Hypertens 2012; 25: 115–119.
Bodnar LM, Catov JM, Roberts JM . Racial/ethnic differences in the monthly variation of preeclampsia incidence. Am J Obstet Gynecol 2007; 196: 324.e1–5.
Conde-Agudelo A, Belizán JM . Risk factors for pre-eclampsia in a large cohort of Latin American and Caribbean women. BJOG 2000; 107: 75–83.
Saftlas AF, Olson DR, Franks AL, Atrash HK, Pokras R . Epidemiology of preeclampsia and eclampsia in the United States, 1979–1986. Am J Obstet Gynecol 1990; 163: 460–465.
Lee CJ, Hsieh TT, Chiu TH, Chen KC, Lo LM, Hung TH . Risk factors for pre-eclampsia in an Asian population. Int J Gynaecol Obstet 2000; 70: 327–333.
Cincotta RB, Brennecke SP . Family history of pre-eclampsia as a predictor for pre-eclampsia in primigravidas. Int J Gynaecol Obstet 1998; 60: 23–27.
Abalos E, Cuesta C, Carroli G, Qureshi Z, Widmer M, Vogel JP, Souza JP WHO Multicountry Survey on Maternal and Newborn Health Research Network. Pre-eclampsia, eclampsia and adverse maternal and perinatal outcomes: a secondary analysis of the World Health Organization Multicountry Survey on Maternal and Newborn Health. BJOG 2014; 121 (Suppl 1): 14–24.
Hayashi K, Matsuda Y, Kawamichi Y, Shiozaki A, Saito S . Smoking during pregnancy increases risks of various obstetric complications: a case-cohort study of the Japan Perinatal Registry Network database. J Epidemiol 2011; 21: 61–66.
Taebi M, Sadat Z, Saberi F, Kalahroudi MA . Early pregnancy waist-to-hip ratio and risk of preeclampsia: a prospective cohort study. Hypertens Res 2015; 38: 80–83.
Coonrod DV, Hickok DE, Zhu K, Easterling TR, Daling JR . Risk factors for preeclampsia in twin pregnancies: a population-based cohort study. Obstet Gynecol 1995; 85 (5 Pt 1): 645–650.
McDonald SD, Best C, Lam K . The recurrence risk of severe de novo pre-eclampsia in singleton pregnancies: a population-based cohort. BJOG 2009; 116: 1578–1584.
Olafsdottir AS, Skuladottir GV, Thorsdottir I, Hauksson A, Thorgeirsdottir H, Steingrimsdottir L . Relationship between high consumption of marine fatty acids in early pregnancy and hypertensive disorders in pregnancy. BJOG 2006; 113: 301–309.
Eskenazi B, Fenster L, Sidney S . A multivariate analysis of risk factors for preeclampsia. JAMA 1991; 266: 237–241.
Zhang J, Troendle JF, Levine RJ . Risks of hypertensive disorders in the second pregnancy. Paediatr Perinat Epidemiol 2001; 15: 226–231.
Boghossian NS, Albert PS, Mendola P, Grantz KL, Yeung E . Delivery blood pressure and other first pregnancy risk factors in relation to hypertensive disorders in second pregnancies. Am J Hypertens 2015; 28: 1172–1179.
Cundy T, Slee F, Gamble G, Neale L . Hypertensive disorders of pregnancy in women with Type 1 and Type 2 diabetes. Diabet Med 2002; 19: 482–489.
Catov JM, Ness RB, Kip KE, Olsen J . Risk of early or severe pre-eclampsia related to pre-existing conditions. Int J Epidemiol 2007; 36: 412–419.
Jacobs DJ, Vreeburg SA, Dekker GA, Heard AR, Priest KR, Chan A . Risk factors for hypertension during pregnancy in South Australia. Aust N Z J Obstet Gynaecol 2003; 43: 421–428.
Wang Z, Wang P, Liu H, He X, Zhang J, Yan H, Xu D, Wang B . Maternal adiposity as an independent risk factor for pre-eclampsia: a meta-analysis of prospective cohort studies. Obes Rev 2013; 14: 508–521.
Conde-Agudelo A, Althabe F, Belizán JM, Kafury-Goeta AC . Cigarette smoking during pregnancy and risk of preeclampsia: a systematic review. Am J Obstet Gynecol 1999; 181: 1026–1035.
Wei J, Liu CX, Gong TT, Wu QJ, Wu L . Cigarette smoking during pregnancy and preeclampsia risk: a systematic review and meta-analysis of prospective studies. Oncotarget 2015; 6: 43667–43678.
Kobashi G, Ohta K, Hata A, Shido K, Fujimoto S, Kondo K . An association between maternal smoking and preeclampsia in Japanese women. Semin Thromb Hemostat 2002; 28: 507–510.
Ward K, Hata A, Jeunemaitre X, Helin C, Nelson L, Namikawa C, Farrington PF, Ogasawara M, Suzumori K, Tomoda S, Berrebi S, Sasaki M, Corvol P, Lifton RP, Lalouel JM . A molecular variant of angiotensinogen associated with preeclampsia. Nat Genet 1993; 4: 59–61.
Kobashi G, Hata A, Shido K, Kato EH, Yamada H, Fujimoto S, Kishi R, Kondo K . Association of a variant of the angiotensinogen gene with pure type of hypertension in pregnancy in the Japanese: implication of a racial difference and significance of an age factor. Am J Med Genet 1999; 86: 232–236.
Zafarmand MH, Franx A, Sabour S, van der Schouw YT, Grobbee DE, de Leeuw PW, Bots ML . The M235T variant of the angiotensinogen gene is related to development of self-reported hypertension during pregnancy: the Prospect-EPIC cohort study. Hypertens Res 2008; 31: 1299–1305.
Kobashi G, Yamada H, Kato EH, Ebina Y, Ohta K, Fujimoto S . Endothelial nitric oxide synthase gene (NOS3) variant and hypertension in pregnancy. Am J Med Genet 2011; 103: 241–244.
Kobashi G, Hata A, Shido K, Ohta K, Yamada H, Fujimoto S, Kondo K . The M235T variant of angiotensinogen gene and body mass index are useful markers for prevention of hypertension in pregnancy; a tree-based analysis of gene-environment interaction. Semin Thromb Hemostat 2002; 28: 501–505.
Luizon MR, Belo VA, Palei AC, Amaral LM, Lacchini R, Sandrim VC, Duarte G, Cavalli RC, Tanus-Santos JE . Effects of NAMPT polymorphisms and haplotypes on circulating visfatin/NAMPT levels in hypertensive disorders of pregnancy. Hypertens Res 2015; 38: 361–366.
Zhan Y, Liu M, You Y, Zhang Y, Wang J, Wang X, Liu S, Liu X . Genetic variations in the vitamin-D receptor (VDR) gene in preeclampsia patients in the Chinese Han population. Hypertens Res 2015; 38: 513–517.
Morgan L . Update on genetics of pre-eclampsia. Pregnancy Hypertens 2013; 3: 59–60.
Duckitt K, Harrington D . Risk factors for pre-eclampsia at antenatal booking: systematic review of controlled studies. BMJ 2005; 330: 565.
Cnossen JS, Leeflang MM, de Haan EE, Mol BW, van der Post JA, Khan KS, ter Riet G . Accuracy of body mass index in predicting pre-eclampsia: bivariate meta-analysis. BJOG 2007; 114: 1477–1485.
Cnossen JS, Vollebregt KC, de Vrieze N, ter Riet G, Mol BW, Franx A, Khan KS, van der Post JA . Accuracy of mean arterial pressure and blood pressure measurements in predicting pre-eclampsia: systematic review and meta-analysis. BMJ 2008; 336: 1117–1120.
Gallos ID, Sivakumar K, Kilby MD, Coomarasamy A, Thangaratinam S, Vatish M . Pre-eclampsia is associated with, and preceded by, hypertriglyceridaemia: a meta-analysis. BJOG 2013; 120: 1321–1332.
Thangaratinam S, Coomarasamy A, O’Mahony F, Sharp S, Zamora J, Khan KS, Ismail KM . Estimation of proteinuria as a predictor of complications of pre-eclampsia: a systematic review. BMC Med 2009; 7: 10.
Salako BL, Olayemi O, Odukogbe AT, Adedapo KS, Aimakhu CO, Alu FE, Ola B . Microalbuminuria in pregnancy as a predictor of preeclampsia and eclampsia. West Afr J Med 2003; 22: 295–300.
Brunelli VB, Prefumo F . Quality of first trimester risk prediction models for pre-eclampsia: a systematic review. BJOG 2015; 122: 904–914.
Drost JT, van der Schouw YT, Maas AH, Verschuren WM . Longitudinal analysis of cardiovascular risk parameters in women with a history of hypertensive pregnancy disorders: the Doetinchem Cohort Study. BJOG 2013; 120: 1333–1339.
Männistö T, Mendola P, Vääräsmäki M, Järvelin MR, Hartikainen AL, Pouta A, Suvanto E . Elevated blood pressure in pregnancy and subsequent chronic disease risk. Circulation 2013; 127: 681–690.
Opdahl S, Romundstad PR, Alsaker MD, Vatten LJ . Hypertensive diseases in pregnancy and breast cancer risk. Br J Cancer 2012; 107: 176–182.
Lykke JA, Langhoff-Roos J, Sibai BM, Funai EF, Triche EW, Paidas MJ . Hypertensive pregnancy disorders and subsequent cardiovascular morbidity and type 2 diabetes mellitus in the mother. Hypertension 2009; 53: 944–951.
Wang IK, Muo CH, Chang YC, Liang CC, Chang CT, Lin SY, Yen TH, Chuang FR, Chen PC, Huang CC, Wen CP, Sung FC, Morisky DE . Association between hypertensive disorders during pregnancy and end-stage renal disease: a population-based study. CMAJ 2013; 185: 207–213.
Behrens I, Basit S, Lykke JA, Ranthe MF, Wohlfahrt J, Bundgaard H, Melbye M, Boyd HA . Association between hypertensive disorders of pregnancy and later risk of cardiomyopathy. JAMA 2016; 315: 1026–1033.
Singh M, Pathak MS, Paul A . A study on atherogenic indices of pregnancy induced hypertension patients as compared to normal pregnant women. J Clin Diagn Res 2015; 9: BC05–BC08.
Behrens I, Basit S, Jensen A, Lykke JA, Nielsen LP, Wohlfahrt J, Kjaer SK, Melbye M, Boyd HA . Hypertensive disorders of pregnancy and subsequent risk of solid cancer-a nationwide cohort study. Int J Cancer 2016; 139: 58–64.
Nelander M, Cnattingius S, Åkerud H, Wikström J, Pedersen NL, Wikström AK . Pregnancy hypertensive disease and risk of dementia and cardiovascular disease in women aged 65 years or older: a cohort study. BMJ Open 2016; 6: e009880.
Ray JG, Vermeulen MJ, Schull MJ, Redelmeier DA . Cardiovascular health after maternal placental syndromes (CHAMPS): population-based retrospective cohort study. Lancet 2005; 366: 1797–1803.
Skjaerven R, Wilcox AJ, Klungsøyr K, Irgens LM, Vikse BE, Vatten LJ, Lie RT . Cardiovascular mortality after pre-eclampsia in one child mothers: prospective, population based cohort study. BMJ 2012; 345: e7677.
Ray JG, Schull MJ, Kingdom JC, Vermeulen MJ . Heart failure and dysrhythmias after maternal placental syndromes: HAD MPS Study. Heart 2012; 98: 1136–1141.
Wilson BJ, Watson MS, Prescott GJ, Sunderland S, Campbell DM, Hannaford P, Smith WC . Hypertensive diseases of pregnancy and risk of hypertension and stroke in later life: results from cohort study. BMJ 2003; 326: 845.
Ahmed R, Dunford J, Mehran R, Robson S, Kunadian V . Pre-eclampsia and future cardiovascular risk among women: a review. J Am Coll Cardiol 2014; 63: 1815–1822.
Bellamy L, Casas JP, Hingorani AD, Williams DJ . Pre-eclampsia and risk of cardiovascular disease and cancer in later life: systematic review and meta-analysis. BMJ 2007; 335: 974.
McDonald SD, Han Z, Walsh MW, Gerstein HC, Devereaux PJ . Kidney disease after preeclampsia: a systematic review and meta-analysis. Am J Kidney Dis 2010; 55: 1026–1039.
WHO The Global Prevalence of Anaemia in 2011. World Health Organization: Geneva. 2015.
Pineles BL, Park E, Samet JM . Systematic review and meta-analysis of miscarriage and maternal exposure to tobacco smoke during pregnancy. Am J Epidemiol 2014; 179: 807–823.
Inoue I, Nakajima T, Williams CS, Quackenbush J, Puryear R, Powers M, Cheng T, Ludwig EH, Sharma AM, Hata A, Jeunemaitre X, Lalouel JM . A nucleotide substitution in the promoter of human angiotensinogen is associated with essential hypertension and affects basal transcription in vitro. J Clin Invest 1997; 99: 1786–1797.
Morgan T, Craven C, Lalouel JM, Ward K . Angiotensinogen Thr235 variant is associated with abnormal physiologic change of the uterine spiral arteries in first-trimester decidua. Am J Obstet Gynecol 1999; 180: 95–102.
Acknowledgements
We express our gratitude to Dr Y Haruyama, Dr T Sairenchi and Dr M Nagao for their critical assistance, and to Ms Y Imai for her technical assistance in manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Umesawa, M., Kobashi, G. Epidemiology of hypertensive disorders in pregnancy: prevalence, risk factors, predictors and prognosis. Hypertens Res 40, 213–220 (2017). https://doi.org/10.1038/hr.2016.126
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.126
Keywords
This article is cited by
-
Association between pregnancy-related complications and development of type 2 diabetes and hypertension in women: an umbrella review
BMC Medicine (2024)
-
Hypertensive disorders of pregnancy increase the incidence of febrile seizures in offspring
Pediatric Research (2024)
-
Childhood growth outcomes 2 years after hypertensive versus normotensive pregnancy: a P4 study
Pediatric Research (2024)
-
Severity of Autism Spectrum Disorder Symptoms Associated with de novo Variants and Pregnancy-Induced Hypertension
Journal of Autism and Developmental Disorders (2024)
-
Association between infertility treatment and hypertensive disorders of pregnancy in the Japan Birth Cohort Consortium: a meta-analysis
Journal of Human Hypertension (2024)