Abstract
Objective:
Birth weight is an important indicator for childhood and adulthood diseases. Published studies lack information on the relative contribution of women's own birth weight to the course of her pregnancy, not only for maternal but especially to neonatal outcome. The aim of the study was to evaluate the relationship of maternal birth weight on maternal and perinatal complications during pregnancy.
Study Design:
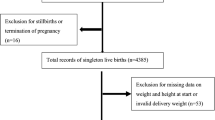
Medical and obstetrical data were collected from 5479 women at 15 hospitals in Beijing, by a systemic cluster sampling survey conducted from 20 June 2013 to 30 November 2013. These women were categorized into five groups, according to their own birth weight: low birth weight (⩽2500 g, n=275), sub-optimal birth weight (2500 to 2999 g, n=1079), optimal birth weight (3000 to 3499 g, n=2590; 3500 to 3999 g, n=1085) and high birth weight (⩾4000 g, n=450). The occurrence of maternal and neonatal complications was recorded and compared among the groups. Statistical analysis was performed by SPSS 20.0 and values of P<0.05 were considered to be statistically significant.
Results:
Low maternal birth weight was associated with higher rates of gestational diabetes mellitus (χ2=21.268, P=0.006) and hypertensive disorders (χ2=10.844, P=0.028). The latter association was strongest in women with a pre-pregnancy body mass index above 25 kg m−2. Low maternal birth weight was also associated with an apparently higher incidence of preterm labor (χ2=18.27, P=0.001) and hypertriglyceridemia (χ2=2.739, P=0.027) in pregnancy. An association between women with low birth weight and a significantly higher rate of small for gestational age infants (χ2=93.507, P<0.001) and low birth weight (χ2=36.256, P<0.001) was detected. High maternal birth weight was associated with an increased risk of pre-pregnancy overweight and obesity (P<0.001), as well as for large for gestational age infants (χ2=93.507, P<0.001) and macrosomia (χ2=72.594, P<0.001).
Conclusions:
In our study, high or low maternal birth weight was strongly associated with maternal and perinatal adverse pregnancy outcomes. This suggests that by controlling the birth weight of female infants among the normal range, adverse outcomes may be decreased in the future and for the following generations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
á Rogvi R, Forman JL, Damm P, Greisen G . Women born preterm or with inappropriate weight for gestational age are at risk of subsequent gestational diabetes and pre-eclampsia. PLoS One 2012; 7 (3): e34001.
de Boo HA, Harding JE . The developmental origins of adult disease (Barker) hypothesis. Aust N Z J Obstet Gynaecol 2006; 46 (1): 4–14.
Tanabe K, Tamakoshi K, Murotsuki J . Association of women's birth weight with their blood pressure during pregnancy and with the body size of their babies. Tohoku J Exp Med 2011; 224 (4): 287–292.
Yan J, Li X, Su R, Zhang K, Yang H . Long-term effects of maternal diabetes on blood pressure and renal function in rat male offspring. PLoS One 2014; 9 (2): e88269.
Barker DJ, Winter PD, Osmond C, Margetts B, Simmonds SJ . Weight in infancy and death from ischaemic heart disease. Lancet 1989; 2: 577–580.
Innes KE, Byers TE, Marshall JA, Barón A, Orleans M, Hamman RF . Association of a woman’s own birth weight with subsequent risk for gestational diabetes. JAMA 2002; 287 (19): 2534–2541.
Wei JN, Sung FC, Li CY, Chang CH, Lin RS, Lin CC et al. Low birth weight and high birth weight infants are both at an increased risk to have type 2 diabetes among schoolchildren in Taiwan. Diabetes Care 2003; 26 (2): 343–348.
Chen Y, Li G, Ruan Y, Zou L, Wang X, Zhang W . An epidemiological survey on low birth weight infants in China and analysis of outcomes of full-term low birth weight infants. BMC Pregnancy Childbirth 2013; 13: 242.
de Jong M, Cranendonk A, van Weissenbruch MM . Components of the metabolic syndrome in early childhood in very-low-birth-weight infants and term small and appropriate for gestational age infants. Pediatr Res 2015; 78: 457–461.
Mbachu II, Udigwe GO, Okafor CI, Umeonunihu OS, Ezeama C, Eleje GU . The pattern and obstetric outcome of hypertensive disorders of pregnancy in Nnewi, Nigeria. Niger J Med 2013; 22 (2): 117–122.
Palatianou ME, Simos YV, Andronikou SK, Kiortsis DN . Long-term metabolic effects of high birth weight: a critical review of the literature. Horm Metab Res 2014; 46 (13): 911–920.
Egeland GM, Skjaerven R, Irgens LM . Birth characteristics of women who develop gestational diabetes: population based study. BMJ 2000; 321 (7260): 546–547.
Yang HX . Diagnostic criteria for gestational diabetes mellitus (WS 331-2011). Chin Med J (Engl) 2012; 125 (7): 1212–1213.
Seghieri G, Anichini R, De Bellis A, Alviggi L, Franconi F, Breschi MC . Relationship between gestational diabetes mellitus and low maternal birth weight. Diabetes Care 2002; 25 (10): 1761–1765.
Lithell HO, McKeigue PM, Berglund L, Mohsen R, Lithell U, Leon DA . Relationship of birthweight and ponderal index to non-insulin-dependent diabetes and insulin response to glucose challenge in men aged 50–60 years. BMJ 1996; 312: 406–410.
Birgisdottir BE, Gunnarsdottir I, Thorsdottir I, Gudnason V, Benediktsson R . Size at birth and glucose intolerance in a relatively genetically homogeneous, high-birth weight population. Am J Clin Nutr 2002; 76 (2): 399–403.
McCance DR, Pettitt DJ, Hanson RL, Jacobsson LT, Knowler WC, Bennett PH . Birth weight and non-insulin dependent diabetes: thrifty genotype, thrifty phenotype, or surviving small baby genotype? BMJ 1994; 308: 942–945.
Dabelea D, Pettitt DJ, Hanson RL, Imperatore G, Bennett PH, Knowler WC . Birth weight, type 2 diabetes, and insulin resistance in Pima Indian children and young adults. Diabetes Care 1999; 22 (6): 944–950.
Phillips DI, Walker BR, Reynolds RM, Flanagan DE, Wood PJ, Osmond C et al. Low birth weight predicts elevated plasma cortisol concentrations in adults from 3 populations. Hypertension 2000; 35: 1301–1306.
Roberts A, Green A, Loughna P, Broughton Pipkin F . PP075. Poor renal function following hypertensive pregnancy: older mothers and smaller babies. Pregnancy Hypertens 2013; 3 (2): 94–95.
Adair LS, Martorell R, Stein AD, Hallal PC, Sachdev HS, Prabhakaran D et al. Size at birth, weight gain in infancy and childhood, and adult blood pressure in 5 low- and middle-income-country cohorts: when does weight gain matter? Am J Clin Nutr 2009; 89 (5): 1383–1392.
Schlembach D, Lang U . Preeclampsia and pregnancy-induced hypertension - diseases determined in the uterus? Gynakol Geburtshilfliche Rundsch 2008; 48 (4): 225–230.
Hemachandra A, Klebanoff M, Duggan A, Hardy JB, Furth SL . The association between intrauterine growth restriction in the fullterm infant and high blood pressure at age 7 years: result from the Collaborative Perinatal Project. Int J Epidemiol 2006; 35: 871–877.
Mutsaerts MA, Groen H, Buiter-Van der Meer A, Sijtsma A, Sauer PJ, Land JA et al. Effects of paternal and maternal lifestyle factors on pregnancy complications and perinatal outcome. A population-based birth-cohort study: the GECKO Drenthe cohort. Hum Reprod 2014; 29 (4): 824–834.
Economides DL, Crook D, Nicolaides KH . Hypertriglyceridemia and hypoxemia in small-for-gestational-age fetuses. Am J Obstet Gynecol 1990; 162 (2): 382–386.
Yeung EH, McLain AC, Anderson N, Lawrence D, Boghossian NS, Druschel C et al. Newborn adipokines and birth outcomes. Paediatr Perinat Epidemiol 2015; 29 (4): 317–325.
Teague AM, Fields DA, Aston CE, Short KR, Lyons TJ, Chernausek SD . Cord blood adipokines, neonatal anthropometrics and postnatal growth in offspring of Hispanic and Native American women with diabetes mellitus. Reprod Biol Endocrinol 2015; 13: 68.
Nohr EA, Vaeth M, Rasmussen S, Ramlau-Hansen CH, Olsen J . Waiting time to pregnancy according to maternal birthweight and prepregnancy BMI. Hum Reprod 2009; 24 (1): 226–232.
Ogonowski J, Miazgowski T, Engel K, Celewicz Z . Birth weight predicts the risk of gestational diabetes mellitus and pregravid obesity. Nutrition 2014; 30 (1): 39–43.
Gonçalves FC, Amorim RJ, Eickmann SH, Lira PI, Lima MC . The influence of low birth weight body proportionality and postnatal weight gain on anthropometric measures of 8-year-old children: a cohort study in Northeast Brazil. Eur J Clin Nutr 2014; 68 (8): 876–881.
Godfrey KM, Barker DJP, Robinson S, Osmond C . Mother’s birthweight and diet in pregnancy in relation to the baby’s thinness at birth. Br J Obstet Gynaecol 1997; 104: 663–667.
Selling KE, Carstensen J, Finnström O, Sydsjö G . Intergenerational effects of preterm birth and reduced intrauterine growth: a population-based study of Swedish mother-offspring pairs. BJOG 2006; 113 (4): 430–440.
Ahlsson F, Gustafsson J, Tuvemo T, Lundgren M . Females born large for gestational age have a doubled risk of giving birth to large for gestational age infants. Acta Paediatrica 2007; 96 (3): 358–362.
Morton SM, De Stavola BL, Leon DA . Intergenerational determinants of offspring size at birth: a life course and graphical analysis using the Aberdeen Children of the 1950 s Study (ACONF). Int J Epidemiol 2014; 43 (3): 749–759.
Costa e Silva LI, Gomes FM, Valente MH, Escobar AM, Brentani AV, Grisi SJ . The intergenerational effects on birth weight and its relations to maternal conditions, São Paulo, Brazil. Biomed Res Int 2015; 2015: 615034.
Acknowledgements
I acknowledge the support of the entire management of the 15 hospitals surveyed in Beijing in the data retrieval efforts for the study (Tongzhou Maternal and Child Health Hospital of Beijing; Peking University Third Hospital; General Hospital of Beijing Military Region Center Hospital of aviation industry; Pinggu Maternal and Child Health Hospital of Beijing; Beijing Hospital of Miyun City; Navy General Hospital, Beijing; Daxing District Hongxing Hospital; Beijing Chui Yang Liu Hospital; Peking University Shougang Hospital; Combined with traditional Chinese and Western Medicine Hospital of Beijing City; Beijing No.6 Hospital; Beijing Changping Hospital of Traditional Chinese Medicine, General Hospital of Jingmei Group). This study was supported by grants from the World Diabetes Foundation (charity No: WDF 10-517, WDF14-908).
Author contributions
HY and WZ designed the study. RS did the literature search with support from YW. RS and WZ analysed the data. CW, HF and LL collected the data. RS, MH and EH wrote the report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Su, R., Zhu, W., Wei, Y. et al. Relationship of maternal birth weight on maternal and neonatal outcomes: a multicenter study in Beijing. J Perinatol 36, 1061–1066 (2016). https://doi.org/10.1038/jp.2016.143
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.143
This article is cited by
-
BMI and risk of gestational diabetes among women of South Asian and Chinese ethnicity: a population-based study
Diabetologia (2021)
-
Body surface area at birth and later risk for gestational diabetes mellitus among primiparous women
Acta Diabetologica (2019)
-
Similarities between acylcarnitine profiles in large for gestational age newborns and obesity
Scientific Reports (2017)