Abstract
The regional neuronal changes taking place in the early and late stages of antipsychotic treatment are still not well characterized in humans. In addition, it is not known whether these regional changes are predictive of or are correlated with treatment response. Using PET with 15O, we evaluated the time course of regional cerebral blood flow (rCBF) patterns generated by a first (haloperidol) and a second (olanzapine) generation antipsychotic drug in patients with schizophrenia during a 6-week treatment trial. Patients were initially scanned after withdrawal of all psychotropic medication (2 weeks), and then blindly randomized to treatment with haloperidol (n=12) or olanzapine (n=17) for a period of 6 weeks. Patients were scanned again after 1 and 6 weeks of treatment. All assessments, including scanning sessions, were obtained in a double-blind manner. As hypothesized, we observed rCBF changes that were common to both the drugs, implicating cortico-subcortical and limbic neuronal networks in antipsychotic action. In addition, in these regions, some patterns seen at weeks 1 and 6 were distinctive, indexing neuronal changes related to an early (ventral striatum, hippocampus) and consolidated (anterior cingulate/medial frontal cortex) stage of drug response. Finally, both after 1 and 6 weeks of treatment, we observed differential patterns of rCBF activation between good and poor responders. After 1 week of treatment, greater rCBF increase in the ventral striatum and greater decrease in the hippocampus were associated with good response.
Similar content being viewed by others
INTRODUCTION
Antipsychotic drugs (APDs) act primarily to relieve positive symptoms of schizophrenia (hallucinations, delusions) with little or no effect on primary negative and cognitive symptoms. It has been recently confirmed that, with the exception of clozapine, first- and second-generation APDs alleviate positive symptoms to the same extent (Lieberman et al, 2005; McEvoy et al, 2006). However, treatment response to APD in schizophrenia is not homogeneous. Only 5–10% of patients experience a full recovery in response to treatment and about 30% of patients are ‘treatment resistant’ despite adequate treatment (Harrow et al, 1997). Consequently, clinicians are faced with difficult decisions when managing their patients' treatment, including how long an adequate trial of APD should last, when is the correct dosing achieved, is the patient compliant with treatment, and will the patient experience a relapse if a switch to another APD is initiated. Thus, several weeks may typically elapse before a decision to switch to another APD is made, leaving the patient poorly treated and vulnerable to hospitalization. We lack biomarkers of treatment response to guide dosing and duration of treatment questions.
There has been considerable debate regarding the time course of response to antipsychotic treatment. According to many descriptions (Gelder et al, 2000; Grace and Bunney, 1995; Marder and Van-Kammen, 2000), there is a delay of 2 to 3 weeks before APD response, a view that has been strongly challenged by recent meta-analyses of clinical trials. An analysis of 42 published clinical trials found the greatest improvement in positive symptoms in the first and second weeks of treatment, with a cumulative improvement over time thereafter (Agid et al, 2003). Another analysis of 21 trials found a linear response pattern up to 28 days of treatment (van den Oord et al, 2008). The regional neuronal changes taking place across the time course of antipsychotic treatment are still not well characterized. Further, it is not known whether these regional changes are predictive of treatment response. Understanding the mechanisms underlying drug response could enhance the development of more effective and selectively targeted antipsychotic agents.
Using PET with 15O, we evaluated the time course of regional cerebral blood flow (rCBF) patterns generated acutely and subacutely in a 6-week trial using a first (haloperidol) and a second (olanzapine) generation APD in patients with schizophrenia. We hypothesized that regions in which the two drugs show similar rCBF changes would more robustly identify regions involved in antipsychotic action, as identified by regions in which rCBF and symptom reduction are correlated. On the basis of our previous work (Lahti et al, 2004; Lahti et al, 2003; Lahti et al, 2006; Lahti et al, 2005), we hypothesized that these regions would include regions in the limbic circuit, such as the ventral striatum, the anterior cingulate cortex (ACC), and the hippocampus. In addition, on the basis of their known differences in preclinical profiles (Chiodo and Bunney, 1983; White and Wang, 1983), we hypothesized that the patterns of rCBF activation between the two drugs would be most different in the striatum, in which haloperidol would increase rCBF potently throughout the dorsal and ventral striatum, whereas rCBF increase with olanzapine would be restricted to the ventral striatum. We further hypothesized that some of the patterns seen after acute (1 week) and subacute (6 weeks) treatment would be distinctive, indexing neuronal changes related to an early vs consolidated stage of drug response. Finally, we hypothesized that the treatment response would correlate with consistent patterns of rCBF changes on acute and subacute treatment.
MATERIALS AND METHODS
Volunteers
Medically healthy individuals with schizophrenia were recruited from the Residential Research Unit of the Maryland Psychiatric Research Center (MPRC) in Baltimore, MD, USA to participate in this study. In total, 37 individuals agreed to participate and gave signed consent. Each of them underwent a Structured Clinical Interview for DSM-III-R (SCID) (Spitzer et al, 1987) at hospital admission. Two research psychiatrists reached a consensus diagnosis of schizophrenia on the basis of the clinical interview and all other sources of data using DSM IV criteria.
Informed Consent
Schizophrenia volunteers were fully informed about the nature of the protocol and after being informed, each gave informed consent. Only patients who were competent and clinically judged to be capable of understanding and appreciating the risks involved in this study were selected for participation. Separate people, including both the principal investigator and the non-investigator clinicians, presented the nature of the protocol to the volunteers on several occasions and assessed their willingness to be involved. Family members or caregivers were involved in the information process when available. A patient's right advocate met every potential patient on admission, and an ombudsman monitored the individuals' understanding of the study and willingness to participate through the study. Before signing consent, each patient completed an Evaluation to Sign Consent Form, a form probing the patient's understanding of some important aspects of the protocol. Participants remained in-patients for the whole length of the study. Patients were closely monitored for increased symptoms and side effects. When clinically necessary, the protocol was interrupted and the individual was restarted on antipsychotic medication. All study personnel completed formal training in the protection of human subjects as required by the University of Maryland School of Medicine and the NIH. The University of Maryland IRB approved this project.
Study Design
Medication withdrawal and collection of the off-medication rCBF scans
All schizophrenia volunteers were withdrawn from the psychotropic medications for a period of 2 weeks before scanning. All other aspects of in-patient milieu treatment were continued during this project. Clinical monitoring was done continuously and intervention (including study termination) was deemed possible on the basis of clinical judgment of adverse behavioral changes requiring treatment. The 2-week medication-free period was designed to allow for the disappearance of APDs from central D2 receptors (Tamminga et al, 1993). Symptoms of schizophrenia were assessed at baseline and at the time of each scanning session using the 18-item version of the Brief Psychiatric Rating Scale (BPRS) (1–7 scale) (Overall and Gorham, 1962). We evaluated the BPRS Total, as well as its Psychosis subscale (items: conceptual disorganization, hallucinatory behavior, and unusual thought content) scores (Hedlund and Vieweg, 1980). Of the 37 patients who signed the consent, 5 dropped out during the withdrawal protocol. Two dropped out because of symptom exacerbation and three because they did not want to continue with the study. These patients were remedicated and quickly returned to their pre-study status. At the end of the medication withdrawal, 32 patients completed a baseline medication-free scanning session (Baseline or off-drug scanning session). We have previously reported on the patterns of correlation between rCBF and symptoms in two independent cohorts of drug-free patients with schizophrenia, one of which included the present group of patients (Lahti et al, 2006).
Randomization
Patients who completed the off-drug scan were blindly randomized to one of the following four groups: (1) haloperidol fixed dose (10 mg) for 6 days followed by haloperidol optimal dose (range 10–20 mg) for 5 weeks (HAL–HAL), (2) olanzapine fixed dose (12.5 mg) for 6 days followed by olanzapine optimal dose (range 12.5–25 mg) for 5 weeks (OLZ–OLZ), (3) placebo for 6 days followed by haloperidol (optimal dose) for 5 weeks (PBO–HAL), and (4) placebo for 6 days followed by olanzapine (optimal dose) for 5 weeks (PBO–OLZ). Among the patients randomized to haloperidol (n=14), 10 were randomized to HAL–HAL and 4 to PBO–HAL. Among the patients randomized to olanzapine (n=18), 14 were randomized to OLZ–OLZ and 4 to PBO–OLZ.
The purpose of the 1-week PBO lead-in period was to allow for a placebo-controlled evaluation of the ability to predict treatment response using the week 1 rCBF patterns.
Medications were prepared in similar-looking capsules by the hospital pharmacist. Medication adjustments were made blindly by the treated psychiatrists in increments of 5 mg for haloperidol and 6 mg for olanzapine. Patients did not receive anticholinergic medication unless their clinical condition required it. A rating of motor symptoms with the MPRC Involuntary Movement Scale preceded the use of anticholinergic medication.
rCBF imaging protocol
Patients were scanned at baseline while off-drug, after 6 days (thereafter referred as week 1 scanning session), and after 6 weeks (week 6 scanning session) of treatment. Patients were scanned during rest condition (two scans), for which they were instructed to lie quietly with eyes open. Concurrently with each scanning session, mental status was assessed using the BPRS. All assessments, including those done during the imaging sessions, were obtained in a double-blind manner.
Dropout
In the HAL–HAL group, two patients dropped out before completing the week 1 scanning session. One dropped out because of psychosis exacerbation and the other one was a voluntary withdrawal.
In the OLZ–OLZ group, one patient dropped out after completing the week 1 scanning session as a voluntary withdrawal. Thus, the analyses presented in this paper reflect imaging data on 29 patients: 12 in the haloperidol group (HAL–HAL n=8, PBO–HAL n=4) and 17 in the olanzapine group (OLZ–OLZ n=13 and PBO–OLZ n=4).
The total schizophrenia volunteer group included 22 men and 7 women. Before the medication withdrawal, three patients in the haloperidol group were treated with either a first-generation or a combination of a first- and a second-generation APD, and eight with a second-generation APD. In the olanzapine group, 2 patients were treated with a combination of a first- and a second-generation APD, and 10 with a second-generation APD. One patient in the haloperidol group and three in the olanzapine group were treated with clozapine before drug withdrawal. However, all four were treated with a daily dosage of ⩽300 mg. None of the patients was treated with a long-acting APD depot preparation.
PET/15O imaging
Patients were scanned on the GE Advanced 3D PET system (General Electrical Healthcare, United Kingdom) located at the PET Center of the Johns Hopkins Hospital. The PET acquires 30 parallel slices with a center-to-center separation of 5 mm, an average transaxial resolution of 5.0 mm full-width at half-maximum (FWHM), and an average resolution of 6.0 mm FWHM, measured in the center of the field of view. For each patient, a single 10-min transmission scan was acquired for attenuation correction using a 10mCi68Ge rotating pin source. The bolus H215O method (Raichle et al, 1983) was used without arterial blood sampling. Approximately 12 mCi H215O was administered with each scan. A total of 7 min elapsed between scans except where specified. Scan acquisition began 15 s after dose delivery. PET data were acquired for 90 s. A thermoplastic mask, custom-made for each patient, was used to minimize head movement and to align head position for subsequent scanning sessions.
Image analysis
The PET blood flow images were analyzed using the statistical parametric mapping (SPM 2) software (Wellcome, Department of Cognitive Neurology, London) (Friston et al, 1996). The scans from each patient were realigned using the first scan as a reference. After realignment all images were transformed into the stereotaxic space of the Montreal Neurological Institute. Before generating the SPM(z) map, the data were smoothed using a 12-mm Gaussian kernel. Blood flow values were scaled using the ratio adjustment method.
Data Analysis
Demographic measures of age, gender, race, and length of illness were compared between the haloperidol and olanzapine drug groups by t-test and χ2 analyses. The BPRS data were analyzed using paired t-test.
The following image analyses were performed:
-
Time-course analysis: To evaluate the time course of rCBF changes induced by each drug, we contrasted the week 1 scans of patients on active medication (haloperidol: n=8; olanzapine: n=13) with their baseline (off-drug) scans (week 1 drug effects), and the week 6 scans of all patients with their baseline scans (week 6 drug effects) using SPM2. As treatment response has been shown to plateau after 4 weeks (van den Oord et al, 2008), all patients, whether or not they had received placebo for 6 days, should have reached optimal response by week 6. For hypothesized regions that showed significant rCBF changes, we calculated the coefficient of correlation between rCBF changes from baseline to week 6 (sampled in the maxima of the identified cluster using a 3 × 3 × 3 pixel ROI) and the BPRS Total and Psychosis change scores for the same period.
-
Conjunction analysis: Similarities in rCBF patterns between the two drugs were assessed between week 6 and baseline using a conjunction analysis (Price and Friston, 1997).
-
Contrast analysis: We contrasted the rCBF changes between week 6 and baseline of each drug (that is, haloperidol (week 6 minus baseline) vs olanzapine (week 6 minus baseline)).
-
Good vs poor treatment responders: SPM analysis. To identify patterns of rCBF change related to treatment response using a whole brain approach, we contrasted the rCBF changes between the good (GR) and poor (PR) responders to the treatment (that is, haloperidol GR vs haloperidol PR, and olanzapine GR vs olanzapine PR) for the following epochs: (1) from baseline to week 6 and (2) from baseline to week 1. Good treatment response was defined as a >10% improvement on the BPRS Psychosis score at the final 6-week assessment. Although a 15–30% reduction in BPRS is traditionally used as an index of good response (Leucht et al, 2005), we used a less stringent threshold because the clinical status of the patients who were taken off their medications for only 2 weeks was likely different from a relapsed state. The subsequent region-of-interest analyses were performed using ANOVA.
For the SPM 2 analyses, the primary criterion for statistical significance of the hypothesized regions was set at p=0.001, uncorrected. For all other brain regions, only clusters of connected voxels above a threshold were tested for significance by means of a spatial extent statistic, which was set at p=0.05, after correcting for multiple comparisons (Friston et al, 1996).
RESULTS
Clinical Effects
There were no differences between patients in the haloperidol and those in the olanzapine groups in terms of age (38.3±12.2 vs 36.1±10.5 years), length of illness (15.3±14.1 vs 11.3±9.6 years), gender (male/female) (10/2 vs 12/5), and race ratios (Caucasian/African American) (5/7 vs 3/14). Overall, patients in the haloperidol group experienced a significant improvement, as measured on the BPRS Psychosis subscale (t=2.26, p<0.05), at the final 6-week evaluation (Table 1). Improvement in the olanzapine group was significant at a trend level as measured on the BPRS Total (t=−2.01, p<0.1) and the BPRS Psychosis subscales (t=−1.56, p<0.2). Improvement over the first week of treatment did not reach significance for either group. Haloperidol patients were treated with a mean dose of 10.4±3.3 mg/day (range: 5–15 mg/day) and the olanzapine patients with a mean dose of 15.9±4.8 mg/day (range: 12.5–25 mg/day). Only two patients (one treated with haloperidol and one treated with olanzapine) experienced extrapyramidal symptoms and were treated with 2 mg benztropine.
Time-Course Analysis
Acute APD effects
Haloperidol: Week 1 vs off-drug and off-drug vs week 1 group average images were contrasted (Table 2 and Figure 1).
rCBF changes with haloperidol after 1 week of treatment. rCBF increases are shown in the top panels and rCBF decreases in the bottom panels. There were significant activations in the ventral striatum (1), the dorsal striatum (2), and the left sensorimotor cortex (3). There were significant deactivations in the ACC (4), the right middle temporal cortex (5), and the cerebellum (6). The display threshold for voxels was set at t=3.11, p<0.001.
Where haloperidol increased rCBF acutely (Figure 1, top panels), there was a significant cluster of rCBF activation encompassing the ventral striatum and the putamen bilaterally. The left cluster extended to the anterior part of the thalamus. There was a significant cluster in the superior portion of the left sensorimotor cortex.
Where haloperidol decreased rCBF acutely (Figure 1, bottom panels), there was a significant cluster of rCBF reduction in the right middle temporal cortex. There were significant maxima of rCBF reduction in the right medial temporal cortex, the ACC, the midbrain, and the cerebellum, bilaterally.
Olanzapine: Week 1 vs off-drug and off-drug vs week 1 group average images were contrasted (Table 2 and Figure 2).
rCBF changes with olanzapine after 1 week of treatment. rCBF increases are shown in the top panels and rCBF decreases in the bottom panels. There were significant activations in the caudate/ventral striatum (1), and the inferior frontal (2) and inferior parietal (3) cortex, both on the right, and significant deactivation in the ACC (4) and the left posterior thalamus (5). The display threshold for voxels was set at t=3.11, p<0.001.
Where olanzapine increased rCBF acutely (Figure 2, top panels), there were significant clusters of rCBF activation in the inferior frontal and inferior parietal cortices, both on the right. There was one significant maxima of activation in the left caudate/ventral striatum.
Where olanzapine decreased rCBF acutely (Figure 2, bottom panels), there was a significant cluster of rCBF deactivation in the left posterior thalamus. In addition, there were significant maxima in the right thalamus, the left medial temporal cortex, and the ACC.
Subacute APD effects
Haloperidol: Week 6 vs off-drug and off-drug vs week 6 (Table 3 and Figure 3) group average images were contrasted. Owing to the large size of the clusters and to better discriminate the regions showing rCBF changes, the data in the tables are reported at a threshold of t>3.75, 45 voxels.
rCBF changes with haloperidol after 6 weeks of treatment. rCBF increases are shown in the top panels and rCBF decreases in the bottom panels. There were significant activations in the ventral striatum (1), the dorsal striatum (2), the thalamus (3), the left post-central cortex (4), and the left inferior parietal cortex (5). There were significant deactivations in the ACC/medial frontal cortex (6), in a large cluster encompassing the temporal pole, part of the inferior frontal cortex and the insula (7), bilaterally, the inferior and middle temporal cortex (8), the superior frontal cortex (9), the inferior parietal cortex (10), and the cerebellum (11). The display threshold for voxels was set at t=3.11, p<0.001.
Where haloperidol increased rCBF subacutely (Figure 3, top panels), there was a significant cluster of rCBF activation encompassing the ventral and dorsal striatum bilaterally. In addition, significant clusters of activation were also identified in the left thalamus, and the left post-central cortex and the inferior parietal cortex bilaterally. Inspection of the data at a lower threshold (t=3.11, p=0.001) indicated that the activation of the thalamus was bilateral.
Where haloperidol decreased rCBF subacutely (Figure 3, bottom panels), there was a large reduction in rCBF in the ACC/medial frontal cortex (MFC) embracing 1275 suprathreshold (t=3.11) voxels. In addition, there was a large rCBF reduction encompassing the temporal pole, part of the inferior frontal cortex, and the insula bilaterally. There were significant clusters of deactivation in the inferior and middle temporal cortex, both on the right, the superior frontal cortex on the right, the inferior parietal cortex on the right, and in the cerebellum bilaterally.
Olanzapine: Week 6 vs off-drug and off-drug vs week 6 group average images were contrasted (Table 4, Figure 4).
rCBF decreases with olanzapine after 6 weeks of treatment. rCBF increases are shown in the top panels and rCBF decreases in the bottom panels. There were significant activations in the right ventral striatum (1), a large cluster encompassing most of the right inferior parietal cortex (2), the superior parietal cortex (3), bilaterally, the right middle temporal cortex (4), and the left middle/inferior frontal cortex (5). There were significant deactivations in the ACC/medial frontal cortex (6), the thalamus (7), and the cerebellum (8). The display threshold for voxels was set at t=3.11, p<0.001.
Where olanzapine increased rCBF subacutely (Figure 4, top panels), there were significant clusters of rCBF activation in several cortical regions, including a large cluster encompassing most of the inferior parietal cortex, the superior parietal cortex, the middle temporal cortex, all three on the right, the left superior parietal cortex, and the left middle/inferior frontal cortex. In addition, there was a significant maxima identified in the ventral striatum on the right.
Where olanzapine decreased rCBF subacutely (Figure 4, bottom panels), there was a large reduction in rCBF in the ACC/MFC embracing 632 suprathreshold (t=3.11) voxels. In addition, there were significant clusters of deactivation in the thalamus and the cerebellum, both on the right. There were significant maxima identified in the thalamus and the midbrain, both on the left.
Correlations between rCBF changes over 6 weeks and clinical improvement
On haloperidol administration, the rCBF decrease in ACC and the rCBF increase in the thalamus were correlated, albeit at a trend level in the thalamus, with clinical improvement, as measured with the BPRS Total or Psychosis change scores (Table 5). On olanzapine administration, the correlation between rCBF decrease in ACC and clinical improvement was medium and did not reach significance.
Conjunction Analysis
Overlap of activation between haloperidol and olanzapine
There was overlap of activation between haloperidol and olanzapine in the left pre- and post-central cortex and in the right ventral striatum/caudate (Table 6).
Overlap of deactivation between haloperidol and olanzapine
There was overlap of deactivation between haloperidol and olanzapine in the ACC/MFC (Table 6).
Contrast Analysis
Regions more activated with haloperidol vs olanzapine
Regions that were more activated with haloperidol vs olanzapine included the putamen and the thalamus, bilaterally, and the left post-central cortex (Table 6).
Regions more activated with olanzapine vs haloperidol
Several cortical regions were significantly more activated with olanzapine vs haloperidol: the right orbitofrontal cortex, the right superior and middle frontal cortex, the inferior frontal cortex, bilaterally, the right superior and inferior parietal cortex, and the right superior temporal cortex (Table 6).
Good (GR) vs Poor (PR) Treatment Responders
GR vs PR: contrast between pattern of changes from baseline to week 6
Haloperidol: After 6 weeks of treatment, GR had significantly more activation in the right ventral striatum and left thalamus, and less activation in the left hippocampus/parahippocampus compared with the PR (Table 7). On using a less stringent threshold (t=2.41, p=0.01), GR also had significantly less activation in the ACC compared with PR.
Olanzapine: Compared with PR, GR had significantly more activation in the ventral striatum, bilaterally, and in the cerebellum, and less activation in several cortical areas, including the sensorimotor, middle and medial frontal, superior parietal cortices, as well as the ACC (Table 8).
GR vs PR: contrast between pattern of changes from baseline to week 1
Haloperidol: After 1 week of treatment, GR had significantly more activation in the right caudate/ventral striatum, and less activation in the left hippocampus compared with PR (Table 7).
Olanzapine: In contrast to PR, GR had significantly more activation in the right caudate/ventral striatum and the ACC, and less activation in the left hippocampus and the left inferior frontal cortex (Table 8).
GR vs PR at week 1: region-of-interest analysis in the ventral striatum and hippocampus
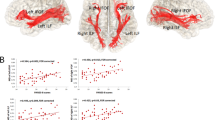
rCBF values sampled in the right ventral striatum and left hippocampus at baseline (off medications) and at week 1 were contrasted between the haloperidol GR and PR, the olanzapine GR and PR, and the placebo patients based on their response (GR or PR) to either drug at the end of the study. In the presence of a significant main effect in the overall ANOVA (F(5, 26)=6.00; p<0.002), pairwise comparisons of mean rCBF within each drug group revealed that compared with PR, GR had a significantly greater increase in rCBF in the ventral striatum (Olanz, p<0.10, Hal, p<0.01) and a significant decrease in rCBF in the hippocampus (Olanz, p<0.005, Hal p<0.001) (GR, n=4 Olanz, n=3 Hal; PR, n=7 Olanz, n=5 Hal) after 1 week of treatment (see Figure 5). In the placebo group, there were no differences between the patients who experienced a good response to treatment (n=4) once they were treated with haloperidol or olanzapine, vs those who did not (n=4). The functional changes in ventral striatum and hippocampus at week 1 were inversely correlated (r=−0.62, p<0.01). In total, 6 out of 7 good responders and only 1 out of 12 poor responders had both an increase in ventral striatum and a decrease in hippocampal rCBF at week 1. These proportions were significantly different (Yates' χ2=8.29, df=1; p=0.004).
rCBF values sampled in the right ventral striatum and the left hippocampus at baseline (off meds) and at week 1 were contrasted between the haloperidol GR and PR, the olanzapine GR and PR, and the placebo patients based on their response (GR or PR) to either drug at the end of the study. Compared with PR, GR had a significantly greater increase in rCBF in the ventral striatum (Olanz, p<0.10, Hal, p<0.01) and a significant decrease in rCBF in the hippocampus (Olanz, p<0.005, Hal p<0.001) (GR, n=4 Olanz, n=3 Hal; PR, n=7 Olanz, n=5 Hal) after 1 week of treatment. In the placebo group, there were no differences between the patients who experienced a good response to treatment (n=4) after treatment with haloperidol or olanzapine vs those who did not (n=4).
DISCUSSION
Using PET with 15O, we evaluated the time course of rCBF patterns generated by a first (haloperidol) and a second (olanzapine) generation APD in patients with schizophrenia during a 6-week treatment trial. As hypothesized, we observed rCBF changes that were common to both drugs, implicating cortico-subcortical and limbic neuronal networks in antipsychotic action. In addition, in these regions, some patterns seen at weeks 1 and 6 were distinctive, indexing neuronal changes related to an early (ventral striatum, hippocampus) and consolidated (ACC/MFC) stage of drug response. Finally, in these regions, we observed differential patterns of rCBF activation between good and poor responders both at weeks 1 and 6. At week 1, greater rCBF increase in the ventral striatum and greater decrease in the hippocampus was associated with good response.
Regions Implicated in Antipsychotic Action
Subcortical regions
On administering both drugs, rCBF activation was observed in the striatum after 1 and 6 weeks of treatment. However, whereas haloperidol activated both the ventral and dorsal striatum, olanzapine activated only the ventral part of the striatum and the ventral part of the caudate nucleus. In addition, both at weeks 1 and 6, good responders in contrast to poor responders in either treatment group showed greater rCBF increase in the ventral striatum.
The functional differences seen between the drugs in the activation of the dorsal striatum may account for the well-known clinical difference between the two drugs in the emergence of motor side effects (Sikich et al, 2004). In preclinical studies, olanzapine, in contrast to haloperidol, shows selective electrophysiological action on dopamine neurons, inducing depolarization blockade in the mesolimbic (A10), but not in the nigrostriatal (A9) cells (Chiodo and Bunney, 1983; White and Wang, 1983). Consistent with this limbic selectivity, olanzapine stimulates immediate early gene (IEG) expression in mesolimbic (ventral striatum, ACC, and medial PFC), but not in the nigrostriatal (dorsal striatum) projection fields (Robertson and Fibiger, 1992; Robertson and Fibiger, 1996). Thus, our finding of selective functional activation of the ventral striatum with olanzapine is consistent with these preclinical data. We have observed the same pattern of ventral, not dorsal, rCBF activation with clozapine, another APD with so-called limbic selectivity (Lahti et al, 2003). A [18F] fallypride PET study comparing the occupancy of striatal D2/D3 dopamine receptors in patients treated with olanzapine or haloperidol failed to find significant differences between the drugs in the degree of receptor occupancy in the dorsal, ventral striatum, and medial thalamus (Kessler et al, 2005). Taken together, these data suggest that the striatal neuronal response measured by this functional study cannot just be understood in terms of DA D2 receptor binding.
Both drugs had opposite functional effects in the thalamus: increased activation with haloperidol and decreased activation with olanzapine. We have observed similar functional patterns after the administration of a single dose of each of these drugs in patients with schizophrenia (Lahti et al, 2005). The activation seen with haloperidol in the putamen, thalamus, and motor cortex is consistent with the activation of a circuit that has been postulated to be related to motor function (Alexander and Crutcher, 1990). On acute olanzapine administration, decrease in thalamic rCBF correlated with sedation, an effect we hypothesized to be associated with its histaminergic properties.
Limbic cortex
On administering each drug, after 6 weeks of treatment, we observed the same pattern of large rCBF decrease in the ACC/MFC, a decrease that was correlated with clinical improvement. This stands in contrast to the limited changes observed in the same region after 1 week of treatment. A decrease in a similar region of the ACC/medial frontal has been reported after risperidone treatment (Ngan et al, 2002) and been found to correlate with clinical improvement. Also consistent with these data are the reports of increased ACC metabolism after a 3- to 4-week antipsychotic medication withdrawal (Holcomb et al, 1996; Miller et al, 1997). In this study, we found that the ACC/medial frontal neuronal response, although already established during the first week of treatment, grows to encompass a large area of the MFC after that. It is thus reasonable to suggest that this ACC/MFC response seems to index a delayed neuronal response to APDs. This region of the ACC/MFC encompasses the anterior region of the rostral ACC (Amodio and Frith, 2006). The anterior rostral ACC, located between the orbital MFC and the posterior rostral ACC/MFC, is thus strategically located to foster interactions between the emotional and cognitive functions subserved by these regions (Bush et al, 2000; Greicius et al, 2003).
Our previous imaging studies have reported rCBF decrease in the hippocampus in association with either haloperidol or clozapine treatment (Lahti et al, 2003). In addition, we have reported that, compared with the normal volunteers, drug-free schizophrenia patients show increased rCBF in the hippocampus, a difference that ‘normalizes’ after haloperidol treatment (Medoff et al, 2001). Liddle et al (2000) reported that the magnitude of metabolism decrease in the left hippocampus after a single dose of risperidone predicted the subsequent reduction in delusions and hallucinations.
In this study, on administration of each drug, we observed a significant rCBF decrease in the medial temporal cortex after 1 week of treatment. At week 6, a significant hippocampal rCBF decrease was observed in the haloperidol group, whereas in the olanzapine group, the decrease was only observed at a liberal threshold (p<0.05). In addition, at week 1, good responders, in contrast to poor responders in either treatment group, showed greater rCBF decrease in the hippocampus. Thus, consistent with the study by Liddle et al (2000), we found that the response in the hippocampus seems to index an early neuronal response to APDs.
Neocortex
On administering haloperidol, the major pattern of functional changes seen in the cortex was that of rCBF deactivation. On the other hand, the pattern seen with olanzapine was that of cortical activation. These opposite cortical patterns were observed in another group of drug-free patients who were scanned after single-dose administration of either haloperidol or olanzapine (Lahti et al, 2005). One might speculate about the therapeutic implication and the mechanism(s) by which such a cortical activation could be achieved with olanzapine. Although the effect of olanzapine in treating positive symptoms is qualitatively similar to that of first-generation drugs, its spectrum of effects may be broader (Davis and Chen, 2001). In the CATIE study, olanzapine treatment was associated with the lowest discontinuation rates in comparison with several second-generation APD and fluphenazine. In addition, in a group of first-episode patients, olanzapine treatment (Keefe et al, 2004) was associated with a greater improvement on the task of information processing and speed compared with low-dose haloperidol.
It is possible that olanzapine's action on other neurotransmitter systems is responsible for its functional effect on cortical regions. Olanzapine induces IEG expression in the medial prefrontal cortex, an effect that is not seen with haloperidol. Several laboratories have shown that olanzapine increases dopamine release in the prefrontal cortex, an action possibly related to its serotonin and/or noradrenergic receptor affinity (Moghaddam and Bunney, 1999; Pehek, 1996; Rollema et al, 1997; Youngren et al, 1999). In addition, olanzapine can antagonize the effects of NMDA antagonists in a variety of experimental designs, including the reversal of PCP-induced deficits in prepulse inhibition (Bakshi and Geyer, 1995). 6-Hydroxydopamine lesions of the VTA that caused dystrophic changes in cortical projection neurons are reversed with olanzapine, but not with haloperidol (Wang and Deutch, 2008), suggesting that olanzapine can exert a trophic effect on lesioned cortical neurons. Speculatively, the functional activation seen in cortical regions might suggest a mechanism by which olanzapine, but not haloperidol, prevents progressive cortical contraction in first-episode schizophrenia (Lieberman et al, 2005). In that study, less improvement in cognitive function after 12 weeks of haloperidol treatment was associated with greater decrease in gray matter volumes, an effect that is not seen with olanzapine. In our study, good response in the olanzapine group was associated with less cortical activation during a resting state. We have reported that, during cognitive task, in the olanzapine, but not in the haloperidol group, rCBF in the ACC/MFC was significantly and positively correlated with improvement in processing speed (Lahti et al, 2005).
Week 1 rCBF Patterns in GR vs PR
These preliminary data point to important drug-induced regional modulation differences in the ventral striatum and hippocampus between PR and GR. As these patterns were not seen in the placebo group, they cannot be explained by subjective reaction to treatment. These patterns of rCBF changes may represent important biomarkers of treatment response.
These data are in agreement with those of Buchsbaum et al (1992, 2007), who found that lower pretreatment and greater increase in striatal metabolic rate with treatment were linked to better clinical response to APDs. Likewise, Cohen et al (1998) found that high pretreatment basal ganglia rates predicted poor treatment response to APDs. Treatment-resistant patients who became responders to clozapine showed higher basal ganglia perfusion compared with those who did not (Rodriguez et al, 1997). As discussed previously, Liddle et al (2000) reported that the metabolism decrease in the hippocampus after a single dose of risperidone predicted subsequent reduction in delusions and hallucinations.
Implication for Antipsychotic Action
These data point to an important role of the ventral striatum in antipsychotic action: increased ventral striatum activity in the early stage of treatment is predictive of treatment response. Imaging studies have shown that, compared with normal volunteers, drug-free patients with schizophrenia have excessive amphetamine-induced release of striatal dopamine DA (Laruelle et al, 1996). In addition, this elevated evoked release of striatal DA in drug-free schizophrenia patients was found to be predictive of treatment response (Abi-Dargham et al, 2000).
The ventral striatum receives glutamatergic (GLU) inputs from multiple regions of the PFC, the hippocampus, the amgydala and the thalamus, and DA inputs originating mainly from the VTA. These inputs synapse on the dendritic spines and shafts of medium-sized GABA-ergic projection neurons (Kotter, 1994; Starr, 1995). The convergence of DA and GLU on the spiny neurons provides a potent modulatory interaction between these neurotransmitters. As DA is known to exert a potent inhibitory effect on GLU neurotransmission (Morari et al, 1998), it is possible that, in good treatment responders, D2 blockade restores GLU transmission that was inhibited through elevated DA. Improved GLU transmission in the VS might result in improved neuronal transmission in projected areas. We have hypothesized that the early physiological processes that lead to therapeutic benefit are related to changes in GLU transmission within the VS and in GLU-mediated projections to limbic regions (Figure 6). Putatively, changes in the ventral striatum and hippocampus rCBF might index neuronal events related to the early stages of drug response, whereas rCBF changes in the ACC/MFC might relate to a more ‘consolidated’ drug response.
APD action likely occurs first in the DA D2-receptor rich ventral striatum (VS), in which DA afferents from the ventral tegmental area (VTA) and glutamatergic (GLU) afferents from the PFC converge on the same spiny neurons, which, in turn, project to the ventral pallidum (VP). The GABA-ergic efferents of the VP project to the thalamus, where they synapse on GLU neurons projecting to the PFC. In good treatment responders, D2 blockade restores GLU transmission, which was inhibited through elevated DA, leading to restored neurotransmission in the VS and projection areas, including the hippocampus and the anterior cingulate cortex (ACC). In poor responders (PR), these processes are impaired and the restoration of GLU transmission is not achieved.
Clinical Implication
Clinicians face the following difficult decisions when managing their patients' antipsychotic medications: how long should an adequate trial of APD last, when is the correct dosing achieved, will the patient experience a relapse if a switch from one APD to another is initiated. In addition, patients who are non-responsive to at least two APDs should be considered for a clozapine trial, a difficult decision considering the risks of agranulocytosis, seizure, and metabolic syndrome. The availability of biomarkers of treatment response could help guide the dosing and duration of treatment questions. Early detection of drug response could yield specific treatment strategies that are tailored to the individual, thus improving the quality of life of patients and drastically reducing the cost associated with treatment strategies that may not work. In addition, understanding the mechanisms underlying drug response could enhance the development of more effective and selectively targeted antipsychotic agents.
Limitations of the Study
A 2-week withdrawal is likely not enough to allow medication-induced brain changes to fully revert to a baseline condition. However, the potent rCBF increase observed in the dorsal and ventral striatum on haloperidol administration strongly suggests that DA receptors were not blocked by residual medication. As schizophrenia volunteers were taken off their medication for only 2 weeks before the treatment phase of the study, their clinical status was likely different from that of a relapsed state. This might limit the generalization of these data. Another important limitation of this study is the limited number of volunteers at each time point, especially in the GR vs PR analysis. In addition, one has to keep in mind that increases in CBF do not necessarily mean that there is overall neuronal activation (excitation), but that the CBF reflects the metabolic substrate of many neurons that are activated and deactivated by excitatory and inhibitory processes.
References
Abi-Dargham A, Rodenhiser J, Printz D, Zea-Ponce Y, Gil R, Kegeles LS et al (2000). Increased baseline occupancy of D2 receptors by dopamine in schizophrenia. Proc Natl Acad Sci USA 97: 8104–8109.
Agid O, Kapur S, Arenovich T, Zipursky RB (2003). Delayed-onset hypothesis of antipsychotic action: a hypothesis tested and rejected. Arch Gen Psychiatry 60: 1228–1235.
Alexander GE, Crutcher MD (1990). Ganglia-thalamocortical circuits: parallel substrates for motor, oculomotor, ‘prefrontal’ and ‘limbic’ functions. Prog Brain Res 85: 119–146.
Amodio DM, Frith CD (2006). Meeting of minds: the medial frontal cortex and social cognition. Nat Rev Neurosci 7: 268–277.
Bakshi VP, Geyer MA (1995). Antagonism of phencyclidine-induced deficits in prepulse inhibition by the putative atypical antipsychotic olanzapine. Psychopharmacology (Berl) 122: 198–201.
Buchsbaum MS, Haznedar MM, Aronowitz J, Brickman AM, Newmark RE, Bloom R et al (2007). FDG-PET in never-previously medicated psychotic adolescents treated with olanzapine or haloperidol. Schizophr Res 94: 293–305.
Buchsbaum MS, Potkin SG, Siegel Jr BV, Lohr J, Katz M, Gottschalk LA et al (1992). Striatal metabolic rate and clinical response to neuroleptics in schizophrenia. Arch Gen Psychiatry 49: 966–974.
Bush GP, Luu P, Posner MI (2000). Cognitive and emotional influences in anterior cingulate cortex. Trends Cogn Sci 4: 215–222.
Chiodo LA, Bunney BS (1983). Typical and atypical neuroleptics: differential effects of chronic administration on the activity of A9 and A10 midbrain dopaminergic neurons. J Neurosci 3: 1607–1619.
Cohen RM, Nordahl TE, Semple WE, Andreason P, Pickar D (1998). Abnormalities in the distributed network of sustained attention predict neuroleptic treatment response in schizophrenia. Neuropsychopharmacology 19: 36–47.
Davis JM, Chen N (2001). The effects of olanzapine on the 5 dimensions of schizophrenia derived by factor analysis: combined results of the North American and international trials. J Clin Psychiatry 62: 757–771.
Friston KJ, Holmes A, Poline JB, Price CJ, Frith CD (1996). Detecting activations in PET and fMRI: levels of inference and power. Neuroimage 4: 223–235.
Gelder MG, Lopez-Ibar JJ, Andreasen N (2000). New Oxford Textbook of Psychiatry. Oxford University Press: New York, NY.
Grace AA, Bunney BS (1995). Electrophysiological Properties of Midbrain Dopamine Neurons Psychopharmacology. Raven Press: New York. pp 163–177.
Greicius MD, Krasnow B, Reiss AL, Menon V (2003). Functional connectivity in the resting brain: a network analysis of the default mode hypothesis. Proc Natl Acad Sci USA 100: 253–258.
Harrow M, Sands JR, Silverstein ML, Goldberg JF (1997). Course and outcome for schizophrenia versus other psychotic patients: a longitudinal study. Schizophr Bull 23: 287–303.
Hedlund JL, Vieweg BW (1980). The brief psychiatric rating scale (BPRS): a comprehensive view. J Oper Psychiatry 11: 48–64.
Holcomb HH, Cascella NG, Thaker GK, Medoff DR, Dannals RF, Tamminga CA (1996). Functional sites of neuroleptic drug action in the human brain: PET/FDG studies with and without haloperidol. Am J Psychiatry 153: 41–49.
Keefe RS, Seidman LJ, Christensen BK, Hamer RM, Sharma T, Sitskoorn MM et al (2004). Comparative effect of atypical and conventional antipsychotic drugs on neurocognition in first-episode psychosis: a randomized, double-blind trial of olanzapine versus low doses of haloperidol. Am J Psychiatry 161: 985–995.
Kessler RM, Ansari MS, Riccardi P, Li R, Jayathilake K, Dawant B et al (2005). Occupancy of striatal and extrastriatal dopamine D2/D3 receptors by olanzapine and haloperidol. Neuropsychopharmacology 30: 2283–2289.
Kotter R (1994). Postsynaptic integration of glutamatergic and dopaminergic signals in the striatum. Prog Neurobiol 44: 163–196.
Lahti AC, Holcomb HH, Weiler MA, Medoff DR, Tamminga CA (2003). Functional effects of antipsychotic drugs: comparing clozapine with haloperidol. Biol Psychiatry 53: 601–608.
Lahti AC, Holcomb HH, Weiler MA, Medoff DR, Frey KN, Hardin M et al (2004). Clozapine but not haloperidol re-establishes normal task-activated rCBF patterns in schizophrenia within the anterior cingulate cortex. Neuropsychopharmacology 29: 171–178.
Lahti AC, Holcomb HH, Tamminga CA, Gold JM, Weiler MA et al (2005). Functional Effects of Haloperidol and Olanzapine During a 6 Week Treatment Period and Relations to Clinical Response. American College of Neuropsychopharmacology; Hawaii.
Lahti AC, Weiler MA, Medoff DR, Tamminga CA, Holcomb HH (2005). Functional effects of single dose first- and second-generation antipsychotic administration in subjects with schizophrenia. Psychiatry Res 139: 19–30.
Lahti AC, Weiler MA, Holcomb HH, Tamminga CA, Carpenter WT, McMahon R (2006). Correlations between rCBF and symptoms in two independent cohorts of drug-free patients with schizophrenia. Neuropsychopharmacology 31: 221–230.
Laruelle M, Abi-Dargham A, van Dyck CH, Gil R, D′Souza CD, Erdos J et al (1996). Single photon emission computerized tomography imaging of amphetamine-induced dopamine release in drug-free schizophrenic subjects. Proc Natl Acad Sci USA 93: 9235–9240.
Leucht S, Kane JM, Kissling W, Hamann J, Etschel E, Engel R (2005). Clinical implications of Brief Psychiatric Rating Scale scores. Br J Psychiatry 187: 366–371.
Liddle PF, Lane CJ, Ngan ET (2000). Immediate effects of risperidone on cortico-striato-thalamic loops and the hippocampus. Br J Psychiatry 177: 402–407.
Lieberman JA, Tollefson GD, Charles C, Zipursky RB, Sharma T, Kahn RS et al (2005). Antipschotic drug effects on brain morphology in first-episode pyschosis. Arch Gen Psychiatry 62: 361–370.
Marder SR, Van-Kammen DP (2000). Dopamine receptor antagonists. In: Kaplan HI, Sadock, B.J. (eds) Comprehensive Textbook of Psychiatry. Lippincott Williams & Wilkins: Baltimore, MD. pp 2356–2377.
McEvoy JP, Lieberman JA, Stroup TS, Davis SM, Meltzer HY, Rosenheck RA et al (2006). Effectiveness of clozapine versus olanzapine, quetiapine, and risperidone in patients with chronic schizophrenia who did not respond to prior atypical antipsychotic treatment. Am J Psychiatry 163: 600–610.
Medoff DR, Holcomb HH, Lahti AC, Tamminga CA (2001). Probing the human hippocampus using rCBF: contrasts in schizophrenia. Hippocampus 11: 543–550.
Miller DD, Andreasen NC, O′Leary DS, Rezai K, Watkins GL, Ponto LL et al (1997). Effect of antipsychotics on regional cerebral blood flow measured with positron emission tomography. Neuropsychopharmacology 17: 230–240.
Moghaddam B, Bunney BS (1999). Acute effects of typical and atypical antipsychotic drugs on the release of dopamine from prefrontal cortex, nucleus accumbens, and striatum of prefrontal cortex, and striatum of the rat: an in vivo microdialysis study. Neuropharmacology 20: 1755–1760.
Morari M, Marti M, Sbrenna S, Fuxe K, Bianchi C, Beani L (1998). Reciprocal dopamine-glutamate modulation of release in the basal ganglia. Neurochem Int 33: 383–397.
Ngan ET, Lane CJ, Ruth TJ, Liddle PF (2002). Immediate and delayed effects of risperidone on cerebral metabolism in neuroleptic naive schizophrenic patients: correlations with symptom change. J Neurol Neurosurg Psychiatry 72: 106–110.
Overall JE, Gorham DR (1962). The Brief Psychiatric Rating Scale. Psychol Rep 10: 799–812.
Pehek EA (1996). Local infusion of the serotonin antagonists ritanserin or ICS 205 930 increases in vivo dopamine release in the rat medial prefrontal cortex. Synapse 24: 12–18.
Price CJ, Friston KJ (1997). Cognitive conjunction: a new approach to brain activation experiments. Neuroimage 5: 261–270.
Raichle ME, Marti WR, Hersevitch P, Mintun MA, Markha J (1983). Brain blood flow measured with intravenous H2 15O implementation and validation. J Nucl Med 24: 790–798.
Robertson GS, Fibiger HC (1992). Neuroleptics increase c-fos expression in the forebrain: contrasting effects of haloperidol and clozapine. Neuroscience 46: 315–328.
Robertson GS, Fibiger HC (1996). Effects of Olanazaping on regional C-Fos expression in rat forebrain. Neuropsychopharmaology 14: 105–110.
Rodriguez VM, Andree RM, Castejon MJ, Zamora ML, Alvaro PC, Delgado JL et al (1997). Fronto-striato-thalamic perfusion and clozapine response in treatment-refractory schizophrenic patients. A 99mTc-HMPAO study. Psychiatry Res 76: 51–61.
Rollema H, Lu Y, Schmidt AW, Zorn SH (1997). Clozapine increases dopamine release in prefrontal cortex by 5-HT1A receptor activation. Eur J Pharmacol 338: R3–R5.
Sikich L, Hamer RM, Bashford RA, Sheitman BB, Lieberman JA (2004). A pilot study of risperidone, olanzapine, and haloperidol in psychotic youth: a double-blind, randomized, 8-week trial. Neuropsychopharmacology 29: 133–145.
Spitzer RL, Williams JBW, Gibbon M (1987). Structured Clinical Interview for DSM III-R (SCID) P.B.
Starr MS (1995). Glutamate/dopamine D1/D2 balance in the basal ganglia and its relevance to Parkinson's disease. Synapse 19: 264–293.
Tamminga CA, Dannals RF, Frost JJ, Wong D, Wanger HN et al (1993). Neuroreceptor and neurochemistry studies with positron emission tomography in psychiatric illness: promise and progress. American Psychiatric Press: Washington, DC.
van den Oord EJ, Adkins DE, McClay J, Lieberman J, Sullivan PF (2009). A systematic method for estimating individual responses to treatment with antipsychotics in CATIE. Schizophr Res 107: 13–21.
Wang HD, Deutch AY (2008). Dopamine depletion of the prefrontal cortex induces dendritic spine loss: reversal by atypical antipsychotic drug treatment. Neuropsychopharmacology 33: 1276–1286.
White FJ, Wang RY (1983). Differential effects of classical and atypical antipsychotic drugs on A9 and A10 dopamine neurons. Science 221: 1054–1057.
Youngren KD, Inglis FM, Pivirotto PJ, Jedema HP, Bradberry CW, Goldman-Rakic PS et al (1999). Clozapine preferentially increases dopamine release in the rhesus monkey prefrontal cortex compared with the caudate nucleus. Neuropsychopharmacology 20: 403–412.
Acknowledgements
The National Institute of Mental Health Grants RO1MH57971 (ACL) and P30-MH40279 (IRC) supported this work. The authors thank all the volunteers with schizophrenia who took part in this project: Dale Warfel, Tamara Michaelidis, Stacey Lee, Angela DeSantis, and the nursing staff of the RRU of the Maryland Psychiatric Research Center for clinical care.
Author information
Authors and Affiliations
Corresponding author
Additional information
DISCLOSURE
Adrienne Lahti, Martin Weiler, Henry Holcomb, and Karen Cropsey have no financial interests to disclose. Carol Tamminga serves as a consultant and/ or advisor for Acadia Pharmaceuticals, Intracellular Therapies, Lilly Pharmaceutical, Alexza Pharmaceuticals, and Lundbeck.
Rights and permissions
About this article
Cite this article
Lahti, A., Weiler, M., Holcomb, H. et al. Modulation of Limbic Circuitry Predicts Treatment Response to Antipsychotic Medication: A Functional Imaging Study in Schizophrenia. Neuropsychopharmacol 34, 2675–2690 (2009). https://doi.org/10.1038/npp.2009.94
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2009.94
Keywords
This article is cited by
-
Disrupted subcortical functional connectome gradient in drug-naïve first-episode schizophrenia and the normalization effects after antipsychotic treatment
Neuropsychopharmacology (2023)
-
Anterior cingulate glutamate metabolites as a predictor of antipsychotic response in first episode psychosis: data from the STRATA collaboration
Neuropsychopharmacology (2023)
-
Changes in corticostriatal connectivity and striatal tissue iron associated with efficacy of clozapine for treatment‑resistant schizophrenia
Psychopharmacology (2022)
-
Influence of cytochrome P450 2D6 polymorphism on hippocampal white matter and treatment response in schizophrenia
npj Schizophrenia (2021)
-
Increased subcortical region volume induced by electroconvulsive therapy in patients with schizophrenia
European Archives of Psychiatry and Clinical Neuroscience (2021)