Abstract
Palliative care aims to improve the quality of life of patients and their families affected by life-threatening illness. This approach applies to a large and growing proportion of neurological disorders, most prominently stroke and dementia. Challenges in the palliative care of patients with incurable neurological diseases include the broad spectrum of the rate of symptom progression, a lack of reliable prognostic markers, scarcity of evidence for efficacy of symptomatic treatments, and a high prevalence of difficulties with communication, cognitive impairment and behavioural disturbances. A genuinely multidisciplinary approach to neurological palliative care is, therefore, required. However, palliative care is not an integral part of neurological training in most countries. This Perspectives article aims to underscore the importance of integrating palliative care into daily clinical practice. The basic principles and challenges of neurological palliative care are also outlined in the light of relevant literature.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
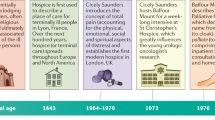
Clark, D. Religion, medicine, and community in the early origins of St. Christopher's Hospice. J. Palliat. Med. 4, 353–360 (2001).
Oliver, D., Borasio, G. D. & Walsh, D. (Eds) Palliative Care in Amyotrophic Lateral Sclerosis—from Diagnosis to Bereavement 2nd edn (Oxford University Press, Oxford, 2006).
Andersen, P. et al. EFNS guidelines on the Clinical Management of Amyotrophic Lateral Sclerosis (MALS)—revised report of an EFNS task force. Eur. J. Neurol. 19, 360–375 (2012).
Fritze, J., Diedrich, U. & Ziegenhagen, D. J. Pflegeversicherung: Härtefälle bei den Privaten [German]. Dtsch. Arztebl. 96, A2654–A2666 (1999).
Projections of mortality and burden of disease 2004–2030. World Health Organization: health statistics and health informations systems [online], (2012).
Voltz, R. et al. (Eds) Palliative Care in Neurology (Oxford University Press, Oxford, 2004).
The American Academy of Neurology Ethics and Humanities Subcommittee. Palliative care in neurology. Neurology 46, 870–872 (1996).
EAPC taskforce on the development of guidelines and a core curriculum for the palliative care for people with neurological disease. European Association for Palliative Care [online], (2012).
Dy, S. M. & Feldman, D. R. Palliative care and rehabilitation for stroke survivors: managing symptoms and burden, maximizing function. J. Gen. Intern. Med. 27, 760–762 (2012).
Müller, J. et al. Progression of dysarthria and dysphagia in postmortem-confirmed parkinsonian disorders. Arch. Neurol. 58, 259–264 (2001).
Traynor, B. J., Alexander, M., Corr, B., Frost, E. & Hardiman, O. Effect of a multidisciplinary amyotrophic lateral sclerosis (ALS) clinic on ALS survival: a population based study, 1996–2000. J. Neurol. Neurosurg. Psychiatry 74, 1258–1261 (2003).
Khot, S., Billings, M., Owens, D. & Longstreth, W. T. Jr. Coping with death and dying on a neurology inpatient service: death rounds as an educational initiative for residents. Arch. Neurol. 68, 1395–1397 (2011).
Turner-Stokes, L. Sykes, N. & Silber, E. Guideline Development Group. Long-term neurological conditions: management at the interface between neurology, rehabilitation and palliative care. Clin. Med. 8, 186–191 (2008).
van der Steen, J. T. Dying with dementia: what we know after more than a decade of research. J. Alzheimers Dis. 22, 37–55 (2010).
Volicer, L. Goals of care in advanced dementia: quality of life, dignity and comfort. J. Nutr. Health Aging 11, 481 (2007).
Creutzfeldt, C. J., Holloway, R. G. & Walker, M. Symptomatic and palliative care for stroke survivors. J. Gen. Intern. Med. 27, 853–860 (2012).
Burton, C. R., Payne, S., Addington-Hall, J. & Jones, A. The palliative care needs of acute stroke patients: a prospective study of hospital admissions. Age Ageing 39, 554–559 (2010).
Oliver, D. J. et al. Medication in the last days of life for motor neuron disease/amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. 11, 562–564 (2010).
Bede, P. et al. Palliative care in amyotrophic lateral sclerosis: a review of current international guidelines and initiatives. J. Neurol. Neurosurg. Psychiatry. 82, 413–418 (2011).
Miyasaki, J. M. et al. Palliative care for advanced Parkinson disease: an interdisciplinary clinic and new scale, the ESAS-PD. Parkinsonism Relat. Disord. 18 (Suppl. 3), S6–S9 (2012).
McLaughlin, D. et al. Living and coping with Parkinson's disease: perceptions of informal carers. Palliat. Med. 25, 177–182 (2011).
Higginson, I. J., Costantini, M., Silber, E., Burman, R. & Edmonds, P. Evaluation of a new model of short-term palliative care for people severely affected with multiple sclerosis: a randomised fast-track trial to test timing of referral and how long the effect is maintained. Postgrad. Med. J. 87, 769–775 (2011).
Golla, H., Galushko, M., Pfaff, H. & Voltz, R. Unmet needs of severely affected multiple sclerosis patients: the health professionals' view. Palliat. Med. 26, 139–151 (2012).
Hui, D. et al. Quantity, design, and scope of the palliative oncology literature. Oncologist 16, 694–703 (2011).
Doyle, D. & O'Connell, S. Breaking bad news: starting palliative care. J. R. Soc. Med. 89, 590–591 (1996).
Chiò, A. & Borasio, G. D. Breaking the news in amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. Other Motor Neuron Disord. 5, 195–201 (2004).
Kierkegaard, S. in, S. K. et al. Die Schriften über sich selbst [German] (ed. Diederichs, E.) 38–39 (Verlag, Regensburg, 1951).
van der Graaff, M. M. et al. Vocal cord dysfunction in amyotrophic lateral sclerosis: four cases and a review of the literature. Arch. Neurol. 66, 1329–1333 (2009).
Lorenzl, S. et al. Nonconvulsive status epilepticus in palliative care patients. J. Pain Symptom Manage. 40, 460–465 (2010).
Li, L. L., Cheong, K. Y., Yaw, L. K. & Liu, E. H. The accuracy of surrogate decisions in intensive care scenarios. Anaesth. Intensive Care. 35, 46–51 (2007).
Feil, N. & de Klerk-Rubin, V. The Validation Breakthrough: Simple Techniques for Communicating with People with Alzheimer's-Type Dementia (Health Professions Press, Baltimore, 2002).
WHO (Eds). National Cancer Control Programmes: Policies and Managerial Guidelines 2nd edn 83–91 (WHO, Geneva, 2002).
Neudert, C., Wasner, M. & Borasio, G. D. Individual quality of life is not correlated with health-related quality of life or physical function in patients with amyotrophic lateral sclerosis. J. Palliat. Med. 7, 551–557 (2004).
Fegg, M. J., Wasner, M., Neudert, C. & Borasio, G. D. Personal values and individual quality of life in palliative care patients. J. Pain Symptom. Manage. 30, 154–159 (2005).
Fegg, M. et al. Meaning in life in patients with amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. 11, 469–474 (2010).
Chiò, A. et al. A cross sectional study on determinants of quality of life in ALS. J. Neurol. Neurosurg. Psychiatry 75, 1597–1601 (2004).
Rodin, G. et al. Pathways to distress: the multiple determinants of depression, hopelessness, and the desire for hastened death in metastatic cancer patients. Soc. Sci. Med. 68, 562–569 (2009).
Breitbart, W. et al. Pilot randomized controlled trial of individual meaning-centered psychotherapy for patients with advanced cancer. J. Clin. Oncol. 30, 1304–1309 (2012).
Balboni, T. et al. Support of cancer patients' spiritual needs and associations with medical care costs at the end of life. Cancer 117, 5383–5391 (2011).
Rabkin, J. G., Wagner, G. J. & Del Bene, M. Resilience and distress among amyotrophic lateral sclerosis patients and caregivers. Psychosom. Med. 62, 271–279 (2000).
Maltoni, M. et al. Palliative sedation in end-of-life care and survival: a systematic review. J. Clin. Oncol. 30, 1378–1383 (2012).
Jox, R. J. et al. Surrogate decision making for patients with end-stage dementia. Int. J. Geriatr. Psychiatry 27, 1045–1052 (2012).
Vandervoort, A. et al. Advance directives and physicians' orders in nursing home residents with dementia in Flanders, Belgium: prevalence and associated outcomes. Int. Psychogeriatr. 24, 1133–1143 (2012).
Seeber, A. A., Hijdra, A., Vermeulen, M. & Willems, D. L. Discussions about treatment restrictions in chronic neurologic diseases: a structured review. Neurology 78, 590–597 (2012).
Dush, D. M. High-tech, aggressive palliative care: in the service of quality of life. J. Palliat. Care 9, 37–41 (1993).
Acknowledgements
I would like to thank Wendy Johnston (Edmonton, Canada), David Oliver (Rochester, UK) and Raymond Voltz (Cologne, Germany) for helpful discussions over many years and critical appraisal of the manuscript.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Borasio, G. The role of palliative care in patients with neurological diseases. Nat Rev Neurol 9, 292–295 (2013). https://doi.org/10.1038/nrneurol.2013.49
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2013.49
This article is cited by
-
Neurological update: the palliative care landscape for atypical parkinsonian syndromes
Journal of Neurology (2023)
-
Development and psychometric evaluation of a new tool for measuring the attitudes of patients with progressive neurological diseases to ethical aspects of end-of-life care
BMC Medical Ethics (2020)
-
Understanding patients’ and caregivers’ perspectives and educational needs in Parkinson’s disease: a multi-ethnic Asian study
Neurological Sciences (2020)
-
Better palliative care for people with a dementia: summary of interdisciplinary workshop highlighting current gaps and recommendations for future research
BMC Palliative Care (2018)
-
The Promise of Telemedicine for Movement Disorders: an Interdisciplinary Approach
Current Neurology and Neuroscience Reports (2018)