Abstract
Fibromyalgia is a disorder characterized by chronic widespread pain in the presence of widespread tenderness, and multiple somatic symptoms. Since the publication of the American College of Rheumatology (ACR) 1990 classification criteria for fibromyalgia, research has proliferated and, in a relatively short period, investigators have begun to unravel the etiology and long-term impact of this complex condition. Although the ACR 1990 criteria have been central to fibromyalgia research during the past two decades, a number of practical and philosophical objections have been raised in relation to them. Principally these objections have centered on the use (or lack thereof) of the tender point examination, the lack of consideration of associated symptoms, and the observation that fibromyalgia might represent the extreme end of a pain continuum. In developing the ACR 2010 criteria, experts have sought to address these issues and to simplify clinical diagnosis. An implicit aim was to facilitate more rigorous study of etiology. The purpose of this Review is to summarize research to date that has described the epidemiology, pathology and clinical course of fibromyalgia, and to assess the probable impact of the ACR 2010 criteria on future research efforts.
Key Points
-
Although the American College of Rheumatology (ACR) 1990 classification criteria for fibromyalgia have facilitated two decades of research, several practical and philosophical objections to them have been raised
-
The ACR 2010 diagnostic criteria were developed to address obstacles and concerns presented in response to the 1990 criteria
-
The ACR 2010 diagnostic criteria comprise a widespread pain index (WPI, measures pain distribution), and the symptom severity (SS) scale (assesses cognitive symptoms, sleep disturbances, fatigue and somatic symptoms)
-
The maximum WPI score is 19, the SS score range is 0–12; WPI≥7 and SS≥5, or WPI 3–6 and SS≥9, classifies individuals as having fibromyalgia
-
Use of the traditional tender-point count is not required in the ACR 2010 criteria
-
The ACR 2010 criteria should facilitate more rigorous study of the etiology of fibromyalgia
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Wolfe, F. et al. The American College of Rheumatology 1990 Criteria for the Classification of Fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum. 33, 160–172 (1990).
Wolfe, F. et al. The American College of Rheumatology preliminary diagnostic criteria for fibromyalgia and measurement of symptom severity. Arthritis Care Res. (Hoboken.) 62, 600–610 (2010).
Gowers, W. R. Lumbago: Its lessons and analogues. Br. Med. J. 1, 117–121 (1904).
Stockman, R. The causes, pathology, and treatment of chronic rheumatism. Edinburgh Medical Journal 15, 107–116 (1904).
Smythe, H. A. Non-articular rheumatism and the fibrosists syndrome in Arthritis and Allied Conditions (ed. Hollander, J. L.) 874–884 (Lea & Febiger, 1972).
Hench, P. K. Fibrositis. Arthritis Rheum. 196, 1087–1088 (1975).
Smythe, H. A. & Moldofsky, H. Two contributions to understanding of the “fibrositis” syndrome. Bull. Rheum. Dis. 28, 928–931 (1977).
Yunus, M., Masi, A. T., Calabro, J. J., Miller, K. A. & Feigenbaum, S. L. Primary fibromyalgia (fibrositis): clinical study of 50 patients with matched normal controls. Semin. Arthritis Rheum. 11, 151–171 (1981).
Goldenberg, D. L. Fibromyalgia syndrome. An emerging but controversial condition. Journal of American Medical Association 257:20, 2782–2787 (1987).
Wolfe, F. & Cathey, M. A. Prevalence of primary and secondary fibrositis. J. Rheumatol. 10, 965–968 (1983).
McBeth, J. & Jones, K. A. Epidemiology of chronic musculoskeletal pain. Best. Pract. Res. Clin. Rheumatol. 21, 403–425 (2007).
McBeth, J. et al. The prevalence of “unexplained” chronic widespread pain in the general population: Results from the General Practice Symptoms Study. Rheumatology 47 [S2], ii184. 2008. Ref Type: Abstract.
McBeth, J., Nicholl, B. I., Cordingley, L., Davies, K. A. & Macfarlane, G. J. Chronic widespread pain predicts physical inactivity: results from the prospective EPIFUND study. Eur. J. Pain 14, 972–979 (2010).
Croft, P., Rigby, A. S., Boswell, R., Schollum, J. & Silman, A. The prevalence of chronic widespread pain in the general population. J. Rheumatol. 20, 710–713 (1993).
Wolfe, F., Ross, K., Anderson, J., Russell, I. J. & Hebert, L. The prevalence and characteristics of fibromyalgia in the general population. Arthritis Rheum. 38, 19–28 (1995).
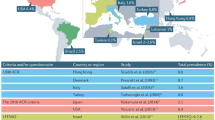
McBeth, J. The epidemiology of chronic widespread pain and fibromyalgia in Fibromyalgia and other central pain syndromes (eds. Wallace, D. J. & Clauw, D. J.) 17–28 (Lippincott Williams & Wilkins, Philidelphia, 2005).
Leveille, S. G. et al. Chronic musculoskeletal pain and the occurrence of falls in an older population. JAMA 302, 2214–2221 (2009).
Thomas, E., Peat, G., Harris, L., Wilkie, R. & Croft, P. R. The prevalence of pain and pain interference in a general population of older adults: cross-sectional findings from the North Staffordshire Osteoarthritis Project (NorStOP). Pain 110, 361–368 (2004).
White, K. P. & Harth, M. Classification, epidemiology, and natural history of fibromyalgia. Current Pain & Headache Reports. 5, 320–329 (2001).
Carmona, L., Ballina, J., Gabriel, R. & Laffon, A. The burden of musculoskeletal diseases in the general population of Spain: results from a national survey. Ann. Rheum. Dis. 60, 1040–1045 (2001).
Makela, M. & Heliovaara, M. Prevalence of primary fibromyalgia in the Finnish population. Br. Med. J. 303, 216–219 (1991).
Senna, E. R. et al. Prevalence of rheumatic diseases in Brazil: a study using the COPCORD approach. J. Rheumatol. 31, 594–597 (2004).
Lawrence, R. C. et al. Estimates of the prevalence of arthritis and selected musculoskeletal disorders in the United States. Arthritis Rheum. 41, 778–799 (1998).
Branco, J. C. et al. Prevalence of fibromyalgia: a survey in five European countries. Semin. Arthritis Rheum. 39, 448–453 (2010).
Macfarlane, G. J. et al. Evaluation of work-related psychosocial factors and regional musculoskeletal pain: results from a EULAR Task Force. Ann. Rheum. Dis. 68, 885–891 (2009).
McBeth, J. et al. Moderation of psychosocial risk factors through dysfunction of the hypothalamic-pituitary-adrenal stress axis in the onset of chronic widespread musculoskeletal pain: findings of a population-based prospective cohort study. Arthritis Rheum. 56, 360–371 (2007).
Chiu, Y. H. et al. Poor sleep and depression are independently associated with a reduced pain threshold. Results of a population based study. Pain 115, 316–321 (2005).
Gupta, A. et al. The role of psychosocial factors in predicting the onset of chronic widespread pain: results from a prospective population-based study. Rheumatology (Oxford) 46, 666–671 (2007).
Jones, E. A. et al. What characterizes persons who do not report musculoskeletal pain? Results from a 4-year population-based longitudinal study (the Epifund study). J. Rheumatol. 36, 1071–1077 (2009).
McBeth, J. et al. Hypothalamic-pituitary-adrenal stress axis function and the relationship with chronic widespread pain and its antecedents. Arthritis Res. Ther. 7, R992–R1000 (2005).
Robinson, K. L., McBeth, J. & Macfarlane, G. J. Psychological distress and premature mortality in the general population: a prospective study. Ann. Epidemiol. 14, 467–472 (2004).
Nicholl, B. I. et al. Premorbid psychosocial factors are associated with poor health-related quality of life in subjects with new onset of chronic widespread pain—results from the EPIFUND study. Pain 141, 119–126 (2009).
Davies, K. A. et al. Restorative sleep predicts the resolution of chronic widespread pain: results from the EPIFUND study. Rheumatology (Oxford) 47, 1809–1813 (2008).
Kennedy, M. & Felson, D. T. A prospective long-term study of fibromyalgia syndrome. Arthritis Rheum. 39, 682–685 (1996).
Waylonis, G. W. & Perkins, R. H. Post-traumatic fibromyalgia. A long-term follow-up. Am. J. Phys. Med. Rehabil. 73, 403–412 (1994).
Granges, G., Zilko, P. & Littlejohn, G. O. Fibromyalgia Syndrome: assessment of the severity of the condition 2 years after diagnosis. J. Rheumatol. 21, 523–529 (1994).
Bengtsson, A. & Backman, E. Long-term follow up of fibromyalgia patients. Scand. J. Rheumatol. 21, 98 (1992).
Walitt, B. et al. The longitudinal outcome of fibromyalgia: a study of 1555 patients. J. Rheumatol. 38, 2238–2246 (2011).
Noller, V. & Sprott, H. Prospective epidemiological observations on the course of the disease in fibromyalgia patients. J. Negat. Results Biomed. 2, 4 (2003).
van Koulil, S., van Lankveld, W., Kraaimaat, F., van Riel, P. & Evers, A. Risk factors for longer term psychological distress in well-functioning fibromyalgia patients: a prospective study into prognostic factors. Patient Educ. Couns. 80, 126–129 (2010).
Boehm, A., Eisenberg, E. & Lampel, S. The contribution of social capital and coping strategies to functioning and quality of life of patients with fibromyalgia. Clin. J. Pain 27, 233–239 (2011).
Wigers, S. H. Fibromyalgia outcome: The predictive value of symptom duration, physical activity, disability pension, and critical life events—a 4.5 year prospective study. J. Psychosom. Res. 41, 235–243 (1996).
Macfarlane, G. J. et al. The natural history of chronic pain in the community: a better prognosis than in the clinic? J. Rheumatol. 23, 1617–1620 (1996).
Papageorgiou, A. C., Silman, A. J. & Macfarlane, G. J. Chronic widespread pain in the population: a seven year follow up study. Ann. Rheum. Dis. 61, 1071–1074 (2002).
Carette, S. Fibromyalgia 20 years later: What have we really accomplished. J. Rheumatol. 22, 590–594 (1995).
Burckhardt, C. S. et al. Guideline for the management of fibromyalgia syndrome pain in adults and children in APS Clinical Practice Guideline Series No. 4 (American Pain Society, Glenview, IL, 2005).
Carville, S. F. et al. EULAR evidence-based recommendations for the management of fibromyalgia syndrome. Ann. Rheum. Dis. 67, 536–541 (2008).
Eich, W. et al. Definition, classification and diagnosis of fibromyalgia syndrome. Schmerz. 22, 255–266 (2008).
Di Franco, M. et al. Pharmacological treatment of fibromyalgia. Clin. Exp. Rheumatol. 28, S110–S116 (2010).
van Koulil S. et al. Tailored cognitive-behavioral therapy and exercise training for high-risk patients with fibromyalgia. Arthritis Care Res. (Hoboken.) 62, 1377–1385 (2010).
Hauser, W., Bernardy, K., Arnold, B., Offenbacher, M. & Schiltenwolf, M. Efficacy of multicomponent treatment in fibromyalgia syndrome: a meta-analysis of randomized controlled clinical trials. Arthritis Rheum. 61, 216–224 (2009).
Macfarlane, G. J., Norrie, G., Atherton, K., Power, C. & Jones, G. T. The influence of socioeconomic status on the reporting of regional and widespread musculoskeletal pain: results from the 1958 British Birth Cohort Study. Ann. Rheum. Dis. 68, 1591–1595 (2009).
Roizenblatt, S., Neto, N. S. & Tufik, S. Sleep Disorders and Fibromyalgia. Curr. Pain Headache Rep. 15, 347–357 (2011).
Ablin, J. N., Buskila, D. & Clauw, D. J. Biomarkers in fibromyalgia. Curr. Pain Headache Rep. 13, 343–349 (2009).
Jones, G. T. et al. Role of road traffic accidents and other traumatic events in the onset of chronic widespread pain: Results from a population-based prospective study. Arthritis Care Res. (Hoboken) 63, 696–701 (2011).
Mork, P. J., Vasseljen, O. & Nilsen, T. I. Association between physical exercise, body mass index, and risk of fibromyalgia: longitudinal data from the Norwegian Nord-Trondelag Health Study. Arthritis Care Res. (Hoboken) 62, 611–617 (2010).
Choi, C. J., Knutsen, R., Oda, K., Fraser, G. E. & Knutsen, S. F. The association between incident self-reported fibromyalgia and nonpsychiatric factors: 25-years follow-up of the Adventist Health Study. J. Pain 11, 994–1003 (2010).
Holliday, K. L. et al. Genetic variation in neuroendocrine genes associates with somatic symptoms in the general population: results from the EPIFUND study. J. Psychosom. Res. 68, 469–474 (2010).
Holliday, K. L. et al. Genetic variation in the hypothalamic-pituitary-adrenal stress axis influences susceptibility to musculoskeletal pain: results from the EPIFUND study. Ann. Rheum. Dis. 69, 556–560 (2010).
Geisser, M. E. et al. The association between experimental and clinical pain measures among persons with fibromyalgia and chronic fatigue syndrome. Eur. J. Pain 11, 202–207 (2007).
Staud, R. New evidence for central sensitization in patients with fibromyalgia. Curr. Rheumatol. Rep. 6, 259 (2004).
Staud, R., Nagel, S., Robinson, M. E. & Price, D. D. Enhanced central pain processing of fibromyalgia patients is maintained by muscle afferent input: a randomized, double-blind, placebo-controlled study. Pain 145, 96–104 (2009).
Yunus, M. B. Towards a model of pathophysiology of fibromyalgia: aberrant central pain mechanisms with peripheral modulation. J. Rheumatol. 19, 846–850 (1992).
Bennett, R. M., Jones, J., Turk, D. C., Russell, I. J. & Matallana, L. An internet survey of 2,596 people with fibromyalgia. BMC. Musculoskelet. Disord. 8, 27 (2007).
Clauw, D. J. Fibromyalgia: an overview. Am. J. Med. 122, S3–S13 (2009).
Dadabhoy, D., Crofford, L. J., Spaeth, M., Russell, I. J. & Clauw, D. J. Biology and therapy of fibromyalgia. Evidence-based biomarkers for fibromyalgia syndrome. Arthritis Res. Ther. 10, 211 (2008).
McBeth, J. An Epidemiological Study of Chronic Widespread Pain. Thesis, University of Manchester (2000).
McBeth, J., Macfarlane, G. J., Hunt, I. M. & Silman, A. J. Risk factors for persistent chronic widespread pain: a community-based study. Rheumatology (Oxford) 40, 95–101 (2001).
McBeth, J., Harkness, E. F., Silman, A. J. & Macfarlane, G. J. Mechanical injury and psychosocial factors in the work-place predict the onset of widespread body pain: a 2-year prospective study amongst cohorts of newly-employed workers. Arthritis Rheum. 48, S237 (2003).
McBeth, J., Macfarlane, G. J. & Silman, A. J. Does chronic pain predict future psychological distress? Pain 96, 239–245 (2002).
McBeth, J., Macfarlane, G. J., Benjamin, S. & Silman, A. J. Features of somatization predict the onset of chronic widespread pain: results of a large population-based study. Arthritis Rheum. 44, 940–946 (2001).
Davies, K. A. et al. The association between neighbourhood socio-economic status and the onset of chronic widespread pain: results from the EPIFUND study. Eur. J. Pain 13, 635–640 (2009).
Theadom, A., Cropley, M. & Humphrey, K. L. Exploring the role of sleep and coping in quality of life in fibromyalgia. J. Psychosom. Res. 62, 145–151 (2007).
Wolfe, F. & Pincus, T. Standard self-report questionnaires in routine clinical and research practice—An opportunity for patients and rheumatologists. J. Rheumatol. 18, 643–646 (1991).
Moldofsky, H. & Scarisbrick, P. Induction of neurasthenic musculoskeletal pain syndrome by selective sleep stage deprivation. Psychosom. Med. 38, 35–44 (1976).
Solitar, B. M. Fibromyalgia: knowns, unknowns, and current treatment. Bull. NYU Hosp. Jt Dis. 68, 157–161 (2010).
Aaron, L. A. et al. Perceived physical and emotional trauma as precipitating events in fibromyalgia. Associations with health care seeking and disability status but not pain severity. Arthritis Rheum. 40, 453–460 (1997).
White, K. P., Nielson, W. R., Harth, M., Ostbye, T. & Speechley, M. Chronic widespread musculoskeletal pain with or without fibromyalgia: psychological distress in a representative community adult sample. J. Rheumatol. 29, 588–594 (2002).
Al-Allaf, A. W. et al. A case–control study examining the role of physical trauma in the onset of fibromyalgia syndrome. Rheumatology. (Oxford) 41, 450–453 (2002).
Buskila, D., Neumann, L., Vaisberg, G., Alkalay, D. & Wolfe, F. Increased rates of fibromyalgia following cervical spine injury. A controlled study of 161 cases of traumatic injury. Arthritis Rheum. 40, 446–452 (1997).
Tishler, M., Levy, O., Maslakov, I., Bar-Chaim, S. & mit-Vazina, M. Neck injury and fibromyalgia—are they really associated? J. Rheumatol. 33, 1183–1185 (2006).
Tishler, M., Levy, O. & mit-Vazina, M. Can fibromyalgia be associated with whiplash injury? A 3-year follow-up study. Rheumatol. Int. 31, 1209–1213 (2010).
Wynne-Jones, G., Jones, G. T., Wiles, N. J., Silman, A. J. & Macfarlane, G. J. Predicting new onset of widespread pain following a motor vehicle collision. J. Rheumatol. 33, 968–974 (2006).
Matsuda, J. B. et al. Serotonin receptor (5-HT2A) and catechol-O-methyltransferase (COMT) gene polymorphisms: triggers of fibromyalgia? Rev. Bras. Reumatol. 50, 141–149 (2010).
Hocking, L. J. et al. Genetic variation in the β2-adrenergic receptor but not catecholamine-O-methyltransferase predisposes to chronic pain: results from the 1958 British Birth Cohort Study. Pain 149, 143–151 (2010).
Nicholl, B. I. et al. No evidence for a role of the catechol-O-methyltransferase pain sensitivity haplotypes in chronic widespread pain. Ann. Rheum. Dis. 69, 2009–2012 (2010).
Nicholl, B. I. et al. Association of HTR2A polymorphisms with chronic widespread pain and the extent of musculoskeletal pain: results from two population-based cohorts. Arthritis Rheum. 63, 810–818 (2011).
Lee, Y. H., Choi, S. J., Ji, J. D. & Song, G. G. Candidate gene studies of fibromyalgia: a systematic review and meta-analysis. Rheumatol. Int. http://dx.doi.org/10.1007/s00296-010-1678-9.
Nielsen, L. A. & Henriksson, K. G. Pathophysiological mechanisms in chronic musculoskeletal pain (fibromyalgia): the role of central and peripheral sensitization and pain disinhibition. Best. Pract. Res. Clin. Rheumatol. 21, 465–480 (2007).
Schmidt-Wilcke, T. & Clauw, D. J. Fibromyalgia: from pathophysiology to therapy. Nat. Rev. Rheumatol. 7, 518–527 (2011).
Clauw, D. J. Fibromyalgia: Update on mechanisms and management. J. Clin. Rheumatol. 13, 102–109 (2007).
Gracely, R. H., Petzke, F., Wolf, J. M. & Clauw, D. J. Functional magnetic resonance imaging evidence of augmented pain processing in fibromyalgia. Arthritis Rheum. 46, 1333–1343 (2002).
Staud, R., Robinson, M. E. & Price, D. D. Isometric exercise has opposite effects on central pain mechanisms in fibromyalgia patients compared to normal controls. Pain 118, 176–184 (2005).
Geisser, M. E. et al. Perception of noxious and innocuous heat stimulation among healthy women and women with fibromyalgia: association with mood, somatic focus, and catastrophizing. Pain 102, 243–250 (2003).
Gibson, S. J., Littlejohn, G. O., Gorman, M. M., Helme, R. D. & Granges, G. Altered heat pain thresholds and cerebral event-related potentials following painful CO2 laser stimulation in subjects with fibromyalgia syndrome. Pain 58, 185–193 (1994).
Kosek, E. & Hansson, P. Modulatory influence on somatosensory perception from vibration and heterotopic noxious conditioning stimulation (HNCS) in fibromyalgia patients and healthy subjects. Pain 70, 41–51 (1997).
Lautenbacher, S. & Rollman, G. B. Possible deficiencies of pain modulation in fibromyalgia. Clin. J. Pain 13, 189–196 (1997).
Petzke, F., Clauw, D. J., Ambrose, K., Khine, A. & Gracely, R. H. Increased pain sensitivity in fibromyalgia: effects of stimulus type and mode of presentation. Pain 105, 403–413 (2003).
Julien, N., Goffaux, P., Arsenault, P. & Marchand, S. Widespread pain in fibromyalgia is related to a deficit of endogenous pain inhibition. Pain 114, 295–302 (2005).
Buskila, D. & Neumann, L. Fibromyalgia syndrome (FM) and nonarticular tenderness in relatives of patients with FM. J. Rheumatol. 24, 941–944 (1997).
Fitzcharles, M. A. & Boulos, P. Inaccuracy in the diagnosis of fibromyalgia syndrome: analysis of referrals. Rheumatology (Oxford) 42, 263–267 (2003).
Choy, E. H. et al. Content and criterion validity of the preliminary core dataset for clinical trials in fibromyalgia syndrome. J. Rheumatol. 36, 2330–2334 (2009).
Mease, P. et al. Fibromyalgia syndrome. J. Rheumatol. 34, 1415–1425 (2007).
Mease, P. J. et al. Fibromyalgia syndrome. J. Rheumatol. 32, 2270–2277 (2005).
Mease, P. J. et al. The efficacy and safety of milnacipran for treatment of fibromyalgiae. A randomized, double-blind, placebo-controlled trial. J. Rheumatol. 36, 398–409 (2009).
Wolfe, F. & Michaud, K. Outcome and predictor relationships in fibromyalgia and rheumatoid arthritis: evidence concerning the continuum versus discrete disorder hypothesis. J. Rheumatol. 36, 831–836 (2009).
Toda, K. Preliminary diagnostic criteria for fibromyalgia should be partially revised: comment on the article by Wolfe et al. Arthritis Care Res. (Hoboken) 63, 308–309 (2011).
Wolfe, F. et al. Fibromyalgia criteria and severity scales for clinical and epidemiological studies: a modification of the ACR Preliminary Diagnostic Criteria for Fibromyalgia. J. Rheumatol. 38, 1113–1122 (2011).
Bennett, R. M. Fibrositis: misnomer for a common rheumatic disorder. West J. Med. 134, 405–413 (1981).
Payne, T. C. et al. Fibrositis and psychologic disturbance. Arthritis Rheum. 25, 213–217 (1982).
Campbell, S. M., Clark, S., Tindall, E. A., Forehand, M. E. & Bennett, R. M. Clinical characteristics of fibrositis I. A “blinded” controlled study of symptoms and tender points. Arthritis Rheum. 26, 817–824 (1983).
Yunus, M. B., Masi, A. T. & Aldag, J. C. Preliminary criteria for primary fibromyalgia syndrome (PFS): multivariate analysis of a consecutive series of PFS, other pain patients, and normal subjects. Clin. Exp. Rheumatol. 7, 63–69 (1989).
Wolfe, F., Cathey, M. A. & Kleinheksel, S. M. Fibrositis (Fibromyalgia) in rheumatoid arthritis. J. Rheumatol. 11:6, 814–818 (1984).
Hartz, A. & Kirchdoerfer, E. Undetected fibrositis in primary care practice. J. Fam. Pract. 25, 365–369 (1987).
Müller, W. The fibrositis syndrome: diagnosis, differential diagnosis and pathogenesis. Scand. J. Rheumatol. 65 (Suppl.) 40–53 (1987).
Greenfield, S., Fitzcharles, M. A. & Esdaile, J. M. Reactive fibromyalgia syndrome. Arthritis Rheum. 35, 678–681 (1992).
Middleton, G. D., McFarlin, J. E. & Lipsky, P. E. The prevalence and clinical impact of fibromyalgia in systemic lupus erythematosus. Arthritis Rheum. 8, 1181–1188 (1994).
Borenstein, D. Prevalence and treatment outcome of primary and secondary fibromyalgia in patients with spinal pain. Spine 20, 796–800 (1995).
Pamuk, G. E., Pamuk, O. N., Set, T., Harmandar, O. & Yesil, N. An increased prevalence of fibromyalgia in iron deficiency anemia and thalassemia minor and associated factors. Clin. Rheumatol. 27, 1103–1108 (2008).
Tietjen, G. E. et al. Allodynia in migraine: association with comorbid pain conditions. Headache 49, 1333–1344 (2009).
Bannwarth, B. et al. Fibromyalgia syndrome in the general population of France: a prevalence study. Joint Bone Spine 76, 184–187 (2009).
Almodovar, R. et al. Fibromyalgia in patients with ankylosing spondylitis: prevalence and utility of the measures of activity, function and radiological damage. Clin. Exp. Rheumatol. 28, S33–S39 (2010).
Jacobsen, S. & Danneskiold, S. Inter-relations between clinical parameters and muscle function in patients with primary fibromyalgia. Clin. Exp. Rheumatol. 7, 493–498 (1989).
Forseth, K. O. & Gran, J. T. The prevalence of fibromyalgia among women aged 20–49 years in Arendal, Norway. Scand. J. Rheumatol. 21, 74–78 (1992).
Lydell, C. & Meyers, O. L. The prevalence of fibromyalgia in a South African community [abstract]. Scand. J. Rheumatol. 94, (Suppl.) 8 (1992).
Raspe, H., Baugmanter, C. & Wolfe, F. The prevalence of fibromyalgia in a rural German community: how much difference do different criteria make? [abstract]. Arthritis Rheum. 36 (Suppl.), S48 (1993).
Prescott, E. et al. Fibromyalgia in the adult Danish population: I. A prevalence study. Scand. J. Rheumatol. 22, 233–237 (1993).
Buskila, D. et al. Assessment of nonarticular tenderness and prevalence of fibromyalgia in children. J. Rheumatol. 20, 368–370 (1993).
Clark, P., Burgos-Vargas, R., Medina-Palma, C., Lavielle, P. & Marina, F. F. Prevalence of fibromyalgia in children: a clinical study of Mexican children. J. Rheumatol. 25, 2009–2014 (1998).
White, K. P., Speechley, M., Harth, M. & Ostbye, T. The London Fibromyalgia Epidemiology Study: the prevalence of fibromyalgia syndrome in London, Ontario. J. Rheumatol. 26, 1570–1576 (1999).
Haq, S. A. et al. Prevalence of rheumatic diseases and associated outcomes in rural and urban communities in Bangladesh: a COPCORD study. J. Rheumatol. 32, 348–353 (2005).
Manahan, L. et al. Rheumatic pain in a Philippine village. A WHO–ILAR COPCORD Study. Rheumatol. Int. 5, 149–153 (1985).
Wenzel, H. G., Mykletun, A. & Nilsen, T. I. Symptom profile of persons self-reporting whiplash: a Norwegian population-based study (HUNT 2). Eur. Spine J. 18, 1363–1370 (2009).
Davatchi, F. et al. The prevalence of musculoskeletal complaints in a rural area in Iran: a WHO-ILAR COPCORD study (stage 1, rural study) in Iran. Clin. Rheumatol. 28, 1267–1274 (2009).
Santos, A. M. et al. Prevalence of fibromyalgia and chronic widespread pain in community-dwelling elderly subjects living in Sao Paulo, Brazil. Maturitas 67, 251–255 (2010).
Branco, J. C. et al. Prevalence of fibromyalgia: a survey in five European countries. Semin. Arthritis Rheum. 39, 448–453 (2010).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
McBeth, J., Mulvey, M. Fibromyalgia: mechanisms and potential impact of the ACR 2010 classification criteria. Nat Rev Rheumatol 8, 108–116 (2012). https://doi.org/10.1038/nrrheum.2011.216
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2011.216
This article is cited by
-
Structural and functional thalamocortical connectivity study in female fibromyalgia
Scientific Reports (2021)
-
Chronic generalized pain disrupts whole brain functional connectivity in mice
Brain Imaging and Behavior (2021)
-
Performance of the American College of Rheumatology 2016 criteria for fibromyalgia in a referral care setting
Rheumatology International (2019)
-
Fibromyalgia: A Critical and Comprehensive Review
Clinical Reviews in Allergy & Immunology (2015)
-
Screening und Frühdiagnostik der Psoriasisarthritis
Zeitschrift für Rheumatologie (2013)