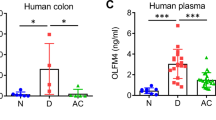
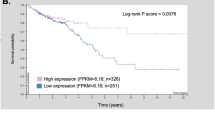
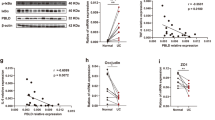
Abstract
Colon carcinogenesis is a multiple-step process involving the accumulation of a series of genetic and epigenetic alterations. The most commonly initiating event of intestinal carcinogenesis is mutation of the adenomatous polyposis coli (APC) gene, which leads to activation of the Wnt/β-catenin pathway. Olfactomedin 4 (OLFM4) has emerged as an intestinal stem-cell marker, but its biological function in the intestine remains to be determined. Here we show that Olfm4 deletion induced colon adenocarcinoma in the distal colon of ApcMin/+ mice. Mechanistically, we found that OLFM4 is a target gene of the Wnt/β-catenin pathway and can downregulate β-catenin signaling by competing with Wnt ligands for binding to Frizzled receptors, as well as by inhibition of the Akt-GSK-3β (Akt-glycogen synthase kinase-3β) pathway. We have shown that both Wnt and nuclear factor-κB (NF-κB) signaling were boosted in tumor tissues of Apc Olfm4 double-mutant mice. These data establish OLFM4 as a critical negative regulator of the Wnt/β-catenin and NF-κB pathways that inhibits colon-cancer development initiated by APC mutation. In addition, Olfm4 deletion significantly enhanced intestinal-crypt proliferation and inflammation induced by azoxymethane/dextran sodium sulfate. Thus, OLFM4 has an important role in the regulation of intestinal inflammation and tumorigenesis, and could be a potential therapeutic target for intestinal malignant tumors. Unlike the human colonic epithelium, the mouse colonic epithelium does not express OLFM4, but nevertheless, systemic OLFM4 deletion promotes colon tumorigenesis and that loss from mucosal neutrophils may have a role to play.
Similar content being viewed by others
Introduction
Colorectal cancer and colitis-associated cancer, a subtype of colorectal cancer associated with inflammatory bowel disease (IBD), are major health risks and leading causes of death. Colon carcinogenesis is generally regarded as being composed of multiple stages of sequential mutations of some oncogenes and tumor suppressors.1 The most common initiating event of colorectal carcinogenesis is mutation of the adenomatous polyposis coli (APC) gene, which leads to activation of the Wnt/β-catenin pathway.2 Identification of molecular events that regulate tumorigenesis after Apc loss is important for understanding the mechanism of colon carcinogenesis and therapeutic development. Wnt signaling via β-catenin is critically important in regulating normal crypt cell homeostasis and is dysregulated in colon carcinogenesis. Almost all colorectal cancers exhibit mutation of either APC or β-catenin, which leads to the blockade of phosphorylation by glycogen synthase kinase-3 (GSK-3), resulting in β-catenin stabilization and enhanced Wnt/β-catenin signaling.3 During the course of tumorigenesis, additional mutations (such as KRAS and TP53) are usually acquired. It has long been recognized that chronic inflammatory bowel disease increases the risk of colorectal cancer. The transcription factor nuclear factor-κB (NF-κB) has also been shown to be a key factor linking inflammation and immunity to cancer development and progression.4 A recent study showed that NF-κB could enhance Wnt signaling, leading to the dedifferentiation of epithelial non-stem cells into tumor-initiating cells.5 However, clearly defining the regulatory mechanism of Wnt signaling and its role in colon carcinogenesis continues to present a challenge.
Olfactomedin 4 (OLFM4, also known as hGC-1 and GW112) is an evolutionarily conserved glycoprotein that belongs to the olfactomedin family.6 It was first cloned in human hematopoietic myeloid cells and is also abundantly expressed in intestinal crypts.6, 7 It affects a diverse set of cellular processes, including proliferation, differentiation, apoptosis, adhesion and innate immunity against bacterial infections.8, 9, 10, 11 OLFM4 transcription is regulated by PU.1,12 NF-κB,13 Notch14 and retinoic acids.10 Its expression is also regulated epigenetically through promoter methylation.7, 12 OLFM4 expression is upregulated in human inflammatory bowel disease, which comprises ulcerative colitis and Crohn’s disease.15, 16 OLFM4 interacts with NOD1 and NOD2,17 which are intracellular sensors for bacterial infection that have been found to be associated with Crohn’s disease.18, 19 A recent study has demonstrated that OLFM4 is a robust marker for intestinal Lgr5-positive stem cells.20
OLFM4 protein tends to be overexpressed in early-stage colon cancer, but reduced or lost in advanced stages of the disease.21, 22 These observations suggest that OLFM4 may be involved in colon carcinogenesis. Here we found that Olfm4 deletion in ApcMin/+ mice leads to adenocarcinoma formation in the distal colon and upregulation of Wnt/β-catenin signaling genes. Olfm4-deficient mice exhibited robust intestinal-crypt hyperplasia and severe inflammation in an azoxymethane/dextran sodium sulfate (AOM/DSS)-induced colitis-associated cancer model. In addition, we showed that OLFM4 is a both a target gene and an inhibitor of the Wnt/β-catenin pathway.
Results
Olfm4 deletion induces more intestinal polyps and colon adenocarcinomas in ApcMin/+ mice
Despite the fact that Olfm4 deficiency alone does not affect the normal architecture or homeostasis of the mouse intestinal epithelium,17 OLFM4’s increased expression in the early stage and reduced expression in the late stage of human colon-cancer patients7 raise the hypothesis that OLFM4 may be involved in colon-cancer development. To test this possibility, we crossed Olfm4−/− mice with ApcMin/+ mice, the later of which provides a model system associated with intestinal tumorigenesis. We first analyzed the mutant mice in a mixed 129Sv/Black Swiss background. Under this genetic background, only a few polys were observed in the proximal small intestine. Loss of Olfm4 in Apc+/− Olfm4+/− and Apc+/− Olfm4−/− (Apc Olfm4 double-mutant) mice did not change the number of polyps observed in the small intestine, but the polyps that were present were larger than those observed in Apc+/− Olfm4+/+ mice (Figures 1a and c). Prominent large tumors in the distal colon were observed in ~40% of Apc+/− Olfm4+/− and Apc+/− Olfm4−/− mice at 3 months of age (Figures 1b and c). Of the 18 mice displaying these tumors, 17 had only a single tumor in the colon, located ~1 cm from the end of the distal colon. Histopathology confirmed that these tumors were all colon adenocarcinoma (Figure 1b). Most of the colon-cancer tissues (80%) were accompanied by robust inflammatory-cell infiltration (Figure 1b). Next, we examined intestinal tumorigenesis in the mutant mice with a pure C57BL6 background. We observed significantly more polyps in the small intestines of Apc Olfm4 double-mutant mice than in Apc+/− Olfm4+/+ mice (Supplementary Figure S1a). More adenocarcinomas were found in the colon of Apc Olfm4 double-mutant mice with a C57BL6 background compared in those with a 129Sv/Black Swiss background (Figure 1c and Supplementary Figures S1b and c). Further, the survival rate of Apc Olfm4 double-mutant mice was worse compared with the wild-type (WT) or Apc+/− Olfm4+/+ mice (Supplementary Figure S1d). These data demonstrate that Olfm4 deletion promotes intestinal polyp development and induces colon adenocarcinoma formation after Apc loss.
Olfm4 deletion induces large polyps in the small intestine and adenocarcinoma formation in the distal colon of Apc+/− mice. (a) Polyp formation (arrow) in the small intestine of ApcMin/+, Apc+/− Olfm4+/− and Apc+/− Olfm4−/− (Apc Olfm4 double-mutant) mice. (b) Adenocarcinoma formation in the distal colon of Apc+/− Olfm4+/− and Apc Olfm4 double-mutant mice. Three representative tumors in mice of each genotype are presented. Hematoxylin and eosin (HE) histology staining is shown below each corresponding tumor. Scale bar, 50 μm. (c) Mean (±s.d.) small intestinal polyp number and size, and colon-tumor incidence in ApcMin/+ (n=20), Apc+/− Olfm4+/− (n=23) and Apc Olfm4 double-mutant mice (n=22) mice.
Wnt/β-catenin signaling is enhanced in Apc Olfm4 double-mutant mice
To understand the molecular mechanism of colon-tumor formation, we determined whether the Wnt//β-catenin pathway, the principal driving force in colon carcinogenesis, was activated in Olfm4-deficient mice. β-Catenin was mainly localized to the edge of colon epithelial cells in WT, ApcMin/+ and Apc+/+ Olfm4−/− mice (Figures 2a–c). Intense homogeneous β-catenin staining in the cytoplasm and nucleus was found in nine out of nine (100%) tumors in Apc+/− Olfm4+/− mice (Figure 2d) and Apc+/− Olfm4−/− mice (Figure 2e). β-Catenin staining was also enhanced in aberrant crypt foci of Apc+/− Olfm4−/− mice (Figure 2g). These results suggest that deletion of Olfm4 leads to the activation of β-catenin signaling in the tumor tissues following Apc loss.
Olfm4 deletion enhances Wnt/β-catenin signaling in Apc Olfm4 double-mutant mice. (a–h) β-Catenin immunohistochemistry staining was performed in the distal colon of Apc+/+ Olfm4+/+ (WT) (a), Apc+/− Olfm4+/+ (b), Apc+/+ Olfm4−/− (c), Apc+/− Olfm4+/− (d) and Apc+/− Olfm4−/− (e and g) mice. Hematoxylin and eosin (HE) staining in (f and h) was performed in mice corresponding to (e and g), respectively. Scale bar, 50 μm. (i) A heatmap from cDNA microarray analysis shows Wnt pathway-related or target gene-expression level in the distal colon of mice with different genotypes. N, tumor-adjacent normal tissue; T, tumor. (j) Mean (±s.d.) (n=3) gene-expression levels for six representative Wnt target genes were confirmed by qRT–PCR. See also Supplementary Tables S1 and S2.
We next studied gene-transcription profiles in the distal colon using cDNA microarray analyses. Compared with WT mice, single deletion of the Apc or Olfm4 gene did not significantly change the gene-expression profiles in the distal colon. Instead, the tumor-adjacent tissues showed moderate expression change. In contrast, marked gene-expression changes were observed in the tumor tissues of Apc+/− Olfm4−/− mice compared with WT mice and adjacent normally appearing tissues (GEO number: GSE54501). Gene ontology analysis demonstrated a strong enrichment for Wnt/β-catenin pathway genes in Apc+/− Olfm4−/− (double-mutant) mice (data not shown). Out of 177 Wnt pathway-related or target genes, 32 genes were upregulated (>2-fold) in the tumor tissues compared with adjacent tissues (Figures 2i and j and Supplementary Table S1). No Wnt genes were found to be downregulated in the tumors. Among the upregulated genes, five Wnt genes (Wnt3, 5a, 6, 10 and 16) and 11 known Wnt pathway-target genes (T, Prox1, Lect2, Mmp7, Apcdd1, Sp5, Lef1, Axin2, Cd44, Wisp1 and Jun) were identified. We also identified the top 15 tumor-related genes that were markedly upregulated (>17-fold) or downregulated (>10-fold) in Apc+/− Olfm4−/− tumor tissues compared with tumor-adjacent normal tissues (Supplementary Table S2). Among these 15 upregulated genes, 8 genes were known Wnt components or target genes: Wnt10a, T (brachyury), Prox1, Wif1, Lect2, Mmp7, Sp5 and Apcdd1. Taken together, these results indicated that combined mutation of Apc and loss of Olfm4 leads to abnormally high and prolonged elevated Wnt/β-catenin signaling activity that may eventually cause distal-colon adenocarcinoma.
OLFM4 is a negative regulator of the Wnt/β-catenin pathway
The above data suggest that Olfm4 might have a role in the regulation of Wnt/β-catenin signaling. We first tested this possibility in 293T cells. Treatment of 293T cells with OLFM4 decreased β-catenin protein levels slightly in total cell lysates and more obviously in subcellular fractions, including cell membranes, cytoplasm and nucleus (Figure 3a). Pretreatment of 293T cells with OLFM4 antagonized Wnt3a-induced upregulation of β-catenin in the cytoplasm and nucleus (Figure 3b). Overexpression of OLFM4 in 293T cells also decreased endogenous β-catenin levels and antagonized Wnt3a-induced upregulation of β-catenin in the cytoplasm (Figure 3c). These observations indicate that OLFM4 can directly downregulate endogenous β-catenin level and antagonize Wnt3a-induced regulation of β-catenin.
OLFM4 decreases β-catenin levels. (a–k) Western blots were performed in 293T cells (a–i), SW480 cells (j) and freshly isolated mouse colon crypts (k) after human OLFM4 treatment (1 μg/ml) (a–j) and mouse Olfm4 treatment (1 μg/ml) (k). β-Actin, total cadherin, Hsp90 and SP1 were used as loading controls in total cell lysate, membrane, cytoplasm and nucleus cell preparations, respectively. (a) β-Catenin levels in total cell lysate, membrane, cytoplasm and nucleus at different time points of OLFM4 treatment. (b) Endogenous and Wnt3a (1 μg/ml)-induced β-catenin levels in the cytoplasm and nucleus of cells pretreated with and without OLFM4 for 30 min. (c) Endogenous and Wnt3a (1 μg/ml)-induced β-catenin levels in the cytoplasm of cells transfected with control (vector) or OLFM4 expression plasmid. (d) β-Catenin phosphorylation at different time points of OLFM4 treatment. (e and f) Akt (T308 or Ser473) phosphorylation at different time points of OLFM4 treatment. (g and h) β-Catenin levels in the cytoplasm of cells pretreated with and without either LiCl (20 mm) or MG132 (10 μm) before OLFM4 treatment for 30 min. (i) β-Catenin levels in total cell lysates of cells transfected with Flag-tagged WT or mutant (S33Y or S31/37T41S45) β-catenin expression plasmids and then treated with or without OLFM4 for 30 min. (j) Total and active β-catenin levels in the cytoplasm or nucleus of SW480 colon-cancer cells at different time points of Olfm4 treatment. (k) β-Catenin levels in the cytoplasm and nucleus of freshly isolated mouse colon crypts at different time points of Olfm4 (or PBS control buffer) treatment. (l) Olfm4 and β-catenin levels in the cytoplasm of Ls174T cells infected with lentiviral control shRNA and Olfm4 shRNA.
We next determined the phosphorylation status of β-catenin in 293T cells when treated with OLFM4. OLFM4 treatment induced β-catenin phosphorylation at multiple sites (T41/S45 and S33/37/T41; Figure 3d). We also found that OLFM4 inhibited Akt phosphorylation at T308 (Figure 3e) and S473 (Figure 3f), an event upstream of β-catenin phosphorylation. To determine whether OLFM4-induced β-catenin degradation occurs through the GSK-3β-mediated pathway, we pretreated 293T cells with LiCl, a potent GSK-3β inhibitor. LiCl treatment abrogated the β-catenin degradation induced by OLFM4 (Figure 3g). The β-catenin degradation induced by OLFM4 was also abrogated by MG132, a proteasome inhibitor (Figure 3h). These results indicate that OLFM4-induced β-catenin degradation through the GSK-3β-mediated proteasome pathway.
We further tested whether OLFM4-induced β-catenin degradation requires the presence of β-catenin phosphorylation sites. Although OLFM4 treatment decreased WT β-catenin expression levels, OLFM4 did not decrease S33Y and S31/37T41S45 mutant β-catenin expression in 293T cells (Figure 3i). This observation suggested that OLFM4 downregulation of β-catenin was dependent on β-catenin’s GSK-3β-mediated phosphorylation sites. We also determined whether OLFM4 could downregulate β-catenin in SW480 colon-cancer cells, which express truncated APC, but WT β-catenin. OLFM4 did not alter the total β-catenin levels in the cytoplasm of SW480 cells, but substantially downregulated cytoplasmic levels of active (unphosphorylated) β-catenin. In addition, OLFM4 effectively reduced the nuclear β-catenin levels in SW480 cells, indicating that OLFM4 can also downregulate β-catenin levels in at least some colon-cancer cells (Figure 3j). Further, we investigated the direct effect of Olfm4 on freshly isolated mouse colon and small intestine crypts. Mouse Olfm4 protein treatment downregulated β-catenin levels in both the cytoplasm and nucleus of colon (Figure 3k) and small intestine (Supplementary Figure S2a) crypts. However, Olfm4 protein did not affect mouse small intestinal and colon organoid differentiation (Supplementary Figures S2b and c) nor did it affect colon organoid growth and proliferation (Supplementary Figures S2d and e). Last, we also established stable Ls174T cell lines infected with control short hairpin RNA (shRNA) or Olfm4 shRNA lentivirus. Olfm4 shRNA eliminated Olfm4 expression and led to increased β-catenin levels in the cytoplasm (Figure 3l). Taken together, these data demonstrate that OLFM4 is a negative regulator of the canonical Wnt/β-catenin pathway.
OLFM4 interacts with Frizzled-7 and -10
Previous studies have shown that two other members of the olfactomedin family, mycilin and olfactomedin 1, interacted with Frizzled receptors and other Wnt pathway regulators (such as Wnt1 and WIF1) and were involved in the Wnt pathway regulation.23, 24 Accordingly, we next determined the potential association of OLFM4 with Frizzled receptors and other Wnt components. We first performed co-immunoprecipitation assays in a colon-cancer cell line, Ls174T, that expresses endogenous OLFM4. We showed that OLFM4 was co-immunoprecipitated with total Frizzled receptors in the cell lysate with and without exogenously added OLFM4 protein (Figure 4a) in Ls174T cells. We then determined the interaction between OLFM4 and each Frizzled receptor (frizzled 1, 2, 3, 4, 5, 6, 7, 8, 9 and 10). We found that OLFM4 specifically co-immunoprecipitated with Frizzled-7 and Frizzled-10 in Ls174T cells but not with other Frizzled receptors (Figure 4b). A reverse co-immunoprecipitation assay confirmed the binding of OLFM4 with Frizzled receptors (Figure 4c). Next, we investigated the association between OLFM4 and Frizzled receptors in 293T cells stably overexpressing OLFM4. A reciprocal co-immunoprecipitation experiment showed that OLFM4 was co-immunoprecipitated with total Frizzled receptors, Frizzled-7 and Frizzled-10 (Figures 4d and e). No co-immunoprecipitation of OLFM4 with Wnt1 or WIF1 was observed (data not shown).
OLFM4 interacts with Frizzled-7 and -10. (a) Ls174T cell lysate in the presence or absence of OLFM4 treatment was immunoprecipitated with OLFM4 antibody or IgG control antibody and then subjected to western blot with a total Frizzled (Fzd) receptors antibody. (b) Ls174T cell lysate was immunoprecipitated with OLFM4 antibody or IgG control antibody and then subjected to western blot with Fzd-7 or Fzd-10 antibody. (c) Ls174T cell lysate was immunoprecipitated with a total Fzd receptors antibody, Fzd-10 antibody or IgG antibody and then subjected to western blot with OLFM4 antibody. (d) Cell lysates from 293T cells stably overexpressing OLFM4 were immunoprecipitated with OLFM4 antibody or IgG control antibody and then subjected to western blot with a total Fzd receptors antibody, Fzd-7 antibody or Fzd-10 antibody. (e) Cell lysate from 293T cells stably overexpressing OLFM4 was immunoprecipitated with a total Fzd receptors antibody, Fzd-7 antibody, Fzd-10 antibody or IgG control antibody and then subjected to western blot with OLFM4 antibody. (f) Microscale thermophoresis (MST) measurements of the OLFM4 interaction with Fzd-7 (solid circles) and Fzd-10 (hollow circles). The solid lines are the best-fit curves to the data using the Hill equation (KD=2.5 μm for the OLFM4–Fzd-7 interaction and KD=10 μm for the OLFM4–Fzd-10 interaction). The error bars represent the s.d. from three independent measurements.
To further confirm and define the binding affinity of the interaction between OLFM4 and Frizzled-7 or Frizzled-10, we performed microscale thermophoresis analysis. The assay revealed the interaction between OLFM4 and Frizzled-7 (with KD=2.5 μm), as well as the interaction between OLFM4 and Frizzled-10 (with KD=10 μm) (Figure 4f). These data indicate that OLFM4 can physically interact with Frizzled-7 and Frizzled-10. The physical interaction between OLFM4 and Frizzled receptors suggests that OLFM4 may negatively regulate Wnt signaling by competing with Wnt ligands for binding to Frizzled receptors. As described above, OLFM4 can also inhibit Wnt signaling through inhibition of Akt phosphorylation and increased GSK-3β-mediated β-catenin degradation. The cooperation of the two mechanisms might be necessary to ensure more complete functional inhibition of Wnt signaling.
OLFM4 is a target gene of the Wnt/β-catenin pathway
It has previously been demonstrated that some Wnt target genes are specifically expressed in intestinal stem cells. We wanted to determine whether OLFM4 is also a Wnt target gene. Analysis of the OLFM4 promoter using the Genomatix software (Ann Arbor, MI, USA) revealed three putative LEF1/TCF (lymphoid enhancer-binding factor 1/T-cell factor)-binding sites within 1 kb upstream of the transcriptional start site (Figure 5a). Accordingly, we hypothesized that OLFM4 expression might be regulated by Wnt/β-catenin signaling. To elucidate the regulation of OLFM4 transcription, we generated luciferase reporter constructs under the control of the OLFM4 1 kb promoter with deletion of each putative LEF/TCF binding core sites individually or in combination (Figure 5b). Both endogenous and Wnt3a-elicited luciferase reporter activities were significantly compromised when each putative LEF/TCF binding core site (or sites in combination) were deleted (Figure 5b).
OLFM4 is a target gene of the Wnt/β-catenin/TCF pathway. (a) Three LEF1/TCF binding sites (in black box) located in the promoter of OLFM4. (b) The core (CAAAG or CTTTG) of the LEF1/TCF binding site was deleted individually or in combination as indicated by gray boxes. Data represent mean (±s.d.) (n=3) relative luciferase activity of corresponding reporter in the presence of Wnt3a or vehicle in 293T cells. *P<0.05 and **P<0.01 when compared with WT vehicle or WT Wnt3a, respectively, two-tailed t-test. (c) Mean (±s.d.) (n=3) OLFM4 mRNA expression determined by qRT–PCR in Ls174T cells (right) after knockdown of TCF4 expression by TCF4 lentivirus shRNA (left). *P<0.01 when compared with control (Con) shRNA, two-tailed t-test. (d) Mean (±s.d.) (n=3) OLFM4 mRNA expression determined by qRT–PCR in Ls174T and SW948 cells treated with IWP2, XAV-939 or DMSO control. *P<0.01 when compared with DMSO group, two-tailed t-test. (e) ChIP assay of LEF1 and TCF4 binding to all three LEF/TCF binding sites in the OLFM4 promoter.
We next determined whether OLFM4 expression is regulated by Wnt/β-catenin signaling pathway in two colon-cancer cell lines with endogenous OLFM4 expression. The OLFM4 expression in Ls174T cells was inhibited by TCF4 shRNA lentivirus infection but not control shRNA (Figure 5c). When we treated Ls174T and SW948 cell lines with two Wnt pathway inhibitors, IWP2 (which inhibits Wnt processing and secretion) and XAV-939 (which stabilizes axin and degrades β-catenin), both inhibitors significantly inhibited OLFM4 transcription (Figure 5d). Finally, we examined whether LEF1 or TCF4 physically interacts with the three potential LEF/TCF binding sites in Ls174T cells using chromatin immunoprecipitation (ChIP) assays. The ChIP assays demonstrated that both LEF1 and TCF4 bind to all three LEF/TCF binding sites (Figure 5e). Taken together, these results indicate that OLFM4 is a target gene of the Wnt/β-catenin/TCF pathway, similar to other intestinal stem-cell markers, such as Lgr5.
NF-κB signaling is enhanced in Apc Olfm4 double-mutant mice
Robust inflammatory-cell (neutrophils, F4/80+ macrophages and CD3+ lymphocytes) infiltrations were observed in the surrounding tissues of colon tumors in Apc Olfm4 double-mutant mice (Supplementary Figure S3a), indicating an inflammation-inhibitory role of Olfm4 in this carcinogenesis process. IkB kinase (IKK) activity assays showed that IKK activity in the tumor tissues of Apc+/− Olfm4−/− mice was significantly higher compared with that in WT, ApcMin/+ and Olfm4−/− mice (Supplementary Figure S3b).
cDNA microarray analysis revealed that many proinflammatory cytokines and chemokines that are important for intestinal carcinogenesis were upregulated in the tumors of Apc+/− Olfm4−/− mice compared with tumor-adjacent normal tissues and WT mice (Supplementary Figures S3c and d and Supplementary Table S3). These cytokines include the NF-κB-regulated genes Tnf, Il-1β and Il-6, which are well known to be implicated in intestinal inflammation and carcinogenesis.25, 26, 27 We also observed a strong upregulation of genes encoding proteins chemotactic for neutrophils, including Cxcl1, Cxcl2, Cxcl3 and Cxcl5. Cxcl1 and Cxcl2 (GRO-α and -β) are regulated by NF-κB and have been implicated in tumor growth and metastasis.28 These results suggested that NF-κB activities were upregulated in Apc Olfm4 double-mutant mice. The presence of enhanced cytokines and chemokines and inflammatory cells in the tumor microenvironment is likely to contribute to colon-tumor formation and growth in the Apc Olfm4 double-mutant mice.
Olfm4 deletion leads to intestinal-crypt hyperplasia, inflammation and mucosa damage in a colitis-associated cancer model
To investigate whether Olfm4 regulates intestinal inflammation and tumorigenesis in Apc-independent murine colorectal-cancer models, we examined the effect of Olfm4 deletion in an AOM/DSS-induced colitis-associated cancer model. After an AOM initial injection, mice were treated with DSS and water for four cycles until we observed symptoms of intestinal burden (Figure 6a). Olfm4−/− mice demonstrated significant weight loss compared with WT mice (Figure 6b). After four DSS and water treatment cycles, all WT mice survived, but only six out of 10 Olfm4−/− mice survived (Figure 6c). The colons in Olfm4−/− mice were significantly shorter than those in WT mice (Figure 6d). The jejunum and ileum in Olfm4−/− mice demonstrated robust inflammation and intestinal-crypt hyperplasia, whereas WT mice showed normal structure with no substantial inflammation (Figures 6e and f). Similarly, colons in Olfm4−/− mice demonstrated severe inflammation and mucosa damage, while only mild to moderate inflammation was observed in WT mice (Figures 6e and f). No tumor formation was observed in the mice studied. These data indicate that Olfm4 is an inhibitor of intestinal inflammation and crypt proliferation induced by AOM/DSS.
Olfm4 deletion results in intestinal-crypt hyperplasia and severe inflammation after AOM/DSS treatment. (a) Schematic of AOM/DSS-induced colitis-associated cancer model. Mice were injected intraperitoneally with AOM (10 mg/kg). After 5 days, mice were treated with 2.5% DSS in their drinking water for 5 days followed by regular water for 16 days. The cycle was repeated four times. (b) WT (n=8) and Olfm4−/− (n=8) mice were weighed after four cycles of DSS and water treatment. *P<0.01, two-tailed t-test. (c) Percentage of survival of WT (n=10) and Olfm4−/− (n=10) mice after four cycles of DSS and water treatment. (d) Length of colon in WT (n=5) and Olfm4−/− (n=5) mice after four cycles of DSS and water treatment. *P<0.01, two-tailed t-test. (e) Mean (±s.d.) histology score of inflammation and tissue damage in the jejunum, ileum and colon of WT (n=8) and Olfm4−/− (n=8) mice after four cycles of DSS and water treatment. *P<0.01 when compared with WT corresponding tissues, two-tailed t-test. (f) HE staining of jejunum, ileum and colon of WT and Olfm4−/− mice after four cycles of DSS and water treatment. Scale bar, 50 μm. The image represents at least five mice in each group.
Discussion
To investigate the role of OLFM4 in intestinal tumorigenesis, we characterized the effect of Olfm4 loss under two circumstances: in the context of activated Wnt signaling, achieved by deletion of Olfm4 in the ApcMin/+mice, and AOM/DSS-induced intestinal inflammation and tumorigenesis. Our data directly implicate Olfm4 in murine colon carcinoma development and indicate that Olfm4 has an inhibitory role in intestinal inflammation and crypt proliferation under certain inflammatory stimuli.
This study reveals a connection between Olfm4 and the Wnt pathway in colon carcinogenesis. Deletion of Olfm4 alone did not initiate Wnt signals in the mouse colon, but potently enhanced such signals after APC mutation. This finding indicates that Olfm4 can synergize with Apc as a negative regulator of the Wnt/β-catenin pathway. The upregulated Wnt/β-catenin pathway-target genes in Apc+/− Olfm4−/− mice may eventually contribute to the colon-tumor formation. For example, Prox1 (31.8-fold), Apcdd1 (62.0-fold) and Trop2 (243.5-fold) gene expression were found to be markedly increased in distal-colon tumors compared with WT tissues. These genes have been associated with colon-cancer growth, aggressiveness and metastasis.28, 29, 30, 31 Five Wnt genes (Wnt3, 5a, 6, 10 and 16) and 11 Wnt pathway-target genes were upregulated, whereas no Wnt genes were found to be downregulated in the tumors. All these gene-expression data point to a remarkably elevated Wnt/β-catenin pathway signaling that may contribute to distal-colon-tumor formation in Apc Olfm4 double-mutant mice.
Our data indicate that Olfm4 is both a target gene of the Wnt pathway and an antagonist of the Wnt pathway (Supplementary Figure S4). Similar to other intestinal stem-cell markers (such as Lgr5), here we have demonstrated that Olfm4 is a target gene of the Wnt/β-catenin pathway. We have previously shown that Olfm4 is also a target gene of the NF-κB pathway.13 Therefore, Olfm4 is a common target gene of both the Wnt and NF-κB pathways in the intestinal stem cells. Olfm4 may require both pathways for its full transcriptional activation after Apc loss. OLFM4 may inhibit Wnt signaling through two possible molecular mechanisms: inhibiting the phosphorylation of Akt and increasing GSK-3β-mediated β-catenin degradation; or competing with Wnt ligands for binding to Frizzled receptors at the cell surface. OLFM4 could act by a dominant-negative mechanism, interacting with the Frizzled receptors and forming non-functional complexes that are incapable of transmitting the Wnt signal. The cooperation of the two mechanisms might be necessary to ensure more complete functional inhibition of Wnt signaling. There are other naturally occurring secreted Wnt antagonists. For example, Frizzled-related protein (FRP) and Wnt inhibitory protein (WIF) bind Wnts, thereby inhibiting interaction between Wnt and Wnt receptors.29, 30 In addition, the Dickkopf-131 and WISE/SOST families antagonize Wnt signaling by binding LRP5/6.32 Therefore, these naturally secreted Wnt inhibitors can act in various ways to inhibit Wnt signals.
Regulation of the Wnt pathway by two other members of olfactomedin family has previously been reported. Olfactomedin 1 in zebrafish regulates retinal axon elongation in vivo and modulates the Wnt signaling pathway by physically interacting with WIF1 and reducing WIF1’s inhibitory Wnt canonical pathway.24 Myocilin modulates Wnt signaling by interacting with Frizzled receptors and FRPs and may perform redundant functions as Wnt proteins in the mammalian eye.23 These observations, together with our study, suggest that olfactomedin family proteins are actively involved in the regulation of the Wnt pathway and may have various effects in different tissues.
Activation of the Wnt/β-catenin pathway is widely associated with oncogenesis; therefore, negative inhibitory mechanisms are critical for tumor suppression and blockade of proliferation in normal tissues. APC and axin negatively regulate β-catenin levels, and both are tumor-suppressor genes that are mutated in colon and hepatocellular cancers.33, 34 A recent human colon-cancer whole-genome sequencing project (Cancer Genome Atlas Network)35 revealed two OLFM4 genomic mutations: G396T (K132N) at exon 3 and G1346A (R449K) at exon 5. The functional implications of these two mutations still remain to be determined. Previous studies have shown that OLFM4 protein expression has been reduced or lost in a portion of human colon cancers, with loss being more prevalent in advanced-stage cancer.21, 35 Based on our observations in these mouse model studies, the loss of OLFM4 protein expression may be critical for colon-cancer progression in humans. These data suggest that OLFM4 may serve as a critical roadblock to colon-cancer progression after APC mutation.
Interaction and cross-regulation between the NF-κB and Wnt signaling pathways have been proposed in previous studies.5, 36 Constitutive IKK2 activation in intestinal epithelial cells has been shown to induce NF-κB activation and simultaneously activate the Wnt/β-catenin pathway.37 Secreting cytokines such as (tumor necrosis factor and interleukin-1β (IL-1β)) have been found to activate the Wnt/β-catenin signaling by inducing GSK-3β phosphorylation.38, 39 Further, it has been shown that β-catenin activation in tumors is not controlled solely by Wnt ligands or mutations activating Wnt signaling, but that additional Wnt-independent cues from the microenvironment are also required for full activation of β-catenin signaling.40 Here we show that Olfm4 is an inhibitor of both the Wnt and NF-κB pathways after Wnt signal initiation. In addition, Olfm4 deletion significantly enhanced intestinal-crypt proliferation and inflammation induced by AOM/DSS. These observations establish Olfm4 as a key regulator of intestinal inflammation and tumor formation in both the presence and absence of Apc. In our study, the activation of the NF-κB pathway and presence of inflammation in the microenvironment may have an important role in distal-colon carcinoma formation.
Our results showed that the NF-κB pathway, the master controller of cancer-related inflammation, and some of the primary inflammatory cytokines (such as tumor necrosis factor, IL-1β, IL-6 and IL-23) were significantly upregulated in the tumors of Apc Olfm4 double-mutant mice, supporting an NF-κB- and inflammation-inhibitory role of Olfm4 in distal-colon tumors. Tumor necrosis factor, IL-1β and IL-6 in the tumor microenvironment have long been known to promote tumor growth and metastasis.41 It has also been reported that the NF-κB/IL-6/Stat3 cascade has a key role in intestinal carcinogenesis.26 Our observation that both the Wnt and NF-κB pathways were significantly upregulated in Apc Olfm4 double-mutant mice suggests that both pathways may synergize to drive intestinal carcinogenesis. Given that both Wnt and NF-κB pathway activation account for increased transcription of several hundred genes, the observed colon-tumor formation is likely to be due to coordination of many genes that are important for tumor growth and promotion. Nevertheless, our results show that deletion of Olfm4 in the context of APC mutation can lead to adenocarcinoma formation in the murine distal colon. Olfm4 thus may have an important role linking inflammation and colon carcinogenesis. Given that it is a regulator of both the Wnt and NF-κB pathways, targeting OLFM4 may be of therapeutic benefit in colon-cancer patients.
Although OLFM4 is expressed in human colon, Olfm4 mRNA was not detected in mouse colon.20 Therefore, its potential tumor-inhibitory effect in the murine distal colon after Apc loss might be from non-epithelial cells. OLFM4 protein exists in the granules of mature neutrophils while its mRNA expression shuts down.20 It is possible that Olfm4 has its role in colon stromal myeloid cells or as a secreted protein in blood plasma. To this end, we performed immunohistochemistry analysis in mouse small intestine and colon tissue. Although Olfm4 was expressed at the bottom of small intestine crypts (in the niche where stem cells reside), in the colon mucosa it was only expressed in the stromal neutrophils and not in the colon epithelium (Supplementary Figure S5).
In summary, we have demonstrated that OLFM4 is a Wnt antagonist and an important negative regulator of the Wnt and NF-κB pathways in the APC-mutated intestine. OLFM4 may have a critical role in impeding colon-cancer development and may therefore prove to be a potential therapeutic target for preventing intestinal malignant tumor formation.
Materials and methods
Mice
Olfm4-deficient mice were generated as described on a mixed genetic background of 129Sv/Black Swiss.17 Backcrossing over six generations created Olfm4-deficient mice with a C57BL6 background. ApcMin/+ mice on a C57BL/6 background were purchased from Jackson Laboratory (Bar Harbor, ME, USA). Male and female Olfm4+/− and ApcMin/+ mice were crossed to generate Apc Olfm4 double-mutant mice and controls. The mice with the same genotypes were randomly chosen for the experimental groups. Mice used were 10- to 12-weeks-old male mice. The animals were maintained in a pathogen-free facility of the National Institutes of Health (Bethesda, MD, USA). The Animal Care and Use Committee of the National Heart, Lung and Blood Institute approved the experiments.
Cells, plasmids and reagents
Human embryonic kidney 293T cells and human colon-cancer cell lines (SW480, SW948 and Ls174T) were purchased from the American Type Culture Collection (Manassas, VA, USA). The 293T cells were grown in Dulbecco's modified Eagle's medium, and colon-cancer cell lines were grown in RPMI-1640 medium and maintained as described previously.17 OLFM4 expression plasmid was described previously.11 β-Catenin and mutant β-catenin (S33Y and S31/37T41S45) expression plasmids were acquired from Addgene (Cambridge, MA, USA). XAV-939, IWP2, LiCl, MG132 and AOM were purchased from Sigma (St Louis, MO, USA). DSS (MW 36 000–50 000) was purchased from MP Biomedicals, LLC (Santa Ana, CA, USA). Human OLFM4 protein was purchased from Sino Biological Inc. (Beijing, China). Mouse Olfm4 protein was custom-made by Creative Biomart (New York, NY, USA). OLFM4 antibody was purchased from Sino Biological Inc. or Abcam (Cambridge, MA, USA). Wnt3a was purchased from R&D Systems (Minneapolis, MN, USA).
qRT–PCR, western blot and co-immunoprecipitation assays
Quantitative real-time–PCR (RT–PCR), western blot and co-immunoprecipitation assays were performed as described previously.17 Primer and probe sets for qRT–PCR were purchased from Life Technologies (Grand Island, NY, USA). Subcellular fractionation was performed using a kit purchased from Thermo Scientific (Waltham, MA, USA) according to the manufacturer’s instructions.
Histopathology and immunohistochemistry
Intestines were washed, fixed in 10% buffered formaldehyde and embedded in paraffin. Tissue sections were stained with hematoxylin and eosin (HE). Immunohistochemistry was performed using the Envision Dual Link System-HRP (DAB+) Kit from Dako (Carpinteria, CA, USA). The sections were stained for macrophages with F4/80 antibody and lymphocytes with CD3 antibody as described previously.7 In AOM/DSS-treated mice, histology was scored as a combination of inflammatory-cell infiltration (scores 0–3) and tissue damage (scores 0–3) as described previously.42 The pictures were taken with an Olympus microscope BX51 (Center Valley, VA, USA).
Mouse intestinal-crypt isolation and organoid culture
Mouse intestinal-crypt isolation and organoid culture were performed using the IntestiCult system from STEMCELL Technologies Inc. (Vancouver, BC, Canada). Growth percentage of crypts was determined by calculating the number of organoids growing on day 3 as a fraction of the total number of crypts that had begun to form an epithelium ~4 h after plating.
Microarray analysis
Total RNA was purified using the RNeasy Plus Mini Kit from Qiagen (Germantown, MD, USA). cDNA microarray analyses were performed by the National Institute of Diabetes and Digestive and Kidney Diseases Core Facility at the National Institutes of Health using Affymetrix Mouse Genome 430 2.0 Array GeneChips (Affymetrix; Santa Clara, CA, USA). Five individual mice were used for each genotype category. The microarray signals were analyzed using the Affymetrix RMA algorithm. The analysis of variance results, false discovery rate reports and heatmaps were generated using Partek Genomic software 6.5 (Partek, St Charles, MO, USA). Enrichment analyses of gene ontology categories, which include disease markers, as well as biological process and pathway analyses, were performed using MetaCore web-access software (http://www.genego.com). The GEO submission number for the microarray data discussed in this publication is GSE54501. The GEO database is available at http://www.ncbi.nlm.nih.gov/geo/info/linking.html.
Luciferase activity assay
The OLFM4-Luc reporter was created as described previously.10 Deletion of LEF1/TCF4 binding sites in the promoter of the OLFM4 gene was performed using the QuickChange Lightning Site-Directed Mutagenesis Kit from Stratagene (La Jolla, CA, USA). Luciferase activities were measured with the Dual-Luciferase Reporter Assay system from Promega (Madison, WI, USA) according to the manufacturer’s instructions.
RNA interference
Lentiviral shRNA against TCF4, Olfm4 and control shRNA were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA) and transduced into cells according to the manufacturer’s instructions.
IKK activity assay
IKK activity was analyzed with the IkB STAR ELISA Kit from Millipore (Billerica, MA, USA) according to the manufacturer’s instructions, except that anti-IkB antibody was replaced with anti-phospho-IkB-a (Ser32) antibody from Cell Signaling Technology (Danvers, MA, USA).
ChIP assay
EZ-Magna ChIP G Kit and ChIP Ab TCF4 and LEF1 were purchased from Millipore. ChIP assays were performed according to the manufacturer’s instructions.
Statistical analysis
Data are represented as mean±s.d. All experiments were performed in at least triplicate. Differences were analyzed by Student’s t-test or analysis of variance using GraphPad Software (version 5.0d, La Jolla, CA, USA). Kaplan–Meier curves were generated with GraphPad Prism 5.0 and analyzed using the log-rank method. P<0.05 was considered statistically significant.
References
Fearon ER . Molecular genetics of colorectal cancer. Annu Rev Pathol 2011; 6: 479–507.
Bienz M, Clevers H . Linking colorectal cancer to Wnt signaling. Cell 2000; 103: 311–320.
Inomata M, Ochiai A, Akimoto S, Kitano S, Hirohashi S . Alteration of beta- catenin expression in colonic epithelial cells of familial adenomatous polyposis patients. Cancer Res 1996; 56: 2213–2217.
Karin M, Greten FR . NF-kappaB: linking inflammation and immunity to cancer development and progression. Nat Rev Immunol 2005; 5: 749–759.
Schwitalla S, Fingerle AA, Cammareri P, Nebelsiek T, Goktuna SI, Ziegler PK et al. Intestinal tumorigenesis initiated by dedifferentiation and acquisition of stem-cell-like properties. Cell 2013; 152: 25–38.
Zhang J, Liu WL, Tang DC, Chen L, Wang M, Pack SD et al. Identification and characterization of a novel member of olfactomedin-related protein family, hGC-1, expressed during myeloid lineage development. Gene 2002; 283: 83–93.
Liu W, Liu Y, Zhu J, Wright E, Ding I, Rodgers GP . Reduced hGC-1 protein expression is associated with malignant progression of colon carcinoma. Clin Cancer Res 2008; 14: 1041–1049.
Liu W, Yan M, Liu Y, McLeish KR, Coleman WG Jr, Rodgers GP . Olfactomedin 4 inhibits cathepsin C-mediated protease activities, thereby modulating neutrophil killing of Staphylococcus aureus and Escherichia coli in mice. J Immunol 2012; 189: 2460–2467.
Liu W, Yan M, Sugui JA, Li H, Xu C, Joo J et al. Olfm4 deletion enhances defense against Staphylococcus aureus in chronic granulomatous disease. J Clin Invest 2013; 123: 3751–3755.
Liu W, Lee HW, Liu Y, Wang R, Rodgers GP . Olfactomedin 4 is a novel target gene of retinoic acids and 5-aza-2'-deoxycytidine involved in human myeloid leukemia cell growth, differentiation, and apoptosis. Blood 2010; 116: 4938–4947.
Liu W, Chen L, Zhu J, Rodgers GP . The glycoprotein hGC-1 binds to cadherin and lectins. Exp Cell Res 2006; 312: 1785–1797.
Rosenbauer F, Wagner K, Zhang P, Knobeloch KP, Iwama A, Tenen DG . pDP4, a novel glycoprotein secreted by mature granulocytes, is regulated by transcription factor PU.1. Blood 2004; 103: 4294–4301.
Chin KL, Aerbajinai W, Zhu J, Drew L, Chen L, Liu W et al. The regulation of OLFM4 expression in myeloid precursor cells relies on NF-kappaB transcription factor. Br J Haematol 2008; 143: 421–432.
VanDussen KL, Carulli AJ, Keeley TM, Patel SR, Puthoff BJ, Magness ST et al. Notch signaling modulates proliferation and differentiation of intestinal crypt base columnar stem cells. Development 2012; 139: 488–497.
Gersemann M, Becker S, Nuding S, Antoni L, Ott G, Fritz P et al. Olfactomedin-4 is a glycoprotein secreted into mucus in active IBD. J Crohns Colitis 2012; 6: 425–434.
Shinozaki S, Nakamura T, Iimura M, Kato Y, Iizuka B, Kobayashi M et al. Upregulation of Reg 1alpha and GW112 in the epithelium of inflamed colonic mucosa. Gut 2001; 48: 623–629.
Liu W, Yan M, Liu Y, Wang R, Li C, Deng C et al. Olfactomedin 4 down-regulates innate immunity against Helicobacter pylori infection. Proc Natl Acad Sci USA 2010; 107: 11056–11061.
Hugot JP, Chamaillard M, Zouali H, Lesage S, Cezard JP, Belaiche J et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn's disease. Nature 2001; 411: 599–603.
Ogura Y, Bonen DK, Inohara N, Nicolae DL, Chen FF, Ramos R et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature 2001; 411: 603–606.
van der Flier LG, Haegebarth A, Stange DE, van de Wetering M, Clevers H . OLFM4 is a robust marker for stem cells in human intestine and marks a subset of colorectal cancer cells. Gastroenterology 2009; 137: 15–17.
Besson D, Pavageau AH, Valo I, Bourreau A, Belanger A, Eymerit-Morin C et al. A quantitative proteomic approach of the different stages of colorectal cancer establishes OLFM4 as a new nonmetastatic tumor marker. Mol Cell Proteomics 2011; 10: 009712.
Seko N, Oue N, Noguchi T, Sentani K, Sakamoto N, Hinoi T et al. Olfactomedin 4 (GW112, hGC-1) is an independent prognostic marker for survival in patients with colorectal cancer. Exp Ther Med 2010; 1: 73–78.
Kwon HS, Lee HS, Ji Y, Rubin JS, Tomarev SI . Myocilin is a modulator of Wnt signaling. Mol Cell Biol 2009; 29: 2139–2154.
Nakaya N, Lee HS, Takada Y, Tzchori I, Tomarev SI . Zebrafish olfactomedin 1 regulates retinal axon elongation in vivo and is a modulator of Wnt signaling pathway. J Neurosci 2008; 28: 7900–7910.
Dinarello CA . Why not treat human cancer with interleukin-1 blockade? Cancer Metastasis Rev 2010; 29: 317–329.
Grivennikov S, Karin E, Terzic J, Mucida D, Yu GY, Vallabhapurapu S et al. IL-6 and Stat3 are required for survival of intestinal epithelial cells and development of colitis-associated cancer. Cancer Cell 2009; 15: 103–113.
Popivanova BK, Kitamura K, Wu Y, Kondo T, Kagaya T, Kaneko S et al. Blocking TNF-alpha in mice reduces colorectal carcinogenesis associated with chronic colitis. J Clin Invest 2008; 118: 560–570.
Kavandi L, Collier MA, Nguyen H, Syed V . Progesterone and calcitriol attenuate inflammatory cytokines CXCL1 and CXCL2 in ovarian and endometrial cancer cells. J Cell Biochem 2012; 113: 3143–3152.
Bafico A, Gazit A, Pramila T, Finch PW, Yaniv A, Aaronson SA . Interaction of frizzled related protein (FRP) with Wnt ligands and the frizzled receptor suggests alternative mechanisms for FRP inhibition of Wnt signaling. J Biol Chem 1999; 274: 16180–16187.
Bovolenta P, Esteve P, Ruiz JM, Cisneros E, Lopez-Rios J . Beyond Wnt inhibition: new functions of secreted Frizzled-related proteins in development and disease. J Cell Sci 2008; 121: 737–746.
Glinka A, Wu W, Delius H, Monaghan AP, Blumenstock C, Niehrs C . Dickkopf-1 is a member of a new family of secreted proteins and functions in head induction. Nature 1998; 391: 357–362.
Clevers H, Nusse R . Wnt/beta-catenin signaling and disease. Cell 2012; 149: 1192–1205.
Korinek V, Barker N, Morin PJ, van Wichen D, de Weger R, Kinzler KW et al. Constitutive transcriptional activation by a beta-catenin–Tcf complex in APC−/− colon carcinoma. Science 1997; 275: 1784–1787.
Morin PJ, Sparks AB, Korinek V, Barker N, Clevers H, Vogelstein B et al. Activation of beta-catenin-Tcf signaling in colon cancer by mutations in beta-catenin or APC. Science 1997; 275: 1787–1790.
Cancer Genome Atlas Network. Comprehensive molecular characterization of human colon and rectal cancer. Nature 2012; 487: 330–337.
Deng J, Miller SA, Wang HY, Xia W, Wen Y, Zhou BP et al. Beta-catenin interacts with and inhibits NF-kappa B in human colon and breast cancer. Cancer Cell 2002; 2: 323–334.
Vlantis K, Wullaert A, Sasaki Y, Schmidt-Supprian M, Rajewsky K, Roskams T et al. Constitutive IKK2 activation in intestinal epithelial cells induces intestinal tumors in mice. J Clin Invest 2011; 121: 2781–2793.
Kaler P, Godasi BN, Augenlicht L, Klampfer L . The NF-kappaB/AKT-dependent induction of Wnt signaling in colon cancer cells by macrophages and IL-1beta. Cancer Microenviron 2009; 21: 69–80.
Oguma K, Oshima H, Aoki M, Uchio R, Naka K, Nakamura S et al. Activated macrophages promote Wnt signalling through tumour necrosis factor-alpha in gastric tumour cells. EMBO J 2008; 27: 1671–1681.
Brabletz T, Jung A, Reu S, Porzner M, Hlubek F, Kunz-Schughart LA et al. Variable beta-catenin expression in colorectal cancers indicates tumor progression driven by the tumor environment. Proc Natl Acad Sci USA 2001; 98: 10356–10361.
Mantovani A, Allavena P, Sica A, Balkwill F . Cancer-related inflammation. Nature 2008; 454: 436–444.
Zaki MH, Boyd KL, Vogel P, Kastan MB, Lamkanfi M, Kanneganti TD . The NLRP3 inflammasome protects against loss of epithelial integrity and mortality during experimental colitis. Immunity 2010; 32: 379–391.
Acknowledgements
We thank Dr Michael A Eckhaus, National Institutes of Health, for the pathology assistance and Dr Ivan Ding, National Institutes of Health, for helpful suggestions and review of our manuscript. This study was supported by the intramural research fund of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Liu, W., Li, H., Hong, SH. et al. Olfactomedin 4 deletion induces colon adenocarcinoma in ApcMin/+ mice. Oncogene 35, 5237–5247 (2016). https://doi.org/10.1038/onc.2016.58
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2016.58
This article is cited by
-
Crosstalk between colorectal CSCs and immune cells in tumorigenesis, and strategies for targeting colorectal CSCs
Experimental Hematology & Oncology (2024)
-
Olfactomedin 4 produces dysplasia but suppresses metastasis of colon cancer
Cancer Gene Therapy (2023)
-
Characterization of olfactomedin 4+ cells in prostate and urethral-tube epithelium during murine postnatal development and in adult mice
Scientific Reports (2023)
-
Increased expression of OLFM4 and lysozyme during necrotizing enterocolitis in neonates: an observational research study
BMC Pediatrics (2022)
-
Intestinal epithelial cell metabolism at the interface of microbial dysbiosis and tissue injury
Mucosal Immunology (2022)