Abstract
Mucopolysaccharidosis (MPS) is a group of inherited conditions involving metabolic dysfunction. Lysosomal enzyme deficiency leads to the accumulation of glycosaminoglycan (GAG) resulting in systemic symptoms, and is categorized into seven types caused by deficiency in one of eleven different enzymes. The pathophysiological mechanism of these diseases has been investigated, indicating impaired autophagy in neuronal damage initiation, association of activated microglia and astrocytes with the neuroinflammatory processes, and involvement of tauopathy. A new inherited error of metabolism resulting in a multisystem disorder with features of the MPS was also identified. Additionally, new therapeutic methods are being developed that could improve conventional therapies, such as new recombinant enzymes that can penetrate the blood brain barrier, hematopoietic stem cell transplantation with reduced intensity conditioning, gene therapy using a viral vector system or gene editing, and substrate reduction therapy. In this review, we discuss the recent developments in MPS research and provide a framework for developing strategies.
Similar content being viewed by others
Introduction
MPS is a group of lysosomal storage diseases (LSDs) arising from deficiencies in enzymatic glycosaminoglycan (GAG) catabolism, and can be classified into seven main diseases [1], which are caused by deficiencies in one of eleven different enzymes, including MPS I (Hurler, Hurler–Scheie, Scheie syndrome), MPS II (Hunter syndrome), MPS III (Sanfilippo syndrome), MPS IV (Morquio syndrome), MPS VI (Maroteaux-Lamy syndrome), MPS VII (Sly syndrome), and MPS IX (Natowicz syndrome, Hyaluronidase deficiency) (Table 1) [2, 3]. The frequency and birth prevalence of disease phenotype varies depending on race (Fig. 1) [4].
Prevalence of MPS (/100,000 live birth/year). MPS type I is prevalent in Caucasian populations (especially in Norway), but type II is prevalent in eastern Asian (especially in Taiwan and Japan). The combined prevalence of MPS tends to be higher in Norway, Australia and Netherlands etc. Modified from ref. [4]
Enzyme deficiency leads to the progressive accumulation of GAGs such as heparan sulfate (HS), dermatan sulfate (DS), and chondroitin sulfate (CS) in lysosomes in various cell types. This is followed by the secondary accumulation of GM2 and GM3 gangliosides in the central nervous system (CNS) [5,6,7,8,9].
Depending on the enzyme deficiency, the catabolism of different GAGs is blocked either singly or in combination. The accumulation of undegraded GAG affects the functions of various tissues and organs. Patients with MPS are typically clinically characterized by coarse facial features, skeletal abnormalities (dysostosis multiplex), hepatosplenomegaly, frequent infections such as otitis media or sinusitis, thick skin, respiratory problems, cardiac involvement, mental retardation, and reduced life expectancy. Expression patterns for these symptoms vary depending on the type of MPS, as shown in Table 1. Obstructive airway disease, respiratory or systemic infection, and cardiac complications are the usual causes of death that commonly occur in the late teens or early adulthood. MPS diagnosis depends on the detection of urinary GAG and deficiencies in specific lysosomal enzymes.
Pathophysiology
Impaired autophagy and the role of microglia in MPS
In MPS, cardiac, skeletal, and CNS abnormalities are the most prominent symptoms. Cardiac valvular disease, obstructive airway disease, or dysostosis multiplexing are thought to be the direct result of GAG accumulation as occupying lesions, but the mechanism of CNS symptoms remains unclear. Lysosomes are likely to involve immune substances and be associated with immune events, including autophagy [9, 10], antigen processing and presentation on MHC [11], lysosomal degranulation [12], and mast cell inflammatory mediator secretion [13]. However, how lysosomal GAG accumulation affects innate and adaptive immune cells remains unclear.
There are studies on impaired autophagy as an initiator of neuronal damage, as lysosome storage in MPS may suppress the fusion of autophagosomes with the lysosome. Suppressed fusion results in cellular death due to the accumulation of autophagosomes including toxic proteins or dysfunctional mitochondria [14,15,16]. Suppressed and impaired autophagy in MPS would likely provide cellular stress, damage, and death. Normal autophagy is considered one of the most essential mechanisms of neuronal death in MPS, because cells in apoptosis are not responded, but damaged, stressed or necrotic cells are responded aggressively by the immune system [17,18,19]. Conserved pattern recognition receptors (PRR) as toll-like receptors (TLRs) on immune cells recognize cellular injury or invading pathogen via the expression of damage-associated molecular patterns (DAMPs) [20, 21]. GAG accumulation activates microglial cells through Tool like receptor 4 (TLR4) and triggers neuro-inflammation, and TLR4 signaling play some important roles in MPS bone and joint disease.
Additionally, in the brain, mononuclear cells such as microglia survey for injury within the CNS and are incorporated in a range of homeostatic processes as phagocytosis, antigen presentation, and neuronal regeneration. These homeostatic processes are reported to play some important roles in MPS-associated neuroinflammation [8, 22, 23].
The extent of microglial cellular phenotype in the pathogenesis of MPS has yet to be elucidated. Wilkinson et al. reported that activated microglia and astrocytes are associated with the neuroinflammatory processes in MPS [8]. They reported increased activated astrocytes and microglial cells in the cortex and spinal cord of mice with MPS I, IIIA, IIIB, or GM2 gangliosidosis, which coincide with an increase in the levels of transcripts associated with macrophage migration and activation [24]. And GAG mediated stimulation of microglial cells through TLRs provides an alternative pathway of immune activation in MPS [25, 26].
Bone and cartilage abnormalities in MPS are also critical. Prenatal lysosomal GAG storage in chondrocytes has been reported in MPS patients and animal models. In human, fetuses aged 18-30 weeks gestation (MPS I, II, III, and IVA) have storage vacuoles in chondrocytes [27, 28]. Tomatsu et al. reported the knee joint of MPSVII mice showed lysosomal storage within the articular cartilage at birth, and the growth plate region in 1–2 days old MPSVII mice already has ballooned vacuolated chondrocytes in the resting and proliferative area [29]. Regarding the pathophysiology, Simmonaro et al. reported MPS VII model mice that were also deficient in TLR4 had improvements in bone length and a reduction in synovial tumor necrosis factor (TNF) RNA levels, although they did not assess the effect on degenerative change in the bones [30]. Xing et al. reported that TLR4 and Component 3 deficiency fail to ameliorate skeletal abnormalities in MPS VII model mouse [31]. And they also showed retroviral vector mediated neonatal gene therapy improved bone length without effect on manifestation of degenerative joint diseases as dysplasia, bone irregularities, and osteophyte formation. Recently, FGF signaling degeneration was reported to be associated with early developmental skeletal defects in MPS II model, suggesting a new venue to discover possible druggable novel key targets in MPSII [32].
Tauopathy in MPS
We reported an autopsy case of a female with Hurler-Scheie syndrome treated with long-term enzyme replacement therapy (ERT), where we detected subunit c mitochondrial ATP synthase (SCMAS) accumulation and mild tauopathy (hyperphosphorylated tau or p-tau and accumulation of both 3-repeat and 4-repeat tau) in the same area of the brain [33, 34]. We detected the expression of phosphorylated tau, 3-repeat isoform RD4, 4-repeat isoform RD3, and Alzheimer precursor protein A4 (APP) (Fig. 2). Typical diseases presenting tauopathy are Alzheimer’s disease (AD), Pick disease, progressive supranuclear palsy, and corticobasal degeneration [35]. These diseases are classified by the number of repeats in the microtubule-binding area (tubulin-binding repeats) in the C terminal, as 3 repeats in Pick disease, 4 repeats in progressive supranuclear palsy, corticobasal degeneration, and both 3 and 4 repeats in AD. In this case study of MPSI pathology, we reported a mild p-tau accumulation of AD pattern. In MPS IIIB model mice, p-tau protein accumulation in the medial entorhinal cortex and co-expression of lysozyme protein in the same neurons have been reported, suggesting that MPS IIIB presenting tauopathy similar to the pathology of AD [36]. In Niemanpick disease type C, Glöckner et al reported that intra-neuronal cholesterol accumulation is induced by tau pathology [37]. There are some other reports suggesting p-tau or SCMAS accumulation occurs as secondary manifestation, and we need more investigation and discussion to have definite conclusion whether these are primary or secondary manifestation in MPS pathophysiology [38].
Tauopathy and Alzheimer precursor protein immunoreactive axons detected in the neuropathology of the patient with MPSI. a Expression of phosphorylated tau in the parahippocampus (arrow) in an MPS I patient (Tau protein AT8, 1:1000; Thermo Fisher Scientific, Tokyo, Japan). A1: Anti-Tau antibody, three repeat isoform RD3 (arrow) (8E6/C11, 1:1000). A2: Anti-Tau antibody, four repeat isoform RD4 (arrow) (1E1/A6, 1:1000). b Alzheimer precursor protein A4 immunoreactive axons (brown area) in the cerebral white matter. Reprinted with permission from ref. [34]
MPS-plus syndrome (MPSPS)
As a novel concept, in 2007, two groups as Kondo et al. and Dursun et al. reported a new disorder with features of the MPS independently in different locations, presenting severe systemic symptoms caused by a specific mutation in the VPS33A gene [39, 40]. Kondo et al. reported several Yakut patients presenting typical symptoms of MPS as coarse faces, dysostosis multiplex, organomegaly, respiratory problems, intellectual disability, and over excretion of heparan sulfate in urine, with atypical symptoms for conventional MPS as heart, kidney, and hematopoietic disorders, and could not be diagnosed as MPS by enzyme assay. They detected homozygous c.1492C>T (p.Arg498Trp) mutations in the VPS33A gene in 13 patients. The detected mutation did not affect either endocytic or autophagic pathways involved in VPS33A. The authors detected lysosomal over-acidification and HS accumulation in patient-derived and VPS33A depleted cells, suggesting a novel role of this gene in lysosomal functions. The HOPS complex is a large, multi-subunit tethering complex that binds organelles together and regulates late endosome-lysosome and autophagosome-lysosome fusion, composed by six subunits as VPS11, 16, 18, 33A, 39, and 41. Recently, VPS11 mutations in patients with infantile onset leukoencephalopathy were reported [40,41,42,43]. The patients in these reports showed distinct phenomena of lysosomal storage and increased urinary excretion of glycosphingolipids suggesting that the defect of a component of the HOPS complex causes accumulation of lysosomal substrates without lysosomal enzyme defects. These reports support the data that a defect in VPS33A, a component of the HOPS complex, causes GAG accumulation [39]. Clinical phenotypes of this disease of VPS33A mutation are similar to conventional MPS, and the authors indicated a new function of VPS33A as the regulation of lysosomal acidification and GAG metabolism other than in endocytosis or autophagy, and proposed this disease as a new LSD-like disease. This new disease was described as mucopolysaccharidosis-plus syndrome (MPSPS) in the Online Mendelian Inheritance in Man (MIM#617303). Almost at the same time, Dursun et al. reported two Turkish siblings with VP33A homozygous variant presenting symptoms of MPSPS by genome-wide genotyping and whole-exome sequencing [40]. Yakut belongs to the Turkic peoples and migrated to Siberia from Central Asia in the 13th century while being mixed with the Mongolians, and it is possible to share the same genetic mutation among them [44].
Differential diagnosis
Clinical differential diagnosis of MPS and its related diseases as mucolipidosis is often difficult, and enzyme assay, evaluation of GAG accumulation, and gene analysis should be a decisive factor. In mouse models, analysis of GAG accumulation in the brain should be difficult to distinguish from accumulation without pathological significance. Shimada et al. developed an analytical method for assessing pathological GAG by tandem mass spectrometer [45,46,47]. We proposed a flowchart of differential inborn error of metabolism diagnosis with dysostosis multiplex including MPS (Fig. 3). Dysotosis multiplex with MPS is different from other LSDs and X-ray findings should be critical to differentiate the diagnosis. In contrast, early diagnosis and interventional therapy have been recognized as important for improved prognosis and quality of life. Additionally, some clinical trials have begun for newborn screening, using tandem mass spectrometry [48, 49].
The algorism of differential diagnosis focusing on radiological findings as a diagnostic tool to assess patients with dysostosis multiplex in neuro-degenerative disorders. MPS mucopolysaccharidosis, GAG glycosaminoglycan, MLII mucolipidosis type II, MLIII mucolipidosis type III, MSD multiple sulfatase deficiency
Trends in treatment
Enzyme replacement therapy (ERT)
There are two insurance approved therapies for MPS, as ERT and hematopoietic stem cell transplantation (HSCT). ERT is currently considered as the standard therapy for MPS I, II, IVA, and VI [50]. This therapeutic method depends on the efficient delivery of intravenously injected recombinant enzymes captured via cell-surface receptors of the affected tissues, as mannose 6 phosphate receptor or mannose receptor [51], and has been reported to improve symptoms or test results including joint mobility, pulmonary function, hepatosplenomegary, and urinary excretion of GAGs [52, 53]. However, conventional ERT provides only insufficient effect on the skeletal or cardiac symptoms [54], and no effect on CNS manifestations mainly because the recombinant enzymes cannot cross the blood-brain barrier (BBB) [55]. And conventional ERT cannot penetrate avascular cartilage and heart valve.
There are some post-marketing surveys of ERT for MPSII. The Hunter Outcome Survey (HOS) is a global, multi-center, longitudinal, observational registry that collects data on the natural history of MPS II and the long-term safety and effect of ERT using recombinant idursulfase (Elaprase®) [56]. In the report on natural history, the data from males in the HOS registry, who did not receive growth hormones or ERT or had not begun treatment, was analyzed [57] (n = 676; January 2014). Patients had large head circumference at all ages, and above-average body weight and body mass index (BMI) during early childhood, with no pubertal growth spurt. By analysis of repeated measurements over time, an increased BMI was detected in patients with cognitive impairment than in those without, but no difference in height, weight, or head circumference between the patients with and without cognitive impairment. Logistic regression modeling revealed that greater BMI was associated with the presence of mental retardation, as were increased weight and head circumference, but not reduced height. And clinical results in IDS-treated patients with MPSII presented an improvement on GAG storage (decreases in urine GAG levels), as well as the 6-min walk test, Left ventricular mass index, forced vital capacity, and forced expiratory volume in 1 s results after 3 years of treatment [58].
Additionally, new ERT generation has been investigated and developed to overcome the existing drawback that it cannot reach the CNS. Conventional recombinant enzymes for LSDs is not effective for CNS manifestations, mainly because the enzyme cannot cross the BBB. The continuous monolayer of brain capillary endothelial cells, the basement membrane, and astrocytes constitute the BBB [59]. To develop the delivery method of intravenously administered proteins to the brain, the system called receptor-mediated transcytosis (RMT) was investigated and utilized. This system is originated from fact that some endogenous proteins as insulin, leptin and transferrin can penetrate the BBB via their specific receptors on the luminal side of brain capillary endothelial cells [60,61,62,63]. For MPS II, the human iduronate-2-sulfatase (hIDS)-fused humanized antibody against the insulin receptor (HIRMAb-IDS) [64], and the fusion protein consisting of a mouse/rat chimeric monoclonal antibody against mouse TfR and hIDS (cTfRMAb-IDS) [65] were investigated. However no reduction in the accumulative GAGs in the brain or cerebrospinal fluid was reported in these studies [64, 65], although Hendricz et al. indicated that MPS II patients with cognitive impairment have elevated levels of CSF GAG [66]. Sonoda et al. developed a BBB-penetrating fusion protein, JR-141, which consists of intact hIDS and an anti-human transferrin receptor (hTfR) antibody [67]. They reported efficient reduction of the GAGs accumulation both in the peripheral tissues and in the CNS by intravenous injection of JR-141 for hTfR knock-in MPSII model mouse, and furthermore, JR-141, but not naked hIDS, was detected in the CNS. These results provided a proof of concept, and the clinical trial has begun for MPS II patients with CNS involvement.
Hematopoietic stem cell transplantation (HSCT)
Allogeneic HSCT has been applied to treat Inherited Error of Metabolism (IEM) associated with LSD [68,69,70]. Since the first report of HSCT for IEM in 1980 [71], many transplants have been performed around the world. Kato et al. reported in the Japanese registry of analysis of HSCT for IEM the improving survival in unrelated cord blood transplantation (UCBT) [72]. The introduction of reduced intensity conditioning (RIC) after 2000 was considered to contribute to this improvement, suggesting UCBT recommendation for those who lack HLA‐identical sibling donor. RIC regimen performed an acceptable success rate and improved long-term quality of life in HSCT for non-malignant diseases in children [73, 74]. Several groups have reported encouraging results in RIC HSCT for X-linked adrenoleukodystrophy (X-ALD) patients [75,76,77,78]. Recent investigation using MPSII model mouse suggests that a milder conditioning regimen could be effective while limiting the risk of side effects for the patients [79].
HSCT is regarded as standard option for young patients with MPS IH, Hurler syndrome [71, 80,81,82]. According to the recommendations of guidelines, HSCT should be indicated when MPS I patients are <2 years of age and show an intelligence quotient (IQ) of ≥70. However, the indication of HSCT for MPSII has been controversial, as some reports suggested a limited benefit [83,84,85]. MPS II is the most frequent type of MPS in Asian patients, and recently, the usefulness of HSCT for MPSII has been reevaluated in Japan and other countries. Guffon et al. reported that the efficacy of HSCT in visceral organs was clear and similar to that of ERT [86]. Annibali et al. reported that HSCT was successful in slowing down the progression of phenotype and the improvement of neurological symptoms was slower in the first years after treatment [87]. Tanaka et al. investigated the effect of HSCT for MPSII, showing the effectiveness of brain- or heart-based therapeutics in MPS II patients when treated before a sign of brain atrophy appeared in MRI or cardiac valve dysfunction became apparent [88]. Furthermore, they indicated outcomes of HSCT superior to those of ERT in MPSII with brain involvement, and same results has been reported by another group [89, 90]. Additionally, some case reports mentioned effectiveness of early HSCT in preventing neurocognitive decline in MPSII [91, 92]. And a clinical study of 12 MPSII patients given HSCT in China showed improvements in speech, neurological impairments, and 100% survival rates [93]. Recently, HSCT has been proposed as one of the important therapeutic options for early-stage MPSII [94].
Recent reports of post-transplantation follow up results of MPS I/II patients have shown that most cases of hepatosplenomegaly, upper-airway obstruction, and recurrent otitis media resolved, but outcomes of orthopedic impairment remained unclear [95]. Regarding other types of MPS, in MPS IIII patients, bone marrow or cord blood derived HSCT fails to prevent neurological deterioration [96]. MPS IVA mainly manifests as dysostosis multiplex without mental retardation. Tomatsu et al. showed that HSCT combined with surgical treatment for MPS IVA preserved independent gait and mobility and improved respiratory function, suggesting HSCT was beneficial [93, 97,98,99]. MPS VI is a progressive disease with dysostosis multiplex, cardiac valve disease, respiratory complication, leukopenia, and hepatosplenomegaly without neurological deficit. Some reports suggested HSCT was effective in leukopenia, hepatosplenomegaly, visual acuity, and mobility. Turbeville et al. reported 45 cases of HSCT for MPS VI, and showed survival rate was 78% at 100 days, and 66% at 1 year and remained 66% at 3 years post-transplantation, with neutrophil recovery in 91% at 35 days post transplantation [100]. MPS VII is very rare, and there are few reports of the case treated with HSCT. Yamada et al. reported allogeneic Bone Marrow Transplantation in a female case [101], and Montano et al. reported five cases with HSCT, two of them died but the three survivors had some clinical benefit [102]. Sisinni et al. reported a case study of HSCT for 2-year-old female patient with MPS VII with stabilization of skeletal deformities and normal neurorecogtive development [103].
Gene therapy
To overcome the weakness of ERT and HSCT, gene therapy for IEM or severe combined immunodeficiency has been investigated and recently, some successful clinical trials have been carried out [104,105,106,107,108,109,110,111,112,113].
In viral vector-mediated gene therapy, two major ways for transduction are: in vivo (intravenous, intracranial, intrathecal, and intraventricular direct injection of viral vector), mainly using adeno-associated viral vector (AAV); and ex-vivo (modified autologous HSCT), mainly using lentiviral vector. AAV-mediated gene therapy has been reported for MPSIII, in which nervous symptoms are profound and there is no indication of ERT or HSCT [114,115,116,117,118]. Intravenous study of MPSIIIA/B and intracranial study of MPSIIIB are now under clinical trial, after completing preclinical studies [119, 120]. The other group studied the effect of AAV9 injected directly to the CSF through intra-cisternal injections in MPS II mice [121]. These data suggest that delivery of AAV vectors directly into the CSF or intravenously are potential treatment options to prevent further CNS pathology for MPS patients with CNS symptoms.
Gene therapy using lentiviral vectors have been employed for several genetic diseases [107,108,109,110,111,112,113] and shown to be effective in mouse or other animal models of MPS I, II, and III [119,120,121,122,123,124,125,126] For MPSII, we have reported the effect on CNS pathology in young adult model mice [124].
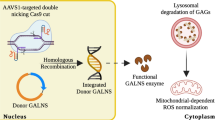
Additionally, Gregory and High et al. developed a new method of gene editing, employing an in vivo gene transfer system via systemic injection of AAV vector including ZFN for direct transduction and integration into the specific locus under the albumin promotor. This method has resulted in robust therapeutic enzyme protein in the liver cell. This method is available for inherited diseases of protein deficiency, such as MPS I/ II, Gaucher disease, Fabry disease, and hemophilia [127, 128]. Laoharawee et al. reported a zinc-finger nuclease (ZFN) system with AAV for MPSII and are starting a clinical trial [129]. In the 1st clinical trial of phase I study, the development team detected urine-GAG reduction without severe adverse effect, although they could not detect sufficient enzyme expression, and are planning to dose up in the next trial [130].
Substrate reduction therapy (SRT)
SRT for MPS has been recognized as an optional therapy to reduce GAG synthesis for correction of the imbalance between the formation and breakdown of GAGs [131, 132]. Genistein (4′ 5,7 trihydroxy isoflavone) is a soy isoflavone, which has been studied as a potential agent to supress the expression of genes coding for enzymes responsible for GAG synthesis. Recent reports suggest that Genistein modulates cell cycle in addition to modifying GAG metabolism [133], and it was shown to cross the BBB in an MPS II mouse model with histochemical evidence of GAG reduction [134]. Additionally, other groups have reported beneficial and adverse effects of SRT using Genisten for MPSI or MPSIII [134,135,136]. In clinical trials, there is not yet any apparent data to indicate that Genistein treatment can cross the BBB. However, it has been associated with an improvement in connective tissue elasticity and range of motion in the joints of MPS II patients [137].
Pentosan polysulphate (PPS) is a semi-synthetic sulfated polysaccharide polymer which has anti-coagulant, pro-chondrial, and anti-inflammatory properties. PPS has been reported to reduce GAG in tissue, to improve cartilaginous and osseous pathologies, and to decrease inflammatory markers in MPS I, III, VI and VII animal models [30, 138, 139]. Polgreen LE showed elevated TNF-α is associated with pain and physical disability in MPS I,II, and VI patients [140]. Hennermann JB reported clinical trial of PPS treatment for MPS I, and showed it was well tolerated and resulted in a significant reduction of urinary GAG excretion and in an improvement of joint mobility and pain, suggesting that PPS being effective for MPS [141].
Conclusions
We can detect wide clinical variation in MPS, and the current ERT or HSCT curative therapies have their limitations. Additionally, the pathophysiological mechanisms remain unclear. However, these mechanisms have been gradually clarified and new therapeutic methods have been established that improve patient prognosis. These include a new recombinant enzyme with the hTfR antibody, RIC-HSCT, gene therapy using a viral vector system or gene editing, and SRT. To improve the patient’s quality of life, we need to investigate the pathological mechanisms and therapeutic methods.
References
Neufeld EF, Muenzer J. The mucopolysaccharidoses. In: Scriver CR, Beaudet AL, Sly WS, editors. The metabolic and molecular basis of inherited disease. New York: McGraw-Hill; 2001. pp 3421–52.
Wraith JE. The mucopolysaccharidoses: a clinical review and guide to management. Arch Dis Child. 1995;72:263–7.
Muenzer J. The mucopolysaccharidoses: a heterogeneous group of disorders with variable pediatric presentations. J Pediatr. 2004;144(5 Suppl):S27–34.
Khan SA, Peracha H, Ballhausen D, Wiesbauer A, Rohrbach M, Gautschi M, et al. Epidemiology of mucopolysaccharidoses. Mol Genet Metab. 2017;121:227–40.
Muenzer J, Wraith JE, Clarke LA. Mucopolysaccharidosis I: management and treatment guidelines. Pediatrics. 2009;123:19–29.
Constantopoulos G, Dekaban AS. Neurochemistry of the mucopolysaccharidoses: brain lipids and lysosomal enzymes in patients with four types of mucopolysaccharidosis and in normal controls. J Neurochem. 1978;30:965–73.
Holley RJ, Deligny A, Wei W, Watson HA, Niñonuevo MR, Dagälv A, et al. Mucopolysaccharidosis type I, unique structure of accumulated heparan sulfate and increased N-sulfotransferase activity in mice lacking alpha-l-iduronidase. J Biol Chem. 2011;286:37515–24.
Wilkinson FL, Holley RJ, Langford-Smith KJ, Badrinath S, Liao A, Langford-Smith A, et al. Neuropathology in mouse models of mucopolysaccharidosis type I, IIIA and IIIB. PLoS One. 2012;7:e35787.
Eskelinen EL, Saftig P. Autophagy: a lysosomal degradation pathway with a central role in health and disease. Biochim Biophys Acta. 2009;1793:664–73.
Mizushima N. Physiological functions of autophagy. Curr Top Microbiol Immunol. 2009;335:71–84.
Dani A, Chaudhry A, Mukherjee P, Rajagopal D, Bhatia S, George A, et al. The pathway for MHCII-mediated presentation of endogenous proteins involves peptide transport to the endo-lysosomal compartment. J Cell Sci. 2004;117(Pt 18):4219–30.
Bossi G, Griffiths GM. Degranulation plays an essential part in regulating cell surface expression of Fas ligand in T cells and natural killer cells. Nat Med. 1999;5:90–96.
Castaneda JA, Lim MJ, Cooper JD, Pearce DA. Immune system irregularities in lysosomal storage disorders. Acta Neuropathol. 2008;115:159–74.
Lum JJ, DeBerardinis RJ, Thompson CB. Autophagy in metazoans: cell survival in the land of plenty. Nat Rev Mol Cell Biol. 2005;6:439–48.
Kiselyov K, Jennigs JJ Jr, Rbaibi Y, Chu CT. Autophagy, mitochondria and cell death in lysosomal storage diseases. Autophagy. 2007;3:259–62.
Settembre C, Fraldi A, Jahreiss L, Spampanato C, Venturi C, Medina D, et al. A block of autophagy in lysosomal storage disorders. Hum Mol Genet. 2008;17:119–29.
Gallucci S, Lolkema M, Matzinger P. Natural adjuvants: endogenous activators of dendritic cells. Nat Med. 1999;5:1249–55.
Matzinger P. The danger model: a renewed sense of self. Science. 2002;296:301–5.
Matzinger P. Tolerance, danger, and the extended family. Annu Rev Immunol. 1994;12:991–1045.
Bianchi ME. DAMPs, PAMPs and alarmins: all we need to know about danger. J Leukoc Biol. 2007;81:1–5.
Piccinini AM, Midwood KS. DAMPening inflammation by modulating TLR signalling. Mediators Inflamm. 2010. https://doi.org/10.1155/2010/672395.
Walter L, Neumann H. Role of microglia in neuronal degeneration and regeneration. Semin Immunopathol. 2009;31:513–25.
Ohmi K, Greenberg DS, Rajavel KS, Ryazantsev S, Li HH, Neufeld EF. Activated microglia in cortex of mouse models of mucopolysaccharidoses I and IIIB. Proc Natl Acad Sci USA. 2003;100:1902–7.
Wada R, Tifft CJ, Proia R. Microglial activation precedes acute neurodegeneration in Sandhoff disease and is suppressed by bone marrow transplantation. Proc Natl Acad Sci USA. 2000;97:10954–9.
DiRosario J, Divers E, Wang C, Etter J, Charrier A, Jukkola P, et al. Innate and adaptive immune activation in the brain of MPS IIIB mouse model. J Neurosci Res. 2009;87:978–90.
Nakao Y, Funami K, Kikkawa S, Taniguchi M, Nishiguchi M, Fukumori Y, et al. Surface-expressed TLR6 participates in the recognition of diacylated lipopeptide and peptidoglycan in human cells. J Immunol. 2005;174:1566–73.
Beck M, Braun S, Coerdt W, Merz E, Young E, Sewell AC. Fetal presentation of Morquio disease type A. Prenat Dian. 1992;12:1019–29.
Martin JJ, Ceuterick C. Prenatal pathology in mucopolysaccharidoses: a comparison with postnatal cases. Clin Neuropathol. 1983;2:122–7.
Tomatsu S, Almeciga-Diaz CJ, Montano AM, Yabe H, Tanaka A, Dung VC, et al. Therapies for the bone in mucopolysaccharidosis. Mol Genet Metab. 2015;114:94–109.
Simonaro CM, Ge Y, Eliyahu E, He X, Jepsen KJ, Schuchman EH. Involvement of the toll-like receptor 4 pathway and use of TNF-alpha antagonists for treatment of the mucopolysaccharidosis. Proc Natl Acad Sci USA. 2010;107:222–7.
Xing EM, Susan W, Ponder KP. The effect of Tlr4 and/or C3 deficiency and of neonatal gene therapy on skeletal disease in mucopolysaccharidodis VII mice. Mol Genet Metab. 2015;114:209–16.
Belleso S, Salvalaio M, Lualdi S, Tognon E, Costa R, Braghetta P, et al. FGF signaling deregulation is associated with early developmental slkeletal defects in animal models for mucopolysaccharidosis type II (MPSII). Hum Mol Genet. 2018;27:2262–75.
Kobayashi H, Ariga M, Tajima A, et al. The first trial of enzyme replacement therapy for mucopolysaccharidosis type I in Japan. (Japanese). J Jpn Pediatr Soc. 2006;110:521–5.
Kobayashi H, Ariga M, Sato Y, Fujiwara M, Fukasawa N, Fukuda T, et al. P-Tau and Subunit c mitochondrial ATP synthase accumulation in the central nervous system of a woman with Hurler-Scheie syndrome treated with enzyme replacement therapy for 12 years. JIMD Rep. 2018. https://doi.org/10.1007/8904_2018_106.
Williams DR. Tauopathies: classification and clinical update on neurodegenerative diseases associated with microtubule-associated protein tau. Intern Med J. 2006;36:652–60.
Ohmi K, Kudo LC, Ryazantsev S, Zhao HZ, Karsten SL, Neufeld EF. Sanfilippo syndrome type B, a lysosomal storage disease, is also a tauopathy. Proc Natl Acad Sci USA. 2009;106:8332–7.
Glöckner F, Ohm TG. Tau pathology induces intraneuronal cholesterol accumulation. J Neuropathol Exp Neurol. 2014;73:846–54.
Kan SH, Aoyagi-Scharber M, Le SQ, Vincelette J, Ohmi K, Bullens S, et al. Delivery of an enzyme-IGFII fusion protein to the mouse brain is therapeutic for mucopolysaccharidosis type IIIB. Proc Natl Acad Sci USA. 2014;111:14870–5.
Kondo H, Maksimova N, Otomo T, Kato H, Imai A, Asano Y, et al. Mutation in VPS33A affects metabolism of glycosaminoglycans: a new type of mucopolysaccharidosis with severe systemic symptoms. Hum Mol Genet. 2017;26:173–83.
Dursun A, Yalnizoglu D, Gerdan OF, Yucel-Yilmaz D, Sagiroglu MS, Yuksel B, et al. A probable new syndrome with the storage disease phenotype caused by the VPS33A gene mutation. Clin Dysmorphol. 2017;26:1–12.
Zhang J, Lachance V, Schaffner A, Li X, Fedick A, Kaye LE, et al. A founder mutation in VPS11 causes an autosomal recessive leukoencephalopathy linked to autophagic defects. PLoS Genet. 2016;12:e1005848.
Edvardson S, Gerhard F, Jalas C, Lachmann J, Golan D, Saada A, et al. Hypomyelination and developmental delay associated with VPS11 mutation in Ashkenazi-Jewish patients. J Med Genet. 2015;52:749–53.
Hörtnagel K, Krägeloh-Mann I, Bornemann A, Döcker M, Biskup S, Mayrhofer H, et al. The second report of a new hypomyelinating disease due to a defect in the VPS11 gene discloses a massive lysosomal involvement. J Inherit Metab Dis. 2016;39:849–57.
Yunusbayev B, Metspalu M, Metspalu E, Valeev A, Litvinov S, Valiev R, et al. The genetic legacy of the expansion of Turkic-speaking nomads across Eurasia. PLoS Genet. 2015;11:e1005068.
Yokoi T, Yokoi K, Akiyama K, Higuchi T, Shimada Y, Kobayashi H, et al. Non-myeloablative preconditioning with ACK2 (anti-c-kit antibody) is efficient in bone marrow transplantation for murine models of mucopolysaccharidosis type II. Mol Genet Metab. 2016;119:232–8.
Shimada Y, Wakabayashi T, Akiyama K, Hoshina H, Higuchi T, Kobayashi H, et al. A method for measuring disease-specific iduronic acid from the non-reducing end of glycosaminoglycan in mucopolysaccharidosis type II mice. Mol Genet Metab. 2016;117:140–3.
Yokoi K, Akiyama K, Kaneshiro E, Higuchi T, Shimada Y, Kobayashi H, et al. Effect of donor chimerism to reduce the level of glycosaminoglycans following bone marrow transplantation in a murine model of mucopolysaccharidosis type II. J Inherit Metab Dis. 2015;38:333–40.
Burton BK, Charrow J, Hoganson GE, Waggoner D, Tinkle B, Braddock SR, et al. Newborn screening for lysosomal storage disorders in Illinois: the initial 15-month experience. J Pediatr. 2017;190:130–5.
Burlina AB, Polo G, Salviati L, Duro G, Zizzo C, Dardis A, et al. Newborn screening for lysosomal storage disorders by tandem mass spectrometry in North East Italy. J Inherit Metab Dis. 2018;41:209–19.
Ohashi. T. Enzyme replacement therapy for lysosomal storage diseases. Pediatr Endocrinol Rev. 2012;10(Suppl 1):26–34.
Gary-Bobo. M, Nirdé. P, Jeanjean A, Morère A, Garcia M. Mannose 6-phosphate receptor targeting and its applications in human diseases. Curr Med Chem. 2007;14:2945–53.
Okuyama T, Tanaka A, Suzuki Y, Ida H, Tanaka T, Cox GF, et al. Japan Elaprase Treatment (JET) study: idursulfase enzyme replacement therapy in adult patients with attenuated Hunter syndrome (Mucopolysaccharidosis II, MPS II). Mol Genet Metab. 2010;99:18–25.
Giugliani R, Hwu WL, Tylki-Szymanska A, Whiteman DA, Pano A. multicenter, open-label study evaluating safety and clinical outcomes in children (1.4-7.5 years) with Hunter syndrome receiving idursulfase enzyme replacement therapy. Genet Med. 2014;16:435–41.
Wraith JE, Scarpa M, Beck M, Bodamer OA, De Meirleir L, Guffon N, et al. Mucopolysaccharidosis type II (Hunter syndrome): a clinical review and recommendations for treatment in the era of enzyme replacement therapy. Eur J Pediatr. 2008;167:267–77.
Muenzer J, Beck M, Eng CM, Giugliani R, Harmatz P, Martin R, et al. Long-term, open-labeled extension study of idursulfase in the treatment of Hunter syndrome. Genet Med. 2011;13:95–101.
Parini R, Jones SA, Harmatz PR, Giugliani R, Mendelsohn NJ. The natural history of growth in patients with Hunter syndrome: data from the Hunter Outcome Survey (HOS). Mol Genet Metab. 2016;117:438–46.
Wraith JE, Beck M, Giugliani R, Clarke J, Martin R, Muenzer J. Initial report from the Hunter Outcome Survey. Genet Med. 2008;10:508–16.
Muenzer J, Giugliani P, Scarpa M, Tylki-Szymanska A, Jego V, Beck M. Clinical outcomes in idursulfatase-treated patients with mucopolysaccharidosis type II: 3-year data from the hunter outcome survey (HOS). Orphanet J Rare Dis. 2017;12:161.
Rubin. LL, Staddon JM. The cell biology of the blood-brain barrier. Annu Rev Neurosci. 1999;22:11–28.
Pardridge WM, Eisenberg J, Yang J. Human blood-brain barrier insulin receptor. J Neurochem. 1985;44:1771–8.
Golden PL, Maccagnan TJ, Pardridge WM. Human blood-brain barrier leptin receptor. Binding and endocytosis in isolated human brain microvessels. J Clin Invest. 1997;99:14–18.
Fishman JB, Rubin JB, Handrahan JV, Connor JR, Fine RE. Receptor-mediated transcytosis of transferrin across the blood-brain barrier. J Neurosci Res. 1987;18:299–304.
Jefferies WA, Brandon MR, Hunt SV, Williams AF, Gatter KC, Mason DY. Transferrin receptor on endothelium of brain capillaries. Nature. 1984;312:162–3.
Boado RJ, Ka-Wai, Hui E, Zhiqiang LuJ, Pardridge WM. Insulin receptor antibody-iduronate 2-sulfatase fusion protein: pharmacokinetics, anti-drug antibody, and safety pharmacology in Rhesus monkeys. Biotechnol Bioeng. 2014;111:2317–25.
Zhou QH, Boado RJ, Lu JZ, Hui EK, Pardridge WM. Brain-penetrating IgG-iduronate 2-sulfatase fusion protein for the mouse. Drug Metab Dispos. 2012;40:329–35.
Hendriksz CJ, Muenzer J, Vanderver A, Davis JM, Burton BK, Mendelsohn NJ, et al. Levels of glycosaminoglycans in the cerebrospinal fluid of healthy young adults, surrogate-normal children, and Hunter syndrome patients with and without cognitive impairment. Mol Genet Metab Rep. 2015;5:103–6.
Sonoda H, Morimoto H, Yoden E, Koshimura Y, Kinoshita M, Golovina G, et al. A blood-brain-barrier-penetrating anti-human transferrin receptor antibody fusion protein for neuronopathic mucopolysaccharidosis II. Mol Ther. 2018;2. 26:1366–74.
Krivit W. Allogeneic stem cell transplantation for the treatment of lysosomal and peroxisomal metabolic diseases. Springe Semin Immunopathol. 2004;26:119–32.
Peters C, Steward CG. on behalf of the NMDP, IBMTR, and the Working Party on Inborn Errors of the EBMT. Hematopoietic cell transplantation for inherited metabolic diseases: An overview of outcomes and practice guidelines. Bone Marrow Transplant. 2003;31:229–39.
Boelens JJ, Prasad VK, Tolar J, Wynn RF, Peters C. Current international perspectives on hematopoietic stem cell transplantation for inherited metabolic disorders. Pediatr Clin North Am. 2010;57:123–45.
Hobbs JR, Hugh‐Jones K, Barrett AJ, Byrom N, Chambers D, Hennry K, et al. Reversal of clinical features of Hurler’s disease and biochemical improvement after treatment by bone‐marrow transplantation. Lancet. 1981;2:709–12.
Kato S, Yabe H, Takakura H, Mugishima H, Ishige M, Tanaka A, et al. Hematopoietic stem cell transplantation for inborn errors of metabolism: a report from the Research Committee on Transplantation for Inborn Errors of Metabolism of the Japanese Ministry of Health, Labour and Welfare and the Working Group of the Japan Society for Hematopoietic Cell Transplantation. Pediatr Transplant. 2016;20:203–14.
Jacobsohn DA, Duerst R, Tse W, Kletzel M. Reduced intensity haemopoietic stem‐cell transplantation for treatment of non‐malignant diseases in children. Lancet. 2004;364:156–62.
Resnick IB, Abdul HA, Shaipra MY, et al. Treatment of X‐linked childhood cerebral adrenoleukodystrophy by the use of an allogeneic stem cell transplantation with reduced intensity conditioning regimen. Clin Transplant. 2005;19:840–7.
Okamura K, Watanabe T, Onishi T, Watanabe H, Fujii E, Mori K, et al. Successful allogeneic unrelated bone marrow transplantation using reduced‐intensity conditioning for the treatment of X‐linked adrenoleukodystrophy in a one-yr-old boy. Pediatr Transplant. 2009;13:130–3.
Awaya T, Kato T, Niwa A, Hiramatsu H, Umeda K, Watanabe K, et al. Successful cord blood transplantation using a reduced‐intensity conditioning regimen for advanced childhood‐onset cerebral adrenoleukodystrophy. Pediatr Transplant. 2011;15:E116–E120.
Niizuma H, Uematsu M, Sakamoto O, Uchiyama T, Horino S, Onuma M, et al. Successful cord blood transplantation with reduced‐intensity conditioning for childhood cerebral X‐linked adrenoleukodystrophy at advanced and early stages. Pediatr Transplant. 2012;16:E63–E70.
Shibata M, Kato T, Awaya T, Adachi S, Heike T. Chronic immune-mediated axonal polyneuropathy following umbilical cord blood transplant for childhood-onset cerebral adrenoleukodystrophy. Pediatr Transplant. 2012;16:E388–91.
Yokoi T, Yokoi K, Akiyama K, Higuchi T, Shimada Y, Kobayashi H, et al. Non-myeloablative preconditioning with ACK2 (anti-c-kit antibody) is efficient in bone marrow transplantation for murine models of mucopolysaccharidosis type II. Mol Genet Metab. 2016;119:232–8.
Staba SL, Escolar ML, Poe M, Kim Y, Martin PL, Szabolcs P, et al. Cord-blood transplants from unrelated donors in patients with Hurler’s syndrome. N Engl J Med. 2004;350:1960–9.
Boelens JJ, Wynn RF, O’Maera A, Veys P, Bertrand Y, Souillet G, et al. Outcomes of hematopoietic stem cell transplantation for Hurler’s syndrome in Europe: a risk factor analysis for graft failure. Bone Marrow Transplant. 2007;40:225–33.
Muenzer J, Wraith JE, Clarke LA. Mucopolysaccharidosis I: management and treatment guidelines. Pediatrics. 2009;123:19–29.
Peters C, Krivit W. Hematopoietic cell transplantation for mucopolysaccharidosis IIB (Hunter syndrome). Bone Marrow Transplant. 2000;25:1097–9.
McKinnis EJ, Sulzbacher S, Rutledge JC, Sanders J, Scott CR. Bone marrow transplantation in Hunter syndrome. J Pediatr. 1996;129:145–148.
Vellodi A, Young E, Cooper A, Lidchi V, Winchester B, Wraith JE. Long-term follow-up following marrow transplantation for Hunter disease. J Inherit Metab Dis. 1999;22:638–48.
Guffon N, Bertrand Y, Forest I, Fouilhoux A, Froissart R. Bone marrow transplantation in children with Hunter Syndrome: outcome after 7 to 17 years. J Pediatr. 2009;154:733–7.
Annibali R, Caponi L, Morganti A, Manna M, Gabrielli O, Ficcadenti A. Hunter syndrome (mucopolysaccharidosis type II), severe phenotype: long term follow‐up on patients undergone to hematopoietic stem cell transplantation. Minerva Pediatr. 2013;65:487–96.
Tanaka A, Okuyama T, Suzuki Y, Sakai N, Takakura H, Sawada T, et al. Long‐term efficacy of hematopoietic stem cell transplantation on brain involvement in patients with mucopolysaccharidosis type II: a nationwide survey in Japan. Mol Genet Metab. 2012;107:513–20.
Tanaka A, Okuyama T, Suzuki Y, et al. Efficacy of enzyme replacement therapy versus hematopoietic stem cell transplantation on brain involvement in MPS II. J Inherit Metab Dis. 2013;2:s265.
Kubaski F, Yabe H, Suzuki Y, Seto T, Hamazaki T, Mason RW, et al. Hematopoietic stem cell transplantation for patients with mucopolysaccharidosis II. Biol Blood Marrow Transplant. 2017;23:1795–803.
Selvanathan A, Ellaway C, Wilson C, Owens P, Shaw PJ, Bhattacharya K. Effectiveness of early hematopoietic stem cell transplantation in preventing neurocognitive decline in mucopolysaccharidosis type II: a case series. JIMD Rep. 2018. https://doi.org/10.1007/8904_2018_104.
Barth AL, de Magalhães TSPC, Reis ABR, de Oliveira ML, Scalco FB, Cavalcanti NC. et al. Early hematopoietic stem cell transplantation in a patient with severe mucopolysaccharidosis II: a 7 years follow-up. Mol Genet Metab. 2017;12:62–68.
Wang J, Luan Z, Jiang H, Fang J, Qin M, Lee V, et al. Allogeneic hematopoietic stem cell transplantation in thirty-four pediatric cases of mucopolysaccharidosis—a ten-year report from the China Children Transplant Group. Biol Blood Marrow Transplant. 2016;22:2100–8.
Patel P, Suzuki Y, Tanaka A, Yabe H, Kato S, Shimada T, et al. Impact of enzyme replacement therapy and hematopoietic stem cell therapy on growth in patients with Hunter syndrome. Mol Genet Metab Rep. 2014;1:184–96.
Prasad VK, Kurtzberg J. Emerging trends in transplantation of inherited metabolic diseases. Bone Marrow Transplant. 2008;41:99–108.
Welling L, Marchal JP, van Hasselt P, van der Ploeg AT, Wijburg FA, Boelens JJ. Early umbilical cord blood-derived stem cell transplantation does not prevent neurological deterioration in mucopolysaccharidosis type III. JIMD Rep. 2015;18: 63–8.
Tomatsu S, Yasuda E, Patel P, Ruhnke K, Shimada T, Mackenzie WG, et al. Morquio A syndrome: diagnosis and current and future therapeuties. Pediatr Endocrinol Rev. 2014;12(supple1):141–51.
Chinen Y, Higa T, Tomatsu S, Suzuki Y, Orii T, Hyakuna N. Long-term therapeutic efficacy of allogenic bone marrow transplantation in a patient with mucopolysaccharidosis IVA. Mol Genet Metab Rep. 2014;1:31–41.
Yabe H, Tanaka A, Chinen Y, Kato S, Sawamoto K, Yasuda E. Hematopoietic stem cell transplantation for Morquio A syndrome. Mol Genet Metab. 2016;117:84–94.
Turbeville S, Nicely H, Rizzo JD, Pederson TL, Orchard PJ, Horwitz ME, et al. Clinical outcomes following hematopoietic stem cell transplantation for the treatment of mucopolysaccharidosis VI. Mol Genet Metab. 2011;102:111–5.
Yamada Y, Kato K, Sukegawa K, Tomatsu S, Fukuda S, Emura S, et al. Treatment of MPS VII (Sly disease) by allogeneic BMT in a female with homozygous A619V mutation. Bone Marrow Transplant. 1998;21:629–34.
Montano AM, Lock-Hock N, Steiner RD, Graham BH, Sziago M, Greenstein R, et al. Clinical course of Sly syndrome (mucopolysaccharidodis type VII). J Med Genet. 2016;53:403–18.
Sisinni L, Pineda M, Coll MJ, Gort L, Turon E, Torrent M et al. Haematopoietc stem cell transplantation for mucopolysaccharidosis type VII; a case report. Pediatr Transplant. 2018;22:e13278.
Naldini L. Ex vivo gene transfer and correction for cell-based therapies. Nat Rev Genet. 2011;12:301–15.
Naldini L. Gene therapy returns to centre stage. Nature. 2015;526:351–60.
Williams DA, Thrasher AJ. Concise review: lessons learned from clinical trials of gene therapy in monogenic immunodeficiency diseases. Stem Cells Transl Med. 2014;3:636–42.
Cartier N, Hacein-Bey-Abina S, Bartholomae CC, Veres G, Schmidt M, Kutschera I, et al. Hematopoietic stem cell gene therapy with a lentiviral vector in X-linked adrenoleukodystrophy. Science. 2009;326:818–23.
Eichler F, Duncan C, Musolino PL, Orchard PJ, De Oliveira S, Thrasher AJ, et al. Hematopoietic stem-cell gene therapy for cerebral adrenoleukodystrophy. N Engl J Med. 2017;377:1630–8.
Aiuti A, Biasco L, Scaramuzza S, Ferrua F, Cicalese MP, Baricordi C, et al. Lentiviral hematopoietic stem cell gene therapy in patients with Wiskott-Aldrich syndrome. Science. 2013;341:1233151.
Biffi A, Montini E, Lorioli L, Cesani M, Fumagalli F, Plati T, et al. Lentiviral hematopoietic stem cell gene therapy benefits metachromatic leukodystrophy. Science.2013;341:1233158.
Sessa M, Lorioli L, Fumagalli F, Acquati S, Redaelli D, Baldoli C, et al. Lentiviral haemopoietic stem-cell gene therapy in early-onset metachromatic leukodystrophy: an ad-hoc analysis of a non-randomised, open-label, phase 1/2 trial. Lancet. 2016;388:476–87. https://doi.org/10.1016/S0140-6736(16)30374-9.
Rosenberg JB, Kaminsky SM, Aubourg P, Crystal RG, Sondhi D. Gene therapy for metachromatic leukodystrophy. J Neurosci Res. 2016;94:1169–79.
Biffi A, Bartolomae CC, Cesana D, Cartier N, Aubourg P, Ranzani M, et al. Lentiviral vector common integration sites in preclinical models and a clinical trial reflect a benign integration bias and not oncogenic selection. Blood. 2011;117:5332–9.
Chen Y, Zheng S, Tecedor L, Davidson BL. Overcoming limitations inherent in sulfamidase to improve mucopolysaccharidosis IIIA gene therapy. Mol Ther. 2018;26:1118–26.
Haurigot V, Marcó S, Ribera A, Garcia M, Ruzo A, Villacampa P, et al. Whole body correction of mucopolysaccharidosis IIIA by intracerebrospinal fluid gene therapy. J Clin Invest. 2013;123:3254–71.
Ruzo A, Marcó S, García M, Villacampa P, Ribera A, Ayuso E, et al. Bosch Correction of pathological accumulation of glycosaminoglycans in central nervous system and peripheral tissues of MPSIIIA mice through systemic AAV9 gene transfer. Hum Gene Ther. 2012;23:1237–46.
Fu H, Cataldi MP, Ware TA, Zaraspe K, Meadows AS, Murrey DA, et al. Functional correction of neurological and somatic disorders at later stages of disease in MPS IIIA mice by systemic scAAV9-hSGSH gene delivery. Mol Ther Methods Clin Dev. 2016;3:16036.
Tardieu M, Zérah M, Husson B, de Bournonville S, Deiva K, Adamsbaum C, et al. Intracerebral administration of adeno-associated viral vector serotype rh.10 carrying human SGSH and SUMF1 cDNAs in children with mucopolysaccharidosis type IIIA disease: results of a phase I/II trial. Hum Gene Ther. 2014;25:506–16.
Gilkes JA, Bloom MD, Heldermon CD. Mucopolysaccharidosis IIIB confers enhanced neonatal intracranial transduction by AAV8 but not by 5, 9 orrh10. Gene Ther. 2016;23:263–71.
Chen YH, Claflin K, Geoghegan JC, Davidson BL. Sialic acid deposition impairs the utility of AAV9, but not peptide-modified AAVs for brain gene therapy in a mouse model of lysosomal storage disease. Mol Ther. 2012;20:1393–9.
Motas S, Haurigot V, Garcia M, Marcó S, Ribera A, Roca C, et al. CNS-directed gene therapy for the treatment of neurologic and somatic mucopolysaccharidosis type II (Hunter syndrome). JCI Insight. 2016;1:e86696.
Visigalli I, Delai S, Politi LS, Di Domenico C, Cerri F, Mrak E, et al. Gene therapy augments the efficacy of hematopoietic cell transplantation and fully corrects mucopolysaccharidosis type I phenotype in the mouse model. Blood. 2010;116:5130–9.
Kobayashi H, Carbonaro D, Pepper K, Petersen D, Ge S, Jackson H, et al. Neonatal gene therapy of MPS I mice by intravenous injection of a lentiviral vector. Mol Ther. 2005;11:776–89.
Wakabayashi T, Shimada Y, Akiyama K, Higuchi T, Fukuda T, Kobayashi H, et al. Hematopoietic stem cell gene therapy corrects neuropathic phenotype in murine model of mucopolysaccharidosis type II. Hum Gene Ther. 2015;26:357–66.
McIntyre C, Derrick Roberts AL, Ranieri E, Clements PR, Byers S, Anson DS. Lentiviral-mediated gene therapy for murine mucopolysaccharidosis type IIIA. Mol Genet Metab. 2008;93:411–8.
Derrick-Roberts AL, Pyragius CE, Kaidonis XM, Jackson MR, Anson DS, Byers S. Lentiviral-mediated gene therapy results in sustained expression of β-glucuronidase for up to 12 months in the gus(mps/mps) and up to 18 months in the gus(tm(L175F)Sly) mouse models of mucopolysaccharidosis type VII. Hum Gene Ther. 2014;25:798–810.
Sharma R, Anguela XM, Doyon Y, Wechsler T, DeKelver RC, Sproul S, et al. In vivo genome editing of the albumin locus as a platform for protein replacement therapy. Blood. 2015;126:1777–84.
Li H, Haurigot V, Doyon Y, Li T, Wong SY, Bhagwat AS, et al. In vivo genome editing restores haemostasis in a mouse model of haemophilia. Nature. 2011;475:217–21.
Laoharawee K, DeKelver RC, Podetz-Pedersen KM, Rohde M, Sproul S, Nguyen HO, et al. Dose-dependent prevention of metabolic and neurologic disease in murine MPS II by ZFN-mediated in vivo genome editing. Mol Ther. 2018;4:1127–36.
SSIEM. 2018: Annual Symposium of the Society for the Study of Inborn Errors of Metabolism, Athens, Greece, 4–7 September 2018. J Inherit Metab Dis. 2018;41(Suppl 1):1573–2665.
Friso A, Tomanin R, Salvalaio M, Scarpa M. Genistein reduces glycosaminoglycan levels in a mouse model of mucopolysaccharidosis type II. Br J Pharmacol. 2010;159:1082–91.
Stapleton M, Kubaski F, Mason RW, Yabe H, Suzuki Y, Orii KE, et al. Presentation and treatments for mucopolysaccharidosis type II (MPS II; Hunter Syndrome). Expert Opin Orphan Drugs. 2017;5:295–307.
Moskot M, Gabig-Cimińska M, Jakóbkiewicz-Banecka J, Węsierska M, Bocheńska K, Węgrzyn G. Cell cycle is disturbed in mucopolysaccharidosis type II fibroblasts, and can be improved by genistein. Gene. 2016;585:100–3.
Kingma SD, Wagemans T, IJlst L, Seppen J, Gijbels MJ, Wijburg FA, et al. Adverse effects of genistein in a Mucopolysaccharidosis Type I Mouse Model. JIMD Rep. 2015;23:77–83. https://doi.org/10.1007/8904_2015_432.
de Ruijter J, Valstar MJ, Narajczyk M, Wegrzyn G, Kulik W, Ijlst L, et al. Genistein in Sanfilippo disease: a randomized controlled crossover trial. Ann Neurol. 2012;71:110–20. https://doi.org/10.1002/ana.22643.
Kim KH, Dodsworth C, Paras A, Burton BK. High dose genistein aglycone therapy is safe in patients with mucopolysaccharidoses involving the central nervous system. Mol Genet Metab. 2013;109:382–5.
Marucha J, Tylki-Szymańska A, Jakóbkiewicz-Banecka J, Piotrowska E, Kloska A, Czartoryska B, et al. Improvement in the range of joint motion in seven patients with mucopolysaccharidosis type II during experimental gene expression-targeted isoflavone therapy (GET IT). Am J Med Genet A. 2011;155 A:2257–62.
Guo N, DeAngelis V, Zhu C, Schuchman EH, Simonaro CM. Pentosan polysulfate treatment of mucopolysaccharidosis type IIIA mice. JIMD Rep. 2018. https://doi.org/10.1007/8904_2018_96. PMID:29654542.
Simonaro CM, D’Angelo M, Haskins ME, Schuchman EH. Joint and bone disease in mucopolysaccharidoses VI and VII: identification of new therapeutic targets and biomarkers using animal models. Pediatr Res. 2005;57(5 Pt 1):701–7.
Polgreen LE, Vehe RK, Rudser K, Kunin-Batson A, Utz JJ, Dickson P, et al. Elevated TNF-α is associated with pain and physical disability in mucopolysaccharidosis types I, II, and VI. Mol Genet Metab. 2016;S1096-7192:30011–7. PMID 26873528
Hennermann JB, Gökce S, Solyom A, Mengel E, Schuchman EH, Simonaro CM. Treatment with pentosan polysulphate in patients with MPS I: results from an open label, randomized, monocentric phase II study. J Inherit Metab Dis. 2016;39:831–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kobayashi, H. Recent trends in mucopolysaccharidosis research. J Hum Genet 64, 127–137 (2019). https://doi.org/10.1038/s10038-018-0534-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s10038-018-0534-8
This article is cited by
-
Dysregulation of genes coding for proteins involved in metabolic processes in mucopolysaccharidoses, evidenced by a transcriptomic approach
Metabolic Brain Disease (2023)
-
Establishing a core outcome set for mucopolysaccharidoses (MPS) in children: study protocol for a rapid literature review, candidate outcomes survey, and Delphi surveys
Trials (2021)
-
Upper Extremity Compressive Neuropathies in the Pediatric and Adolescent Populations
Current Reviews in Musculoskeletal Medicine (2020)
-
Hip morphology in mucopolysaccharidosis type IVA through radiograph, magnetic resonance imaging and arthrogram assessment
International Orthopaedics (2020)
-
Changes in expressions of genes involved in the regulation of cellular processes in mucopolysaccharidoses as assessed by fibroblast culture-based transcriptomic analyses
Metabolic Brain Disease (2020)