Abstract
Background
Whether the diagnosis of prostate cancer is a contributory psychological stress that causes excess risk of suicide among affected men remains controversial. We performed a meta-analysis of previous studies to investigate suicide incidence and associated risk factors among men diagnosed with prostate cancer.
Methods
The MEDLINE, Embase, Cochrane Library, and PsycINFO databases were searched to identify eligible studies published before April 2018. The inverse variance method with random-effects modeling was used to calculate summary relative risks (RRs) and their associated 95% confidence intervals (CIs).
Results
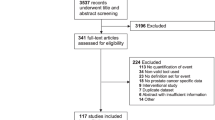
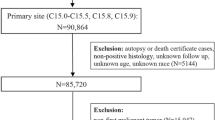
Eight observational studies involving 1,281,393 men diagnosed with prostate cancer and 842,294 matched prostate cancer-free men were included. An overall increased RR of suicide of 2.01 (95% CI: 1.52–2.64; P < 0.001; I2 = 91.8%) was observed among men diagnosed with prostate cancer compared with those without prostate cancer during the first year, especially during the first 6 months (RR = 2.24, 95% CI: 1.77–2.85; P < 0.001; I2 = 61.1%) after diagnosis. Moreover, prostate cancer patients were at an increased risk of suicide among men aged 75 years or older (RR = 1.51, 95% CI: 1.04–2.18; P = 0.028; I2 = 91.5%) and treated with hormonal therapy (RR = 1.80, 95% CI: 1.54–2.12; P < 0.001; I2 = 0%). Furthermore, marital status, race, disease risk category, and socioeconomic status were not associated with increased suicide risk in men with prostate cancer.
Conclusions
Current evidence indicates that the risk of suicide is increased among men diagnosed with prostate cancer, particularly those aged 75 years or older, <12 months after diagnosis, and treated with hormonal therapy. Healthcare providers should be aware of these special populations considered at high risk of suicide. Hence, further research should be conducted to refine suicide risk assessment with detection tools and to develop the best practices for prevention.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer. 2010;127:2893–917.
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90.
Hugosson J, Aus G, Lilja H, Lodding P, Pihl CG, Pileblad E. Prostate specific antigen based biennial screening is sufficient to detect almost all prostate cancers while still curable. J Urol. 2003;169:1720–3.
Chen PM, Chen SC, Liu CJ, Hung MH, Tsai CF, Hu YW, et al. The association between prostate cancer and mood disorders: a nationwide population-based study in Taiwan. Int Psychogeriatr. 2015;27:481–90.
Bill-Axelson A, Garmo H, Nyberg U, Lambe M, Bratt O, Stattin P, et al. Psychiatric treatment in men with prostate cancer-results from a Nation-wide, population-based cohort study from PCBaSe Sweden. Eur J Cancer. 2011;47:2195–201.
Mehnert A, Lehmann C, Graefen M, Huland H, Koch U. Depression, anxiety, post-traumatic stress disorder and health-related quality of life and its association with social support in ambulatory prostate cancer patients. Eur J Cancer Care (Engl). 2010;19:736–45.
CDC/Suicide Statistics 2009 resources page. Center for Disease Control Web site. http://www.cdc.gov/ViolencePrevention/suicide/statistics/. Accessed 26 Aug 2011.
Erlangsen A, Stenager E, Conwell Y. Physical diseases as predictors of suicide in older adults: a nationwide, register-based cohort study. Soc Psychiatry Psychiatr Epidemiol. 2015;50:1427–39.
Angst J, Angst F, Stassen HH. Suicide risk in patients with major depressive disorder. J Clin Psychiatry. 1999;2:57–62.
Berglund M, Ojehagen A. The influence of alcohol drinking and alcohol use disorders on psychiatric disorders and suicidal behavior. Alcohol Clin Exp Res. 1998;22:333–45.
Fang F, Fall K, Mittleman MA, Sparén P, Ye W, Adami HO, et al. Suicide and cardiovascular death after a cancer diagnosis. N Engl J Med. 2012;366:1310–8.
Yousaf U, Christensen ML, Engholm G, Storm HH. Suicides among Danish cancer patients 1971–1999. Br J Cancer. 2005;92:995–1000.
Simpson WG, Klaassen Z, Jen RP, Hughes WM 5th, Neal DE Jr, Terris MK. Analysis of suicide risk in patients with penile cancer and review of the literature. Clin Genitourin Cancer. 2018;16:257–61.
Akechi T, Okamura H, Nishiwaki Y, Uchitomi Y. Predictive factors for suicide ideation in patients with unresectable lung carcinoma: a 6 month follow-up study. Am Cancer Soc. 2002;95:1085–93.
Schairer C, Brown LM, Chen BE, Howard R, Lynch CF, Hall P, et al. Suicide after breast cancer: an international population-based study of 723,819 women. J Natl Cancer Inst. 2006;98:1416–9.
Bill-Axelson A, Garmo H, Lambe M, Bratt O, Adolfsson J, Nyberg U, et al. Suicide risk in men with prostate-specific antigen-detected early prostate cancer: a nationwide population-based cohort study from PCBaSe Sweden. Eur Urol. 2010;57:390–5.
Carlsson S, Sandin F, Fall K, Lambe M, Adolfsson J, Stattin P, et al. Risk of suicide in men with low-risk prostate cancer. Eur J Cancer. 2013;49:1588–99.
Dalela D, Krishna N, Okwara J, Preston MA, Abdollah F, Choueiri TK, et al. Suicide and accidental deaths among patients with non-metastatic prostate cancer. BJU Int. 2016;118:286–97.
Fall K, Fang F, Mucci LA, Ye W, Andrén O, Johansson JE, et al. Immediate risk for cardiovascular events and suicide following a prostate cancer diagnosis: prospective cohort study. PLoS Med. 2009;6:e1000197.
Fang F, Keating NL, Mucci LA, Adami HO, Stampfer MJ, Valdimarsdóttir U, et al. Immediate risk of suicide and cardiovascular death after a prostate cancer diagnosis: cohort study in the United States. J Natl Cancer Inst. 2010;102:307–14.
Juurlink DN, Herrmann N, Szalai JP, Kopp A, Redelmeier DA. Medical illness and the risk of suicide in the elderly. Arch Intern Med. 2004;164:1179–84.
Klaassen Z, Arora K, Wilson SN, King SA, Madi R, Neal DE Jr, et al. Decreasing suicide risk among patients with prostate cancer: implications for depression, erectile dysfunction, and suicidal ideation screening. Urol Oncol. 2018;36:60–6.
Higgins JPT, Green S. Cochrane handbook for systematic reviews of interventions version 5.1.0 [updated March 2011]. Cochrane Collab. 2011.
Moher D, Liberati A, Tetzlaff J, Altman DG. PRISMA group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–9.
Wells G, Shea B, O’Connell D, Robertson J, Peterson J, Welch V, et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analysis. Ottawa Hospital Research Institute website. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. 2014.
Greenland S. Quantitative methods in the review of epidemiologic literature. Epidemiol Rev. 1987;9:1–30.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.
Llorente MD, Burke M, Gregory GR, Bosworth HB, Grambow SC, Horner RD, et al. Prostate cancer: a significant risk factor for late-life suicide. Am J Geriatr Psychiatry. 2005;13:195–201.
Smith DP, Bang A, Egger S, Yu XQ, Egger S, Chambers S, et al. Risk of suicide after a prostate cancer diagnosis: a populationwide study in New South Wales (NSW) Australia. BJU Int. 2015;116:22.
Klaassen Z, Jen RP, DiBianco JM, Reinstatler L, Li Q, Madi R, et al. Factors associated with suicide in patients with genitourinary malignancies. Cancer. 2015;121:1864–72.
Meyer CP, Dalela D, Hanske J, Abdollah F, Sammon JD, Schmid M, et al. Suicide and accidental deaths in prostate cancer. Eur Urol Suppl. 2015;14:366.
Korfage IJ, Essink-Bot ML, Janssens AC, Schröder FH, de Koning HJ. Anxiety and depression after prostate cancer diagnosis and treatment: 5-year follow-up. Br J Cancer. 2006;94:1093–8.
Watts S, Leydon G, Birch B, Prescott P, Lai L, Eardley S, et al. Depression and anxiety in prostate cancer: a systematic review and meta-analysis of prevalence rates. BMJ Open. 2014;4:e003901
Pirl WF, Siegel GI, Goode ML, Smith MR. Depression in men receiving androgen deprivation therapy for prostate cancer: a pilot study. Psychooncology. 2002;11:518–23.
Cheng AT. Mental illness and suicide: a case-control study in east Taiwan. Arch Gen Psychiatry. 1995;52:594–603.
Herr HW, O’sullivan M. Quality of life of asymptomatic men with nonmetastatic prostate cancer on androgen deprivation therapy. J Urol. 2000;163:1743–6.
Legarreta M, Bueler E, DiMuzio J, McGlade E, Yurgelun-Todd D. Suicide behavior and chronic pain: an exploration of pain-related catastrophic thinking, disability, and descriptions of the pain experience. J Nerv Ment Dis. 2018;206:217–22.
Van Leeuwen P, Schroeder F. Risk factors: increased risk of suicide after prostate cancer diagnosis. Nat Rev Urol. 2010;7:369–70.
Coleman RE. Metastatic bone disease: clinical features, pathophysiology and treatment strategies. Cancer Treat Rev. 2001;27:165–76.
Cattell H. Suicide in the elderly. Adv Psychiatr Treat. 2000;6:102–8.
Acknowledgements
This study was supported by grants from the National Natural Science Foundation of China (Grant No. 61301294). The supporting institution had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Author contributions
SW conceived the study idea. ZG, SG, CG, SX, JZ, LG, and SW performed literature search, study selection, data extraction, methodological quality assessment. YL and FC performed statistical analyses and interpretation of corresponding results. ZG drafted the initial manuscript. SW modified the initial manuscript. SW had primarily responsibility for final content. All authors made critical comment for the initial manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Guo, Z., Gan, S., Li, Y. et al. Incidence and risk factors of suicide after a prostate cancer diagnosis: a meta-analysis of observational studies. Prostate Cancer Prostatic Dis 21, 499–508 (2018). https://doi.org/10.1038/s41391-018-0073-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-018-0073-6
This article is cited by
-
Sexual health and treatment-related sexual dysfunction in sexual and gender minorities with prostate cancer
Nature Reviews Urology (2023)
-
Living with prostate cancer: a mixed-method evaluation of group therapy intervention to alleviate psychological distress in a Canadian setting
Supportive Care in Cancer (2023)
-
Effects of yoga in men with prostate cancer on quality of life and immune response: a pilot randomized controlled trial
Prostate Cancer and Prostatic Diseases (2022)
-
Top, bottom or vers? Creating a more equitable health system for sexual and gender minority patients with prostate cancer
Nature Reviews Urology (2022)
-
Depression, anxiety, and suicidality in patients with prostate cancer: a systematic review and meta-analysis of observational studies
Prostate Cancer and Prostatic Diseases (2021)