Abstract
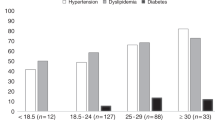
Advances in allogeneic hematopoietic stem cell transplantation (HSCT) in malignant and non-malignant diseases result in more long-term survivors, in whom cardiovascular (CV) disease is one leading non-cancer cause of death. This study aimed to evaluate risk factors and subclinical CV organ damage in survivors after HSCT in pediatric age. We enrolled 64 children in a cross-sectional approach 3.3 ± 3.1 years after HSCT. Anthropometric data, laboratory values, office and 24-h ambulatory blood pressure monitoring (ABPM) were evaluated, showing a high prevalence of obesity, hypertension and dyslipidemia. CV organ damage was determined by non-invasive measurements of aortic pulse wave velocity (PWV), left ventricular mass index (LVMI), and carotid intima media thickness (IMT). Increased IMT and elevated PWV reflecting subclinical vascular damage were detected in 48% (IMT) and 6% (PWV) of our population. For IMT, physical activity had a positive impact and was worsened by time after HSCT. Our results show a surprisingly high rate of subclinical CV organ damage and classical risk factors. Therefore, diagnosis and management of well-known CV risk factors belong to clinical care after HSCT.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Passweg JR, Baldomero H, Bader P, Bonini C, Cesaro S, Dreger P, et al. Hematopoietic stem cell transplantation in Europe 2014: more than 40 000 transplants annually. Bone Marrow Transplant. 2016;51:786–92.
Majhail NS, Tao L, Bredeson C, Davies S, Dehn J, Gajewski JL, et al. Prevalence of hematopoietic cell transplant survivors in the United States. Biol Blood Marrow Transplant. 2013;19:1498–501.
Armenian SH, Sun C, Kawashima T, Arora M, Leisenring W, Sklar CA et al. Long-term health-related outcomes in survivors of childhood cancer treated with HSCT versus conventional therapy: a report from the Bone Marrow Transplant Survivor Study (BMTSS) and Childhood Cancer Survivor Study (CCSS). Blood. 2011;118:1413–20.
Eapen M, Ahn KW, Orchard PJ, Cowan MJ, Davies SM, Fasth A, et al. Long-term survival and late deaths after hematopoietic cell transplantation for primary immunodeficiency diseases and inborn errors of metabolism. Biol Blood Marrow Transplant. 2012;18:1438–45.
Bonfim C, Ribeiro L, Nichele S, Bitencourt M, Loth G, Koliski A, et al. Long-term survival, organ function, and malignancy after hematopoietic stem cell transplantation for fanconi anemia. Biol Blood Marrow Transplant. 2016;22:1257–63.
Bresters D, Lawitschka A, Cugno C, Pötschger U, Dalissier A, Michel G, et al. Incidence and severity of crucial late effects after allogeneic HSCT for malignancy under the age of 3 years: TBI is what really matters. Bone Marrow Transplant. 2016;51:1482–9.
Armenian SH, Sun C-L, Vase T, Ness KK, Blum E, Francisco L, et al. Cardiovascular risk factors in hematopoietic cell transplantation (HCT) survivors: role in development of subsequent cardiovascular disease. Blood. 2012;120:4505–13.
Chow EJ, Wong K, Lee SJ, Cushing-Haugen KL, Flowers MED, Friedman DL, et al. Late cardiovascular complications after hematopoietic cell transplantation. Biol Blood Marrow Transplant. 2014;20:794–800.
Bhatia S, Francisco L, Carter A, Sun C, Baker KS, Gurney JG, et al. Late mortality after allogeneic hematopoietic cell transplantation and functional status of long-term survivors: report from the bone marrow transplant survivor study. Blood. 2007;110:3784–92.
Tichelli A, Bucher C, Rovo A, Stussi G, Stern M, Paulussen M, et al. Premature cardiovascular disease after allogeneic hematopoietic stem-cell transplantation. Blood. 2007;110:3463–71.
Baker KS, Chow E, Steinberger J. Metabolic syndrome and cardiovascular risk in survivors after hematopoietic cell transplantation. Bone Marrow Transplant. 2012;47:619–25.
Majhail NS, Flowers ME, Ness KK, Jagasia M, Carpenter Pa, Arora M, et al. High prevalence of metabolic syndrome after allogeneic hematopoietic cell transplantation. Bone Marrow Transplant. 2009;43:49–54.
Bielorai B, Weintraub Y, Hutt D, Hemi R, Kanety H, Modan-Moses D, et al. The metabolic syndrome and its components in pediatric survivors of allogeneic hematopoietic stem cell transplantation. Clin Transplant. 2017;31:e12903.
Dzau V, Braunwald E. Resolved and unresolved issues in the prevention and treatment of coronary artery disease: a workshop consensus statement. Am Heart J. 1991;121:1244–63.
Verbeke F, Maréchal C, Van Laecke S, Van Biesen W, Devuyst O, Van Bortel LM, et al. Aortic stiffness and central wave reflections predict outcome in renal transplant recipients. Hypertens. 2011;58:833–8.
Zoungas S, Cameron JD, Kerr PG, Wolfe R, Muske C, McNeil JJ, et al. Association of carotid intima-medial thickness and indices of arterial stiffness with cardiovascular disease outcomes in CKD. Am J Kidney Dis. 2007;50:622–30.
Polak JF, Pencina MJ, Pencina KM, O’Donnell CJ, Wolf PA, D’Agostino RB. Carotid-wall intima-media thickness and cardiovascular events. N Engl J Med. 2011;365:213–21.
Ben-Shlomo Y, Spears M, Boustred C, May M, Anderson SG, Benjamin EJ, et al. Aortic pulse wave velocity improves cardiovascular event prediction: an individual participant meta-analysis of prospective observational data from 17,635 subjects. J Am Coll Cardiol. 2014;63:636–46.
Vlachopoulos C, Aznaouridis K, Stefanadis C. Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol. 2010;55:1318–27.
Morrison KM, Dyal L, Conner W, Helden E, Newkirk L, Yusuf S, et al. Cardiovascular risk factors and non-invasive assessment of subclinical atherosclerosis in youth. Atherosclerosis. 2010;208:501–5.
Aggoun Y, Szezepanski I, Bonnet D. Noninvasive assessment of arterial stiffness and risk of atherosclerotic events in children. Pediatr Res. 2005;58:173–8.
Glucksberg H, Storb R, Fefer A, Buckner CD, Neiman PE, Clift RA, et al. Clinical manifestations of graft-versus-host disease in human recipients of marrow from HL-A-matched sibling donors. Transplantation. 1974;18:295–304.
Filipovich AH, Weisdorf D, Pavletic S, Socie G, Wingard JR, Lee SJ, et al. National Institutes of Health Consensus Development Project on criteria for clinical trials in chronic graft-versus-host disease: I. Diagnosis and staging working group report. Biol Blood Marrow Transplant. 2005;11:945–56.
Doyon A, Kracht D, Bayazit AK, Deveci M, Duzova A, Krmar RT, et al. Carotid artery intima-media thickness and distensibility in children and adolescents: reference values and role of body dimensions. Hypertension. 2013;62:550–6.
Kracht D, Shroff R, Baig S, Doyon A, Jacobi C, Zeller R, et al. Validating a new oscillometric device for aortic pulse wave velocity measurements in children and adolescents. Am J Hypertens. 2011;24:1294–9.
Barlow S, Expert Committee. Expert Committee Recommendations Regarding the Prevention, Assessment, and Treatment of Child and Adolescent Overweight and Obesity: Summary Report. Pediatrics. 2007;120:S164–92.
Fernández JR, Redden DT, Pietrobelli A, Allison DB. Waist circumference percentiles in nationally representative samples of African-American, European-American, and Mexican-American children and adolescents. J Pediatr. 2004;145:439–44.
Borchert-Mörlins B, Thurn D, Schmidt BMW, Büscher AK, Oh J, Kier T, et al. Factors associated with cardiovascular target organ damage in children after renal transplantation. Pediatr Nephrol. 2017;32:2143–54.
Sharma AK, Metzger DL, Daymont C, Hadjiyannakis S, Rodd CJ. LMS tables for waist-circumference and waist-height ratio Z-scores in children aged 5-19 y in NHANES III: association with cardio-metabolic risks. Pediatr Res. 2015;78:723–9.
Joan C Han, Debbie A Lawlor, Sue YS Kimm, (2010) Childhood obesity. The Lancet 375 (9727):1737–1748.
Van Bortel LM, Duprez D, Starmans-Kool MJ, Safar ME, Giannattasio C, Cockcroft J, et al. Clinical applications of arterial stiffness, Task Force III: recommendations for user procedures. Am J Hypertens. 2002;15:445–52.
Thurn D, Doyon A, Sözeri B, Bayazit AK, Canpolat N, Duzova A, et al. Aortic pulse wave velocity in healthy children and adolescents: reference values for the vicorder device and modifying factors. Am J Hypertens. 2015;28:1480–8.
Touboul P-J, Hennerici MG, Meairs S, Adams H, Amarenco P, Bornstein N, et al. Mannheim carotid intima-media thickness and plaque consensus (2004-6–2011). Cerebrovasc Dis. 2012;34:290–6.
Devereux RB, Alonso DR, Lutas EM, Gottlieb GJ, Campo E, Sachs I, et al. Echocardiographic assessment of left ventricular hypertrophy: comparison to necropsy findings. Am J Cardiol. 1986;57:450–8.
Chinali M, Emma F, Esposito C, Rinelli G, Franceschini A, Doyon A, et al. Left ventricular mass indexing in infants, children, and adolescents: a simplified approach for the identification of left ventricular hypertrophy in clinical practice. J Pediatr. 2016;170:193–8.
Wühl E, Witte K, Soergel M, Mehls O, Schaefer F, German Working Group on Pediatric Hypertension. Distribution of 24-h ambulatory blood pressure in children: normalized reference values and role of body dimensions. J Hypertens. 2002;20:1995–2007.
Lurbe E, Agabiti-Rosei E, Cruickshank JK, Dominiczak A, Erdine S, et al. 2016 European $ociety of hypertension guidelines for the management of high blood pressure in children and adolescents. J Hypertens. 2016;34(10):1887-920.
Cole TJ. The LMS method for constructing normalized growth standards. Eur J Clin Nutr. 1990;44:45–60.
Schrappe M, Reiter A, Henze G, Welte K, Gadner H, Ritter J et al. Key treatment questions in childhood acute lymphoblastic leukemia: results in 5 consecutive trials performed by the ALL-BFM Study Group from 1981 to 2000 Kernfragen der Behandlung von akuten lymphoblastischen Leukämien. Klin Padiatr. 2013;225 Suppl 1;S62–72.
Schwartz GJ, Schneider MF, Maier PS, Moxey-Mims M, Dharnidharka VR, Warady BA, et al. Improved equations estimating GFR in children with chronic kidney disease using an immunonephelometric determination of cystatin C. Kidney Int. 2012;82(4):445–53.
Kozakova M, Morizzo C, Bianchi V, Marchetti S, Federico G, Palombo C. Hemodynamic overload and intra-abdominal adiposity in obese children: Relationships with cardiovascular structure and function. Nutr Metab Cardiovasc Dis. 2016;26:60–6.
Andersen LB, Riddoch C, Kriemler S, Hills A, Hills A. Physical activity and cardiovascular risk factors in children. Br J Sports Med. 2011;45:871–6.
London GM, Marchais SJ, Guerin AP, Pannier B. Arterial stiffness: pathophysiology and clinical impact. Clin Exp Hypertens. 26:689–99.
Krystal JI, Reppucci M, Mayr T, Fish JD, Sethna C. Arterial stiffness in childhood cancer survivors. Pediatr Blood Cancer. 2015;62:1832–7.
Zanchetti A, Hennig M, Hollweck R, Bond G, Tang R, Cuspidi C, et al. Baseline values but not treatment-induced changes in carotid intima-media thickness predict incident cardiovascular events in treated hypertensive patients: findings in the european lacidipine study on atherosclerosis (ELSA). Circulation. 2009;120:1084–90.
García-Hermoso A, González-Ruiz K, Triana-Reina HR, Olloquequi J, Ramírez-Vélez R. Effects of exercise on carotid arterial wall thickness in obese pediatric populations: a meta-analysis of randomized controlled trials. Child Obes. 2017;13(2):138-145.
Thijssen DHJ, Cable NT, Green DJ. Impact of exercise training on arterial wall thickness in humans. Clin Sci. 2012;122:311–22.
Kesting SV, Götte M, Seidel CC, Rosenbaum D, Boos J. One in four questioned children faces problems regarding reintegration into physical education at school after treatment for pediatric cancer. Pediatr Blood Cancer. 2016;63:737–9.
Chow EJ, Simmons JH, Roth CL, Baker KS, Hoffmeister Pa, Sanders JE, et al. Increased cardiometabolic traits in pediatric survivors of acute lymphoblastic leukemia treated with total body irradiation. Biol Blood Marrow Transplant. 2010;16:1674–81.
Hoffmeister Pa, Hingorani SR, Storer BE, Baker KS, Sanders JE. Hypertension in long-term survivors of pediatric hematopoietic cell transplantation. Biol Blood Marrow Transplant. 2010;16:515–24.
Kollias A, Dafni M, Poulidakis E, Ntineri A, Stergiou GS. Out-of-office blood pressure and target organ damage in children and adolescents. J Hypertens. 2014;32:2315–31.
Neilan TG, Coelho-Filho OR, Pena-Herrera D, Shah RV, Jerosch-Herold M, Francis SA, et al. Left ventricular mass in patients with a cardiomyopathy after treatment with anthracyclines. Am J Cardiol. 2012;110:1679–86.
Mohty M, Malard F, Abecassis M, Aerts E, Alaskar AS, Aljurf M, et al. Sinusoidal obstruction syndrome/veno-occlusive disease: current situation and perspectives—a position statement from the European Society for Blood and Marrow Transplantation (EBMT). Bone Marrow Transplant. 2015;50:781–9.
Pearce EN. Hypothyroidism and dyslipidemia: modern concepts and approaches. Curr Cardiol Rep. 2004;6:451–6.
Lipshultz SE, Landy DC, Lopez-Mitnik G, Lipsitz SR, Hinkle AS, Constine LS, et al. Cardiovascular status of childhood cancer survivors exposed and unexposed to cardiotoxic therapy. J Clin Oncol. 2012;30:1050–7.
Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. Pediatrics. 2011 Dec;128 Suppl 5:S213–56.
Krug S, Jekauc D, Poethko-Müller C, Woll A, Schlaud M. Zum Zusammenhang Zwischen Körperlicher Aktivität und Gesundheit bei Kindern und Jugendlichen Ergebnisse des Kinder–und Jugendgesundheitssurveys (KiGGS) und des Motorik-Moduls (MoMo). Bundesgesundheitsblatt–Gesundh–Gesundh. 2012;55:111–20.
Acknowledgements
We would like to thank the participating patients and families for their support of this study, especially for their time and adherence. Many people were involved in patient care and organization of this study. Special thanks goes to the outpatient nurse staff and the study nurse team of the pediatric oncology and of pediatric nephology. We would like to thank the HSCT-team as well as the heads of the Depts. of Pediatric Oncology and Haematology at Hannover Medical School (Prof. C. Kratz) and the University of Essen (Prof. D. Reinhardt) for their support of this study. This work was supported by the German Ministry of Education and Research through the Integrated Research and Treatment Center Transplantation (ref. 01EO0802), by the Verein für krebskranke Kinder e.V., and by the Betreuungsnetzwerk für schwerkranke Kinder Hannover e.V.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Anette Melk and Rita Beier contributed equally to this work.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Borchert-Mörlins, B., Memaran, N., Sauer, M. et al. Cardiovascular risk factors and subclinical organ damage after hematopoietic stem cell transplantation in pediatric age. Bone Marrow Transplant 53, 983–992 (2018). https://doi.org/10.1038/s41409-018-0104-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-018-0104-x
This article is cited by
-
Ambulatory blood pressure monitoring in children and adolescents post-hematopoietic stem cell transplantation
Pediatric Nephrology (2024)
-
Nephrotoxische Chemotherapie in der Kindheit erhöht das Risiko für eine chronische Nierenerkrankung
Die Nephrologie (2023)
-
Masked Hypertension in Healthy Children and Adolescents: Who Should Be Screened?
Current Hypertension Reports (2023)
-
Preventing the adverse cardiovascular consequences of allogeneic stem cell transplantation with a multi-faceted exercise intervention: the ALLO-Active trial protocol
BMC Cancer (2022)
-
Heart Transplant, Kawasaki Disease, and Bone Marrow Transplant: Are There Consequences?
Current Atherosclerosis Reports (2022)