Abstract
Background/Objectives
Undernutrition is a frequent condition among hospitalized patients, with a significant impact on patient’s outcome and hospital costs. Whether undernutrition is reported similarly at the national level has seldom been assessed. We aimed to (1) assess regional differences within Switzerland regarding undernutrition prevalence, management, and cost reimbursement and (2) identify the factors associated with reporting of undernutrition status and its management.
Subjects/Methods
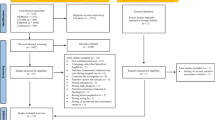
Observational cross-sectional study including routine statistics from the Swiss hospital discharge databases for years 2013 and 2014 (seven administrative regions). All adults aged ≥20 with length of hospital stay of at least 1 day was included. Reported undernutrition was defined based on the International Classification of Diseases (ICD)-10 codes. Nutritional management and “reimbursable” undernutrition codes were also assessed.
Results
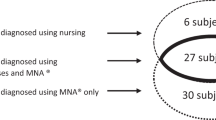
Of the initial 1,784,855 hospitalizations, 3.6% had reported undernutrition, the prevalence ranging between 1.8% (Ticino) and 4.6% (Mittelland). Use of different undernutrition-related ICD-10 codes also varied considerably across regions. Multivariable analysis showed a twofold variation in reported undernutrition: multivariable-adjusted odds ratio and 95% confidence interval relative to Eastern Switzerland: 2.31 (2.23, 2.38) for Mittelland and 0.74 (0.70, 0.79) for Ticino. Over half (59.6%) of hospitalizations with reported undernutrition also included information on undernutrition management, ranging between 28.6% (Ticino) and 67.2% (Zürich). Only one third (36.8%) of undernutrition-related codes were reimbursable, ranging between 8.3% (Ticino) and 50.7% (Zürich).
Conclusions
In Switzerland, there is considerable regional variation regarding reporting of undernutrition prevalence, management, and cost reimbursement. Undernutrition appears to be insufficiently managed and valued.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Imoberdorf R, Meier R, Krebs P, Hangartner PJ, Hess B, Staubli M, et al. Prevalence of undernutrition on admission to Swiss hospitals. Clin Nutr. 2010;29:38–41.
Beck AM, Balknas UN, Camilo ME, Furst P, Gentile MG, Hasunen K, et al. Practices in relation to nutritional care and support--report from the Council of Europe. Clin Nutr. 2002;21:351–4.
Sorensen J, Kondrup J, Prokopowicz J, Schiesser M, Krähenbühl L, Meier R, et al. EuroOOPS: an international, multicentre study to implement nutritional risk screening and evaluate clinical outcome. Clin Nutr. 2008;27:340–9.
Kruizenga H, van Keeken S, Weijs P, Bastiaanse L, Beijer S, Huisman-de Waal G, et al. Undernutrition screening survey in 564,063 patients: patients with a positive undernutrition screening score stay in hospital 1.4 d longer. Am J Clin Nutr. 2016;103:1026–32.
Meijers JMM, JMGA Schols, vanBokhorst-de van der Schueren MAE, Dassen T, Janssen MAP, Halfens RJG. Malnutrition prevalence in The Netherlands: results of the Annual Dutch National Prevalence Measurement of Care Problems. Br J Nutr. 2008;101:417–23.
Corkins MR, Guenter P, DiMaria-Ghalili RA, Jensen GL, Malone A, Miller S, et al. Malnutrition diagnoses in hospitalized patients: United States, 2010. J Parenter Enter Nutr. 2014;38:186–95.
Russell CA, Elia M. Nutrition Screening Survey in the UK and Republic of Ireland in 2010. A report by BAPEN. 2011.
Khalatbari-Soltani S, Marques-Vidal P. The economic cost of hospital malnutrition in Europe; a narrative review. Clin Nutr Espen. 2015;10:e89–e94.
Marques-Vidal P, Khalatbari-Soltani S, Sahli S, Coti Bertrand P, Pralong F, Waeber G. Undernutrition is associated with increased financial losses in hospitals. Clin Nutr. 2018;37:681–6.
Giannopoulos GA, Merriman LR, Rumsey A, Zwiebel DS. Malnutrition coding 101: financial impact and more. Nutr Clin Pract. 2013;28:698–709.
Herzlinger RE, Richman BD, Boxer RJ. Achieving universal coverage without turning to a single payer: lessons from 3 other countries. JAMA. 2017;317:1409–10.
Vonzun N, Sterchi AB, Imoberdorf R, Rühlin M. Mangelernährung und DRG – Die Schweizer Lösung. Aktuel- Ernahr. 2014;39:392–6.
Khalatbari-Soltani S, Marques-Vidal P. Impact of nutritional risk screening in hospitalized patients on management, outcome and costs: a retrospective study. Clin Nutr. 2016;35:1340–6.
Insam C, Paccaud F, Marques-Vidal P. The region makes the difference: disparities in management of acute myocardial infarction within Switzerland. Eur J Prev Cardiol. 2014;21:541–8.
Sundararajan V, Quan H, Halfon P, Fushimi K, Luthi JC, Burnand B, et al. Cross-national comparative performance of three versions of the ICD-10 Charlson index. Med Care. 2007;45:1210–5.
Guenter P, Jensen G, Patel V, Miller S, Mogensen KM, Malone A, et al. Addressing disease-related malnutrition in hospitalized patients: a call for a National Goal. Jt Comm J Qual Patient Saf. 2015;41:469–73.
Elia M, Russell CA, Stratton RJ. Malnutrition in the UK: policies to address the problem. Proc Nutr Soc. 2010;69:470–6.
Fisch T, Pury P, Probst N, Bordoni A, Bouchardy C, Frick H, et al. Variation in survival after diagnosis of breast cancer in Switzerland. Ann Oncol. 2005;16:1882–8.
Waitzberg DL, Caiaffa WT. Correia MITD. Hospital malnutrition: the Brazilian national survey (IBRANUTRI): a study of 4000 patients. Nutrition. 2001;17:573–80.
Scrimshaw NS, SanGiovanni JP. Synergism of nutrition, infection, and immunity: an overview. Am J Clin Nutr. 1997;66:464s–77s.
Schneider SM, Veyres P, Pivot X, Soummer AM, Jambou P, Filippi J, et al. Malnutrition is an independent factor associated with nosocomial infections. Br J Nutr. 2004;92:105–11.
Hébuterne X, Lemarié E, Michallet M, de Montreuil CB, Schneider SM, Goldwasser F. Prevalence of malnutrition and current use of nutrition support in patients with cancer. J Parenter Enter Nutr. 2014;38:196–204.
Brisbois TD, Hutton JL, Baracos VE, Wismer WV. Taste and smell abnormalities as an independent cause of failure of food intake in patients with advanced cancer--an argument for the application of sensory science. J Palliat Care. 2006;22:111–4.
Jie B, Jiang ZM, Nolan MT, Efron DT, Zhu SN, Yu K, et al. Impact of nutritional support on clinical outcome in patients at nutritional risk: a multicenter, prospective cohort study in Baltimore and Beijing teaching hospitals. Nutrition. 2010;26:1088–93.
Bounoure L, Gomes F, Stanga Z, Keller U, Meier R, Ballmer P, et al. Detection and treatment of medical in patients with or at-risk of malnutrition: Suggested procedures based on validated guidelines. Nutrition. 2016;32:790–8.
Ess S, Savidan A, Frick H, Rageth C, Vlastos G, Lütolf U, et al. Geographic variation in breast cancer care in Switzerland. Cancer Epidemiol. 2010;34:116–21.
Schindler K, Pernicka E, Laviano A, Howard P, Schutz T, Bauer P, et al. How nutritional risk is assessed and managed in European hospitals: a survey of 21,007 patients findings from the 2007-2008 cross-sectional nutritionDay survey. Clin Nutr. 2010;29:552–9.
Weiss V, Heinemann S, Himmel W, Nau R, Hummers-Pradier E. [The use of benzodiazepines and Z-drugs for patients with sleeping problems - A survey among hospital doctors and nurses]. Dtsch Med Wochenschr. 2016;141:e121–6.
Funk KL, Ayton CM. Improving malnutrition documentation enhances reimbursement. J Am Diet Assoc. 1995;95:468–75.
Cederholm T, Bosaeus I, Barazzoni R, Bauer J, Van Gossum A, Klek S, et al. Diagnostic criteria for malnutrition - An ESPEN Consensus Statement. Clin Nutr. 2015;34:335–40.
Author contributions
S.K.-S and P.M.-V. conceived the paper. S.K.-S. analyzed data and wrote the manuscript. P.M.-V. supervised the analysis, and had primary responsibility for final content. G.W. and C.d.M. reviewed the manuscript and provided critical recommendations. All authors have read and approved the final manuscript.
Funding
Saman Khalatbari-Soltani is supported by a Swiss Excellence Government scholarship awarded by Swiss Confederation [Ref No. 2014.0739]. Carlos de Mestral is supported by the Swiss National Science Foundation [PNR69 Ref No. 406940_145187]. The funding source had no involvement in the study design, data collection, analysis and interpretation, writing of the report, or decision to submit the article for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Khalatbari-Soltani, S., de Mestral, C., Waeber, G. et al. Large regional disparities in prevalence, management and reimbursement of hospital undernutrition. Eur J Clin Nutr 73, 121–131 (2019). https://doi.org/10.1038/s41430-018-0149-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-018-0149-3
This article is cited by
-
May nutritional status worsen during hospital stay? A sub-group analysis from a cross-sectional study
Internal and Emergency Medicine (2019)