Abstract
Objective: To investigate effects of growth and food intake in infancy on iron status at the age of 12 months in a population with high birth weight and high frequency of breast-feeding.
Design: In a longitudinal observational study infants' consumption and growth were recorded. Weighed 2 day food records at the ages of 6, 9 and 12 months were used to analyse food and nutrient intake.
Setting: Healthy-born participants were recruited from four maternity wards. Blood samples and growth data were collected from healthcare centres and food consumption data at home.
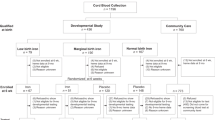
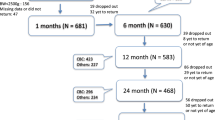
Subjects: Newborn infants (n=180) were selected randomly according to the mother's domicile and 77% (n=138) participated, of them, 83% (n=114), or 63% of original sample, came in for blood sampling.
Results: Every fifth child was iron-deficient (serum ferritin<12 µg/l and mean corpuscular volume<74 fl) and 2.7% were also anaemic (Hb<105 g/l). Higher weight gain from 0 to 12 months was seen in infants who were iron-deficient at 12 months (6.7±0.9 kg) than in non-iron-deficient infants (6.2±0.9 kg) (P=0.050). Serum transferrin receptors at 12 months were positively associated with length gain from 0 to 12 months (adjusted r2=0.14; P=0.045) and mean corpuscular volume negatively to ponderal index at birth (adjusted r2=0.14; P=0.019) and 12 months (adjusted r2=0.17; P=0.006). Iron-deficient infants had shorter breast-feeding duration (5.3±2.2 months) than non-iron-deficient (7.9±3.2 months; P=0.001). Iron status indices were negatively associated with cow's milk consumption at 9–12 months, significant above 460 g/day, but were positively associated with iron-fortified breakfast cereals, fish and meat consumption.
Conclusions: In a population of high birth weight, iron deficiency at 12 months is associated with faster growth and shorter breast-feeding duration from 0 to 12 months of age. The results suggest that a diet of 9–12-month-olds should avoid cow's milk above 500 g/day and include fish, meat and iron-fortified breakfast cereals to improve iron status.
Sponsorship: The Icelandic Research Council, Research Fund of the University of Iceland.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Asobayire, FS, Adou, P, Davidsson, L, Cook, JD & Hurrell, RF (2001). Prevalence of iron deficiency with and without concurrent anemia in population groups with high prevalences of malaria and other infections: a study in Cote d'Ivoire. Am. J. Clin. Nutr., 74, 776–782.
Atladottir, H & Thorsdottir, I (2000). Energy intake and growth of infants in Iceland—a population with high frequency of breast-feeding and high birth weight. Eur. J. Clin. Nutr., 54, 695–701.
Birgisdottir, BE, Gunnarsdottir, I, Thorsdottir, I, Gudnason, V & Benediktsson, R (2002). Size at birth and glucose intolerance in a high birth weight population. >Am. J. Clin. Nutr., 76, 399–403.
Black, AE, Cole, TJ, Wiles, SJ & White, F (1983). Daily variation in food intake of infants from 2 to 18 months. Hum. Nutr. Appl. Nutr., 37, 448–458.
Bougle, D, Laroche, D & Bureau, F (2000). Zinc and iron status and growth in healthy infants. Eur. J. Clin. Nutr., 54, 764–767.
British Nutrition Foundation (1995). Iron and mental and motor behaviour in childhood. In:Iron: Nutritional and Physiological Significance. The Report of the British Nutrition Foundation Task Force, pp65–78, London: Chapman & Hall
Cook, JD, Dassenko, SA & Whittaker, P (1991). Calcium supplementation: effect on iron absorption. Am. J. Clin. Nutr., 53, 106–111.
Dallman, PR, Siimes, MA & Stekel, A (1980). Iron deficiency in infancy and childhood. Am. J. Clin. Nutr., 33, 86–118.
Department of Health (1994). Weaning and the Weaning Diet, Report on health and social subjects, no. 45 London: HMSO
Domellof, M, Lonnerdal, B, Dewey, KG, Cohen, RJ, Rivera, LL & Hernell, O (2002). Sex differences in iron status during infancy. Pediatrics, 110, 545–552.
Duncan, B, Schifman, RB, Corrigan, JJ Jr & Schaefer, C (1985). Iron and the exclusively breast-fed infant from birth to six months. J. Pediatr. Gastroenterol. Nutr., 4, 421–425.
Engelmann, MD, Davidsson, L, Sandstrom, B, Walczyk, T, Hurrell, RF & Michaelsen, KF (1998a). The influence of meat on nonheme iron absorption in infants. Pediatr. Res., 43, 768–773.
Engelmann, MD, Sandstrom, B & Michaelsen, KF (1998b). Meat intake and iron status in late infancy: an intervention study. J. Pediatr. Gastroenterol. Nutr., 26, 26–33.
Fairweather-Tait, SJ (1992). Iron deficiency in infancy; easy to prevent—or is it?. Eur. J. Clin. Nutr., 46, S9–14.
Freeman, VE, Mulder, J, van't Hof, MA, Hoey, HM & Gibney, MJ (1998). A longitudinal study of iron status in children at 12, 24 and 36 months. Public Health Nutr., 1, 93–100.
Fuchs, GJ, Farris, RP, DeWier, M, Hutchinson, SW, Warrier, R, Doucet, H & Suskind, RM (1993). Iron status and intake of older infants fed formula vs cow milk with cereal. Am. J. Clin. Nutr., 58, 343–348.
Gibson, SA (1999). Iron intake and iron status of preschool children: associations with breakfast cereals, vitamin C and meat. Public Health Nutr., 2, 521–528.
Gill, DG, Vincent, S & Segal, DS (1997). Follow-on formula in the prevention of iron deficiency: a multicentre study. Acta Paediatr., 86, 683–689.
Hallberg, L, Brune, M & Rossander-Hulthen, L (1987). Is there a physiological role of vitamin C in iron absorption?. Ann. NY Acad. Sci., 498, 324–332.
Hallberg, L, Brune, M, Erlandsson, M, Sandberg, AS & Rossander-Hulten, L (1991). Calcium: effect of different amounts on nonheme- and heme-iron absorption in humans. Am. J. Clin. Nutr., 53, 112–119.
Idjradinata, P & Pollitt, E (1993). Reversal of developmental delays in iron-deficient anaemic infants treated with iron. Lancet, 341, 1–4.
INACG (International Nutritional Anemia Consultative Group), WHO, UNICEF (1998). Guidelines for the use of Iron Supplements to Prevent and Treat Iron Deficiency Anemia, Washington, DC: Ilsi Press
Lawson, MS, Thomas, M & Hardiman, A (1998). Iron status of Asian children aged 2 years living in England. Arch. Dis. Child., 78, 420–426.
Lozoff, B, Brittenham, GM, Wolf, AW, McClish, DK, Kuhnert, PM, Jimenez, E, Jimenez, R, Mora, LA, Gomez, I & Krauskoph, D (1987). Iron deficiency anemia and iron therapy effects on infant developmental test performance. Pediatrics, 79, 981–995.
Lozoff, B, Jimenez, E, Hagen, J, Mollen, E & Wolf, AW (2000). Poorer behavioral and developmental outcome more than 10 years after treatment for iron deficiency in infancy. Pediatrics, 105, E51
Male, C, Persson, LA, Freeman, V, Guerra, A, van't Hof, MA & Haschke, F (2001). Prevalence of iron deficiency in 12-mo-old infants from 11 European areas and influence of dietary factors on iron status (Euro-Growth study). Acta Paediatr., 90, 492–498.
Michaelsen, KF, Milman, N & Samuelson, G (1995). A longitudinal study of iron status in healthy Danish infants: effects of early iron status, growth velocity and dietary factors. Acta Paediatr., 84, 1035–1044.
Mills, AF (1990). Surveillance for anaemia: risk factors in patterns of milk intake. Arch. Dis. Child., 65, 428–431.
Morton, RE, Nysenbaum, A & Price, K (1988). Iron status in the first year of life. J. Pediatr. Gastroenterol. Nutr., 7, 707–712.
Nielsen, GA, Thomsen, BL & Michaelsen, KF (1998). Influence of breastfeeding and complementary food on growth between 5 and 10 months. Acta Paediatr., 87, 911–917.
Nokes, C, van den Bosch, C & Bundy, DAB (1998). The Effects of Iron Deficiency and Anemia on Mental and Motor Performance, Educational Achievement, and Behavior in Children: an Annotated Bibliography, International Nutritional Anemia Consultative Group (INACG) publication
Nordic Experts on Nutrition (1996). [Nordic Nutrition Recommendations], Nordic Council of Ministers. Copenhagen: AKA-Print
Oti-Boateng, P, Seshadri, R, Petrick, S, Gibson, RA & Simmer, K (1998). Iron status and dietary iron intake of 6–24-month-old children in Adelaide. J. Paediatr. Child Health, 34, 250–253.
Palsson, G, Sigurdsson, JA & Gudbjornsdottir, H (1996). [Health Care of Infants], Directorate of Health. Reykjavik: Oddi Ltd
Persson, LA, Lundstrom, M, Lonnerdal, B & Hernell, O (1998). Are weaning foods causing impaired iron and zinc status in 1-year-old Swedish infants? A cohort study. Acta Paediatr., 87, 618–622.
Pizarro, F, Yip, R, Dallman, PR, Olivares, M, Hertrampf, E & Walter, T (1991). Iron status with different infant feeding regimens: relevance to screening and prevention of iron deficiency. J. Pediatr., 118, 687–692.
Punnonen, K, Irjala, K & Rajamaki, A (1997). Serum transferrin receptor and its ratio to serum ferritin in the diagnosis of iron deficiency. Blood, 89, 1052–1057.
Reddy, MB & Cook, JD (1997). Effect of calcium intake on nonheme-iron absorption from a complete diet. Am. J. Clin. Nutr., 65, 1820–1825.
Sherriff, A, Emond, A, Hawkins, N & Golding, J (1999). Haemoglobin and ferritin concentrations in children aged 12 and 18 months. ALSPAC Children in Focus Study Team. Arch. Dis. Child., 80, 153–157.
Siimes, MA, Salmenpera, L & Perheentupa, J (1984). Exclusive breast- feeding for 9 months: risk of iron deficiency. J. Pediatr., 104, 196–199.
Skikne, BS, Flowers, CH & Cook, JD (1990). Serum transferrin receptor: a quantitative measure of tissue iron deficiency. Blood, 75, 1870–1876.
Solomons, NW & Ruz, M (1997). Zinc and iron interaction: concepts and perspectives in the developing world. Nutr. Res., 17, 177–185.
Steingrimsdottir, L (1995). [Infant Diet], Icelandic Nutrition Council. Reykjavik: Isafold Ltd
Stevens, D & Nelson, A (1995). The effect of iron in formula milk after 6 months of age. Arch. Dis. Child., 73, 216–220.
Thane, CW, Walmsley, CM, Bales, CJ, Prentice, A & Cole, TJ (2000). Risk factors for poor iron status in British toddlers: further analysis of data from the National Diet and Nutrition Survey of children aged 1.5–4.5 years. Public Health Nutr., 3, 433–440.
Thorsdottir, I & Birgisdottir, BE (1998). Different weight gain in women of normal weight before pregnancy: postpartum weight and birth weight. Obstet. Gynecol., 92, 377–383.
Thorsdottir, I, Birgisdottir, BE, Johannsdottir, IM, Harris, DP, Hill, J, Steingrimsdottir, L & Thorsson, AV (2000). Different beta-casein fractions in Icelandic versus Scandinavian cow's milk may influence diabetogenicity of cow's milk in infancy and explain low incidence of insulin-dependent diabetes mellitus in Iceland. Pediatrics, 106, 719–724.
Tunnessen, WW Jr & Oski, FA (1987). Consequences of starting whole cow milk at 6 months of age. J. Pediatr., 111, 813–816.
Walter, T, Dallman, PR, Pizarro, F, Velozo, L, Pena, G, Bartholmey, SJ, Hertrampf, E, Olivares, M, Letelier, A & Arredondo, M (1993). Effectiveness of iron-fortified infant cereal in prevention of iron deficiency anemia. Pediatrics, 91, 976–982.
Wharf, SG, Fox, TE, Fairweather-Tait, SJ & Cook, JD (1997). Factors affecting iron stores in infants 4–18 months of age. Eur. J. Clin. Nutr., 51, 504–509.
WHO (2001). Iron Deficiency Anaemia. Assessment, Prevention and Control. A Guide for Programme Managers, WHO/NHD/01.3 Geneva: WHO
Acknowledgements
We thank the staff in the laboratories at Landspitali University Hospital in Reykjavik, Iceland and the Research Department of Human Nutrition (FHE) at the Royal Veterinary and Agricultural University in Copenhagen, Denmark.
Author information
Authors and Affiliations
Contributions
Guarantor: I Thorsdottir.
Contributors: IT was project leader and made the greatest contribution to this paper. BSG worked on the calculations and statistical analysis and assisted with the writing of the paper. HA worked on the data collection in the infant dietary survey. KFM participated in the project planning and administered the analysis of ferritin and transferrin receptors. GP participated in the project planning and took care of all blood sampling.
Corresponding author
Rights and permissions
About this article
Cite this article
Thorsdottir, I., Gunnarsson, B., Atladottir, H. et al. Iron status at 12 months of age — effects of body size, growth and diet in a population with high birth weight. Eur J Clin Nutr 57, 505–513 (2003). https://doi.org/10.1038/sj.ejcn.1601594
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1601594
Keywords
This article is cited by
-
Multivariate linear mixture models for the prediction of febrile seizure risk and recurrence: a prospective case–control study
Scientific Reports (2023)
-
Rapid increase in the body mass index of very preterm infants is a risk factor for iron deficiency during infancy
Scientific Reports (2023)
-
Child linear growth trajectories during the first three years of life in relation to infant iron status: a prospective cohort study in rural Vietnam
BMC Nutrition (2022)
-
Impact and interactions between risk factors on the iron status of at-risk neonates
Journal of Perinatology (2022)
-
Prevalence and associated factors of iron deficiency in Spanish children aged 1 to 11 years
European Journal of Pediatrics (2021)