Abstract
Study design: Experimental animal model to assess ischemic spinal cord injury following occlusion of the thoraco-abdominal aorta.
Objectives: To measure whether melatonin administered to rabbits before and after occlusion exerts an effect on the repair of ischemia–reperfusion (IR) injury.
Setting: Medical Biology Laboratory, Inonu University, Malatya, Turkey
Methods: Rabbits were divided into three IR treatment groups and one sham-operated (ShOp) control group. The three treatment groups had their infrarenal aorta temporarily occluded for 25 min, while the ShOp group had laparotomy without aortic occlusion. Melatonin was administered either 10 min before aortic occlusion or 10 min after the clamp was removed. Physiologic saline was administered to the control animals. After treatment, the animals were euthanized and lumbosacral spinal cord tissue was removed for the determination of relevant enzyme activities.
Results: Malondialdehyde levels, indicating the extent of lipid peroxidation, were found to be significantly increased in the nonmelatonin treated (IR) group when compared to the ShOp group. Melatonin, whether given to pre- or post occlusion groups, suppressed malondialdehyde levels below that of the ShOp group. Catalase (CAT) and glutathione peroxidase (GSH-Px) enzyme activities were increased in the IR group compared to the ShOp group. Melatonin given preocclusion resulted in a significant decrease in both CAT and GSH-Px enzyme levels. The superoxide dismutase (SOD) enzyme activity was decreased in the ischemia–reperfusion treatment group. However, the melatonin treatment increased SOD enzyme activity to levels approximating that of the ShOp group.
Conclusion: To our knowledge, this is the first study that shows the effects of melatonin administered both pre- and postischemia on induced oxidative damage to injured spinal cords. Our data also expands on reports that melatonin administration may significantly reduce the incidence of spinal cord injury following temporary aortic occlusion.
Similar content being viewed by others
Introduction
Experimental models and clinical observations of acute spinal cord injury support the concepts of primary and secondary injury in which the initial mechanical insult is followed by a series of deleterious events that promote progressive tissue damage and ischemia. Whereas the fate of the primary injury depends upon the circumstances of the trauma, the outcome of the secondary injury may be amenable to therapeutic modulation. The extent of lipid peroxidation is a useful parameter for evaluating the cellular disturbances caused by spinal cord injury caused by ischemia/reperfusion (IR) in experimental conditions.1,2,3,4,5,6,7,8,9,10
Free oxygen radicals have been implicated in postischemic cell injury and cellular death, while free radical scavengers such as superoxide dismutase (SOD) and catalase (CAT) are associated with an amelioration of ischemic injury.11 To prevent such damage, a variety of biological defense systems are activated in normal cells. Among these, the enzymes superoxide dismutase (SOD, EC 1.15.1.1), catalase (CAT, EC 1.11.1.6), and glutathione peroxidase (GSH-Px, EC 1.11.1.9) are the best-known components of the biological protective system.12,13,14,15 It is recognized that these enzymes may be important protectors against lipid peroxidation and damage due to free radicals after the onset of neuronal ischemia.
Melatonin, which is considered to be an antioxidant agent for free oxygen radicals, has been reported to have a role in the treatment of a variety of cerebral pathologies including ischemia, vasospasm and brain edema in experimental settings.10,16,17,18
However, there are conflicting reports concerning melatonin's scavenging activity on superoxide anions.11 The results presented here indicate that melatonin is effective in preventing secondary damage due to peroxidation of lipid membranes in the ischemic spinal cord. Melatonin treatment promotes a significant increase in protective enzyme levels and may have a potential role in an alternative treatment for spinal cord ischemia.
Materials and methods
General animal care and surgery
This study was performed in the Medical Biology Research laboratory of Inonu University, Faculty of Medicine. The experimental protocol was evaluated and approved by the Ethics Review Committee of Inonu University, Faculty of Medicine, prior to the study. In total, 32 adult male New Zealand rabbits weighing 2.8–3.5 kg were used. The animals were kept at optimal (18–21°C) room temperature and fed a standard diet (Oguzlar Yem Sanayi Eskisehir, Turkey). A 12 h light–dark cycle (8:00 am–8:00 pm light/ 8:01 pm–7:59 am dark) was implemented. Free access to food and water was allowed.
The animals were anesthetized by intramuscular (i.m.) injection of ketamine (70 mg/kg) (Ketalar, Parke-Davis, Eczacibasi, Istanbul, Turkey) and xylazine (5 mg/kg) (Rompun, Bayer, Istanbul, Turkey) and allowed to breathe spontaneously. Additional doses were occasionally required during the surgery. Body temperatures were measured by rectal thermometry and maintained at 37°C with a pad and heating lamp. The arterial pressure, heart rate and arterial blood gases were monitored continuously. pO2, pCO2 and pH were determined to be normal during surgery.
Melatonin preparation
Melatonin (Sigma, St Louis, MO, USA) was dissolved in a minimum volume of ethanol (0.5 ml) and diluted to the desired concentration with physiological saline.
Ischemia–reperfusion procedure
The spinal cord ischemia model described by Zivin and DeGirolami19 was used in this study. Briefly, the thoraco-abdominal aorta was clamped by a ‘Bulldog’ atraumatic infantile vascular compression clamp approximately 1 cm below the renal artery. The location of the clamping corresponds to the L3 vertebrae of the animal. Experimental animals were subjected to 25 min of cross clamp time. At the end of the occlusion period, the clamp was removed and restoration of blood flow was visually verified. For the control study, the ShOp group was subjected to only laparotomy without aortic compression.
Setting of groups and melatonin administration
In total, 32 rabbits were divided into three treatment groups and one control group. The control group containing eight rabbits was ShOp. The second group of eight animals was subjected to IR by clamping the thoraco-abdominal aorta for 25 min. Each rabbit in the IR group received an equivalent dose of aqueous-buffered saline administered intraperitoneally (i.p.) 10 min after the clamp was removed. Another eight rabbits in the Pre-IR group were given 10.0 mg/kg melatonin i.p. 10 min before the aorta was clamped for ischemia and reperfusion.7,20 The remaining eight rabbits (Post-IR group) were given 10.0 mg/kg melatonin IP 10 min after the aortic clamp was removed.
Sacrificing of animals and sample preparation
Rabbits were killed by ketamine overdose after reperfusion. Intra-arterial perfusion was performed with a left ventricular cannula while the right atrium was opened widely. During the perfusion, circulating blood was washed out with 500 ml physiological saline under 110 cmH2O pressure. The lumbosacral cords between L4-S1 were immediately removed. The tissues were collected under a surgical microscope at × 400 magnification using a × 16 ocular and a × 25 objective (OPMI-99 microscope, Carl Zeiss Inc. Germany). Spinal cord samples were, labeled as group1A, 1B, etc to 4A, 4B, etc for coded blind biochemical studies, placed in liquid nitrogen immediately and then transported to the laboratory for measurement of antioxidant enzyme activities and lipid peroxidation levels. Spinal cord tissue samples were divided into four equal parts for homogenization. An Ultra-Turrax homogenizer (model T25, Janke and Kunkel, Germany) 9500 rpm (4 × 10 s at 4°C) was used. The homogenates were centrifuged at 1000 g for 10 min and supernatants were collected. The first part was homogenized in a ratio of one part wet tissue to 9 ml of cold 1.15% KCl. From this 1:9 homogenate, 0.5 ml was used for the MDA assay. The remaining three parts were homogenized as above (1:9) but with the addition of 0.02 M potassium phosphate (pH 7.0) as a buffer. The buffered homogenate was equally divided for CAT, SOD and GSH-Px activity determination. Chemicals were purchased from Sigma Chemical Co. (St Louis, MO, USA) unless otherwise stated.
Measurement of MDA levels and antioxidant enzyme activities
Malonaldehyde
Malonaldehyde levels were measured spectrophotometrically by the method of Uchiyama and Mihara,21 which follows changes in malonaldehyde precursors in tissue through use of the thiobarbituric acid (TBA) test. To 0.5 ml of tissue homogenate, 3 ml of 1% H3PO4 and 1 ml 0.6% TBA aqueous solution was added, stirred and heated in a boiling water bath for 45 min. After cooling, 4 ml of n-butanol was added and the mixture was shaken. The butanol layer was separated by centrifugation and the absorbance of the butanol layer was measured spectrophotometrically at 535 and 520 nm. The difference between the two optical densities was a measure of the TBA value. Results are expressed as nmol per gram wet weight (nmol/gww).
Superoxide dismutase
SOD enzyme activity was measured by the indirect spectrophotometric assay described by McCord and Fridovich.23 SOD catalyzes the dismutation of superoxide radicals. SOD activity was determined in the supernatant using its inhibitory action on the superoxide-dependent reduction of cytocrome c by a xanthine/xanthine oxidase mixture. In a total volume of 1.1 ml, the reaction mixture contained phosphate buffer (20 mM, pH 7.0), 0.1 M EDTA, 50 μM xanthine and 10 μM cytocrome c. The reaction was initiated by adding xanthine oxidase, and the rate of cytochrome c reduction was monitored spectrophotometrically at 550 nm.
Catalase
CAT activity was measured spectrophotometrically by the method of Luck.24 Samples were diluted 1:10 in cold potassium dihydrogen phosphate buffer (pH 7.0) incubated with occasional shaking for 10 min at 4°C and centrifuged, followed by a repeated extraction. Supernatants were combined, and 0.04 ml was added into 3 ml 0.01 M of H2O2-phosphate buffer, mixed well, and read on a spectrophotometer containing a constant temperature unit attachment. Blank readings were performed in a control cuvette that included enzyme solution as in the experimental sample but with H2O2-free phosphate buffer. Decreases in absorbance measurements at 240 nm are followed until the optical density reaches 0.450. The time (Δt) required for the optical density to reach 0.400 was recorded and used to obtain the value k from the formula 0.1175/Δt. The value k is then converted to CAT units.
Glutathione peroxidase
GSH-Px activity was measured spectrophotometrically by the method of Lawrance and Burk.25 The assay measures the oxidized glutathione formed in the GSH-Px reaction by coupling it to the oxidation of NADPH via glutathione reductase. The reaction mixture contained 50 mM potassium phosphate buffer (pH 7), 1 mM EDTA, 1 mM NaN3, 0.01 EU/ml GSSG-reductase, 1 mM GSH, 1.5 mM cumene-hydroperoxide and 0.25 mM H2O2. All ingredients were prepared fresh each time except for the enzyme. For each assay, the enzyme was added to 0.8 ml of the above mixture and allowed to incubate at room temperature before initiation of the reaction with the peroxide solution. Absorbance at 340 nm was recorded for 5 min. Enzyme activity was calculated as micromoles per minute. In blank reactions, the enzyme was replaced by water and readings were subtracted from each assay. Protein was measured by the Lowry procedure,22 using bovine serum albumin as a standard.
Statistical evaluation
The Mann–Whitney U-test was used for determining the significance of the results. Treatment differences with P-values less than 0.05 are considered significant and are represented by a single star (*) and P-values less than 0.01 are considered very significant and are represented with two stars (**). The Kruskal–Wallis nonparametric analysis of variance test (ANOVA) was used to compare inter- and intragroup variations of antioxidant enzyme activities as well as lipid peroxidation levels of the lumbosacral cord tissue. The values are given as the mean of eight duplicate measurements (16 samples per group) as well as the standard error of the mean.
Results
The clinical and physiological status of the animals did not change during the course of the study. Two deaths occurred during the ischemia procedure, and the dead rabbits were replaced with new ones to keep the numbers in each group equal.
Lipid peroxidation
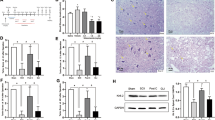
MDA levels were found to be significantly increased in the IR group compared to the ShOp, Pre-IR and Post-IR groups. However, in the Pre-IR and Post-IR groups, MDA levels did not show significant differences when compared to the ShOp group (Table 1).
Antioxidant enzyme activities
Cu–Zn SOD activity in the IR group was significantly reduced when compared to the ShOp group. Between the Post-IR and IR groups, Cu–Zn SOD enzyme activity showed significant increase. Between the Post-IR and Pre-IR groups, Cu–Zn SOD activity also had a significant decrease. However, when both groups were compared with the ShOp group, the changes were not statistically significant (Table 1).
CAT enzyme activity in the IR group showed significant increases compared with ShOp, Post-IR and the Pre-IR group. CAT enzyme activities in the Pre-IR and Post-IR group were reduced in comparison with the ShOp group. CAT enzyme activity was significantly higher in the Post-IR group than in the Pre-IR group as seen in Table 1.
GSH-Px enzyme activity in the IR group and the Post-IR group showed significant increases when compared to the ShOp group. Also, GSH-Px enzyme activity in the IR group and in the Post-IR group showed significant increases when compared to the Pre-IR group. Observed GSH-Px enzyme activity increased in the IR group when compared to the ShOp group. This is most likely due to an increase in peroxide levels in ischemic tissues. When melatonin was exogenously administered to the Pre-IR group, its protective effect on free radical production minimized the need for GSH-Px increased enzyme activity (Table 1). However, exogenous melatonin administration to the Post-IR group was not as effective as in the Pre-IR group in spite of melatonin's protective effect, and GSH-Px enzyme activity increased two and one-half-fold.
Discussion
Ischemic injury to the spinal cord, that is, vascular occlusion, global ischemia, surgical repair of aortic pathologies, coagulopathy and spinal trauma, results in cell and tissue damage.11,18,26,27,28,29,30 Free oxygen radicals can impair the function of the cellular components.14,15,31 Free oxygen radical-induced damage has been implemented in postischemic cell injury and cell death, while free radical scavengers such as SOD, CAT and GSH-Px are associated with partial amelioration of ischemic injury.4,5
The extent of lipid peroxidation is a useful parameter for evaluating cellular disturbances caused by spinal cord trauma under experimental conditions.32,33,34 The literature mentioned above outlines the biochemical basis and evidence for the occurrence of oxygen radical generation and lipid peroxidation during the acute phase of central nervous system (CNS) trauma or stroke (ischemic and hemorrhagic).
Identification of oxygen radicals and lipid peroxidation, important pathophysiological mediators of trauma or stroke-induced neural degeneration rather than simple epiphenomena, depends upon the successful demonstration of their association with actual secondary physiological and structural degenerative events. Moreover, their significance in the pathophysiology of CNS trauma or stroke must be supported by experimental observations that pharmacological antagonism of either oxygen radical generation and/or lipid peroxidation results in therapeutic effects.1,2,3,4,5,6,7,8,9,11,17,28,35,36
Work by Fujimoto et al5 showed that potent protective effects of melatonin on experimental trauma induced on rat spinal cords at T12 showed increased MDA levels after the injury. This work showed that melatonin facilitated recovery of the damaged spinal cord. As a measure of melatonin protection, Fujimoto et al determined the reduction of TBA reactive substance content. The studies presented in this paper also show the protective effects of melatonin when administered both before and after IR injury to the spinal cord as opposed to Fujimoto's use of direct physical trauma to the spinal cord.
Our results are in good agreement with those in the literature,35,36,37 indicating that increases in MDA levels are indicators of the extensiveness of the IR injury and most likely due to tissue membrane damage after IR injury.
CAT is an important scavenging enzyme against free oxygen radicals since it removes H2O2 produced during metabolic processes.10,31,38,39 In our study, observed changes in CAT activity indicate that IR-induced tissue damage could be treated with melatonin. The administration of melatonin brings CAT activity to levels even below that of the ShOp group. The amount of CAT may be critical for the protective effect against the oxidative stress under pathological conditions such as IR injury.
Protective effects of melatonin were shown by decreased SOD activity in damaged spinal cord tissues but at a smaller scale than the decreases observed in CAT activity.15 However, Nishibe showed that SOD activity is generally much lower than that of CAT activity in spinal cord tissues.40 Therefore, SOD activity changes observed due to melatonin treatment are less pronounced than those seen in CAT.14 The data reported here are in agreement with Kaynar et al,31 who found that SOD and glutathione activities were not significantly different, while CAT activity was significantly higher in traumatic spinal cord segments.
In addition to its documented free radical scavenging activity, melatonin may regulate glutathione synthesis through glutathione synthetase activation.25 On the other hand, Barlow-Walden et al16 reported that acute administration of melatonin causes a two-fold rise in GSH-Px activity in rat brain. GSH-Px is thought to be the principal enzyme eliminating peroxides in the brain. This oxidative enzyme reduces the formation of hydroxyl radicals formed via iron-catalyzed Fenton-type reactions from H2O2. Our results show statistically significant increases in GSH-Px activity in the Post-IR (ie, melatonin administrated) group versus the ShOp group, suggesting that melatonin has a free radical scavenging effect. GSH-Px activity in the cerebral cortex and hippocampus is more stable than that of SOD activity observed in the same locations.31 However, GSH-Px shows a significant decrease only at 48 h in rat brains.16 The administration of pharmacological doses of melatonin increases GSH-Px activity in the brain. Thus, our data show that both CAT and GSH-Px activities were higher in IR injury.
Barlow-Walden et al16 proposed two possible explanations for the induction of the GSH-Px activity: (1) the increase in GSH-Px activity is elicited by the antioxidative activity of melatonin, which protects the enzyme from inactivation by hydroxyl radicals and (2) an enzyme induction is mediated by changes in GSH-Px gene expression. In agreement with these theories, our studies showed that the highest levels of GSH-Px activity were in the post-IR group.
The apparent role of oxygen free radicals in ischemic neuronal damage and other types of injuries has stimulated interest in antioxidants and free radical scavengers as potential therapeutic agents.16,41 Among these, melatonin molecule is a potent-free radical scavenger.17,37 Melatonin is also a highly soluble and easily diffusible molecule. Owing to its extreme lipophilicity, it crosses morphophysiological barriers such as the blood brain barrier, cell membrane and basal membrane, diffusing into all body fluids.42 Thus, exogenous melatonin administration can provide on-site protection against free radical damage.18,43
The present study shows that antioxidant enzyme levels due to the extensive presence of free radicals in damaged tissue were significantly changed in the presence of melatonin. Changes observed in free radical scavenger enzyme concentration indicate that melatonin might have provided significant protection against the effect of the free radical damage. We suggest that the mechanisms of this protection are either (1) melatonin causing an induction of antioxidant enzyme levels or (2) melatonin acting as a free radical scavenger that lowers the need for extensive production of endogenous antioxidant enzymes. Further experiments must be carried out to determine the protective mechanism of melatonin action. In the literature, there are studies that demonstrate the protective effect of melatonin. However, in these studies, the treatment with melatonin was always administered after IR damage.17,18,37
To our knowledge, this is the first study that shows the protective effects of melatonin administration in an attempt to prevent IR induced oxidative damage on spinal cord injury before it has occurred. Our results demonstrate that prior application of melatonin can reduce damage to spinal cord IR-induced injury. The data show that spinal cord ischemia caused significant changes in the activities of endogenous antioxidants.
References
De La Torre JC . Spinal cord injury. Review of basic and applied research. Spine 1981; 6: 315–335.
Faden AI, Jacobs TP, Holaday J . Opiate antagonist improves neurologic recovery after spinal injury. Science 1981; 211: 493–494.
Faden AI, Jacobs TP, Holaday JW . Thyrotropin-releasing hormone improves recovery after spinal trauma in cats. N Engl J Med 1981; 305: 1063–1067.
Faden AI . TRH analog YM-14673 improves outcome following traumatic brain and spinal injury in rats: dose–response studies. Brain Res 1989; 486: 228–235.
Fujimoto T, Nakamura T, Ikeda T, Takagi K . Potent protective effects of melatonin on experimental spinal cord injury. Spine 2000; 25: 769–775.
Johnson SH, Kraimer JM, Graeber GM . Effects of flunarizine on neurological recovery and spinal cord blood flow in experimental spinal cord ischemia in rabbits. Stroke 1993; 24: 1547–1553.
Kasai H, Nishimura S . DNA damage induced by asbestos in the presence of hydrogen peroxide. Gann 1984; 75: 841–844.
Katircioglu SF et al. Effects of prostacyclin on spinal cord ischemia: an experimental study. Surgery 1993; 114: 36–39.
Kochar A, Zivin JA, Lyden PD, Mazzarella V . Glutamate antagonist therapy reduces neurologic deficits products by focal central nervous system. Arch Neurol 1988; 45: 148–153.
McCord JM . Oxygen-derived free radicals in post-ischemic tissue injury. N Engl J Med 1983; 312: 59–63.
Kouchoukos NL, Rokkas CK . Descending thoracic and thoraco-abdominal aortic surgery for aneurysm or dissection how do we minimize the risk of spinal cord injury? Semin Thorac Cardiovasc Surg 1993; 5: 47–54.
Cuevas P, Carceller-Benito F, Reimers D . Administration of bovine superoxide dismutase prevents sequelae of spinal cord ischemia in the rabbit. Anat Embryol 1989; 179: 251–253.
Cuevas P, Reimers D, Carceller F, Iimenez A . Ischemic reperfusion injury in rabbit spinal cord. Protective effect of superoxide dismutase on neurological recovery and spinal infarction. Acta Anat 1990; 137: 303–310.
Lim KH et al. Prevention of reperfusion injury of the ischemic spinal cord. Use of recombinant superoxide dismutase. Ann Thorac Surg 1986; 42: 282–286.
Taoka Y et al. Superoxide radicals play important roles in the pathogenesis of spinal cord injury. Paraplegia 1995; 33: 450–453.
Barlow-Walden LR et al. Melatonin stimulates brain glutathione peroxidase activity. Neurochem Int 1995; 26: 497–502.
Reiter RJ, Acuna-Castroviejo Tan DX, Burkhardt S . Free radical-mediated molecular damage. Mechanisms for the protective actions of melatonin in the central nervous system. Ann NY Acad Sci 2001; 939: 200–215.
Tan DX et al. Significance of melatonin in antioxidative defence system: reactions and products. Biol Signals Recept 2000; 9: 137–159.
Zivin JA, DeGirolami U . Spinal cord infarction. A highly reproducible stroke model. Stroke 1980; 11: 200–202.
Chen LD et al. Melatonin prevents the suppression of cardiac Ca (2+)-stimulated ATPase activity induced by alloxan. Am J Physiol 1994; 267: 57–62.
Uchiyama M, Mihara M . Determination of malonaldehyde precursor in tissues by thiobarbituric acid test. Anal Biochem 1978; 86: 271–278.
Lowry OH, Rosenbrough NJ, Farr AL, Randall RJ . Protein measurement with the Folin phenol reagent. J Biol Chem 1951; 193: 265–275.
McCord JM, Fridovich I . Superoxide dismutase. An enzymic function for erythrocuprein (Hemocuprein). J Biol Chem 1969; 244: 6049–6055.
Luck H . Catalase. In: Bergmayer HU (ed). Methods of Enzymatic Analysis. 2nd edn. Academic press: New York 1963, pp 885–888.
Lawrance RA, Burk RF . Glutathione peroxidase activity in selenium deficient rat liver. Biochem Biophys Res Commun 1976; 71: 952–958.
Connolly JE . Prevention of paraplegia secondary to operation on the aorta. J Cardiovasc Surg (Torino) 1986; 27: 410–417.
Crawford ES et al. Thoracoabdominal aortic aneurysms: preoperative and intraoperative factors determining immediate and long-term results of operations in 605 patients. J Vasc Surg 1986; 3: 389–404.
Svensson LG et al. Cross-clamping of the thoracic aorta. Influence of aortic shunts, laminectomy, papaverine, calcium channel blocker, allopurinol, and superoxide dismutase on spinal cord blood flow and paraplegia in baboon. Ann Surg 1986; 204: 38–47.
Tator CH, Fehling MG . Review of the secondary injury theory of acute spinal cord trauma with emphasis on vascular mechanisms. J Neurosurg 1991; 75: 15–26.
Verdant A et al. Surgery of the descending thoracic aorta. Spinal cord protection with the Gott shunt. Ann Thorac Surg 1988; 42: 147–154.
Kaynar MY et al. Changes in the activity of antioxidant enzymes (SOD, GPx, CAT) after experimental spinal cord injury. Tokushima J Exp Med 1988; 41: 133–136.
Barut S et al. Lipid peroxidation in experimental spinal cord injury. Time–level relationship. Neurosurg Rev 1993; 16: 53–59.
Hall ED, Braughler JM . Effects of intravenous methylprednisolone on spinal cord lipid peroxidation and (Na++ K+)-ATPase activity. J Neurosurg 1982; 57: 247–249.
Tuzgen S et al. The effect of epidural cooling on lipid peroxidation after experimental spinal cord injury. Spinal Cord 1998; 36: 654–657.
Marini CP, Conningham IN . Issues surrounding spinal cord protection. Adv Cardiac Surg 1993; 4: 89–106.
Oldfield EH, Pllinkett RJ, Nylander Jr WA, Meacham WF . Barbiturate protection in acute experimental spinal cord ischemia. J Neurosurg 1982; 56: 511–516.
Reiter RJ, Tan DX, Manchester LC . Biochemical reactivity of melatonin with reactive oxygen and nitrogen species: a review of the evidence. Cell Biochem Biophys 2001; 34: 237–256.
Scott MD, Lubin BH, Zuo L, Kuypers FA . Erythrocyte defence against hydrogen peroxide: preeminent importance of catalase. J Lab Clin Med 1991; 118: 7–16.
Slater TF . Free-radical mechanisms in tissue injury. Biochem J 1984; 222: 1–15.
Nishibe M . Experimental studies on the mechanism of spinal cord ischemia: the state of free radical scavengers. Hokkaido Igaku Zasshi 1989; 64: 301–308.
Althaus JS et al. The use of salicylate hydroxylation to detect hydroxyl radical generation in ischemic and traumatic brain injury. Mol Chem Neuropathol 1993; 20: 147–162.
Marshall KA et al. Evaluation of the antioxidant activity of melatonin in vitro. Free Radio Biol Med 1996; 21: 307–315.
Tan DX et al. The pineal hormone melatonin inhibits DNA-adduct formation induced by the chemical carcinogen safrole in vivo. Cancer Lett 1993; 70: 65–71.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Erten, S., Kocak, A., Ozdemir, I. et al. Protective effect of melatonin on experimental spinal cord ischemia. Spinal Cord 41, 533–538 (2003). https://doi.org/10.1038/sj.sc.3101508
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101508
Keywords
This article is cited by
-
The effects of apigenin administration on the inhibition of inflammatory responses and oxidative stress in the lung injury models: a systematic review and meta-analysis of preclinical evidence
Inflammopharmacology (2022)
-
Comparison of the neuroprotective effects of brimonidine tartrate and melatonin on retinal ganglion cells
International Ophthalmology (2018)
-
Melatonin Inhibits Neural Cell Apoptosis and Promotes Locomotor Recovery via Activation of the Wnt/β-Catenin Signaling Pathway After Spinal Cord Injury
Neurochemical Research (2017)
-
The effect of melatonin on spinal cord after ischemia in rats
Spinal Cord (2016)
-
Studies on protection against ischemia reperfusion injury after SCI
Spinal Cord (2016)