-
PDF
- Split View
-
Views
-
Cite
Cite
Brenda Eskenazi, Amy R. Marks, Ralph Catalano, Tim Bruckner, Paolo G. Toniolo, Low birthweight in New York city and upstate New York following the events of September 11th, Human Reproduction, Volume 22, Issue 11, November 2007, Pages 3013–3020, https://doi.org/10.1093/humrep/dem301
Close - Share Icon Share
Abstract
We examined pregnancy outcomes in New York City (NYC) and upstate New York after the September 11, 2001 World Trade Center disaster.
Using birth certificate data for NY residents (n = 1660,401 births), we estimated risk of low birthweight (LBW: <2500 g) and preterm birth (<37 weeks) one week after September 11th versus three weeks before, and for 10 four-week intervals post-disaster versus these intervals in the two previous years. To corroborate regression results, we used time-series analysis.
One week after September 11th in NYC, we observed an adjusted odds of 1.44 for births <1500 g (P = 0.07) and 1.67 for births 1500–1999 g (P = 0.01), but a decreased odds of 2000–2499 g. We found no immediate change in LBW upstate or preterm in either location. In extended analyses, we found, in both locations, increased odds of <1500-g births around New Year and 33–36 weeks post-disaster and decreased odds of moderate preterm for several weeks post-disaster. Time-series analyses yielded similar findings.
The events of September 11, 2001 in NYC were associated with immediate increases in births <2000 g, slightly delayed decreased preterm delivery, and delayed increases in LBW among infants exposed periconception or in the first two trimesters. Stress may contribute to observed associations.
Introduction
The September 11, 2001 terrorist attack on New York City's (NYC) World Trade Center (WTC) resulted in substantial loss of life, widespread social and economic disruption (U.S. Department of Labor Bureau of Labor Statistics, 2004), and lingering fears of future attacks. The disaster's health impact extended beyond the plumes of contaminated smoke and dust emitted from the WTC (Lioy et al., 2002; Landrigan et al., 2004; Wolff et al., 2005). Several studies report extensive psychological sequelae (Schuster et al., 2001; Galea et al., 2002; Schlenger et al., 2002; DeLisi et al., 2003; Pulcino et al., 2003). In a nationally representative sample of adults interviewed soon after September 11th, 44% reported stress-related symptoms (Schuster et al., 2001). Months afterwards, post-traumatic stress (PTS) prevalence was higher in NYC (11.2%) than anywhere in the USA (Schlenger et al., 2002), particularly among women (Pulcino et al., 2003).
The American College of Obstetrics and Gynecology (2001) cautioned that pregnant women might be particularly vulnerable to the event's impact. Research on the effects of acute stressors find higher risk of preterm labor immediately following earthquakes (Weissman et al., 1989; Salinas et al., 1998) and of preterm and very low birthweight (VLBW: <1500 g) deliveries months after widespread community bereavement, such as from a political assassination and man-made or natural disasters (Catalano and Hartig, 2001; Glynn et al., 2001).
Mechanistic studies indicate that timing of parturition may be influenced by stress (McLean et al., 1995; Hobel et al., 1999; Lockwood, 1999). The stress response in pregnancy involves both the maternal hypothalamic–pituitary–adrenal axis and sympathetic nervous system and their interaction with the fetal unit (Mancuso et al., 2004). Maternal stress results in changes in adrenal cortisol, norepinephrine and epinephrine, which stimulate the production of placental corticotropin-releasing hormone (CRH) (Mancuso et al., 2004). CRH increases naturally over the course of gestation and appears to be related to the timing of parturition (Lockwood, 1999). Women delivering prematurely have higher plasma CRH as early as 18 weeks gestation (Hobel et al., 1999; Mancuso et al., 2004). Complex physiological changes lead to dampened physiological and psychological stress response as pregnancy progresses (de Weerth and Buitelaar, 2005), leading some to suggest that stress exposures later in pregnancy may be less likely to initiate parturition (Glynn et al., 2001; Hobel, 2004). Others have found later stress to be more critical (Hedegaard et al., 1993; Catalano and Hartig, 2001). Stress may also impact the immune system (Herbert and Cohen, 1993) or result in maladaptive coping behaviors such as smoking and alcohol use (Paarlberg et al., 1999), which may in turn affect pregnancy outcomes (Goldenberg et al., 2000; U.S. Department of Health and Human Services, 2001).
A few studies investigated the impact of September 11th on pregnant women residing and/or working near the WTC. One study reported reduced gestation and birthweight in term births (Lederman et al., 2004), and another reported no differences in either outcome, but an increase in intrauterine growth retardation (IUGR) (Berkowitz et al., 2003). These studies did not differentiate between the possible toxic and psychological causes of their findings.
Additional studies of more remote populations also showed inconsistent results, with one in Holland reporting no difference in gestation but lower mean birthweight among term infants in utero on September 11, 2001, compared with one year later (Smits et al., 2006), and another in Boston finding a curiously lower risk of preterm delivery, particularly among women exposed to the event during their first trimester (Rich-Edwards et al., 2005).
The present study assesses whether the events of September 11th were associated with an immediate or delayed increase in rates of low birthweight (LBW) or preterm birth among newborns in NYC and upstate New York (NY). We hypothesized that women in upstate NY would be less affected than those in NYC. We theorize that effects would be due, in part, to the psychological distress triggered by these events.
Materials and Methods
Population
We obtained birth certificate data from the Office of Vital Statistics, NYC Department of Health and Mental Hygiene and the Vital Records Section, NY State Department of Health for liveborn, singleton infants delivered between January 1996 and December 2002 to NY residents who did not have diabetes listed as a pregnancy complication (n = 1660,401). To protect individuals' identity, variables were provided in categories, e.g. birthweight in 500-g intervals and date of birth collapsed into week of birth. County of maternal residence was not specified, but NYC data included borough, with Manhattan subdivided by residential zip code into lower, mid-town and upper Manhattan. We define ‘upstate’ NY residents as those who lived outside of NYC, including from Nassau, Suffolk and Westchester Counties.
We aimed to examine the psychosocial impact of the events of September 11th; therefore, except where noted, NYC analyses excluded births to residents of lower Manhattan, i.e. zip codes below West 14th and East Houston Streets, where there was greatest potential toxic exposure (Huber et al., 2004; Wolff et al., 2005). We also excluded records missing birthweight (<0.1%) or child's gender (<0.001%). This study has been approved by the Committee for the Protection of Human Subjects, University of California, Berkeley.
Definition of outcomes
We examined the risk of delivering a liveborn infant of <1500, 1500–1999 and 2000–2499 g compared with infants weighing ≥2500 g. Of infants with recorded gestational age (GA) weighing <1500, 1500–1999 and 2000–2499 g, 94, 80 and 46% were <37 weeks gestation, with 79, 22 and 4% <32 weeks, respectively. Birthweight is considered to be more accurately and completely reported on birth certificates than GA (Reichman and Hade, 2001; Roohan et al., 2003). Nevertheless, we examined the risk of delivering preterm: <32 (‘very preterm’) and 32 to <37 (‘moderate preterm’) versus ≥37 completed weeks gestation, based on last menstrual period.
Statistical analysis
Regression models were estimated separately for each outcome and for residents of NYC and upstate NY. To investigate whether the disaster was associated with immediate changes in birth outcomes, we used multiple logistic regression to compare the risk of LBW or preterm delivery in the week beginning Tuesday, September 11th relative to the prior three-week period. Within NYC (excluding 285 births from lower Manhattan), 8465 births were eligible for this analysis (6304 before, 2161 after); in upstate NY, 9753 were included (7259 before, 2494 after).
To explore whether associations differed depending on when in gestation the disaster occurred, we extended analyses to include 10 four-week intervals following September 11th relative to the same four-week intervals during the preceding two years (i.e. eight weeks ‘unexposed’ versus four weeks ‘exposed’). Within NYC, each exposed interval averaged 8065 births, and comparison groups averaged 16 464. In upstate NY, exposed intervals averaged 9153 births, and comparison groups averaged 18 947.
For preterm analyses, records with missing GA were excluded (4%). Repeating analyses with births missing GA classified as either term or preterm did not substantially alter results.
Covariates for multivariate models were selected a priori from the literature, including infant sex, maternal race/ethnicity, age, education, nationality, smoking, parity, insurance, initiation of prenatal care in the first trimester and hypertensive disorder (i.e. chronic hypertension, pregnancy-induced hypertension, pre-eclampsia and/or eclampsia listed as a complication of pregnancy) (see Table 1 for categories). We found no multicollinearity. No records lacked parity or smoking status, and race/ethnicity, education, payer and hypertensive disorder were coded with separate unknown/‘other’ categories. Missing values of maternal age, birthplace and prenatal care were grouped with the reference group.
Demographic characteristics of gravidas residing in NYC (excluding lower Manhattan) and upstate NY in the three weeks before and the one week after September 11, 2001
| . | NYC, n (%) . | Upstate NY, n (%) . |
|---|---|---|
| Total | 8465 (100) | 9753 (100) |
| Infant sex | ||
| Male | 4365 (52) | 5055 (52) |
| Female | 4100 (48) | 4698 (48) |
| Smoker | ||
| No | 8237 (97) | 8413 (86) |
| Yes | 228 (3) | 1340 (14) |
| Maternal race/ethnicity | ||
| Non-Hispanic white | 2215 (26) | 7217 (74) |
| African–American | 2702 (32) | 1034 (11) |
| Hispanic | 2664 (31) | 1119 (11) |
| Asian/other | 884 (10) | 383 (4) |
| Maternal natality | ||
| US Born | 3834 (45) | 8090 (83) |
| Foreign-born | 4631 (55) | 1663 (17) |
| Maternal age (years) | ||
| <18 | 296 (3) | 243 (2) |
| 18–34 | 6813 (80) | 7677 (79) |
| >35 | 1356 (16) | 1833 (19) |
| Maternal education | ||
| <H.S. graduate | 2086 (25) | 1457 (15) |
| ≥H.S. graduate | 6338 (75) | 8174 (84) |
| Unknown | 41 (0) | 122 (1) |
| Parity | ||
| 1 | 3902 (46) | 3913 (40) |
| 2–5 | 4381 (52) | 5673 (58) |
| ≥6 | 182 (2) | 167 (2) |
| Hypertensive disorder | ||
| No | 7980 (94) | 8917 (91) |
| Yes | 356 (4) | 425 (4) |
| Unknown | 129 (2) | 411 (4) |
| Payer of delivery | ||
| Insurance/HMO | 3593 (42) | 6795 (70) |
| Medicaid | 4585 (54) | 2477 (25) |
| Self pay | 254 (3) | 209 (2) |
| Unknown | 33 (0) | 272 (3) |
| Prenatal care initiation | ||
| First trimester | 5348 (63) | 7075 (73) |
| >First/none/missing | 3117 (37) | 2678 (27) |
| . | NYC, n (%) . | Upstate NY, n (%) . |
|---|---|---|
| Total | 8465 (100) | 9753 (100) |
| Infant sex | ||
| Male | 4365 (52) | 5055 (52) |
| Female | 4100 (48) | 4698 (48) |
| Smoker | ||
| No | 8237 (97) | 8413 (86) |
| Yes | 228 (3) | 1340 (14) |
| Maternal race/ethnicity | ||
| Non-Hispanic white | 2215 (26) | 7217 (74) |
| African–American | 2702 (32) | 1034 (11) |
| Hispanic | 2664 (31) | 1119 (11) |
| Asian/other | 884 (10) | 383 (4) |
| Maternal natality | ||
| US Born | 3834 (45) | 8090 (83) |
| Foreign-born | 4631 (55) | 1663 (17) |
| Maternal age (years) | ||
| <18 | 296 (3) | 243 (2) |
| 18–34 | 6813 (80) | 7677 (79) |
| >35 | 1356 (16) | 1833 (19) |
| Maternal education | ||
| <H.S. graduate | 2086 (25) | 1457 (15) |
| ≥H.S. graduate | 6338 (75) | 8174 (84) |
| Unknown | 41 (0) | 122 (1) |
| Parity | ||
| 1 | 3902 (46) | 3913 (40) |
| 2–5 | 4381 (52) | 5673 (58) |
| ≥6 | 182 (2) | 167 (2) |
| Hypertensive disorder | ||
| No | 7980 (94) | 8917 (91) |
| Yes | 356 (4) | 425 (4) |
| Unknown | 129 (2) | 411 (4) |
| Payer of delivery | ||
| Insurance/HMO | 3593 (42) | 6795 (70) |
| Medicaid | 4585 (54) | 2477 (25) |
| Self pay | 254 (3) | 209 (2) |
| Unknown | 33 (0) | 272 (3) |
| Prenatal care initiation | ||
| First trimester | 5348 (63) | 7075 (73) |
| >First/none/missing | 3117 (37) | 2678 (27) |
H.S. graduate, high school graduate; HMO, health maintenance organization; NYC, New York City; upstate NY, upstate New York.
Demographic characteristics of gravidas residing in NYC (excluding lower Manhattan) and upstate NY in the three weeks before and the one week after September 11, 2001
| . | NYC, n (%) . | Upstate NY, n (%) . |
|---|---|---|
| Total | 8465 (100) | 9753 (100) |
| Infant sex | ||
| Male | 4365 (52) | 5055 (52) |
| Female | 4100 (48) | 4698 (48) |
| Smoker | ||
| No | 8237 (97) | 8413 (86) |
| Yes | 228 (3) | 1340 (14) |
| Maternal race/ethnicity | ||
| Non-Hispanic white | 2215 (26) | 7217 (74) |
| African–American | 2702 (32) | 1034 (11) |
| Hispanic | 2664 (31) | 1119 (11) |
| Asian/other | 884 (10) | 383 (4) |
| Maternal natality | ||
| US Born | 3834 (45) | 8090 (83) |
| Foreign-born | 4631 (55) | 1663 (17) |
| Maternal age (years) | ||
| <18 | 296 (3) | 243 (2) |
| 18–34 | 6813 (80) | 7677 (79) |
| >35 | 1356 (16) | 1833 (19) |
| Maternal education | ||
| <H.S. graduate | 2086 (25) | 1457 (15) |
| ≥H.S. graduate | 6338 (75) | 8174 (84) |
| Unknown | 41 (0) | 122 (1) |
| Parity | ||
| 1 | 3902 (46) | 3913 (40) |
| 2–5 | 4381 (52) | 5673 (58) |
| ≥6 | 182 (2) | 167 (2) |
| Hypertensive disorder | ||
| No | 7980 (94) | 8917 (91) |
| Yes | 356 (4) | 425 (4) |
| Unknown | 129 (2) | 411 (4) |
| Payer of delivery | ||
| Insurance/HMO | 3593 (42) | 6795 (70) |
| Medicaid | 4585 (54) | 2477 (25) |
| Self pay | 254 (3) | 209 (2) |
| Unknown | 33 (0) | 272 (3) |
| Prenatal care initiation | ||
| First trimester | 5348 (63) | 7075 (73) |
| >First/none/missing | 3117 (37) | 2678 (27) |
| . | NYC, n (%) . | Upstate NY, n (%) . |
|---|---|---|
| Total | 8465 (100) | 9753 (100) |
| Infant sex | ||
| Male | 4365 (52) | 5055 (52) |
| Female | 4100 (48) | 4698 (48) |
| Smoker | ||
| No | 8237 (97) | 8413 (86) |
| Yes | 228 (3) | 1340 (14) |
| Maternal race/ethnicity | ||
| Non-Hispanic white | 2215 (26) | 7217 (74) |
| African–American | 2702 (32) | 1034 (11) |
| Hispanic | 2664 (31) | 1119 (11) |
| Asian/other | 884 (10) | 383 (4) |
| Maternal natality | ||
| US Born | 3834 (45) | 8090 (83) |
| Foreign-born | 4631 (55) | 1663 (17) |
| Maternal age (years) | ||
| <18 | 296 (3) | 243 (2) |
| 18–34 | 6813 (80) | 7677 (79) |
| >35 | 1356 (16) | 1833 (19) |
| Maternal education | ||
| <H.S. graduate | 2086 (25) | 1457 (15) |
| ≥H.S. graduate | 6338 (75) | 8174 (84) |
| Unknown | 41 (0) | 122 (1) |
| Parity | ||
| 1 | 3902 (46) | 3913 (40) |
| 2–5 | 4381 (52) | 5673 (58) |
| ≥6 | 182 (2) | 167 (2) |
| Hypertensive disorder | ||
| No | 7980 (94) | 8917 (91) |
| Yes | 356 (4) | 425 (4) |
| Unknown | 129 (2) | 411 (4) |
| Payer of delivery | ||
| Insurance/HMO | 3593 (42) | 6795 (70) |
| Medicaid | 4585 (54) | 2477 (25) |
| Self pay | 254 (3) | 209 (2) |
| Unknown | 33 (0) | 272 (3) |
| Prenatal care initiation | ||
| First trimester | 5348 (63) | 7075 (73) |
| >First/none/missing | 3117 (37) | 2678 (27) |
H.S. graduate, high school graduate; HMO, health maintenance organization; NYC, New York City; upstate NY, upstate New York.
We also conducted time-series analyses on birthweight to determine whether observed values post-disaster differed from expected. We performed these analyses because logistic regression could yield type I or II errors if patterns over time (i.e. autocorrelation) in odds of <1500, 1500–1999 and 2000–2499 g exhibit high or low values coinciding with September 11th. We employed the strategy devised by Box et al. (1994) to identify and model autocorrelation in the odds of each of the three LBW groups. We derived Box–Jenkins models for 297 weeks beginning Tuesday, January 2, 1996 and ending Monday, September 10, 2001. We then used these models to forecast the ratios for each LBW group relative to births ≥2500 g for the week starting Tuesday, September 11, 2001. We determined whether the observed value was outside the limits of the 95% confidence interval (CI) of the forecasted value for that week.
We also subjected the four-week interval data to an interrupted time-series analysis to determine if autocorrelation in the birthweight series could have induced the logistic regression results. This method also used the Box–Jenkins approach to derive statistically expected values of the ratio of each LBW group to infants weighing ≥2500 g from its history. The method requires adding a binary variable scored 1 for the period starting September 11, 2001 and 0 otherwise to the best fitting Box–Jenkins model. Coefficients for the binary variable are the difference between the observed ratio and that expected contingent on history. In NYC analyses, we adjusted for the proportion of women in each interval initiating prenatal care in the first trimester.
Results
Population characteristics
During the four-week period around September 11th, proportions of births <1500, 1500–1999 and 2000–2499 g were, respectively, 1.4, 1.2 and 4.1% in NYC, and 0.9, 0.8 and 3.0% in upstate NY. The proportion of very preterm and moderate preterm were, respectively, 1.5 and 8.0% in NYC, and 1.4 and 7.2% in upstate NY. As shown in Table 1, during this period, about half of NYC mothers were primiparous, foreign-born and had delivery paid by Medicaid. About one-third were African–American, one-third Hispanic and a quarter non-Hispanic white mothers. In upstate NY, 17% of mothers were foreign-born, 25% had Medicaid-paid deliveries, and most births were to non-Hispanic white mothers. In both locations, characteristics were similar in the three weeks before and one after September 11th, except that NYC mothers delivering post-disaster were more likely to have had first trimester prenatal care (P = 0.04).
Proportions of LBW and preterm during the 40 weeks after September 11th and the same period in the two previous years were similar to those above (Supplementary Table S1). Demographic characteristics were also nearly identical to those noted above and were generally similar before and after the event (Supplementary Table S2). In NYC, noticeably more women had first trimester prenatal care in the 40 weeks after September 11th (65%) than the period before (58%).
The week after September 11th
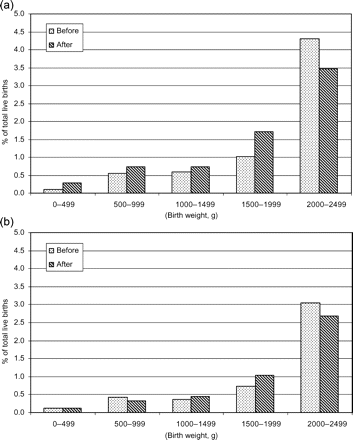
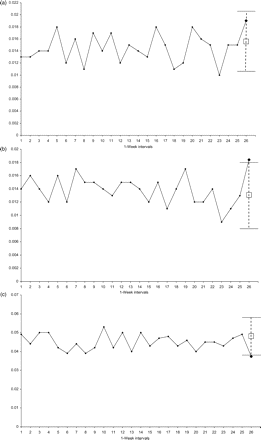
In NYC, in the week after September 11th compared with the weeks before, we observe a shift in the LBW distribution, with a higher proportion of births <2000 g, and a lower proportion between 2000 and 2499 g (Fig. 1). A similar albeit attenuated pattern is observed in upstate NY. Table 2 shows that among NYC infants, there was a borderline increased odds of birthweight <1500 g [adjusted odds ratio (aOR) = 1.44] and an increased odds of weighing 1500–1999 g (aOR = 1.67), but a non-significant decreased odds of weighing 2000–2499 g (aOR = 0.83). There were no significant changes in any LBW category in upstate NY. Figure 2 presents time-series results for NYC, showing 26 weeks of observed ratios of LBW to normal-weight births with the predicted ratio for each group for the week beginning September 11th forecasted from history. Time-series findings for NYC and upstate NY agree with logistic results, except that the ratio of NYC births 2000–2499 to ≥2500 g is now significantly lower than predicted (Fig. 2c).
Percentage of total live births in birthweight categories <2500 g born in NYC (excluding lower Manhattan) and upstate NY during the week beginning September 11, 2001 and the three weeks before
(a) NYC (excluding lower Manhattan) (n = 8465 live births). (b) Upstate NY (n = 9753 live births)
Time series results of weekly intervals preceding and including the week of September 11th
The points connected by the solid line represent the ‘observed’ ratio of births weighing <1500 (a), 1500–1999 (b) and 2000–2499 g (c) to those weighing ≥2500 g in NYC (excluding lower Manhattan) for 26 seven-day periods ending with the period starting September 11, 2001. The ‘predicted’ value for the seven-day period beginning September 11th is shown with a square and is forecasted from the history of the 297 weeks before that week (only 26 weeks are shown). The upper and lower 95% CI for the predicted value for the week beginning September 11th is indicated with broken lines. The ‘observed’ ratio for the week beginning September 11th is shown with a diamond. (a) <1500 versus ≥2500 g, (b) 1500–1999 versus ≥2500 g and (c) 2000–2499 versus ≥2500 g
Adjusteda OR and 95% CI for risk of delivering a LBW infant (<1500, 1500–1999 and 2000–2499 g) in NYC (excluding births in lower Manhattan) and in upstate NY during the week beginning September 11, 2001 compared with the previous three weeks
| . | N (% LBW) . | Crude OR . | Adjusted* OR (95% CI) . | P-value . |
|---|---|---|---|---|
| <1500 versus ≥2500 g | ||||
| NYC | 8017 (1.4) | 1.41 | 1.44 (0.97, 2.15) | 0.07 |
| Upstate NY | 9386 (0.9) | 0.97 | 0.89 (0.54, 1.46) | 0.63 |
| 1500–1999 versus ≥2500 g | ||||
| NYC | 8002 (1.2) | 1.67 | 1.67 (1.11, 2.52) | 0.01 |
| Upstate NY | 9377 (0.8) | 1.43 | 1.42 (0.88, 2.29) | 0.15 |
| 2000–2499 versus ≥2500 g | ||||
| NYC | 8246 (4.1) | 0.81 | 0.83 (0.63, 1.07) | 0.15 |
| Upstate NY | 9586 (3.0) | 0.88 | 0.87 (0.66, 1.16) | 0.34 |
| . | N (% LBW) . | Crude OR . | Adjusted* OR (95% CI) . | P-value . |
|---|---|---|---|---|
| <1500 versus ≥2500 g | ||||
| NYC | 8017 (1.4) | 1.41 | 1.44 (0.97, 2.15) | 0.07 |
| Upstate NY | 9386 (0.9) | 0.97 | 0.89 (0.54, 1.46) | 0.63 |
| 1500–1999 versus ≥2500 g | ||||
| NYC | 8002 (1.2) | 1.67 | 1.67 (1.11, 2.52) | 0.01 |
| Upstate NY | 9377 (0.8) | 1.43 | 1.42 (0.88, 2.29) | 0.15 |
| 2000–2499 versus ≥2500 g | ||||
| NYC | 8246 (4.1) | 0.81 | 0.83 (0.63, 1.07) | 0.15 |
| Upstate NY | 9586 (3.0) | 0.88 | 0.87 (0.66, 1.16) | 0.34 |
aControlling for gender, maternal smoking (yes/no), race/ethnicity (non-Hispanic white, African–American, Hispanic, Asian/other), education (<high school graduate versus high school graduate or more), country of birth (USA versus foreign-born), age (<18, 18–34, 35+ years), parity (first, second–fifth, sixth or more), prenatal care initiation (first trimester versus later or none), payer for delivery (private insurance/HMO, medicaid, self-pay, unknown) and maternal hypertensive disorder during pregnancy. LBW, low birthweight; upstate NY, upstate New York.
Adjusteda OR and 95% CI for risk of delivering a LBW infant (<1500, 1500–1999 and 2000–2499 g) in NYC (excluding births in lower Manhattan) and in upstate NY during the week beginning September 11, 2001 compared with the previous three weeks
| . | N (% LBW) . | Crude OR . | Adjusted* OR (95% CI) . | P-value . |
|---|---|---|---|---|
| <1500 versus ≥2500 g | ||||
| NYC | 8017 (1.4) | 1.41 | 1.44 (0.97, 2.15) | 0.07 |
| Upstate NY | 9386 (0.9) | 0.97 | 0.89 (0.54, 1.46) | 0.63 |
| 1500–1999 versus ≥2500 g | ||||
| NYC | 8002 (1.2) | 1.67 | 1.67 (1.11, 2.52) | 0.01 |
| Upstate NY | 9377 (0.8) | 1.43 | 1.42 (0.88, 2.29) | 0.15 |
| 2000–2499 versus ≥2500 g | ||||
| NYC | 8246 (4.1) | 0.81 | 0.83 (0.63, 1.07) | 0.15 |
| Upstate NY | 9586 (3.0) | 0.88 | 0.87 (0.66, 1.16) | 0.34 |
| . | N (% LBW) . | Crude OR . | Adjusted* OR (95% CI) . | P-value . |
|---|---|---|---|---|
| <1500 versus ≥2500 g | ||||
| NYC | 8017 (1.4) | 1.41 | 1.44 (0.97, 2.15) | 0.07 |
| Upstate NY | 9386 (0.9) | 0.97 | 0.89 (0.54, 1.46) | 0.63 |
| 1500–1999 versus ≥2500 g | ||||
| NYC | 8002 (1.2) | 1.67 | 1.67 (1.11, 2.52) | 0.01 |
| Upstate NY | 9377 (0.8) | 1.43 | 1.42 (0.88, 2.29) | 0.15 |
| 2000–2499 versus ≥2500 g | ||||
| NYC | 8246 (4.1) | 0.81 | 0.83 (0.63, 1.07) | 0.15 |
| Upstate NY | 9586 (3.0) | 0.88 | 0.87 (0.66, 1.16) | 0.34 |
aControlling for gender, maternal smoking (yes/no), race/ethnicity (non-Hispanic white, African–American, Hispanic, Asian/other), education (<high school graduate versus high school graduate or more), country of birth (USA versus foreign-born), age (<18, 18–34, 35+ years), parity (first, second–fifth, sixth or more), prenatal care initiation (first trimester versus later or none), payer for delivery (private insurance/HMO, medicaid, self-pay, unknown) and maternal hypertensive disorder during pregnancy. LBW, low birthweight; upstate NY, upstate New York.
We also examined the logistic regression results for preterm delivery for the week after September 11th. We observed no significant changes in risk of being born early in either NYC or upstate NY, although the slight increase in very preterm births in NYC were consistent with the birthweight results (aOR = 1.30; 95% CI = 0.89, 1.91) (Supplementary Table S3).
Regression results for both birthweight and preterm outcomes were virtually identical when residents of lower Manhattan were included.
Ten four-week intervals after september 11th
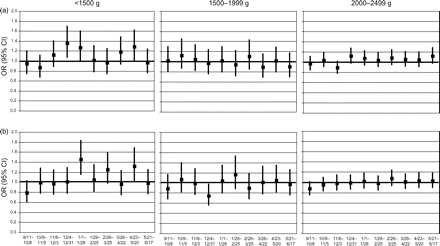
Figure 3 presents logistic results for LBW in the 10 four-week intervals post-disaster. Despite the increased risk in the week after September 11th reported above, because of fewer low-weight births in the three subsequent weeks, we observed no overall change in odds of LBW during the first four-week interval. However, in NYC in the two intervals bracketing the New Year (December 4, 2001 to January 28, 2002), we observed an increased adjusted odds of delivering an infant <1500 g (aOR = 1.36, P = 0.01; and aOR = 1.28, P = 0.04). The next period of elevated odds occurred in the interval 33 to 36 weeks (April 23 to May 20, 2002) after September 11th (aOR = 1.29, P = 0.03)(Fig. 3a). In upstate NY, we observed a similar peak in the odds of <1500-g deliveries in January, 2002 (aOR = 1.46, P = 0.001) and in the interval 33–36 weeks after September 11th (aOR = 1.32, P = 0.03) (Fig. 3b). Unlike NYC, upstate NY showed a decreased odds of birthweight 1500–1999 g during December, 2001 (aOR = 0.74, P = 0.03) (Fig. 3b). Time-series results (Supplementary Table S4) were consistent with these results from logistic models.
Adjusted OR* and 95% CI for risk of delivering a low birthweight infant (<1500, 1500–1999 and 2000–2499 g) in NYC (excluding births in lower Manhattan) and in upstate NY for 10 four-week intervals following September 11, 2001 compared with the same intervals from each of two years before
*Multiple logistic regression controlling for gender, maternal smoking (yes/no), race/ethnicity (non-Hispanic white, African–American, Hispanic, Asian/other), education (<high school graduate versus high school graduate or more), country of birth (USA versus foreign-born), age (<18, 18–34, >35 years), parity (first, second–fifth, sixth or more), prenatal care initiation (first trimester versus later or none), payer for delivery (private insurance/HMO, medicaid, self-pay, unknown) and maternal hypertensive disorder during pregnancy. HMO, health maintenance organization
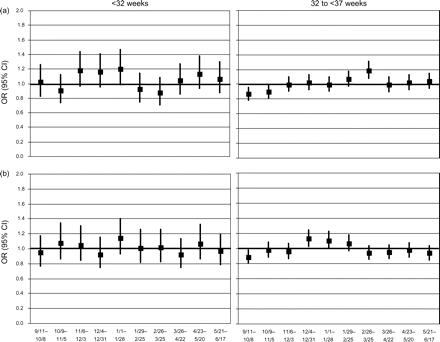
Around the New Year, when we observed increases in <1500-g births, we found non-significant increases in odds of very preterm births (P = 0.07–0.14) in NYC and significant increases in moderate preterm births (P < 0.05) in upstate NY (Fig. 4). We also observed a decreased odds of moderate preterm delivery in the first eight weeks following the disaster in NYC (OR = 0.87, P = 0.01; and OR = 0.90, P = 0.03) and in the first four weeks (OR = 0.89, P = 0.02) in upstate NY.
Adjusted OR* and 95% CI for risk of preterm delivery (<32, 32 to <37 weeks) in NYC (excluding births in lower Manhattan) and in upstate NY for 10 four-week intervals following September 11, 2001, compared with the same intervals from each of two years before
*Multiple logistic regression controlling for gender, maternal smoking (yes/no), race/ethnicity (non-Hispanic white, African–American, Hispanic, Asian/other), education (<high school graduate versus high school graduate or more), country of birth (USA versus foreign-born), age (<18, 18–34, >35 years), parity (first, second–fifth, sixth or more), prenatal care initiation (first trimester versus later or none), payer for delivery (private insurance/HMO, medicaid, self-pay, unknown) and maternal hypertensive disorder during pregnancy
Logistic regression results for birthweight and preterm outcomes in NYC were virtually identical when births from lower Manhattan were included (data not shown).
Discussion
We reported an increase in deliveries of infants weighing <2000 g in NYC in the week of September 11th, but a decrease in infants weighing 2000–2499 g. We observed no significant LBW increase in upstate NY. We also found increased odds of birthweight <1500 g around the New Year (infants who would have been in their first or second trimester of gestation at the time of the disaster) and 33–36 weeks post-disaster (conceived around or after September 11th) in both NYC and upstate NY. Patterns of preterm birth were largely consistent with these birthweight findings, although there was a decrease in moderately preterm births in both locations in the period after September 11th.
A woman's stress response is dependent on many factors, including the nature and severity of the stressor (de Weerth and Buitelaar, 2005), and there may be different responses immediately and distally. Acute effects of stress on pregnancy outcomes have rarely been studied. Reports following natural disasters suggest increased emergency care for labor and vaginal bleeding just after the 1994 Northridge earthquake (Salinas et al., 1998), and for premature rupture of membranes and premature labor within 48 h of the 1984 Haifa earthquake (Weissman et al., 1989).
Previous studies of birth outcomes following September 11th focused on the later, rather than immediate, impact. Similar to our findings, Lederman et al. (2004) found lower birthweight among term infants born to women living/working near the WTC compared with ‘unexposed’ women uptown. Among both groups, they also found shortened gestation when the event occurred in the first trimester. However, in another study, Berkowitz et al. (2003) found that proximity to the WTC site within three weeks after the disaster was associated with IUGR in offspring, regardless of trimester of exposure, with no differences in birthweight or GA. By comparing women from near the WTC to elsewhere in NYC, these studies failed to account for the fact that controls likely shared exposure to stress even if not environmental exposures.
Our findings in upstate NY of decreases in preterm in the first month, but later increases in LBW are consistent with results from previous studies on the more geographically remote impact of these events. Smits et al. (2006) found lower birthweight (~70 g) in term infants of Dutch women in their second or third trimesters during September 11th; adjustment for GA suggested that earlier delivery played a role, but GA was not itself associated with exposure. In contrast, Rich-Edwards et al. (2005) found slightly longer GA and lower risk of preterm among Boston women in the first trimester during September 11th.
We found decreased preterm births in NY one to two months after the disaster. Engel et al. (2005) assessed PTS during pregnancy in NYC women exposed to the WTC during their first two trimesters and subsequently found PTS to be associated with longer GA. They note that others have linked PTS with depressed cortisol production, despite other types of stress often being associated with increased cortisol (Yehuda, 2002; Seng et al., 2005). Alternatively, Rich-Edwards et al. (2005) hypothesized that their results of longer GA in Boston may be attributable to more vulnerable pregnancies being lost, yielding a healthier exposed population eligible for live birth. Further evidence for this competing mortality hypothesis derives from Catalano et al. (2005) who observed the highest rate of male fetal deaths in six consecutive years in November/December of 2001 in California and January 2002 in NYC (Catalano et al., 2006). According to this hypothesis, we may have underestimated the effect of the disaster if the more vulnerable had been culled from the population by fetal death.
We had hypothesized that women further away from a disaster may have less stress associated with the event. We observed immediate effects only in NYC, but longer-term effects both in NYC and upstate. This may provide some indication that higher levels of stress are necessary to induce acute effects on birth outcome. Alternatively, upstate and NYC groups also differed in demographic characteristics that might be associated with differences in the stress response, and/or its influence on birth outcomes.
We observed in both locations an increase in LBW around the New Year and again 33–36 weeks post-disaster. The relevance of the timing is difficult to explain—the increase around Christmas/New Years may be directly related to the event having occurred earlier in gestation, or it may be related to the heightened emotion of the post-disaster holiday. However, the increase in VLBW 33–36 weeks after September 11th suggests that exposure periconception may also impact birth outcomes, although exact mechanisms remain unknown.
We hypothesize that the increased incidence of LBW is mainly due to stress-initiated early parturition; however, because of limitations in the data available to us, we were not able to test our hypothesis thoroughly. Although birthweight is accurately recorded on birth certificates (Reichman and Hade, 2001; Roohan et al., 2003), the quality of GA data is less reliable. Having outcomes provided categorically further limited analyses, and lack of detailed medical information prevented investigation into the etiology of our findings. In addition, exposure may have been misclassified since birth certificates only record residence and not location at the time of the disaster or the extent of individuals' distress. However, births to NY residents who left the state after the disaster are included.
This study also has a number of strengths. For the most part, we found converging results using two statistical methods. Regression analyses controlled for individual-level covariates and utilized a much larger sample that was subject to less bias than previous studies. Time-series analyses used >5 years of birth data to predict expected outcomes controlling for temporal and seasonal trends. We were able to examine both the immediate and distal impact of the WTC disaster. Had we examined birth outcomes only by month or trimester, the finding of an immediate, short-lived impact would have been diluted by the subsequent drop in LBW deliveries.
We attempted to determine the impact of psychological distress independent of toxic exposure by both including and excluding residents of lower Manhattan and found that results were unchanged. However, we were unable to identify residents of other areas with moderate chemical exposure (Huber et al., 2004; Wolff et al., 2005). While we have theorized that our findings are due to psychological distress triggered by this disaster, we cannot rule out other factors including chemical exposure to explain some of the findings.
In summary, our findings contribute to the growing body of evidence suggesting that psychological distress may affect pregnancy outcomes. Our methodology supports the parallel use of multiple regression modeling and time-series analysis techniques in future studies of community-wide stressors and birth outcomes.
Funding
This publication was made possible by small grants from the Center for Health Research, University of California, Berkeley and the Robert Wood Johnson Foundation's Health and Society Scholars program. This research was also supported by grant numbers: RD 83171001 from EPA and PO1 ES009605 from NIEHS. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIEHS, NIH, or EPA.
Acknowledgements
The authors wish to thank Katherine Kogut of UC Berkeley for her editorial comments, and the Bureau of Biometrics and Health Statistics, New York State Department of Health, and the Vital Records Section of the New York City Department of Health and Mental Hygiene for providing the vital statistics data.