-
PDF
- Split View
-
Views
-
Cite
Cite
Marco Ferrario, Paolo Chiodini, Lloyd E Chambless, Giancarlo Cesana, Diego Vanuzzo, Salvatore Panico, Roberto Sega, Lorenza Pilotto, Luigi Palmieri, Simona Giampaoli, for the CURORE Project Research Group, Prediction of coronary events in a low incidence population. Assessing accuracy of the CUORE Cohort Study prediction equation, International Journal of Epidemiology, Volume 34, Issue 2, April 2005, Pages 413–421, https://doi.org/10.1093/ije/dyh405
Close - Share Icon Share
Abstract
Background The aims of this paper are to derive a 10-year coronary risk predictive equation for adult Italian men, and to assess its accuracy in comparison with the Framingham Heart Study (FHS) and PROCAM study equations.
Methods The CUORE study is a prospective fixed-cohort study. Eleven cohorts, from the north and the centre–south of Italy, had been investigated at baseline between 1982 and 1996, adopting MONICA methods to measure risk factors. Among this sample of 6865 men, aged 35–69 years and free of coronary heart disease (CHD) at baseline, 312 first fatal and non-fatal major coronary events occurred in 9.1 years median follow-up. Calibration, as the difference between 10-year predicted and actual risk, and discrimination, as the ability of the risk functions to separate high-risk from low-risk subjects, have been assessed to compare accuracy of the FHS, the PROCAM, and the CUORE study equations.
Results The best CUORE equation includes age, total cholesterol, systolic blood pressure, cigarette smoking, HDL-cholesterol, diabetes mellitus, hypertension drug treatment, and family history of CHD (area under the ROC curve = 0.75). The uncalibrated estimates of the 10-year risk in this CUORE follow-up data were 0.093 and 0.109 higher (P < 0.05) from the Framingham and PROCAM risk scores, respectively, than the Kaplan–Meier estimate for CUORE, indicating risk overestimates for both equations. Standard recalibration techniques improved accuracy of the FHS equation only. PROCAM overestimates were prominent in the higher risk deciles. With an alternative method for recalibration better risk estimates were obtained, but a cohort study was needed to obtain a properly calibrated risk equation.
Conclusions The CUORE Project predictive equation showed better accuracy of the FHS and PROCAM equations, overcoming frequently reported risk overestimates. The CUORE equation may be adopted to identify men with high coronary risk in Italy.
American and European cardiological societies recommend the identification of high-risk subjects using predictive equations1–7 for the prevention of coronary heart diseases (CHDs) at the individual level. The Framingham Heart Study (FHS) and the PROCAM study equations are two well-known examples of such predictive equations. More recently the SCORE Project proposed a predictive equation based on CVD mortality derived from several European cohorts.
Improving CHD risk prediction continues to be a major challenge, due to the reported disputed findings in their generalizability.89–10 At the European level, risk overestimates were reported when the FHS equation was applied to southern German cohorts11 as well as to a wide British cohort.12 Risk overestimates may be even more pronounced when equations derived from high-risk populations are applied to subjects of low-risk populations.13 The accuracy of the FHS equation, derived from a white North American population, has been assessed for some minorities living in the US.14 Marrugat et al. reported minor differences between CHD events registered in a Spanish population and predicted events in the same population based on the recalibrated FHS equation.15 In a recent paper both the FHS and PROCAM study equations evidenced poor estimation of the absolute risk in the PRIME French and northern Ireland cohorts,16 leading the authors to conclude that population-specific risk functions are needed. Large population-based cohorts followed for a long time period are essential, in particular when study subjects come from low incidence populations. In Italy, predictive risk equations have been derived from the cohorts recruited decades ago in the Seven Countries Study, or including only coronary deaths as endpoints.17,18
The aims of the present paper are to report on a 10-year coronary risk predictive equation for Italian men aged 35–69 years, free of CHD at baseline, and to assess the accuracy of this equation in comparison with the equations recently reported by the FHS and the PROCAM study.
Methods
Study design and cohort characteristics
The CUORE Cohorts Project is a large, prospective fixed-cohort follow-up study that includes cohorts from the northwest, the northeast, the centre and the south of Italy of both gender groups, recruited in comparable calendar years. The CUORE cohorts were originally investigated to assess cardiovascular risk factor distributions and time trends from the first half of the 1980s to the first half of the 1990s. Of the original 17 cohorts 11 were followed up until December 31, 1998 to ascertain fatal and non-fatal major coronary events and strokes.
We excluded from the analysis two factory-based cohorts with a short follow-up period, three cohorts with incomplete follow-up of non-fatal events or because of unavailable data on prevalent CHD cases at baseline, and one entirely female cohort. Women were excluded because of the small number of events due to the low incidence and the shorter follow-up period. Of the 11 remaining population-based cohorts, 7 were randomly selected samples of 25–64-year-old residents of two WHO MONICA Italian populations (Brianza and Friuli).19 The PAMELA Study, which aimed to identify normal values for ambulatory blood pressure, recruited a random sample of the 25–74-year-old residents of the town of Monza in 1990–93 and was investigated by the MONICA Brianza team.20 The Emostatico Study was a random sample of the 45–64-year-old residents of the town of Udine in Friuli, enrolled in 1995–96 and investigated by the MONICA Friuli team. The MATISS Study, conducted by the Istituto Superiore di Sanità in Rome, surveyed independent random samples of the 20–69-year-old residents of four small towns in the Latina province (located south of Rome), in different time periods between 1983 and 1995.21 The analysis was restricted to 6865 men aged 35–69 years free of CHD events at baseline with complete data on the risk factors considered.
Measurement of coronary risk factors
Coronary risk factors were investigated at baseline by three collaborating centres adhering to the standardized procedures and quality standards of the WHO MONICA Project (http://www.ktl.fi/publications/monica/manual/index.htm). Briefly, trained technicians took the blood pressure of the sitting subjects, at rest for ≥10 min, using a standard mercury sphygmomanometer. Systolic and diastolic blood pressure were taken at the first and fifth phase of the Korotkoff sounds, using standard mercury sphygmomanometers equipped with two side cuff bladders (13 and 17 cm). The average of two measurements, taken 5 min apart, was used as the study variable.
Venous blood specimens were taken from the ante-cubital vein using a tourniquet only if necessary. Subjects were asked to fast for 12 h before drawing blood. Specimens were refrigerated at −4°C and shipped within 4 h to the collaborating laboratories: the University Department of Clinical Pathology of the Desio Hospital, the Laboratory of Clinical Biochemistry of the Istituto Superiore di Sanità in Rome, and the Istituto Analisi Chimico-Cliniche of the St Maria Misericordia Hospital in Udine. In the MATISS Study specimens were refrigerated at −20°C for no more than 1 week. Serum total cholesterol and HDL-cholesterol determinations were done using the enzymatic method in all laboratories, the HDL-cholesterol subfraction was separated using the phosphotungstate–Mg2+ method at the Brianza and Rome laboratories and the PEG 6000 method at the Udine lab. Triglycerides were determined on sera using the GPO-PAP enzymatic colorimetric method at the Brianza and Udine lab and the Trinder method at the Rome lab. LDL-cholesterol was calculated from the Friedewald formula.22 Laboratories took part in the MONICA external quality control program (http://www.ktl.fi/publications/monica/tchol/tcholqa.htm, http://www.ktl.fi/publications/monica/hdl/hdlqa.htm), achieving acceptable results for time trend analysis, whose requirements are usually more strict than for assessing individual exposure levels.
Standardized interviews, derived from the MONICA Project, were administered to participants in each centre. For the cohorts included in the analysis common and comparable formats could be identified for information on cigarette smoking, classifying current smokers (regular and occasional smokers) and non-smokers (never plus past smokers), on the use of antihypertensive medications within the past 2 weeks, and family history of myocardial infarction (MI) or CHD before the age of 60 among first-degree relatives. Diabetes mellitus was defined using self-reported diagnoses, information on insulin and oral hypoglycaemic treatments, and fasting blood glucose (FBG) (available for 68% of the subjects) exceeding 126 mg/dl. In a sensitivity analysis, exclusion of FBG in the definition does not substantially modify the CUORE predictive coefficients. A positive history of CHD at baseline was attributed using information of documented or self-reported hospitalization for MI, unstable angina pectoris or cardiac revascularization, or ECG findings of MI (Minnesota codes 1-1 or 1-2, except 1-2-6).
Height and weight were measured on subjects without shoes and wearing light clothing. Body mass index (BMI) was computed as weight in kilograms divided by squared height in metres.
Ascertainment of incident major coronary events
Deaths were identified through an active collection of information on subject vital status from the municipalities of residence, and by tracking subjects who moved away to different towns. Death certificates were obtained from Local Health Districts and coded according to the International Classification of Diseases and Causes of Deaths—IX Revision (ICD IX). Vital status and death certificates were available for 99% of the subjects. Underlying causes of death ICD IX codes 410–414, 798, 799 as well as 250, 428, 440 codes in association with 410–414 codes in other causes were considered as suspected coronary deaths and further investigated for validation.
Non-fatal coronary events were ascertained through record linkage techniques23 using hospital discharge diagnosis (HDD) records with ICD IX 410–411 codes for suspected acute infarction and ICD IX CM 36.0-9 codes for coronary surgery revascularization. For selected cohorts, recruited before the 1990s when the completeness of the HDD database was inadequate, MONICA registers, rescreening of the cohorts, phone and postal interviews were also used to identify suspected events.
Suspected cases of MI were validated according to MONICA diagnostic criteria.24 In total 312 first major coronary events were included in the analysis: 105 MONICA validated coronary deaths (25 definite fatal MI, 59 possible fatal MI, and 21 sudden cardiac deaths), 96 MONICA definite non-fatal MIs, 68 MONICA possible non-fatal MIs, 28 coronary revascularizations, and 15 silent MIs with new major Q-waves (Minnesota Codes 1-1 and 1-2), available for 39% participants of the MATISS 1983 and MATISS 1987 cohorts, rescreened in 1994.
Statistical analyses
Age-adjusted incident MI rates were calculated for each risk factor, categorizing continuous risk factors in quintiles, from Poisson regression models.25,26 Cox proportional hazard models have been fitted separately according to FHS and PROCAM categorizations of risk factors.2,6 Gaussian distributions were assumed to test the differences between coefficients from different models.
A basic equation with age in years, total cholesterol in mg/dl, systolic blood pressure in mm Hg, smoking status (current smokers vs never smokers and past smokers) and BMI was fitted first. The identification of the best CUORE equation was pursued by assessing the contribution of the additional risk factors in terms of improvements in predictive discrimination, estimated as the area under the ROC curve (AUC), the probability that a cohort member with an event had a higher predicted 10-year coronary risk of event than a member without an event.27
We compared prediction accuracy of risk equations with the best CUORE equation. The FHS and the PROCAM equations were tested in the original form and after recalibration, adopting the method proposed by D'Agostino,13 which takes into consideration the population-specific risk factor means and 10-year Kaplan–Meier survival probability, as well as an alternative method suggested by Chambless.28 Due to missing values for triglycerides, the PROCAM equation was assessed on 5794 subjects.
Accuracy was assessed in terms of discrimination (AUC) and calibration. For the comparisons of discrimination abilities (AUC) of the three equations we adopt a split-sample approach, to reduce the expected over fit for CUORE when the equation is fitted and evaluated on the same dataset. The CUORE dataset was randomly separated into two parts, with half the subjects in each; the CUORE equation was fit on the first half of the dataset and then applied in combination with the other two study equations on the other half, to calculate the AUC values. This was repeated 1000 times on bootstrap resamples with replacement.29 The AUCs were ordered from smallest to largest and the middle 95% range constituted a 95% bootstrap confidence interval (CI). Note that recalibration does not affect discrimination.
The overall calibration was assessed using bootstrap 95% CI (1000 resamples) to test the difference between the observed 10-year Kaplan–Meier probability of coronary event and the predicted estimates from the original and the recalibrated FHS and PROCAM equations.
In addition, the Hosmer–Lemeshow (HL) statistic was used as an indicator of goodness of fit, comparing predicted and observed number of events by deciles of risk score, without a formal test of statistical significance.30 The statistical analysis was carried out in SAS (SAS Institute, Cary, NC).
Results
The essential descriptive characteristics of the 11 cohorts are reported in Table 1). Each collaborating centre contributed with cohorts of similar sample sizes, recruited at baseline in comparable examination periods and with overlapping age ranges. The numbers of person-years and coronary events, and the age-adjusted 10-year incidence rates for the risk factors are reported in Table 2) for 35–69-year-old subjects. The overall 10-year incidence of major coronary events in these CUORE cohorts was 5.1 per 100 person-years, and 5.6 and 4.7 per 100 person-years for the north (Brianza and Friuli) and the south (Rome) cohorts, respectively. Higher rates for higher quintiles of systolic blood pressure, total cholesterol, LDL-cholesterol, and lower quintiles of HDL-cholesterol were found, but less clear associations were evidenced for triglycerides and BMI quintiles. Higher absolute risk was detected among current smokers and past smokers in comparison with never smokers. Diabetic subjects in comparison with non-diabetic subjects showed a 1.54 incidence rate ratio. Rate ratios were also elevated for subjects with positive family history of CHD (1.48) and for subjects taking hypertension medication (2.0) in comparison with their referent categories.
Description of the main characteristics of cohorts included in the analysis
| Center—cohort . | Baseline examination periods . | Age range (years) . | Sample size (n) . | Median follow-up (years) . | Events (n) . |
|---|---|---|---|---|---|
| Brianza—MONICA 1st Survey | 1986–87 | 35–64 | 573 | 12.1 | 50 |
| Brianza—MONICA 2nd Survey | 1989–90 | 35–64 | 596 | 9.1 | 33 |
| Brianza—MONICA 3rd Survey | 1993–94 | 35–64 | 578 | 4.7 | 16 |
| Brianza—PAMELA Study | 1990–93 | 35–69 | 710 | 7.3 | 29 |
| Friuli—MONICA 1st Survey | 1986–86 | 35–64 | 524 | 12.7 | 26 |
| Friuli—MONICA 2nd Survey | 1989–89 | 35–64 | 347 | 9.6 | 10 |
| Friuli—MONICA 3rd Survey | 1994–94 | 35–64 | 655 | 4.5 | 10 |
| Friuli—Emostatico Study | 1995–96 | 45–64 | 192 | 2.6 | 4 |
| Rome—MATISS 83 Survey | 1983–84 | 35–69 | 1211 | 14.6 | 84 |
| Rome—MATISS 87 Survey | 1986–87 | 35–69 | 863 | 11.6 | 40 |
| Rome—MATISS 93 Survey | 1993–95 | 35–69 | 616 | 5.2 | 10 |
| Total | 35–69 | 6865 | 9.1 | 312 |
| Center—cohort . | Baseline examination periods . | Age range (years) . | Sample size (n) . | Median follow-up (years) . | Events (n) . |
|---|---|---|---|---|---|
| Brianza—MONICA 1st Survey | 1986–87 | 35–64 | 573 | 12.1 | 50 |
| Brianza—MONICA 2nd Survey | 1989–90 | 35–64 | 596 | 9.1 | 33 |
| Brianza—MONICA 3rd Survey | 1993–94 | 35–64 | 578 | 4.7 | 16 |
| Brianza—PAMELA Study | 1990–93 | 35–69 | 710 | 7.3 | 29 |
| Friuli—MONICA 1st Survey | 1986–86 | 35–64 | 524 | 12.7 | 26 |
| Friuli—MONICA 2nd Survey | 1989–89 | 35–64 | 347 | 9.6 | 10 |
| Friuli—MONICA 3rd Survey | 1994–94 | 35–64 | 655 | 4.5 | 10 |
| Friuli—Emostatico Study | 1995–96 | 45–64 | 192 | 2.6 | 4 |
| Rome—MATISS 83 Survey | 1983–84 | 35–69 | 1211 | 14.6 | 84 |
| Rome—MATISS 87 Survey | 1986–87 | 35–69 | 863 | 11.6 | 40 |
| Rome—MATISS 93 Survey | 1993–95 | 35–69 | 616 | 5.2 | 10 |
| Total | 35–69 | 6865 | 9.1 | 312 |
Description of the main characteristics of cohorts included in the analysis
| Center—cohort . | Baseline examination periods . | Age range (years) . | Sample size (n) . | Median follow-up (years) . | Events (n) . |
|---|---|---|---|---|---|
| Brianza—MONICA 1st Survey | 1986–87 | 35–64 | 573 | 12.1 | 50 |
| Brianza—MONICA 2nd Survey | 1989–90 | 35–64 | 596 | 9.1 | 33 |
| Brianza—MONICA 3rd Survey | 1993–94 | 35–64 | 578 | 4.7 | 16 |
| Brianza—PAMELA Study | 1990–93 | 35–69 | 710 | 7.3 | 29 |
| Friuli—MONICA 1st Survey | 1986–86 | 35–64 | 524 | 12.7 | 26 |
| Friuli—MONICA 2nd Survey | 1989–89 | 35–64 | 347 | 9.6 | 10 |
| Friuli—MONICA 3rd Survey | 1994–94 | 35–64 | 655 | 4.5 | 10 |
| Friuli—Emostatico Study | 1995–96 | 45–64 | 192 | 2.6 | 4 |
| Rome—MATISS 83 Survey | 1983–84 | 35–69 | 1211 | 14.6 | 84 |
| Rome—MATISS 87 Survey | 1986–87 | 35–69 | 863 | 11.6 | 40 |
| Rome—MATISS 93 Survey | 1993–95 | 35–69 | 616 | 5.2 | 10 |
| Total | 35–69 | 6865 | 9.1 | 312 |
| Center—cohort . | Baseline examination periods . | Age range (years) . | Sample size (n) . | Median follow-up (years) . | Events (n) . |
|---|---|---|---|---|---|
| Brianza—MONICA 1st Survey | 1986–87 | 35–64 | 573 | 12.1 | 50 |
| Brianza—MONICA 2nd Survey | 1989–90 | 35–64 | 596 | 9.1 | 33 |
| Brianza—MONICA 3rd Survey | 1993–94 | 35–64 | 578 | 4.7 | 16 |
| Brianza—PAMELA Study | 1990–93 | 35–69 | 710 | 7.3 | 29 |
| Friuli—MONICA 1st Survey | 1986–86 | 35–64 | 524 | 12.7 | 26 |
| Friuli—MONICA 2nd Survey | 1989–89 | 35–64 | 347 | 9.6 | 10 |
| Friuli—MONICA 3rd Survey | 1994–94 | 35–64 | 655 | 4.5 | 10 |
| Friuli—Emostatico Study | 1995–96 | 45–64 | 192 | 2.6 | 4 |
| Rome—MATISS 83 Survey | 1983–84 | 35–69 | 1211 | 14.6 | 84 |
| Rome—MATISS 87 Survey | 1986–87 | 35–69 | 863 | 11.6 | 40 |
| Rome—MATISS 93 Survey | 1993–95 | 35–69 | 616 | 5.2 | 10 |
| Total | 35–69 | 6865 | 9.1 | 312 |
Person-years, number of events, and age-adjusted 10-year event incident rates, by risk factor categories (the CUORE project)
| Risk factors . | Categories . | Person-years . | No. of events (%) . | Rates (per 100 person-years) . |
|---|---|---|---|---|
| Systolic blood pressure quintiles (mm Hg) | <122 | 13 219 | 34 (11) | 2.3 |
| 122–131 | 13 062 | 48 (16) | 2.9 | |
| 132–140 | 11 237 | 54 (17) | 3.3 | |
| 141–154 | 11 407 | 66 (21) | 3.4 | |
| >154 | 11 315 | 110 (35) | 4.9 | |
| Total cholesterol quintiles (mg/dl) | <190 | 12 319 | 29 (9) | 2.0 |
| 190–212 | 12 103 | 45 (15) | 3.2 | |
| 213–233 | 12 063 | 53 (17) | 3.3 | |
| 234–259 | 11 760 | 73 (23) | 4.4 | |
| >259 | 11 995 | 112 (36) | 6.8 | |
| LDL-cholesterol quintiles (mg/dl) | <113 | 10 026 | 29 (10) | 1.8 |
| 113–133 | 9935 | 31 (12) | 2.0 | |
| 134–151 | 9898 | 54 (20) | 3.4 | |
| 152–174 | 9686 | 58 (22) | 3.5 | |
| >174 | 9589 | 96 (36) | 6.0 | |
| HDL-cholesterol quintiles (mg/dl) | <40 | 13 329 | 77 (25) | 4.1 |
| 40–45 | 11 565 | 68 (22) | 4.0 | |
| 46–52 | 12 696 | 68 (22) | 3.5 | |
| 53–60 | 11 203 | 55 (17) | 3.2 | |
| >60 | 11 447 | 44 (14) | 2.3 | |
| Triglycerides quintiles (mg/dl) | <83 | 10 176 | 40 (14) | 2.4 |
| 83–109 | 10 228 | 58 (21) | 3.4 | |
| 110–142 | 10 088 | 54 (20) | 3.0 | |
| 143–199 | 10 188 | 61 (22) | 3.7 | |
| >199 | 10 039 | 63 (23) | 3.9 | |
| BMI quintiles (kg/m2) | <23.8 | 11 779 | 47 (15) | 2.7 |
| 23.8–25.7 | 11 844 | 60 (19) | 3.4 | |
| 25.8–27.4 | 12 022 | 80 (26) | 4.5 | |
| 27.5–29.5 | 12 049 | 59 (19) | 3.2 | |
| >29.5 | 11 997 | 64 (21) | 3.2 | |
| Cigarette smoking | Never smoker | 14 861 | 39 (12) | 1.9 |
| Past smoker | 21 077 | 111 (36) | 3.0 | |
| Current smoker | 24 301 | 162 (52) | 4.6 | |
| Prevalence of diabetes | No | 57 301 | 283 (91) | 3.3 |
| Yes | 2938 | 29 (9) | 5.1 | |
| Hypertension medications | No | 55 277 | 249 (80) | 3.1 |
| Yes | 4962 | 63 (20) | 6.2 | |
| Family history of CHD | No | 49 805 | 238 (76) | 3.1 |
| Yes | 10 434 | 74 (24) | 4.6 |
| Risk factors . | Categories . | Person-years . | No. of events (%) . | Rates (per 100 person-years) . |
|---|---|---|---|---|
| Systolic blood pressure quintiles (mm Hg) | <122 | 13 219 | 34 (11) | 2.3 |
| 122–131 | 13 062 | 48 (16) | 2.9 | |
| 132–140 | 11 237 | 54 (17) | 3.3 | |
| 141–154 | 11 407 | 66 (21) | 3.4 | |
| >154 | 11 315 | 110 (35) | 4.9 | |
| Total cholesterol quintiles (mg/dl) | <190 | 12 319 | 29 (9) | 2.0 |
| 190–212 | 12 103 | 45 (15) | 3.2 | |
| 213–233 | 12 063 | 53 (17) | 3.3 | |
| 234–259 | 11 760 | 73 (23) | 4.4 | |
| >259 | 11 995 | 112 (36) | 6.8 | |
| LDL-cholesterol quintiles (mg/dl) | <113 | 10 026 | 29 (10) | 1.8 |
| 113–133 | 9935 | 31 (12) | 2.0 | |
| 134–151 | 9898 | 54 (20) | 3.4 | |
| 152–174 | 9686 | 58 (22) | 3.5 | |
| >174 | 9589 | 96 (36) | 6.0 | |
| HDL-cholesterol quintiles (mg/dl) | <40 | 13 329 | 77 (25) | 4.1 |
| 40–45 | 11 565 | 68 (22) | 4.0 | |
| 46–52 | 12 696 | 68 (22) | 3.5 | |
| 53–60 | 11 203 | 55 (17) | 3.2 | |
| >60 | 11 447 | 44 (14) | 2.3 | |
| Triglycerides quintiles (mg/dl) | <83 | 10 176 | 40 (14) | 2.4 |
| 83–109 | 10 228 | 58 (21) | 3.4 | |
| 110–142 | 10 088 | 54 (20) | 3.0 | |
| 143–199 | 10 188 | 61 (22) | 3.7 | |
| >199 | 10 039 | 63 (23) | 3.9 | |
| BMI quintiles (kg/m2) | <23.8 | 11 779 | 47 (15) | 2.7 |
| 23.8–25.7 | 11 844 | 60 (19) | 3.4 | |
| 25.8–27.4 | 12 022 | 80 (26) | 4.5 | |
| 27.5–29.5 | 12 049 | 59 (19) | 3.2 | |
| >29.5 | 11 997 | 64 (21) | 3.2 | |
| Cigarette smoking | Never smoker | 14 861 | 39 (12) | 1.9 |
| Past smoker | 21 077 | 111 (36) | 3.0 | |
| Current smoker | 24 301 | 162 (52) | 4.6 | |
| Prevalence of diabetes | No | 57 301 | 283 (91) | 3.3 |
| Yes | 2938 | 29 (9) | 5.1 | |
| Hypertension medications | No | 55 277 | 249 (80) | 3.1 |
| Yes | 4962 | 63 (20) | 6.2 | |
| Family history of CHD | No | 49 805 | 238 (76) | 3.1 |
| Yes | 10 434 | 74 (24) | 4.6 |
Person-years, number of events, and age-adjusted 10-year event incident rates, by risk factor categories (the CUORE project)
| Risk factors . | Categories . | Person-years . | No. of events (%) . | Rates (per 100 person-years) . |
|---|---|---|---|---|
| Systolic blood pressure quintiles (mm Hg) | <122 | 13 219 | 34 (11) | 2.3 |
| 122–131 | 13 062 | 48 (16) | 2.9 | |
| 132–140 | 11 237 | 54 (17) | 3.3 | |
| 141–154 | 11 407 | 66 (21) | 3.4 | |
| >154 | 11 315 | 110 (35) | 4.9 | |
| Total cholesterol quintiles (mg/dl) | <190 | 12 319 | 29 (9) | 2.0 |
| 190–212 | 12 103 | 45 (15) | 3.2 | |
| 213–233 | 12 063 | 53 (17) | 3.3 | |
| 234–259 | 11 760 | 73 (23) | 4.4 | |
| >259 | 11 995 | 112 (36) | 6.8 | |
| LDL-cholesterol quintiles (mg/dl) | <113 | 10 026 | 29 (10) | 1.8 |
| 113–133 | 9935 | 31 (12) | 2.0 | |
| 134–151 | 9898 | 54 (20) | 3.4 | |
| 152–174 | 9686 | 58 (22) | 3.5 | |
| >174 | 9589 | 96 (36) | 6.0 | |
| HDL-cholesterol quintiles (mg/dl) | <40 | 13 329 | 77 (25) | 4.1 |
| 40–45 | 11 565 | 68 (22) | 4.0 | |
| 46–52 | 12 696 | 68 (22) | 3.5 | |
| 53–60 | 11 203 | 55 (17) | 3.2 | |
| >60 | 11 447 | 44 (14) | 2.3 | |
| Triglycerides quintiles (mg/dl) | <83 | 10 176 | 40 (14) | 2.4 |
| 83–109 | 10 228 | 58 (21) | 3.4 | |
| 110–142 | 10 088 | 54 (20) | 3.0 | |
| 143–199 | 10 188 | 61 (22) | 3.7 | |
| >199 | 10 039 | 63 (23) | 3.9 | |
| BMI quintiles (kg/m2) | <23.8 | 11 779 | 47 (15) | 2.7 |
| 23.8–25.7 | 11 844 | 60 (19) | 3.4 | |
| 25.8–27.4 | 12 022 | 80 (26) | 4.5 | |
| 27.5–29.5 | 12 049 | 59 (19) | 3.2 | |
| >29.5 | 11 997 | 64 (21) | 3.2 | |
| Cigarette smoking | Never smoker | 14 861 | 39 (12) | 1.9 |
| Past smoker | 21 077 | 111 (36) | 3.0 | |
| Current smoker | 24 301 | 162 (52) | 4.6 | |
| Prevalence of diabetes | No | 57 301 | 283 (91) | 3.3 |
| Yes | 2938 | 29 (9) | 5.1 | |
| Hypertension medications | No | 55 277 | 249 (80) | 3.1 |
| Yes | 4962 | 63 (20) | 6.2 | |
| Family history of CHD | No | 49 805 | 238 (76) | 3.1 |
| Yes | 10 434 | 74 (24) | 4.6 |
| Risk factors . | Categories . | Person-years . | No. of events (%) . | Rates (per 100 person-years) . |
|---|---|---|---|---|
| Systolic blood pressure quintiles (mm Hg) | <122 | 13 219 | 34 (11) | 2.3 |
| 122–131 | 13 062 | 48 (16) | 2.9 | |
| 132–140 | 11 237 | 54 (17) | 3.3 | |
| 141–154 | 11 407 | 66 (21) | 3.4 | |
| >154 | 11 315 | 110 (35) | 4.9 | |
| Total cholesterol quintiles (mg/dl) | <190 | 12 319 | 29 (9) | 2.0 |
| 190–212 | 12 103 | 45 (15) | 3.2 | |
| 213–233 | 12 063 | 53 (17) | 3.3 | |
| 234–259 | 11 760 | 73 (23) | 4.4 | |
| >259 | 11 995 | 112 (36) | 6.8 | |
| LDL-cholesterol quintiles (mg/dl) | <113 | 10 026 | 29 (10) | 1.8 |
| 113–133 | 9935 | 31 (12) | 2.0 | |
| 134–151 | 9898 | 54 (20) | 3.4 | |
| 152–174 | 9686 | 58 (22) | 3.5 | |
| >174 | 9589 | 96 (36) | 6.0 | |
| HDL-cholesterol quintiles (mg/dl) | <40 | 13 329 | 77 (25) | 4.1 |
| 40–45 | 11 565 | 68 (22) | 4.0 | |
| 46–52 | 12 696 | 68 (22) | 3.5 | |
| 53–60 | 11 203 | 55 (17) | 3.2 | |
| >60 | 11 447 | 44 (14) | 2.3 | |
| Triglycerides quintiles (mg/dl) | <83 | 10 176 | 40 (14) | 2.4 |
| 83–109 | 10 228 | 58 (21) | 3.4 | |
| 110–142 | 10 088 | 54 (20) | 3.0 | |
| 143–199 | 10 188 | 61 (22) | 3.7 | |
| >199 | 10 039 | 63 (23) | 3.9 | |
| BMI quintiles (kg/m2) | <23.8 | 11 779 | 47 (15) | 2.7 |
| 23.8–25.7 | 11 844 | 60 (19) | 3.4 | |
| 25.8–27.4 | 12 022 | 80 (26) | 4.5 | |
| 27.5–29.5 | 12 049 | 59 (19) | 3.2 | |
| >29.5 | 11 997 | 64 (21) | 3.2 | |
| Cigarette smoking | Never smoker | 14 861 | 39 (12) | 1.9 |
| Past smoker | 21 077 | 111 (36) | 3.0 | |
| Current smoker | 24 301 | 162 (52) | 4.6 | |
| Prevalence of diabetes | No | 57 301 | 283 (91) | 3.3 |
| Yes | 2938 | 29 (9) | 5.1 | |
| Hypertension medications | No | 55 277 | 249 (80) | 3.1 |
| Yes | 4962 | 63 (20) | 6.2 | |
| Family history of CHD | No | 49 805 | 238 (76) | 3.1 |
| Yes | 10 434 | 74 (24) | 4.6 |
Tables 3 and 4 present the values of the coefficients estimated in the CUORE dataset, according to risk factor classifications of the two referent studies (FHS and PROCAM study). No statistically significant differences in risk factor coefficients have been found between CUORE and FHS, with the exception of age and the higher cholesterol levels (>240 mg/dl). Instead, in addition to age, HDL-cholesterol and triglycerides coefficients differed between the CUORE and PROCAM equations.
Comparison of proportional hazard predictive coefficients in the FHS and those calculated in the CUORE dataset
| . | FHS . | . | CUORE . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||||
| Age (years) | 0.049 | 0.005 | 0.071 | 0.007 | 2.56* | |||||
| Blood pressure | ||||||||||
| Normal including optimal (S < 130, D < 85) | Reference | Reference | ||||||||
| High normal (S < 140, D < 90) | 0.270 | 0.151 | 0.308 | 0.195 | 0.15 | |||||
| Stage I hypertension (S < 160, D < 100) | 0.513 | 0.136 | 0.141 | 0.176 | −1.67 | |||||
| Stage II–IV hypertension (S > 160, D > 100) | 0.610 | 0.154 | 0.515 | 0.175 | −0.41 | |||||
| Current smoking (%) | 0.519 | 0.104 | 0.534 | 0.114 | 0.10 | |||||
| Diabetes (%) | 0.405 | 0.179 | 0.495 | 0.193 | 0.34 | |||||
| Total cholesterol (mg/dl) | ||||||||||
| <200 | Reference | Reference | ||||||||
| 200–240 | 0.270 | 0.127 | 0.653 | 0.182 | 1.73 | |||||
| ≥240 | 0.642 | 0.134 | 1.110 | 0.174 | 2.13* | |||||
| HDL-cholesterol (mg/dl) | ||||||||||
| <35 | 0.385 | 0.120 | −0.011 | 0.195 | −1.73 | |||||
| 35–60 | Reference | Reference | ||||||||
| ≥60 | −0.580 | 0.201 | −0.525 | 0.156 | 0.22 | |||||
| . | FHS . | . | CUORE . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||||
| Age (years) | 0.049 | 0.005 | 0.071 | 0.007 | 2.56* | |||||
| Blood pressure | ||||||||||
| Normal including optimal (S < 130, D < 85) | Reference | Reference | ||||||||
| High normal (S < 140, D < 90) | 0.270 | 0.151 | 0.308 | 0.195 | 0.15 | |||||
| Stage I hypertension (S < 160, D < 100) | 0.513 | 0.136 | 0.141 | 0.176 | −1.67 | |||||
| Stage II–IV hypertension (S > 160, D > 100) | 0.610 | 0.154 | 0.515 | 0.175 | −0.41 | |||||
| Current smoking (%) | 0.519 | 0.104 | 0.534 | 0.114 | 0.10 | |||||
| Diabetes (%) | 0.405 | 0.179 | 0.495 | 0.193 | 0.34 | |||||
| Total cholesterol (mg/dl) | ||||||||||
| <200 | Reference | Reference | ||||||||
| 200–240 | 0.270 | 0.127 | 0.653 | 0.182 | 1.73 | |||||
| ≥240 | 0.642 | 0.134 | 1.110 | 0.174 | 2.13* | |||||
| HDL-cholesterol (mg/dl) | ||||||||||
| <35 | 0.385 | 0.120 | −0.011 | 0.195 | −1.73 | |||||
| 35–60 | Reference | Reference | ||||||||
| ≥60 | −0.580 | 0.201 | −0.525 | 0.156 | 0.22 | |||||
0.01 < P < 0.05.
Comparison of proportional hazard predictive coefficients in the FHS and those calculated in the CUORE dataset
| . | FHS . | . | CUORE . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||||
| Age (years) | 0.049 | 0.005 | 0.071 | 0.007 | 2.56* | |||||
| Blood pressure | ||||||||||
| Normal including optimal (S < 130, D < 85) | Reference | Reference | ||||||||
| High normal (S < 140, D < 90) | 0.270 | 0.151 | 0.308 | 0.195 | 0.15 | |||||
| Stage I hypertension (S < 160, D < 100) | 0.513 | 0.136 | 0.141 | 0.176 | −1.67 | |||||
| Stage II–IV hypertension (S > 160, D > 100) | 0.610 | 0.154 | 0.515 | 0.175 | −0.41 | |||||
| Current smoking (%) | 0.519 | 0.104 | 0.534 | 0.114 | 0.10 | |||||
| Diabetes (%) | 0.405 | 0.179 | 0.495 | 0.193 | 0.34 | |||||
| Total cholesterol (mg/dl) | ||||||||||
| <200 | Reference | Reference | ||||||||
| 200–240 | 0.270 | 0.127 | 0.653 | 0.182 | 1.73 | |||||
| ≥240 | 0.642 | 0.134 | 1.110 | 0.174 | 2.13* | |||||
| HDL-cholesterol (mg/dl) | ||||||||||
| <35 | 0.385 | 0.120 | −0.011 | 0.195 | −1.73 | |||||
| 35–60 | Reference | Reference | ||||||||
| ≥60 | −0.580 | 0.201 | −0.525 | 0.156 | 0.22 | |||||
| . | FHS . | . | CUORE . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||||
| Age (years) | 0.049 | 0.005 | 0.071 | 0.007 | 2.56* | |||||
| Blood pressure | ||||||||||
| Normal including optimal (S < 130, D < 85) | Reference | Reference | ||||||||
| High normal (S < 140, D < 90) | 0.270 | 0.151 | 0.308 | 0.195 | 0.15 | |||||
| Stage I hypertension (S < 160, D < 100) | 0.513 | 0.136 | 0.141 | 0.176 | −1.67 | |||||
| Stage II–IV hypertension (S > 160, D > 100) | 0.610 | 0.154 | 0.515 | 0.175 | −0.41 | |||||
| Current smoking (%) | 0.519 | 0.104 | 0.534 | 0.114 | 0.10 | |||||
| Diabetes (%) | 0.405 | 0.179 | 0.495 | 0.193 | 0.34 | |||||
| Total cholesterol (mg/dl) | ||||||||||
| <200 | Reference | Reference | ||||||||
| 200–240 | 0.270 | 0.127 | 0.653 | 0.182 | 1.73 | |||||
| ≥240 | 0.642 | 0.134 | 1.110 | 0.174 | 2.13* | |||||
| HDL-cholesterol (mg/dl) | ||||||||||
| <35 | 0.385 | 0.120 | −0.011 | 0.195 | −1.73 | |||||
| 35–60 | Reference | Reference | ||||||||
| ≥60 | −0.580 | 0.201 | −0.525 | 0.156 | 0.22 | |||||
0.01 < P < 0.05.
Comparison of proportional hazard predictive coefficients in the PROCAM study and those calculated in the CUORE dataset
| . | PROCAM . | . | CUORE . | . | . | |||
|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||
| Age (years) | 0.103 | 0.008 | 0.062 | 0.008 | −3.62* | |||
| LDL-cholesterol (mg/dl) | 0.013 | 0.001 | 0.012 | 0.001 | 20.71 | |||
| HDL-cholesterol (mg/dl) | −0.032 | 0.006 | −0.011 | 0.005 | 2.69** | |||
| ln Triglycerides (mg/dl) | 0.317 | 0.134 | −0.089 | 0.154 | −1.99*** | |||
| Systolic blood pressure (mm Hg) | 0.010 | 0.003 | 0.012 | 0.003 | 0.47 | |||
| Current smoking (%) | 0.658 | 0.113 | 0.543 | 0.124 | −0.69 | |||
| Family history of MI (%) | 0.382 | 0.135 | 0.290 | 0.142 | −0.47 | |||
| Diabetes (%) | 0.399 | 0.158 | 0.280 | 0.217 | −0.44 | |||
| . | PROCAM . | . | CUORE . | . | . | |||
|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||
| Age (years) | 0.103 | 0.008 | 0.062 | 0.008 | −3.62* | |||
| LDL-cholesterol (mg/dl) | 0.013 | 0.001 | 0.012 | 0.001 | 20.71 | |||
| HDL-cholesterol (mg/dl) | −0.032 | 0.006 | −0.011 | 0.005 | 2.69** | |||
| ln Triglycerides (mg/dl) | 0.317 | 0.134 | −0.089 | 0.154 | −1.99*** | |||
| Systolic blood pressure (mm Hg) | 0.010 | 0.003 | 0.012 | 0.003 | 0.47 | |||
| Current smoking (%) | 0.658 | 0.113 | 0.543 | 0.124 | −0.69 | |||
| Family history of MI (%) | 0.382 | 0.135 | 0.290 | 0.142 | −0.47 | |||
| Diabetes (%) | 0.399 | 0.158 | 0.280 | 0.217 | −0.44 | |||
P < 0.001
0.001 < P < 0.01
0.01 < P < 0.05.
Comparison of proportional hazard predictive coefficients in the PROCAM study and those calculated in the CUORE dataset
| . | PROCAM . | . | CUORE . | . | . | |||
|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||
| Age (years) | 0.103 | 0.008 | 0.062 | 0.008 | −3.62* | |||
| LDL-cholesterol (mg/dl) | 0.013 | 0.001 | 0.012 | 0.001 | 20.71 | |||
| HDL-cholesterol (mg/dl) | −0.032 | 0.006 | −0.011 | 0.005 | 2.69** | |||
| ln Triglycerides (mg/dl) | 0.317 | 0.134 | −0.089 | 0.154 | −1.99*** | |||
| Systolic blood pressure (mm Hg) | 0.010 | 0.003 | 0.012 | 0.003 | 0.47 | |||
| Current smoking (%) | 0.658 | 0.113 | 0.543 | 0.124 | −0.69 | |||
| Family history of MI (%) | 0.382 | 0.135 | 0.290 | 0.142 | −0.47 | |||
| Diabetes (%) | 0.399 | 0.158 | 0.280 | 0.217 | −0.44 | |||
| . | PROCAM . | . | CUORE . | . | . | |||
|---|---|---|---|---|---|---|---|---|
. | b . | SE . | b . | SE . | Z . | |||
| Age (years) | 0.103 | 0.008 | 0.062 | 0.008 | −3.62* | |||
| LDL-cholesterol (mg/dl) | 0.013 | 0.001 | 0.012 | 0.001 | 20.71 | |||
| HDL-cholesterol (mg/dl) | −0.032 | 0.006 | −0.011 | 0.005 | 2.69** | |||
| ln Triglycerides (mg/dl) | 0.317 | 0.134 | −0.089 | 0.154 | −1.99*** | |||
| Systolic blood pressure (mm Hg) | 0.010 | 0.003 | 0.012 | 0.003 | 0.47 | |||
| Current smoking (%) | 0.658 | 0.113 | 0.543 | 0.124 | −0.69 | |||
| Family history of MI (%) | 0.382 | 0.135 | 0.290 | 0.142 | −0.47 | |||
| Diabetes (%) | 0.399 | 0.158 | 0.280 | 0.217 | −0.44 | |||
P < 0.001
0.001 < P < 0.01
0.01 < P < 0.05.
Table 5) reports the coefficients, the corresponding hazard ratios (and 95% CIs) for the risk factors included in the best CUORE equation and the 10-year survival probability at the mean value of the risk factors. In addition to the risk factors of the basic model (age in years, total cholesterol in mg/dl, systolic blood pressure in mm Hg, smoking status), the best CUORE equation included: diabetes mellitus, HDL-cholesterol (in mg/dl), hypertension medications, and family history of premature CHD. This model increased the AUC, assessed on the same dataset, from 0.731 for the basic model to 0.750 for the final best model. BMI was not included because it did not improve predictive accuracy and its coefficient was never statistically significant.
The best CUORE prediction equation for 35–69 years old Italian men
. | Mean or proportion (SD) . | β-Coefficient . | P . | Hazard ratio . | 95% CI . |
|---|---|---|---|---|---|
| Age (years) | 50.8 (9.2) | 0.06318 | <0.0001 | 1.065 | 1.050–1.081 |
| Systolic blood pressure (10 mm Hg) | 138.5 (20.5) | 0.08800 | 0.0014 | 1.092 | 1.086–1.098 |
| Current cigarette smoking (yes/no) | 0.39 (0.49) | 0.62903 | <0.0001 | 1.876 | 1.495–2.353 |
| Total cholesterol (10 mg/dl) | 224.7 (43.7) | 0.08900 | <0.0001 | 1.093 | 1.091–1.096 |
| HDL-cholesterol (10 mg/dl) | 50.2 (13.9) | −0.12340 | 0.0044 | 0.884 | 0.876–0.891 |
| Diabetes (yes/no) | 0.05 (0.22) | 0.41956 | 0.0331 | 1.521 | 1.034–2.238 |
| Hypertension medications (yes/no) | 0.10 (0.30) | 0.60611 | <0.0001 | 1.833 | 1.354–2.483 |
| Family history of CHD (yes/no) | 0.17 (0.37) | 0.32015 | 0.0169 | 1.377 | 1.059–1.791 |
| Baseline 10-year event-free survivala | 0.96586 |
. | Mean or proportion (SD) . | β-Coefficient . | P . | Hazard ratio . | 95% CI . |
|---|---|---|---|---|---|
| Age (years) | 50.8 (9.2) | 0.06318 | <0.0001 | 1.065 | 1.050–1.081 |
| Systolic blood pressure (10 mm Hg) | 138.5 (20.5) | 0.08800 | 0.0014 | 1.092 | 1.086–1.098 |
| Current cigarette smoking (yes/no) | 0.39 (0.49) | 0.62903 | <0.0001 | 1.876 | 1.495–2.353 |
| Total cholesterol (10 mg/dl) | 224.7 (43.7) | 0.08900 | <0.0001 | 1.093 | 1.091–1.096 |
| HDL-cholesterol (10 mg/dl) | 50.2 (13.9) | −0.12340 | 0.0044 | 0.884 | 0.876–0.891 |
| Diabetes (yes/no) | 0.05 (0.22) | 0.41956 | 0.0331 | 1.521 | 1.034–2.238 |
| Hypertension medications (yes/no) | 0.10 (0.30) | 0.60611 | <0.0001 | 1.833 | 1.354–2.483 |
| Family history of CHD (yes/no) | 0.17 (0.37) | 0.32015 | 0.0169 | 1.377 | 1.059–1.791 |
| Baseline 10-year event-free survivala | 0.96586 |
10-year survival at the mean of the risk factors.
The best CUORE prediction equation for 35–69 years old Italian men
. | Mean or proportion (SD) . | β-Coefficient . | P . | Hazard ratio . | 95% CI . |
|---|---|---|---|---|---|
| Age (years) | 50.8 (9.2) | 0.06318 | <0.0001 | 1.065 | 1.050–1.081 |
| Systolic blood pressure (10 mm Hg) | 138.5 (20.5) | 0.08800 | 0.0014 | 1.092 | 1.086–1.098 |
| Current cigarette smoking (yes/no) | 0.39 (0.49) | 0.62903 | <0.0001 | 1.876 | 1.495–2.353 |
| Total cholesterol (10 mg/dl) | 224.7 (43.7) | 0.08900 | <0.0001 | 1.093 | 1.091–1.096 |
| HDL-cholesterol (10 mg/dl) | 50.2 (13.9) | −0.12340 | 0.0044 | 0.884 | 0.876–0.891 |
| Diabetes (yes/no) | 0.05 (0.22) | 0.41956 | 0.0331 | 1.521 | 1.034–2.238 |
| Hypertension medications (yes/no) | 0.10 (0.30) | 0.60611 | <0.0001 | 1.833 | 1.354–2.483 |
| Family history of CHD (yes/no) | 0.17 (0.37) | 0.32015 | 0.0169 | 1.377 | 1.059–1.791 |
| Baseline 10-year event-free survivala | 0.96586 |
. | Mean or proportion (SD) . | β-Coefficient . | P . | Hazard ratio . | 95% CI . |
|---|---|---|---|---|---|
| Age (years) | 50.8 (9.2) | 0.06318 | <0.0001 | 1.065 | 1.050–1.081 |
| Systolic blood pressure (10 mm Hg) | 138.5 (20.5) | 0.08800 | 0.0014 | 1.092 | 1.086–1.098 |
| Current cigarette smoking (yes/no) | 0.39 (0.49) | 0.62903 | <0.0001 | 1.876 | 1.495–2.353 |
| Total cholesterol (10 mg/dl) | 224.7 (43.7) | 0.08900 | <0.0001 | 1.093 | 1.091–1.096 |
| HDL-cholesterol (10 mg/dl) | 50.2 (13.9) | −0.12340 | 0.0044 | 0.884 | 0.876–0.891 |
| Diabetes (yes/no) | 0.05 (0.22) | 0.41956 | 0.0331 | 1.521 | 1.034–2.238 |
| Hypertension medications (yes/no) | 0.10 (0.30) | 0.60611 | <0.0001 | 1.833 | 1.354–2.483 |
| Family history of CHD (yes/no) | 0.17 (0.37) | 0.32015 | 0.0169 | 1.377 | 1.059–1.791 |
| Baseline 10-year event-free survivala | 0.96586 |
10-year survival at the mean of the risk factors.
The results of the prediction accuracy assessment of the considered study equations are reported in Table 6), with the CUORE equation coefficients estimated from a random half of the data and AUC estimated for all equations on the other half. The FHS and PROCAM equations showed somewhat lower AUC values in comparison with the CUORE equation, but the differences were not statistically significant (data not shown).
Summary of risk prediction accuracy assessments for different equations
| . | Discriminationa . | . | Overall calibrationc . | . | Deciles calibratione (HLftest) . | . | . | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Risk prediction equations . | AUCb . | 95%CI . | Survivald . | 95%CI . | All cohorts . | North cohorts . | South cohorts . | ||||
| FHS original | 0.093 | 0.087–0.099 | 419.0 | 164.4 | 262.9 | ||||||
| FHS recalibrated—D'Agostino | 0.723 | 0.670–0.779 | 0.014 | 0.008–0.021 | 27.1 | 14.8 | 31.6 | ||||
| FHS recalibrated—Chambless | 20.000 | 20.007–0.006 | 19.9 | 33.8 | 13.2 | ||||||
| PROCAM study original | 0.109 | 0.100–0.116 | 797.0 | 299.4 | 516.3 | ||||||
| PROCAM recalibrated—D'Agostino | 0.735 | 0.678–0.790 | 0.047 | 0.038–0.054 | 220.3 | 72.3 | 168.7 | ||||
| PROCAM recalibrated—Chambless | 20.000 | 20.008–0.007 | 53.0 | 62.9 | 32.5 | ||||||
| CUORE study | 0.742 | 0.684–0.796 | — | — | 15.5 | 27.3 | 9.7 | ||||
| . | Discriminationa . | . | Overall calibrationc . | . | Deciles calibratione (HLftest) . | . | . | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Risk prediction equations . | AUCb . | 95%CI . | Survivald . | 95%CI . | All cohorts . | North cohorts . | South cohorts . | ||||
| FHS original | 0.093 | 0.087–0.099 | 419.0 | 164.4 | 262.9 | ||||||
| FHS recalibrated—D'Agostino | 0.723 | 0.670–0.779 | 0.014 | 0.008–0.021 | 27.1 | 14.8 | 31.6 | ||||
| FHS recalibrated—Chambless | 20.000 | 20.007–0.006 | 19.9 | 33.8 | 13.2 | ||||||
| PROCAM study original | 0.109 | 0.100–0.116 | 797.0 | 299.4 | 516.3 | ||||||
| PROCAM recalibrated—D'Agostino | 0.735 | 0.678–0.790 | 0.047 | 0.038–0.054 | 220.3 | 72.3 | 168.7 | ||||
| PROCAM recalibrated—Chambless | 20.000 | 20.008–0.007 | 53.0 | 62.9 | 32.5 | ||||||
| CUORE study | 0.742 | 0.684–0.796 | — | — | 15.5 | 27.3 | 9.7 | ||||
From the slip-sample approach (1000 resamples).
AUC, area under ROC curve.
From the bootstrap method (1000 resamples).
Difference between means of 10-year predicted survival (based on study risk equations) and Kaplan–Meier survival observed in CUORE.
Deciles for the entire CUORE dataset.
HL χ2 test (a value exceeding 20 is considered an index of poor calibration).
Summary of risk prediction accuracy assessments for different equations
| . | Discriminationa . | . | Overall calibrationc . | . | Deciles calibratione (HLftest) . | . | . | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Risk prediction equations . | AUCb . | 95%CI . | Survivald . | 95%CI . | All cohorts . | North cohorts . | South cohorts . | ||||
| FHS original | 0.093 | 0.087–0.099 | 419.0 | 164.4 | 262.9 | ||||||
| FHS recalibrated—D'Agostino | 0.723 | 0.670–0.779 | 0.014 | 0.008–0.021 | 27.1 | 14.8 | 31.6 | ||||
| FHS recalibrated—Chambless | 20.000 | 20.007–0.006 | 19.9 | 33.8 | 13.2 | ||||||
| PROCAM study original | 0.109 | 0.100–0.116 | 797.0 | 299.4 | 516.3 | ||||||
| PROCAM recalibrated—D'Agostino | 0.735 | 0.678–0.790 | 0.047 | 0.038–0.054 | 220.3 | 72.3 | 168.7 | ||||
| PROCAM recalibrated—Chambless | 20.000 | 20.008–0.007 | 53.0 | 62.9 | 32.5 | ||||||
| CUORE study | 0.742 | 0.684–0.796 | — | — | 15.5 | 27.3 | 9.7 | ||||
| . | Discriminationa . | . | Overall calibrationc . | . | Deciles calibratione (HLftest) . | . | . | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Risk prediction equations . | AUCb . | 95%CI . | Survivald . | 95%CI . | All cohorts . | North cohorts . | South cohorts . | ||||
| FHS original | 0.093 | 0.087–0.099 | 419.0 | 164.4 | 262.9 | ||||||
| FHS recalibrated—D'Agostino | 0.723 | 0.670–0.779 | 0.014 | 0.008–0.021 | 27.1 | 14.8 | 31.6 | ||||
| FHS recalibrated—Chambless | 20.000 | 20.007–0.006 | 19.9 | 33.8 | 13.2 | ||||||
| PROCAM study original | 0.109 | 0.100–0.116 | 797.0 | 299.4 | 516.3 | ||||||
| PROCAM recalibrated—D'Agostino | 0.735 | 0.678–0.790 | 0.047 | 0.038–0.054 | 220.3 | 72.3 | 168.7 | ||||
| PROCAM recalibrated—Chambless | 20.000 | 20.008–0.007 | 53.0 | 62.9 | 32.5 | ||||||
| CUORE study | 0.742 | 0.684–0.796 | — | — | 15.5 | 27.3 | 9.7 | ||||
From the slip-sample approach (1000 resamples).
AUC, area under ROC curve.
From the bootstrap method (1000 resamples).
Difference between means of 10-year predicted survival (based on study risk equations) and Kaplan–Meier survival observed in CUORE.
Deciles for the entire CUORE dataset.
HL χ2 test (a value exceeding 20 is considered an index of poor calibration).
A bootstrap test reveals that the uncalibrated estimates of the 10-year risk in this CUORE follow-up data were 0.093 and 0.109 higher from the Framingham and PROCAM risk scores, respectively, as applied to CUORE, than the Kaplan–Meier estimate for CUORE. The difference between the average estimates of the risk given by the Kaplan–Meier estimates for CUORE and the recalibrated FHS and PROCAM equations continue to be statistically significant when the D'Agostino method is adopted. With the Chambless alternative recalibration method the difference in survival estimates are smaller, indicating an improved overall calibration.
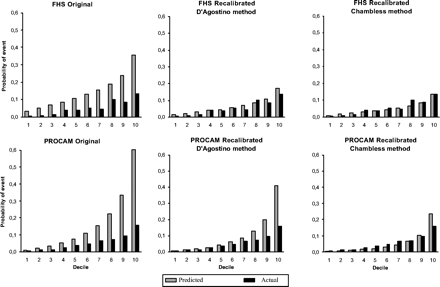
Even when the overall calibration is successfully achieved, residual unbalances may persist between predicted and observed risk estimates at different risk levels (i.e. selective over- or under-estimates at low- or high-risk levels), and this is reflected in Table 6) in the HL statistics for all the equations considered, calculated on the entire CUORE dataset and separately for the northern and the southern cohorts. Discrepancies between predicted and actual risk are also graphically shown in Figure 1, for the entire CUORE cohort. Clear overestimates of the risk are present in particular in the higher-risk deciles for both the FHS and the PROCAM original study equations. With the D'Agostino recalibration method the risk overestimates equation decreased consistently, but remained quite high for the PROCAM equation. This is in part due to the non-effective overall recalibration. Overestimates of both FHS and PROCAM equations were further reduced when the equations were recalibrated using the alternative method, but for PROCAM equation residual overestimates at the highest-risk deciles remained (balanced by small but consistent underestimates in the lower-risk deciles). The CUORE equation reveals more accurate prediction of risk within deciles of risk not only when applied to the entire database, but also to the northern and southern cohorts.
Predicted and actual 10-year risk of incident major coronary events, for deciles of risk estimated by the Framingham and the PROCAM equations, in the CUORE dataset.
Discussion
The CUORE equation for prediction of coronary events takes into consideration a wider number of risk factors, includes subjects from the north and the centre–south of the country and non-fatal and fatal validated major coronary events as the endpoint. In addition, the cohort recruitment periods, the age range of subjects, and the length of follow-up allow direct comparisons with the equations reported by reference studies.2,6 Only 35–69-year-old subjects were included because this was the age range common to most cohorts included in the analysis. The exclusion of women is a limitation of this study, but the small number of events did not allow stable risk estimates (n = 103 events, median follow-up 4.9 years, with a rate of 1.2 per 1000 person-years). An extension of the follow-up period is underway and more stable estimates will be available for women.
The CUORE equation includes well-known risk factors for CHDs: age, total cholesterol, systolic blood pressure, cigarette smoking, HDL cholesterol, diabetes mellitus, hypertension drug treatment, and family history of CHD. In contrast to previous Italian predictive equations31 BMI was not an independent risk factor, nor did it improve predictive accuracy. Presumably the residual impact of BMI is minor when several other risk factors are considered into the model, due to the association of obesity with diabetes, higher total cholesterol, blood pressure, and lower HDL-cholesterol levels.32 In the CUORE model, hypertension medication emerged as an independent risk factor, as reported in other studies.5 This finding may be explained by the fact that, for a given current blood pressure level, persons on drug treatment for hypertension have a history of previously higher BP than those without drug treatment.
Absolute risk estimates require a complete case finding in the follow-up and representative samples, which are directly related to participation rates in population-based samples. In the CUORE study, we calculated the age-standardized incidence ratio (SIR) between observed and expected events, the latter estimated from 5-year age-specific and gender-specific rates provided by MONICA registers.33 The overall SIR values for all the cohorts was 101.2% indicating a good coverage of the case finding in the follow-up. Nevertheless, some cohorts with a low participation rate at baseline (around 65%) reported somewhat lower SIR values (around 90%). Non-responders to population surveys have a higher probability of dying in the follow-up than responders (non-participation bias34) and that may produce underestimates in absolute risk. In a small sample (n = 406) of the PAMELA Study of non-responding men, the age-adjusted relative risks were 1.5 for all-causes of death and 1.2 for coronary death in comparison with responders (R. Sega, unpublished data), indicating that for CHDs the bias in our study may be smaller than expected.
Predictive discrimination, as measured by the area under the ROC curve, resulted in similar values for the CUORE, FHS, and PROCAM equations. However, the original Framingham and PROCAM equations showed considerable discrepancies between the observed and the predicted 10-year risk of CHD in the CUORE data. The recalibration method proposed by D'Agostino produces a substantial enhancement in calibration of the FHS equation, but smaller improvements of the PROCAM equation as evidenced by the larger values of the HL statistic, i.e. the smaller agreement between observed and expected number of events by deciles of risk. For the latter equation the relative degree of overestimation in the CUORE dataset is not equally distributed among coronary risk levels, as indicated by the HL statistics. The risk overestimates using the recalibrated PROCAM equation are greater in the upper-risk deciles, where threshold values presently adopted for drug treatments for hypertension and hypercholesterolaemia are more likely to be placed. The alternative method of recalibration28 improves the risk estimates also of the PROCAM equation. The important point is that a cohort study in a low incidence country was needed to obtain a properly calibrated risk equation. Simply applying the PROCAM equation, recalibrated using crude estimates of population 10-year risk for persons at mean risk levels, was not sufficient to improve the risk estimation.
Apparently the forced inclusion of triglycerides (present in the PROCAM equation) almost nullifies the protective effect of HDL-cholesterol in the CUORE data, a powerful protective factor in low CHD incidence populations.35 Moreover, recently published US pooled analyses did not show improvements in the discrimination function between controls and CHD cases when triglycerides are included in the model.36 The CUORE equation is specific for CHDs, and therefore no direct comparisons can be done with cardiovascular death prediction equation.7 For the ongoing discussion of the assessment of cardiovascular risk, this paper represents a contribution whose function, calibration to current regional or local event rates and risk profiles, is deemed as indispensable.37
In conclusion, the 10-year CUORE Cohort Study predictive equation of first major coronary events shows similar discrimination as the FHS and PROCAM equations and avoids the risk overestimates, produced not only by the original equations but also when standard recalibration procedures are adopted. In addition, since the CUORE equation reveals better accuracy in comparison with the FHS and PROCAM recalibrated equations, even when applied separately to the northern and southern CUORE cohorts, it may be adopted to identify high coronary risk adult men from low incidence populations, if further validated in other low-risk populations.
The CUORE study is a prospective fixed-cohort study, including cohorts from the north and the centre–south of Italy.
Among 6865 men, aged 35–69 years, CHD-free at baseline, in 9.1 years median follow-up 312 first fatal and non-fatal major coronary events occurred.
The CUORE predictive equation, which includes age, total cholesterol, systolic blood pressure, cigarette smoking, HDL-cholesterol, diabetes mellitus, hypertension drug treatment, and family history of CHD, showed better accuracy than the Framingham and the PROCAM equations, overcoming frequently reported risk overestimates.
The Progetto CUORE Research Group: MM Ferrario, G Cesana, R Sega, P Chiodini, S Sarman, C Fornari, G Corrao, L Bolognesi, Centro Ricerche Patologia Cronico-degenerativa, Università degli Studi Milano-Bicocca, Monza; D Vanuzzo, L Pilotto, T Feresin, K Mauro, M Martini, F Mattiussi, G Picco, Cardiovascular Prevention Centre, Azienda Socio-Sanitaria 4 Medio Friuli and Agenzia Regionale della Sanità, Udine; S Panico, E Celentano, A Mattiello, R Galasso, M Del Pezzo, M Santucci de Magistris, Università degli Studi Federico II, Naples; S Giampaoli, L Palmieri, F Dima, C Lo Noce, A Santaquilani, P Caiola De Sanctis, F Pannozzo, F Seccareccia, Centro Nazionale di Epidemiologia, Sorveglianza e Promozione della Salute, Istituto Superiore di Sanità, Rome, Italy.
The CUORE Project was supported with grants from the Italian Ministry of Health and co-ordinated by the Centro di Epidemiologia, Sorveglianza e Promozione della Salute dell‘Istituto Superiore di Sanità, Roma.
References
Martin MJ, Hulley SB, Browner WS et al. Serum cholesterol, blood pressure, and mortality implications from a cohort of 361,662 men.
Wilson PWF, D'Agostino RB, Levy D et al. Prediction of coronary heart disease using risk factor categories.
Jackson R. Guidelines on preventing cardiovascular disease in clinical practice.
Prevention of coronary heart disease in clinical practice. Recommendations of the second Joint Task Force of European and other Societies on Coronary Prevention.
Executive Summary of the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III).
Assmann G, Cullen P, Schulte H. Simple scoring scheme for calculating the risk of acute coronary events based on the 10-year follow-up of the Prospective Cardiovascular Munster (PROCAM) Study.
Conroy RM, Pyörälä K, Fitzgerald AP et al. on behalf of the SCORE project group. Estimation of ten year risk of fatal cardiovascular disease in Europe: the SCORE project.
Liao Y, McGee DL, Cooper RS et al. How generalizable are coronary risk prediction models? Comparison of Framingham and two national cohorts.
Menotti A, Keys A, Blackburn H et al. Comparison of multivariate predictive power of major risk factors for coronary heart disease in different countries: results from eight nations of the Seven Countries Study, 25-year follow-up.
The BMI and Mortality in Diverse Population Collaborative Group. Prediction of mortality from Coronary Heart Disease among Diverse Populations. Is there a common predictive function?
Hense HW, Schulte H, Löwel H, Assmann G, Keil U. Framingham risk function overestimates risk of coronary heart disease in men and women from Germany-results from the MONICA Augsburg and PROCAM cohorts.
Brindle P, Emberson J, Lampe F et al. Predictive accuracy of the Framingham coronary risk score in British men: prospective cohort study.
Chambless LE, Dobson AJ, Patterson CC et al. On the use of a logistic score in predicting risk of coronary heart disease.
D'Agostino RB, Grundy S, Sullivan LM et al. Validation of the Framingham Coronary Heart Disease Prediction Scores. Results of a Multiple Ethnic Groups Investigation.
Marrugat J, D'Agostino R, Sullivan L et al. An adaptation of the Framingham coronary heart disease risk function to European Mediterranean areas.
Empana JP, Ducimetière P, Arveiler D et al. Are the Framingham and PROCAM coronary heart disease risk functions applicable to different European populations?
Menotti A, Lanti M, Puddu PE et al. Coronary heart disease incidence in northern and southern European populations: a reanalysis of the seven countries study for a European coronary risk chart.
Menotti A, Farchi G, Seccareccia F, the RIFLE Research Group. The prediction of coronary heart disease mortality as a function of major risk factors in over 30,000 men in the Italian Rifle Pooling Project (Risk factors and life expectancy). A comparison with the MRFIT primary screenees.
Ferrario M, Sega R, Chatenoud L et al. Time trends of major coronary risk factors in a northern Italian population (1986–1994). How remarkable are socio-economic differences in an industrialised low CHD incidence country?
Cesana GC, De Vito G, Ferrario M et al. Ambulatory blood pressure normalcy: The PAMELA Study.
Giampaoli S, Poce A, Sciarra F et al. Change in cardiovascular risk factors during a 10-year community intervention program.
Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge.
Fornari C, Bagnardi V, Corrao G et al. Record linkage procedures to detect cardiovascular endpoints in follow-up studies (abstract).
Tunstall-Pedoe H for the WHO MONICA Project. The World Health Organization MONICA Project (Monitoring Trends and Determinants in Cardiovascular Disease): A major international collaboration.
Wilcosky T, Chambless LE. A comparison of direct adjustment and regression adjustment of proportions and rates.
Kleinbaum D, Kupper L, Muller K. Applied Regression Analysis and other Multivariable Regression Methods. 2nd edn. Boston: PWS-KENT Publishing Company,
Campbell G. General methodology I: advances in statistical methodology for the evaluation of diagnostic laboratory tests.
Chambless LE, Heiss G, Shahar E, Earp MJ, Toole J. Prediction of ischemic stroke risk in the atherosclerosis risk in communities study.
DiCiccio TJ, Efron B. Bootstrap confidence intervals. Technical Report No. 175, Division of Biostatistics, Stanford University,
Menotti A, Seccareccia F, Blackburn H, Keys A. Coronary mortality and its prediction in samples of US and Italian railroad employees in 25 years within the Seven Countires Study of cardiovascular diseases.
Anderson KM, Odell PM, Wilson PWF et al. Cardiovascular risk profiles.
Ferrario M, Cesana GC, Vanuzzo D et al. Surveillance of ischaemic heart disease: results from the Italian MONICA populations.
Belfante R, Reed D, MacLean C et al. Response bias in the Honolulu Heart Program.
Ferrario M, Cesana GC, Heiss G et al. Demographic and behavioral correlates of high density lipoprotein cholesterol. An international comparison between Northern Italy and the United States.
Avins AL, Neuhaus JM. Do triglycerides provide meaningful information about heart disease risk?