Abstract
This study focuses on the co-engineering of salbutamol sulphate (SS), a common bronchodilator, and mannitol (MA), a mucolytic, as a potential combination therapy for mucus hypersecretion. This combination was chosen to have a synergic effect on the airways: the SS will act on the β2-receptor for relaxation of smooth muscle and enhancement of ciliary beat frequency, whilst mannitol will improve the fluidity of mucus, consequently enhancing its clearance from the lung. A series of co-spray-dried samples, containing therapeutically relevant doses of SS and MA, were prepared. The physico-chemical characteristics of the formulations were evaluated in terms of size distribution, morphology, thermal and moisture response and aerosol performance. Additionally, the formulations were evaluated for their effects on cell viability and transport across air interface Calu-3 bronchial epithelial cells, contractibility effects on bronchial smooth muscle cells and cilia beat activity using ciliated nasal epithelial cells in vitro. The formulations demonstrated size distributions and aerosol performance suitable for inhalation therapy. Transport studies revealed that the MA component of the formulation enhanced penetration of SS across the complex mucus layer and the lung epithelia cells. Furthermore, the formulation in the ratios of SS 10−6 and MA 10−3 M gave a significant increase in cilia beat frequency whilst simultaneously preventing smooth muscle contraction associated with mannitol administration. These studies have established that co-spray dried combination formulations of MA and SS can be successfully prepared with limited toxicity, good aerosol performance and the ability to increase ciliary beat frequency for improving the mucociliary clearance in patients suffering from hyper-secretory diseases, whilst simultaneously acting on the underlying smooth muscle.










Similar content being viewed by others
REFERENCES
Barker AF. Bronchiectasis. N Engl J Med. 2002;346(18):1383–93.
Murray TS, Egan M, Kazmierczak BI. Pseudomonas aeruginosa chronic colonization in cystic fibrosis patients. Curr Opin Pediatr. 2007;19(1):83.
Barker AF, Couch L, Fiel SB, Gotfried MH, Ilowite J, Meyer KC, et al. Tobramycin solution for inhalation reduces sputum Pseudomonas aeruginosa density in bronchiectasis. Am J Respir Crit Care Med. 2000;162(2):481–5.
Geller DE. Aerosol antibiotics in cystic fibrosis. Respir Care. 2009;54(5):658–70.
Yang Y, Tsifansky MD, Shin S, Lin Q, Yeo Y. Mannitol-guided delivery of ciprofloxacin in artificial cystic fibrosis mucus model. Biotechnol Bioeng. 2011;108(6):1441–9.
Anderson P. Emerging therapies in cystic fibrosis. Ther Adv Respir Dis. 2010;4(3):177–85.
Wood AJJ, Ramsey BW. Management of pulmonary disease in patients with cystic fibrosis. N Engl J Med. 1996;335(3):179–88.
Brannan JD, Anderson SD, Perry CP, Freed-Martens R, Lassig AR, Charlton B. The safety and efficacy of inhaled dry powder mannitol as a bronchial provocation test for airway hyperresponsiveness: a phase 3 comparison study with hypertonic (4.5%) saline. Respir Res. 2005;6(1):144.
Robinson M, Daviskas E, Eberl S, Baker J, Chan HK, Anderson S, et al. The effect of inhaled mannitol on bronchial mucus clearance in cystic fibrosis patients: a pilot study. Eur Respir J. 2001;14(3):678–85.
Hasani A, Toms N, O’Connor J, Dilworth J, Agnew J. Effect of salmeterol xinafoate on lung mucociliary clearance in patients with asthma. Respir Med. 2003;97(6):667–71.
Fazio F, Lafortuna C. Effect of inhaled salbutamol on mucociliary clearance in patients with chronic bronchitis. Chest. 1981;80(6 Suppl):827–30.
Bennett WD. Effect of β-adrenergic agonists on mucociliary clearance. J Allergy Clin Immunol. 2002;110(6, Supplement):S291–7.
Mortensen J, Hansen A, Falk M, Nielsen I, Groth S. Reduced effect of inhaled beta 2-adrenergic agonists on lung mucociliary clearance in patients with cystic fibrosis. CHEST J. 1993;103(3):805–11.
Robinson M, Bye PTB. Mucociliary clearance in cystic fibrosis. Pediatr Pulmonol. 2002;33(4):293–306.
Ong HX, Traini D, Bebawy M, Young PM. Epithelial profiling of antibiotic controlled release respiratory formulations. Pharm Res. 2011;28(9):2327–38.
Haghi M, Young PM, Traini D, Jaiswal R, Gong J, Bebawy M. Time-and passage-dependent characteristics of a Calu-3 respiratory epithelial cell model. Drug Dev Ind Pharm. 2010;36(10):1207–14.
Ong HX, Traini D, Salama R, Anderson SD, Daviskas E, Young PM. The effects of mannitol on the transport of ciprofloxacin across respiratory epithelia. Mol Pharm. 2013;10(8):2915–24.
Devalia J, Sapsford R, Rusznak C, Toumbis M, Davies R. The effects of salmeterol and salbutamol on ciliary beat frequency of cultured human bronchial epithelial cells, in vitro. Pulm Pharmacol. 1992;5(4):257–63.
Labiris N, Dolovich M. Pulmonary drug delivery. Part I: physiological factors affecting therapeutic effectiveness of aerosolized medications. Br J Clin Phamacol. 2003;56(6):588–99.
Adi H, Young PM, Chan H-K, Agus H, Traini D. Co-spray-dried mannitol–ciprofloxacin dry powder inhaler formulation for cystic fibrosis and chronic obstructive pulmonary disease. Eur J Pharm Sci. 2010;40(3):239–47.
Haghi M, Traini D, Bebawy M, Young PM. Deposition, diffusion and transport mechanism of dry powder microparticulate salbutamol, at the respiratory epithelia. Mol Pharm. 2012;9(6):1717–26.
Palacio M, Cuffini S, Badini R, Karlsson A, Palacios S. Solid-state characterization of two polymorphic forms of R-albuterol sulfate. J Pharm Biomed Anal. 2007;43(4):1531–4.
Shariare M, de Matas M, York P. Effect of crystallisation conditions and feedstock morphology on the aerosolization performance of micronised salbutamol sulphate. Int J Pharm. 2011;415(1):62–72.
Begat P, Young PM, Edge S, Kaerger JS, Price R. The effect of mechanical processing on surface stability of pharmaceutical powders: visualization by atomic force microscopy. J Pharm Sci. 2003;92(3):611–20.
Heng D, Lee SH, Kwek JW, Ng WK, Chan H-K, Tan RB. Assessing the combinatorial influence of climate, formulation and device on powder aerosolization using the Taguchi experimental design. Powder Technol. 2012;226:253–60.
Tee S, Marriott C, Zeng X, Martin G. The use of different sugars as fine and coarse carriers for aerosolised salbutamol sulphate. Int J Pharm. 2000;208(1):111–23.
Young PM, Edge S, Traini D, Jones MD, Price R, El-Sabawi D, et al. The influence of dose on the performance of dry powder inhalation systems. Int J Pharm. 2005;296(1):26–33.
Ong HX, Traini D, Young PM. Pharmaceutical applications of the Calu-3 lung epithelia cell line. Expert Opin Drug Deliv. 2013;0(0):1–16.
Hirsh AJ. Altering airway surface liquid volume: inhalation therapy with amiloride and hyperosmotic agents. Adv Drug Deliv Rev. 2002;54(11):1445–62.
McDougall CM, Blaylock MG, Douglas JG, Brooker RJ, Helms PJ, Walsh GM. Nasal epithelial cells as surrogates for bronchial epithelial cells in airway inflammation studies. Am J Respir Cell Mol Biol. 2008;39(5):560.
Rutland J, Cole PJ. Nasal mucociliary clearance and ciliary beat frequency in cystic fibrosis compared with sinusitis and bronchiectasis. Thorax. 1981;36(9):654–8.
Andersen I, Camner P, Jensen PL, Philipson K, Proctor DF. A comparison of nasal and tracheobronchial clearance. Arch Environ Health. 1974;29(5):290–3.
Yaghi A, Zaman A, Dolovich MB. The direct effect of hyperosmolar agents on ciliary beating of human bronchial epithelial cells. J Aerosol Med Pulm Drug Deliv. 2012;25(2):88–95.
Daviskas E, Anderson SD, Eberl S, Chan HK, Young IH, Seale JP. Effects of terbutaline in combination with mannitol on mucociliary clearance. The Eur Respir J. 2002;20(6):1423–9.
Duchateau GS, Merkus FW, Zuidema J, Graamans K. Correlation between nasal ciliary beat frequency and mucus transport rate in volunteers. Laryngoscope. 1985;95(7):854–9.
Boek WM, Graamans K, Natzijl H, van Rijk PP, Huizing EH. Nasal mucociliary transport: new evidence for a key role of ciliary beat frequency. Laryngoscope. 2002;112(3):570–3.
Anderson SD, Brannan J, Spring J, Spalding N, Rodwell LT, Chan K, et al. A new method for bronchial-provocation testing in asthmatic subjects using a dry powder of mannitol. Am J Respir Crit Care Med. 1997;156(3):758–65.
Leuppi JD, Brannan JD, Anderson SD. Bronchial provocation tests: the rationale for using inhaled mannitol as a test for airway hyperresponsiveness. Swiss Med Wkly. 2002;132(13/14):151–8.
Fujimoto N, Zhao C, Shichi H. The effects of prostaglandins E2 and F2α on porcine ciliary muscle cells in culture. Curr Eye Res. 1995;14(12):1155–63.
Ma X, Cheng Z, Wang Y, Unruh H, Stephens NL, Laviolette M. Changes in biophysical and biochemical properties of single bronchial smooth muscle cells from asthmatic subjects. Am J Physiol Lung Cell Mol Physiol. 2002;283(6):L1181–9.
Pang I-H, Shade DL, Tamm E, DeSantis L. Single-cell contraction assay for human ciliary muscle cells. Effect of carbachol. Invest Ophthalmol Vis Sci. 1993;34(5):1876–9.
Oldenburg PJ, Wyatt TA, Sisson JH. Ethanol attenuates contraction of primary cultured rat airway smooth muscle cells. Am J Respir Cell Mol Biol. 2010;43(5):539–45.
Govindaraju V, Michoud M-C, Ferraro P, Arkinson J, Safka K, Valderrama-Carvajal H, et al. The effects of interleukin-8 on airway smooth muscle contraction in cystic fibrosis. Respir Res. 2008;9(1):76.
Kume H, Hall IP, Washabau RJ, Takagi K, Kotlikoff MI. Beta-adrenergic agonists regulate KCa channels in airway smooth muscle by cAMP-dependent and -independent mechanisms. The J Clin Investig. 1994;93(1):371–9.
Salathe M. Effects of β-agonists on airway epithelial cells. J Allergy Clin Immunol. 2002;110(6):S275–81.
Acknowledgements
A/Professor Traini is the recipient of an Australian Research Council Future Fellowship (project number FT12010063). A/Professor Young is the recipient of an Australian Research Council Future Fellowship (project number FT110100996). This project was supported by ARC-Linkage grant no. LP100100451. The authors would also like to acknowledge Lynn Moir for her expert advice on the smooth muscle contraction studies.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Table 1
Spray drying conditions for single mannitol (MA) and co-spray-dried mannitol/salbutamol sulphate (SS). (DOCX 51 kb)
Supplementary Fig. 1
Particle size distribution of single spray-dried mannitol (MA) and co-spray-dried salbutamol sulphate with mannitol (SS/MA) measured using laser diffraction. Data represents the mean ± SD of at least three replicate experiments. (JPEG 214 kb)
Supplementary Fig. 2
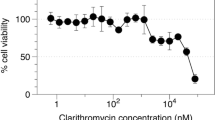
The effect of SS and MA on Calu-3 cells viability after 72-h drug exposure. The data represented the mean ± SD of at least three separate determinations. (JPEG 357 kb)
Supplementary Fig. 3
Transepithelial electrical resistance (TEER) of Calu-3 cells after transport experiments. Data represents the mean ± SD of at least three separate determinations. (JPEG 167 kb)
Rights and permissions
About this article
Cite this article
Ong, H.X., Traini, D., Ballerin, G. et al. Combined Inhaled Salbutamol and Mannitol Therapy for Mucus Hyper-secretion in Pulmonary Diseases. AAPS J 16, 269–280 (2014). https://doi.org/10.1208/s12248-014-9560-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1208/s12248-014-9560-4