Abstract
Heat stroke is a life-threatening condition that can be fatal if not appropriately managed. Although heat stroke has been recognised as a medical condition for centuries, a universally accepted definition of heat stroke is lacking and the pathology of heat stroke is not fully understood. Information derived from autopsy reports and the clinical presentation of patients with heat stroke indicates that hyperthermia, septicaemia, central nervous system impairment and cardiovascular failure play important roles in the pathology of heat stroke. The current models of heat stroke advocate that heat stroke is triggered by hyperthermia but is driven by endotoxaemia. Endotoxaemia triggers the systemic inflammatory response, which can lead to systemic coagulation and haemorrhage, necrosis, cell death and multi-organ failure. However, the current heat stroke models cannot fully explain the discrepancies in high core temperature (Tc) as a trigger of heat stroke within and between individuals. Research on the concept of critical Tc as a limitation to endurance exercise implies that a high Tc may function as a signal to trigger the protective mechanisms against heat stroke. Athletes undergoing a period of intense training are subjected to a variety of immune and gastrointestinal (GI) disturbances. The immune disturbances include the suppression of immune cells and their functions, suppression of cell-mediated immunity, translocation of lipopolysaccharide (LPS), suppression of anti-LPS antibodies, increased macrophage activity due to muscle tissue damage, and increased concentration of circulating inflammatory and pyrogenic cytokines. Common symptoms of exercise-induced GI disturbances include diarrhoea, vomiting, gastrointestinal bleeding, and cramps, which may increase gut-related LPS translocation.
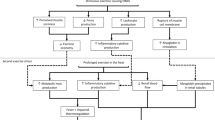
This article discusses the current evidence that supports the argument that these exercise-induced immune and GI disturbances may contribute to the development of endotoxaemia and heat stroke. When endotoxaemia can be tolerated or prevented, continuing exercise and heat exposure will elevate Tc to a higher level (>42°C), where heat stroke may occur through the direct thermal effects of heat on organ tissues and cells. We also discuss the evidence suggesting that heat stroke may occur through endotoxaemia (heat sepsis), the primary pathway of heat stroke, or hyperthermia, the secondary pathway of heat stroke. The existence of these two pathways of heat stroke and the contribution of exercise-induced immune and GI disturbances in the primary pathway of heat stroke are illustrated in the dual pathway model of heat stroke. This model of heat stroke suggests that prolonged intense exercise suppresses anti-LPS mechanisms, and promotes inflammatory and pyrogenic activities in the pathway of heat stroke.






Similar content being viewed by others
References
Gisolfi CV, Mora F. The hot brain: survival, temperature and the human body. Cambridge (MA): MIT Press, 2000: 77–120
Bouchama A. Heatstroke: a new look at an ancient disease. Intensive Care Med 1995; 21: 623–625
Moseley P, Gisolfi CV. New frontiers in thermoregulation and exercise. Sports Med 1993; 16: 163–167
Camus G, Deby-Dupont G, Duchateau J, et al. Are similar inflammatory factors invovled instrenuous exercise and sepsis? Intensive Care Med 1994; 20: 602–610
Bouchama A, Knochel JP. Heat Stroke. N Engl J Med 2002; 346: 1978–1988
Hales RJS, Hubbard RW, Gaffin SL. Limitation of heat tolerance. In: Fregly MJ, Blatteis CM, editors. Hand book of physiology: environmental physiology. Vol. 1. New York: Oxford University Press, 1996: 285–287, 295-312
Hales RJS, Sakurada S. Heat tolerance: a role for fever? Ann N Y Acad Sci 1998; 856: 188–205
Bouchama A, Al-Sedairy S, Siddiqui S, et al. Elevated pyrogenic cytokines in heatstroke. Chest 1993; 104: 1498–1502
Bouchama A, Bridey F, Hammami MM, et al. Activation of coagulation and fibrinolysis in heatstroke. Thromb Haemost 1996; 76: 909–915
Doran JE. Biological effects of endotoxin. In: Kraft CH, editor. Gut-derived infectious toxic shock: current studies in hematology and blood transfusion. Vol. 59. Basel: Karger, 1992: 66–99
Greisman SE. Induction of endotoxin tolerance. In: Nowotny A, editor. Beneficial effects of endotoxins. New York: Plenum Press, 1983: 149–196
Nieman DC. Immune response to heavy exertion. J Appl Physiol 1997; 82: 1385–1394
Nieman DC. Exercise and resistance to infection. Can J Physiol Pharmacol 1998; 76: 573–580
Nieman DC, Nehlsen-Cannarella SL. The immune response to exercise. Semin Hematol 1994; 31: 166–179
Nieman DC. Exercise, upper respiratory tract infection, and the immune system. Med Sci Sports Exerc 1994; 26: 128–139
Mackinnon LT. Overtraining effects on immunity and performance in athletes. Immunol Cell Biol 2000; 78: 502–509
Hack V, Weiss C, Friedmann B, et al. Decreased plasma glutamin level and CD4+ T cell number in response to 8 weeks of anaerobic training. Am J Physiol 1997; 272: E788–E795
Gleeson M, Pyne DB. Exercise effects on mucosal immunity. Immunol Cell Biol 2000; 78: 536–544
Mackinnon LT. Advances in exercise immunology. Champaign (IL): Human Kinetics Publisher, 1999: 33, 314
Smith LL. Overtraining, excessive exercise, and altered immunity. Sports Med 2003; 33: 347–364
Cantwell JD. Gastrointestinal disorders in runners. JAMA 1981; 246: 1404–1405
Fogoros RN. Runner’s trot: gastrointestinal disturbances in runners. JAMA 1980; 243: 1743–1744
McMahon LF, Ryan MJ, Larson D, et al. Occult gastrointestinal blood loss in marathon runners. Ann Intern Med 1984; 100: 846–847
Marshall JC. The gut as a potential trigger of exercise-induced inflammatory responses. Can J Physiol Pharmacol 1998; 76: 479–484
Moses FM. Gastrointestinal bleeding and the athlete. Am J Gastroenterol 1993; 88: 1157–1159
Sullivan SN, Wong C. Runners’ diarrhea: different pattern and associated factors. J Clin Gastroenterol 1992; 14: 101–104
Butcher JD. Runner’s diarrhea and other intestinal problems of athletes. Am Fam Physician 1993; 48: 623–625
Bosenberg AT, Brock-Utne JG, Gaffin SL, et al. Strenuous exercise causes systemic endotoxemia. J Appl Physiol 1988; 65: 106–108
Brock Utne JG, Gaffin SL, Wells MT, et al. Endotoxaemia in exhausted runners after a long-distance race. S Afr Med J 1988; 73: 533–536
Camus G, Nys M, Poortmans JR, et al. Endotoxemia, production of tumor necrosis factor alpha and polymorphonuclear neutrophil activation following strenuous exercise in humans. Eur J Appl Physiol 1998; 79: 62–68
Pals KL, Chang RT, Ryan AL, et al. Effect of running intensity on intestinal permeability. J Appl Physiol 1997; 82: 571–576
Ryan AL. Heat stroke and endotoxemia: sensitization or tolerance to enditoxins? In: Gisolfi CV, Lamb DR, Nadel ER, editors. Perspectives in exercise science and sports medicine. Vol. 6. Carmel (IN): Cooper Publishing Group, 1993: 335–370
Epstein Y, Moran DS, Shapiro Y, et al. Exertional heat stroke: a case series. Med Sci Sports Exerc 1999; 31: 224–228
Shibolet S, Coll R, Gilat T, et al. Heat stroke: its clinical picture and mechanism in 36 cases. Q J Med 1967; 36: 525–547
Keren G, Epstein Y, Magazanik A. Temporary heat intolerance in a heatstroke patient. Aviat Space Environ Med 1981; 52: 116–117
Merican MI. Management of heatstroke in Malaysian pilgrims in Saudi Arabia. Med J Malaysia 1989; 44: 183–188
Malamud N, Haymaker W, Custer R. Heat stroke: a clinicopathologic study of 125 fatal cases. Mil Surg 1946; 99: 397–449
Chao TC, Sinniah R, Pakiam JE. Acute heat stroke deaths. Pathology 1981; 13: 145–156
Hart GR, Anderson RJ, Crumpler CP, et al. Epidemic classical heat stroke: clinical characteristics and course of 28 patients. Medicine 1982; 61: 189–197
Anderson RJ, Reed G, Knochel JP. Heatstroke. Adv Intern Med 1983; 28: 115–140
Clowes GHA, O’Donnel TF. Heat stroke. N Engl J Med 1974; 291: 564–567
Shvartz E, Shapiro Y, Magazanik A, et al. Heat acclimation, physical fitness, and responses to exercise in temperate and hot environment. J Appl Physiol 1977; 43: 678–683
Shapiro Y, Magazanik A, Udassin R, et al. Heat intolerance in former heatstroke patients. Ann Intern Med 1979; 90: 913–916
Costrini AM, Pitt HA, Gustafson AB, et al. Cardiovascular and metabolic manifestation of heat stroke and severe heat exhaustion. Am J Med 1979; 66: 296–302
Knochel JP, Reed G. Disorders of heat regulation. In: Narins R, editor. Maxwell & Kleeman’s clinical disorders of fluid and electrolyte metabolism. 5th ed. New York: McGraw-Hill, 1994: 1549–1590
Centers for Disease Control. Heat-related mortality in Chicago, July 1995. MMWR Morb Mortal Wkly Rep 1995; 44: 577–579
Barrow MW, Clark KA. Heat-related illnesses. Am Fam Physician 1998; 58: 749–759
Yaqub B, Al Deeb S. Heat strokes: aetiopathogenesis, neurological characteristics, treatment and outcome. J Neurol Sci 1998; 156: 144–151
Samarasinghe JL. Heat stroke in young adults. Trop Doct 2001; 31: 217–219
Nadel ER, Mack GW, Nose H, et al. Tolerance to severe heat and exercise: peripheral vascular responses to body fluid changes. In: Hales RJS, Richards DAB, editors. Heat stress: physical exertion and environment. Amsterdam: Elsevier Science Publisher, 1987: 117–131
Stitt J. Central regulation of body temperature. In: Gisolfi CV, Lamb DR, Nadel ER, editors. Perspectives in exercise science and sports medicine. Vol. 6. Carmel (IN): Cooper Publishing Group, 1993: 2–39
Brinnel H, Cabanac M, Hales JRS. Critical upper levels of body temperature, tissue thermosensitivity and selective brain cooling in hyperthermia. In: Hales JRS, Richards DAB, editors. Heat stress: physical exertion and environment. Amsterdam: Elsevier, 1987: 209–240
Shibolet S, Lancaster MC, Danon Y. Heatstroke: a review. Aviat Space Environ Med 1976; 47: 280–301
Adolf EF, Fulton FB. The effects of exposure to high temperature upon the circulation in man. Am J Physiol 1924; 67: 573–588
Coris EE, Ramirez AM, Van Durme DJ. Heat illness in athletes. Sports Med 2004; 34: 9–16
Levick JJ. Remarks on sunstroke. Am J Med Sci 1859; 73: 40–55
Chaves Carballo E, Bouchama A. Fever, heatstroke, and hemorrhagic shock and encephalopathy. J Child Neurol 1998; 13: 286–287
Sohal RS, Sun SC, Colcolough HL, et al. Heat Stroke: an electron microscopic study of endothelial cell damage and disseminated intravascular coagulation. Arch Intern Med 1968; 122: 43–47
Knochel JP. Heat stroke and related heat stress disorders. Dis Mon 1989; 35: 301–378
Bouchama A, Parhar S, El-Yagi A, et al. Endotoxemia and the release of tumor necrosis factor and interleukin1-alpha in acute heat stroke. J Appl Physiol 1991; 70: 2640–2644
Gathiram P, Gaffin SL, Brock Utne JG, et al. Prophylactic corticosteroid suppresses endotoxemia in heat-stressed primates. Aviat Space Environ Med 1988; 59: 142–145
Gathiram P, Wells MT, Brock Utne JG, et al. Antilipopolysaccharide improves survival in primates subjected to heat stroke. Circ Shock 1987; 23: 157–164
Gathiram P, Wells MT, Brock Utne JG, et al. Prophylactic corticosteroid increases survival in experimental heat stroke in primates. Aviat Space Environ Med 1988; 59: 352–355
Butkow N, Mitchell D, Laburn H, et al. Heat stroke and endotoxemia in rabbits. In: Hales JRS, editor. Thermal physiology. New York: Raben Press, 1984: 511–514
Lambert GP, Gisolfi CV, Berg DJ, et al. Hyperthermia-induced intestinal permeability and role of oxidative and nitrosative stress. J Appl Physiol 2002; 92: 1750–1761
Sakurada S, Hales RJS. A role for gastrointestinal endotoxins in enhancement of heat tolerance by physical fitness. J Appl Physiol 1998; 84: 207–214
Gathiram P, Wells MT, Brock Utne JG, et al. Prevention of endotoxaemia by non-absorbable antibiotics in heat stress. J Clin Pathol 1987; 40: 1364–1368
Bouchama A, Hammami MM, Haq A, et al. Evidence for endothelial cell activation/injury in heatstroke. Crit Care Med 1996; 24: 1173–1178
Gathiram P, Gaffin SL, Brock Utne JG, et al. Time course of endotoxemia and cardiovascular changes in heat-stressed primates. Aviat Space Environ Med 1987; 58: 1071–1074
Charan NB, Robinson WA, Mathew M. Heat stroke, disseminated intravascular coagulation and death in a long distance runner. J Assoc Physicians India 1975; 23: 917–919
Weiss BP, Mascola L, Fannin SL. Public health at the 1984 summer Olympics: the Los Angeles County experience. Am J Public Health 1986; 78: 686–688
Wetterhall SF, Coulombier DM, Herndon JM, et al. Medical care delivery at the 1996 Olympic Games. Centers for Disease Control and Prevention Olympics Surveillance Unit. JAMA 1998; 279: 1463–1468
Roydhouse N. Heat stroke in runners. N Z Med J 1979; 89: 361
Armstrong LE, Crago AE, Adams R, et al. Whole-body cooling of hyperthermic runners: comparison of two field therapies. Am J Emerg Med 1996; 14: 355–358
Richards CRB, Richards DAB. Medical management for fun runs. In: Hales RJS, Richards DAB, editors. Heat stress: physical exertion and environment. Amsterdam: Elsevier, 1987: 513–525
Richards R, Richards D. Fatal heat stroke in a’ fun run’. Med J Aust 1980; 2: 225–226
Wyndham CH, Strydom NB. The danger of an inadequate water intake during marathon running. S Afr Med J 1969; 43: 893–896
Roberts WO. Exercise-associated collapse in endurance events: a classification system. Phys Sportsmed 1989; 20: 17–28
Robinson S, Wiley SL, Boudurant LG, et al. Temperature regulation of men following heat stroke. Isr J Med Sci 1976; 12: 786–795
Maron MB, Wagner JA, Horvath SM. Thermoregulatory responses during competitive marathon running. J Appl Physiol 1977; 42: 909–914
Pugh LGCE, Corbett JL, Johnson RH. Rectal temperatures, weight losses and sweat rates in marathon running. J Appl Physiol 1967; 23: 347–352
Costill DL, Kammer WF, Fisher A. Fluid ingestion during distance running. Arch Environ Health 1970; 21: 520–525
Gilat T, Shibolet S, Sohar E. The mechanisms of heat stroke. J Trop Med Hyg 1963; 66: 204–212
Hubbard RW, Bowers WD, Matthews WT, et al. Rat model of acute heat stroke mortality. J Appl Physiol 1977; 42: 809–816
Dubose DA, McCreary J, Sowders L, et al. Relationship between rat heat stress mortality and alterations in reticuloendothelial carbon clearance function. Aviat Space Environ Med 1983; 54: 1090–1095
Khogali M, El-sayed H, Amar M, et al. Management and therapy regimen during cooling and in the recovery room at different heat stroke treatment centres. In: Khogali M, Hales RJS, editors. Heat stroke and temperature regulation. Sydney: Academic Press, 1983: 149–156
Shapiro Y, Seidman DS. Field and clinical observations of exertional heat stroke patients. Med Sci Sports Exerc 1990; 22: 6–14
Hanson PG, Zimmermann SW. Exertional heat stroke in novice runners. JAMA 1979; 242: 154–157
Dubose DA, Wenger B, Flinn SD, et al. Distribution and mitogen response of peripheral blood lymphocytes after exertional heat injury. J Appl Physiol 2003; 95: 2381–2389
Gonzalez-Alonso J, Teller C, Andersen SL, et al. Influence of body temperature on the development of fatigue during prolong exercise in the heat. J Appl Physiol 1999; 86: 1032–1039
Walters TJ, Ryan KL, Tate LM, et al. Exercise in the heat is limited by a critical internal temperature. J Appl Physiol 2000; 89: 799–806
Fuller A, Carter RN, Duncan M. Brain and abdominal temperatures at fatigue in rats exercising in the heat. J Appl Physiol 1998; 84: 877–883
Nielsen B, Nybo L. Cerebral changes during exercise in the heat. Sports Med 2003; 33: 1–11
Cheung SS, Sleivert GG. Multiple triggers of hyperthermic fatigue and exhaustion. Exerc Sport Sci Rev 2003; 32: 100–106
Mack GW. Hypothalamic control of body temperature: insights from the past. J Appl Physiol 2004; 97: 1593–1594
Matsukawa K. Central control of the cardiovascular system during exercise. In: Nose H, Gisolfi CV, Imaizumi K, editors. Exercise, nutrition, and environmental stress. Vol. 1 Transverse City (MI): Coopers Publishing Group, 2001: 39–64
Hideaki S. Stress response to exercise and its possible hypothalamic regulation: role of arginine-vasopressin. In: Nose H, Gisolfi CV, Imaizumi K, editors. Exercise, nutrition, and environmental stress. Vol. 1. Transverse City (MI): Coopers Publishing Group, 2001: 21–38
Hissa R. Central control of body temperature. Arctic Med Res 1990; 49: 3–15
Berg A, Muller HM, Rathmann S, et al. The gastrointestinal system: an essential target organ of the athlete’s health and physical performance. Exerc Immunol Rev 1999; 5: 78–95
Granger DN, Richardson PD, Kvietys PR, et al. Intestinal blood flow. Gastroenterology 1980; 78: 837–863
Clausen JP. Effect of physical training on cardiovascular adjustment to exercise in man. Physiol Rev 1977; 57: 779–815
Oktedalen O, Lunde OC, Opstad PK, et al. Changes in gastrointestinal mucosa after long-distance running. Scand J Gastroenterol 1992; 27: 270–274
Hall DM, Baumgardner KR, Oberley TD, et al. Splanchnic tissue undergo hypoxic stress during whole body hyperthermia. Am J Physiol 1999; 276: G1195–G1203
Buckman MT. Gastrointestinal bleeding in long-distance runners. Ann Intern Med 1984; 101: 127–128
Eichner ER. Gastrointestinal bleeding in athletes. Phys Sportsmed 1989; 17: 128–140
Thomson PD, Funk EJ, Carleton RA, et al. Incidence of death during jogging in Rhode Island from 1975 through 1980. JAMA 1982; 247: 2535–2538
Porter AM. Marathon running and the caecal slap syndrome. Br J Sports Med 1982; 10: S22–S25
Rehrer NJ, Meijer GA. Biomechanical vibration of the abdominal region during and bicycling. J Sports Med Phys Fitness 1991; 31: 231–234
Bouchama A. Features and outcomes of classic heat stroke. Ann Intern Med 1999; 130: 613
Gathiram P, Wells MT, Raidoo D, et al. Portal and systemic plasma lipopolysaccharide concentrations in heat-stressed primates. Circ Shock 1988; 25: 223–230
Moseley PL, Gapen C, Wallen ES, et al. Thermal stress induces epithelial permeability. Am J Physiol 1994; 267: C425–C434
Morseley PL. Exercise, heat, and thermotolerance: molecular mechanisms. In: Gisolfi CV, Lamb DR, Nadel ER, editors. Perspectives in exercise science and sports medicine: exercise, heat, and thermoregulation. Vol. 6. Carmel (IN): Cooper Publishing Group, 1993: 305–325
Shapiro Y, Alkan M, Epstein Y, et al. Increase in rat intestinal permeability to endotoxin during hyperthermia. Eur J Appl Physiol Occup Physiol 1986; 55: 410–412
Gathiram P, Gaffin SL, Wells MT, et al. Superior mesenteric artery occlusion shock in cats: modification of the endotoxemia by antilipopolysaccharide antibodies (anti-LPS). Circ Shock 1986; 19: 231–237
Gaffin SL, Brock Utne JG, Zanotti A, et al. Hypoxia-induced endotoxemia in primates: role of reticuloendothelial system function and anti-lipopolysaccharide plasma. Aviat Space Environ Med 1986; 57: 1044–1049
Shephard RJ, Shek PN. Immune dysfunction as a factor in heat illness. Crit Rev Immunol 1999; 19: 285–302
Janeway CA, Travers P, Walport M, et al. Immune biology. New York: Garland Publishing, 2001: 70–87
Flegel WA, Baumstark MW, Weinstock C, et al. Prevention of endotoxin-induced monokine release by human low- and high-density lipoproteins and by apolipoprotein A-1. Infect Immun 1993; 61: 5140–5146
Freudenberg MA, Bog-Hansen TC, Back U, et al. Interaction of lipopolysaccharides with plasma high density lipoproteins. Infect Immun 1980; 28: 373–380
Shephard RJ, Shek PN. Acute and chronic over-exertion: do depressed immune responses provide useful markers. Int J Sports Med 1998; 19: 159–171
Gleeson M, McDonald WA, Cripps AW, et al. The effect on immunity of long-term intensive training in elite swimmers. Clin Exp Immunol 1995; 102: 210–216
White DJ, Riccobene E, Nucci R, et al. Evaporation versus iced gastric lavage treatment of heatstroke: comparative efficacy in canine model. Crit Care Med 1987; 15: 748–750
White DJ, Kamath R, Nucci R, et al. Evaporation versus iced gastric lavage treatment of heatstroke: comparative efficacy in canine model. Am J Emerg Med 1993; 11: 1–3
Burger FJ, Fuhrman FA. Evidence of injury by heat in mammilian tissues. Am J Physiol 1964; 206: 1057–1061
Frankel HM. Effect of restraint on rat exposed to high temperature. J Appl Physiol 1959; 14: 997–999
Craig EA. The heat shock response. CRC Crit Rev Biochem 1984; 18: 239–280
Moseley PL. Heat shock proteins and heat adaptation of the whole organism. J Appl Physiol 1997; 83: 1413–1417
Lock M, Noble EG. Stress proteins: the exercise response. Can J Appl Physiol 1995; 20: 155–167
Pedersen BK, Rohde T, Zacho M. Immunity in athletes. J Sports Med Phys Fitness 1996; 36: 236–245
Pedersen BK, Rohde T, Ostrowski K. Recovery of the immunne system after exercise. Acta Physiol Scand 1998; 162: 325–332
Nehlsen-Cannarella SL, Nieman DC, Balk-Lamberton AJ, et al. The effects of moderate exercise training on immune response. Med Sci Sports Exerc 1991; 23: 64–70
Nieman DC, Nehlsen-Cannarella SL, Donohue KM, et al. The effects of acute moderate exercise on leukocyte and lymphocyte subpopulaitons. Med Sci Sports Exerc 1991; 23: 578–585
Nieman DC, Berk LS, Simpson-Westerberg M, et al. Effects of long-endurance running on immune system parameters and lymphocyte function in experienced marathoners. Int J Sports Med 1989; 10: 317–323
Gabriel H, Muller HJ, Urhausen A, et al. Suppresses PMA-induced oxidative burst and unimpaired phagocytosis of circulating granulocytes one week after a long endurance exercise. Int J Sports Med 1994; 15: 441–445
Nieman DC, Simandle S, Henson DA, et al. Lymphocyte proliferative response to 2.5 hours of running. Int J Sports Med 1995; 16: 404–408
Singh A, Zelazowska EB, Petrides JS, et al. Lymphocyte subset responses to exercise and glucocorticoid suppression in healthy men. Med Sci Sports Exerc 1996; 28: 822–828
Nieman DC, Faboaga OR, Butterworth DE, et al. Carbohydrate supplementation affects blood granulocyte and monocyte trafficking but not function after 2.5h of running. Am J Clin Nutr 1997; 66: 153–159
Gannon GA, Rhind SG, Suzui M, et al. Circulating levels of peripheral blood leukocytes and cytokines following competitive cycling. Can J Appl Physiol 1997; 22: 133–147
Miles MP, Mackinnon LT, Grove DS, et al. The relationship of natural killer cell counts, perforin mRNA and CD2 expression to post-exercise natural killer cell activity in humans. Acta Physiol Scand 2002; 174: 317–325
Green K, Rowbottom DG, Mackinnon LT. Exercise and T-lymphocyte function: a comparison of proliferation in PBMC and NK cell-depleted PBMC culture. J Appl Physiol 2002; 92: 2390–2395
Henson DA, Nieman DC, Parker JCD, et al. Carbohydrate supplementation and lymphocyte proliferative response to long endurance running. Int J Sports Med 1998; 19: 574–580
Nieman DC, Nehlsen-Cannarella SL, Fagoaga OR, et al. Immune response to two hours of rowing in elite female rowers. Int J Sports Med 1999; 20: 476–481
Kappel M, Tvede N, Galbo H, et al. Evidence that the effect of physical exercise on NK cell activity is mediated by epinephrine. J Appl Physiol 1991; 70: 2530–2534
Nieman DC, Ahle JC, Henson DA, et al. Indomethacin does not alter natural killer cell response to 2.5h of running. J Appl Physiol 1995; 79: 748–755
Nieman DC, Henson DA, Garner EB, et al. Carbohydrate affects natural killer cell redistribution but not activity after running. Med Sci Sports Exerc 1997; 29: 1318–1324
Gabriel H, Schwarz L, Steffens G, et al. Immunoregulatory hormones, circulating leukocyte and lymphocyte subpopulations before and after endurance exercise of different intensities. Int J Sports Med 1992; 13: 359–366
Kargotich S, Keast D, Goodman C, et al. The influence of blood volume changes on leukocyte and lymphocyte subpopulations in elite swimmers following interval training of varying intensities. Int J Sports Med 1997; 18: 373–380
Tvede N, Kappel M, Halkjoer-Kristensen J, et al. The effects of light, moderate, and severe bicycle exercise on lymphocyte subsets, natural and lymphokine killer cells, lymphocyte proliferative response and interleukin 2 production. Int J Sports Med 1993; 15: 275–282
Nieman DC, Miller AR, Henson DA, et al. Effect of high-versus moderate-intensity exercise on lymphocyte subpopulations and proliferative response. Int J Sports Med 1994; 15: 199–206
Nieman DC, Miller AR, Henson DA, et al. Effects of high- vs moderate-intensity exercise on natural killer cell activity. Med Sci Sports Exerc 1993; 25: 1126–1134
Nieman DC, Henson DA, Sampson CS, et al. The acute immune response to exhaustive resistance exercise. Int J Sports Med 1995; 16: 322–328
Kappel M, Poulsen TD, Galbo H, et al. Effects of elevated plasma noradrenaline concentration on the immune system in humans. Eur J Appl Physiol 1998; 79: 93–98
Berk LS, Nieman DC, Youngberg S, et al. The effect of long endurance running on natural killer cells in marathoners. Med Sci Sports Exerc 1990; 22: 207–212
Linde F. Running and upper respiratory tract infections. Scand J Sport Sci 1987; 9: 21–23
Peters EM, Bateman ED. Respiratory tract infections: an epidemiological survey. S Afr Med J 1983; 64: 582–584
Peters EM, Goetzsche JM, BGrobbelaar B, et al. Vitamin C supplementation reduces the incidence of postrace symptoms of upper-respiratory-tract infection in ultra-marathon runners. Am J Clin Nutr 1993; 57: 170–174
Fitzgerald L. Overtraining increases the susceptibility to infection. Int J Sports Med 1991; 12: S5–S8
Nieman DC, Johanssen LM, Lee JW, et al. Infectious episodes in runners before and after the Los Angeles Marathon. J Sports Med Phys Fitness 1990; 30: 316–328
Weiss C, Kinscherf R, Roth S, et al. Lymphocyte subpopulations and concentrations of soluble CD8 and CD4 antigen after anaerobic training. Int J Sports Med 1995; 16: 117–121
Nieman DC, Cook VD, Henson DA, et al. Moderate exercise training and natural killer cell cytotoxic activity in breast cancer patients. Int J Sports Med 1995; 16: 334–337
Nieman DC, Henson DA, Gusewitch G, et al. Physical activity and immne function in elderly women. Med Sci Sports Exerc 1993; 25: 823–831
Kumae T, Yamasaki K, Ishizaki K, et al. Effects of summer camp endurance training on non-specific immunity in longdistance runners. Int J Sports Med 1999; 20: 390–395
Gleeson M, McDonald WA, Pyne DB, et al. Immune status and respiratory illness for elite swimmers during a 12-week training cycle. Int J Sports Med 2000; 21: 302–307
Pedersen BK, Bruunsgaard H, Jensen M, et al. Exercise and the immune system: influence of nutrition and aging. J Sci Med Sport 1999; 2: 234–252
Nieman DC. Exercise, infection, and immunity. Int J Sports Med 1994; 15: S131–S141
Pedersen BK, Hoffman-Goetz L. Exercise and the immune system: regulation, integration, and adaptation. Physiol Rev 2000; 80: 1055–1081
Shephard RJ, Shek PN. Immune responses to inflammation and trauma: a physical training model. Can J Appl Physiol 1998; 76: 469–472
Armstrong LE, Epstein Y, Greenleaf JE, et al. American College of Sports Medicine position stand: heat and cold illnesses during distance running. Med Sci Sports Exerc 1996; 28: i–x
Suzuki K, Nakaji S, Yamada M, et al. Systemic inflammatory response to exhaustive exercise: cytokine kinetics. Exerc Immunol Rev 2002; 8: 6–48
Cannon JG. Inflammatory cytokines in nonpathological states. News Physiol Sci 2000; 15: 298–303
Pedersen BK. Exercise and cytokines. Immunol Cell Biol 2000; 78: 532–535
Smith IK. Cytokine hypothesis of overtraining: a physiological adaptation to excessive stress. Med Sci Sports Exerc 2000; 32: 317–331
Dinarello CA. Roles of interleukin-1 in infectious diseases. Immunol Rev 1992; 127: 119–146
Shephard RJ, Rhind SG, Shek PN. Exercise and training: Infleuences on cytotoxicity, interleukin-1, interleukin-2 and receptor structure. Int J Sports Med 1994; 15: S154–S166
Nehlsen-Cannarella SL, Fagoaga OR, Nieman DC, et al. Carbohydrate and the cytokine response to 2.5h of running. J Appl Physiol 1997; 82: 1662–1667
Pedersen BK, Ostrowski K, Rohde T, et al. The cytokine response to strenuous exercise. Can J Physiol Pharmacol 1998; 76: 505–511
Epstein FH. Acute phase proteins and other systemic responses to inflammation. N Engl J Med 1999; 340: 449–454
Old LJ. Tumor necrosis factor: another chapter in the long history of endotoxin. Nature 1987; 330: 600–603
Smith JA. Neutrophil, host defense, and inflammation: a double edged sword. J Leukoc Biol 1994; 56: 672–686
Luheshi GN, Stefferl A, Turnbull AV, et al. Febrile response to tissue inflammation involves both peripheral and brain IL-1 and TNF-alpha in the rat. Am J Physiol 1997; 272: R862–R868
Ostrowski K, Rohde T, Asp S, et al. Pro- and anti-inflammatory cytokine balance in strenuous exercise in human. J Physiol 1999; 515: 287–291
Hammami MM, Bouchama A, Al Sedairy S, et al. Concentrations of soluble tumor necrosis factor and interleukin-6 receptors in heatstroke and heatstress. Crit Care Med 1997; 25: 1314–1319
Bouchama A, Hammami MM, Al Shail E, et al. Differential effects of in vitro and in vivo hyperthermia on the production of interleukin-10. Intensive Care Med 2000; 26: 1646–1651
Chang DM. The role of cytokines in heat stroke. Immunol Invest 1993; 22: 553–561
Lin MT, Liu HH, Yang YL. Involvement of interleukin-1 receptor mechanisms in development of arterial hypotension in rat heatstroke. Am J Physiol 1997; 273: H2072–H2077
Liu CC, Chien CH, Lin MT. Glucocorticoids reduce interleukin-1 concentration and result in neuroprotective effects in rat heatstroke. J Physiol 2000; 527 (2): 333–343
Lin MT, Kao TY, Hsu SSF. Interleukin-1beta production during the onset of heat stroke in rabbits. Neurosci Lett 1994; 174: 17–20
Bopst M, Haas C, Car B, et al. The combined inactivation of tumor necrosis factor and interleukin-6 prevents induction of the major acute phase proteins by endotoxin. Eur J Immunol 1998; 28: 4130–4137
Hammami MM, Bouchama A, Shail E, et al. Elevated serum level of soluble interleukin-2 receptor in heatstroke. Intensive Care Med 1998; 24: 988
Chiu WT, Kao TY, Lin MT. Increased survival in experimental rat heatstroke by continuous perfusion of interleukin-1 receptor antagonist. Neurosci Res 1996; 24: 159–163
Pedersen BK, Steensberg A, Fischer C, et al. Exercise and cytokine with particular focus on muscle derived IL-6. Exerc Immunol Rev 2001; 7: 18–31
Cooper AL, Brouwer S, Turnbull AV, et al. Tumor necrosis factor-alpha and fever after peripheral inflammation in the rat. Am J Physiol 1994; 267: R1431–R1436
Ostrowski K, Hermann C, Bangash A, et al. A trauma-like elevation of plasma cytokines in humans in response to treadmill running. J Appl Physiol 1998; 513: 889–894
Drenth JPH, Van Uum SHM, Deuren MV, et al. Endurance run increases circulating IL-6 and IL-1ra but downregulates ex vivo TNF-alpha and IL-1beta production. J Appl Physiol 1995; 79: 1497–1503
Nieman DC, Nehlsen-Cannarella SL, Fagoaga OR, et al. Immune function in female elite rowers and non-athletes. Br J Sports Med 2000; 34: 181–187
Moldoveanu AI, Shephard RJ, Shek PN. Exercise elevates plasma levels but not gene expression of IL-1beta, IL-6, TNF-alpha in blood mononuclear cells. J Appl Physiol 2000; 89: 1499–1504
Pedersen BK, Steensberg A, Schjerling P. Exercise and interleukin-6. Curr Opin Hematol 2001; 8: 137–141
Farber JL, Chien KR, Mittnacht S. The pathogenesis of irreversible cell injury in ischemia. Am J Pathol 1981; 102: 271–281
Clow A, Hucklebridge F. The impact of psychological stress on immune function in the athlete population. Exerc Immunol Rev 2001; 7: 5–17
Steensberg A, Toft AD, Bruunsgaard H, et al. Strenuous exercise decreases the percentage of type I T cells in the circulation. J Appl Physiol 2001; 91: 1708–1712
Bruunsgaard H, Hartkopp A, Mohr T, et al. In vivo cell-mediated immunity and vaccination response following prolonged, intense exercise. Med Sci Sports Exerc 1997; 29: 1176–1181
Nieman DC, Nehlsen-Cannarella SL, Fagoaga OR, et al. Influence of mode and carbohydrate on the cytokine response to heavy exertion. Med Sci Sports Exerc 1998; 30: 671–678
Moore GE, Holbein ME, Knochel JP. Exercise-associated collapse incyclists is unrelated to endotoxemia. Med Sci Sports Exerc 1995; 27: 1238–1242
Nieman DC, Henson DA, Smith LL, et al. Cytokine changes after a marathon race. J Appl Physiol 2001; 91: 109–114
Aarseth HP, Eide I, Skeie B, et al. Heat stroke in endurance exercise. Acta Med Scand 1986; 220: 279–283
Koizumi T, Nomura H, Kobayashi T, et al. Fatal rhabdomyolysis during mountaineering. J Sports Med Phys Fitness 1996; 36: 72–74
Lee RP, Bishop GF, Ashton CM. Severe heat stroke in an experienced athlete. Med J Aust 1990; 153: 100–104
Hart LE, Egier BP, Shimizu AG, et al. Exertional heat stroke: the runner’s nemesis. CMAJ 1980; 122: 1144–1150
Hoffman-Goetz L, Pedersen BK. Exercise and the immune system: a model of the stress response? Immunol Today 1994; 15: 382–387
Epstein Y, Shani Y, Moran DS, et al. Exertional heat stroke: the prevention of a medical emergency. J Basic Clin Physiol Pharmacol 2000; 11: 395–401
Epstein Y, Sohar E, Shapiro Y. Exertional heat-stroke: a preventable condition. Isr J Med Sci 1995; 31: 454–462
Nieman DC. Exercise immunology: nutritional countermeasures. Can J Appl Physiol 2001; 26 Suppl.: S45–S55
Pedersen BK. Influence of physical activity on the cellular immune system: mechanisms of action. Int J Sports Med 1991; 12 Suppl. 1: S23–S29
Acknowledgements
The authors are grateful to the Defence Science Organisation National Laboratories, Singapore, for supporting the preparation of this manuscript. The views expressed in this manuscript are those of the authors. They do not represent the views of the Ministry of Defence, Singapore.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lim, C.L., Mackinnon, L.T. The Roles of Exercise-Induced Immune System Disturbances in the Pathology of Heat Stroke. Sports Med 36, 39–64 (2006). https://doi.org/10.2165/00007256-200636010-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/00007256-200636010-00004