INTRODUCTION
Chronic hyperglycemia is one of the main characteristics of diabetes mellitus. There are two forms of the disease, which are classified based upon insulin dependence: type 1 diabetes mellitus (T1DM) or T2DM. T1DM is considered a progressive autoimmune disorder of the pancreas causing the destruction of islet β-cells and resulting in diminished insulin production. The subsequent insulin deficiency results in elevated blood glucose levels. T2DM is generally coupled with metabolic syndrome, which includes increased insulin resistance, hyperglycemia, obesity, dyslipidemia and hypertension. Persistent exposure to elevated glucose levels has been recognized as one of the major causal factors of diabetic complications resulting in pathologies, such as atherogenesis, myocardial infraction, stroke and diabetic cardiomyopathy[1]. In this review, we will discuss one of the major fibrotic signaling pathways, the advanced glycation end product (AGE)/the receptor for AGE (RAGE) signaling cascade driven by chronic hyperglycemia in T2DM, as well as propose an alternate pathway that may offer insight into cardiovascular extracellular matrix (ECM) remodeling.
FIBROBLAST MEDIATED ECM REMODELING
In the heart 70%-80% of the cellular mass is composed of myocytes, and the remaining 20%-30% the total cell number includes fibroblasts, vascular smooth muscle cells, and endothelial cells[2,3]. Fibroblasts are the most abundant cardiac cell types of the latter group, and these cells are accountable for homeostatic upkeep and pathological ECM alterations observed in the heart[2,3]. Fibroblasts also function as sensory cells recognizing mechanical and chemical changes within the cell’s microenvironment[4]. Fibroblasts communicate with the surrounding ECM to maintain the structural arrangements of the heart as well as sustain vital cellular tasks, such as viability, proliferation, and motility[5].
In pathologies, like T2DM, where biochemical and mechanical stimuli alter the communication between the ECM and fibroblasts, profibrotic signaling cascades are subsequently activated to elevate fibrotic accumulation and subsequently increased heart stiffness[4,6,7]. Increased ECM deposition and accumulation may result from either enhanced matrix protein synthesis and/or decreased structural degradation. With elevated matrix production and accumulation structural ECM rearrangements would cause alterations in fibroblast-matrix interactions. These changes often result in transformations in fibroblast phenotype. Fibroblast isolates from hypertensive animals as well as from infarcted regions of the heart exhibit increased matrix production and accumulation, reduced cell migration, and greater contractility[8-10]. In these instances, changes in fibroblast phenotype correspond to increases in fibroblast to myofibroblast differentiation. Myofibroblasts are defined as a “stressed” fibroblast having increased matrix production as well as enhanced contractile properties[11-13].
This cell type is not commonly found in healthy myocardium, however upon pathological cardiac injury, myofibroblast populations will increase in the myocardium from differentiated interstitial and adventitial fibroblasts[13]. While initially beneficial in pathologies requiring enhanced scar formation to maintain organ integrity (e.g., myocardial infarction), myofibroblasts become detrimental to organ function if an increased population of myofibroblasts persists. Due to the high glucose levels seen in diabetic patients, studies have demonstrated an elevated synthesis and accumulation of the ECM, otherwise known as fibrosis, to increase ventricular stiffness to negatively impact heart function[14,15]. Ultimately, myofibroblasts are detrimental due to their critical role in cardiac pathology and remodeling, and in certain environments, such as diabetes mellitus, improper regulation of myofibroblasts leads to maladaptive tissue remodeling[13,16].
HYPERGLYCEMIA AND AGE
Numerous reports have documented chronic hyperglycemia is the causative agent responsible nonenzymatic formation of AGEs on substrates resistant to turnover, such as collagen[13]. These modifications will not only reinforce the ECM by adding surplus collagen structural crosslinks but also as a RAGE agonist. Chronic hyperglycemia, as observed in T2DM patients, increases the generation of AGEs. High levels of glucose nonenzymatically react with long-lived proteins forming reversible Schiff base intermediates and eventually, Amadori compounds[17]. Amadori products will undergo additional chemical alterations to be converted to nonreversible crosslinked AGES[17]. AGEs are also found to accumulate in normoglycemic patients as a result of longevity. Under high glucose settings observed in diabetics, AGE formation is accelerated, resulting in cardiac dysfunction as well as interstitial fibrosis[17-20]. AGE-modified collagen causes an increase in matrix stiffness causing it be resistance to hydrolytic turnover, resulting in an accumulation of ECM[17,21].
In vivo and in vitro studies demonstrate that AGEs account for many of the diabetic cardiovascular complications through their engagement of RAGE[22]. RAGE is capable of binding to multiple ligands. Under normoglycemic conditions the receptor is ordinarily expressed at reduced basal levels, however due to aging and to chronic hyperglycemia, RAGE expression is increased[17,20]. AGE/RAGE cascade activation promotes fibrosis growth factor secretion, increased matrix deposition progressing to multi-organ fibrosis, as well as increased RAGE expression[21,23-25]. Increased AGE crosslinks, AGE/RAGE cascade activation, and increased matrix accumulation have been correlated with the development of cardiovascular complications by increasing diastolic left ventricular stiffness[21,25,26]. AGEs have been demonstrated to increase expression of multiple collagen types, decrease proteoglycans synthesis, as well as generate ECM crosslinking. Interestingly, AGEs can be bound to other macromolecules to compound their negative impacts on a number tissues[15,27,28]. Also, they have been shown to perturb cell-matrix interactions, alter cell adhesion, and vascular permeability. Many of the maladaptive ECM alterations have been shown to be relatively corrected by disrupting the AGE/RAGE signaling cascade[29]. Therefore, the AGE/RAGE cascade provides a hypothetical focus for the management of diabetes-mediated ECM related cardiovascular diseases.
AGE/RAGE SIGNALING PATHWAY
Increased AGE/RAGE signaling has been demonstrated to promote key pathways that upregulate ECM protein expression and accumulation. In addition, activation of downstream signaling kinases such as p38, extracellular signal-regulated kinase 1/2 (ERK 1/2), nuclear factor-kappaB (NF-κB), and c-Jun N-terminal kinase (JNK), have been shown to mobilize multiple transcription factors to stimulate expression of growth factors and ECM protein accumulation[30-33]. Numerous studies have suggested that AGE/RAGE signaling pathways are ligand- and cell type dependent. For example, in endothelial progenitor cells, AGE/RAGE cascade activation inhibited migration while promoting apoptosis to further atherosclerosis in diabetic patients[34,35]. Upon treatment with anti-RAGE peptide antibodies, AGE/RAGE signaling pathway was down regulated and diabetic atherosclerotic lesions and vascular injury was significantly attenuated[34]. It also has been reported that AGE/RAGE is implicated in diabetic related macrovascular complications, arterial injury, as well as the progression of diabetic nephropathy and retinopathy[36]. In a T2DM leptin receptor deficient (db/db) mouse model, using RAGE blocking antibody, left ventricular diastolic chamber stiffness and the cardiac systolic function was attenuated in conjunction with reduced fibrosis. It has been proposed the multiple outcomes of AGE/RAGE signaling operate through protein kinase C (PKC). Utilizing cell culture experiments to model T1DM and T2DM hyperglycemic growth conditions in vitro, PKC activity was increased and followed by subsequent activation of various prostaglandins, cytokines, and increased ECM protein expression[22]. Immunoblotting experiments using of cellular lysates revealed PKC-α, -βI, -βII, -δ, -ε, and -ζ isoform activity was increased in endothelial cells[37].
The PKC kinase family is defined based upon their second messenger requirements. The conventional PKC family, which includes PKC-α, -βI, -βII, and -γ, is stimulated by calcium, phosphatidylserine, diacylglycerol, or phorbol-12-myristate-13-acetate. Members of the novel PKC group, which includes -δ, -ε, -θ and -η are also activated by the above ligands with the exception of calcium. The atypical PKC family, which includes -ζ and -ι/λ, cannot be activated by any of the above second messengers[38]. To date, PKC isoform activation has been associated with vascular alterations, including increased permeability, contractility, ECM synthesis, cell growth, and apoptosis[37], and these perturbations in vascular cell homeostasis have been shown to be mediated by differing PKC isoforms[37]. Of these isoforms, PKC-β and PKC-ζ emerged as a preferred substrate in the aortic and cardiac tissue of diabetic mice[39,40]. Additional examination of multiple PKC isoforms has identified of PKC-ζ as the most plausible target for RAGE phosphorylation[41].
PKC-ζ is involved in propagating a multiple of cascade pathways that lead to mitogen-activated protein kinase (MAPK) activation. The MAPK family plays a pivotal role in numerous cellular processes, including development, phenotype differentiation, and ECM protein synthesis. In a study by Koya et al[37], ERKs were demonstrated to be activated in a PKC-dependent manner. ERKs are a subfamily of MAPKs involved in signaling cascades responsible for multiple cellular functions, such as differentiation and proliferation. Stimulation of ERK signaling cascades involve activation of a molecular switch, Raf, to trigger a stepwise serine kinase cascade through activation of Raf, MAPK kinase kinase, MAPK kinase, MAPK, and ERK[42]. Activated ERK will translocate into the nucleus to activate transcription factors to initiate cellular proliferation, differentiation, and matrix accumulation[43-45].
AGE/RAGE and PKC-ζ signaling cascades have been demonstrated to increase ERK activation, both independently as well as synergistically; thereby PKC-ζ serves as a common molecular mediator between these two different cascades[46,47]. Phosphorylation of RAGE at Ser391 is a ligand-dependent mechanism that is required to perpetuate AGE/RAGE signaling[41]. PKC-ζ has been demonstrated to phosphorylate Ser391 of the intracellular RAGE domain. However in order for this to occur, PKC-ζ must be activated by Ras, a small GTPase, to initiate the cascade[41]. Recently, our lab and others have found that Rap1a, a small Ras-like GTPase, may also play a role in AGE/RAGE signaling in diabetes.
RAP1A: A MOLECULAR SWITCH
Rap1a, member of the Ras superfamily, operates as a binary molecular switch. This relay system is capable of transmitting a number of diverse signals from members of the Ras superfamily to effect changes in nuclear transcription, thus coupling extracellular stimulation to intracellular signaling cascades. In fact, Rap1a has been demonstrated to participate in hypertrophic pathways, integrin-mediated adhesion, cell attachment, migration, and cell junction formation. Studies have shown that Rap1a induced-ERK1/2 activation contributes to vascular pathologies as well as plays a role in the cardiovascular ion channels responsible for rhythmic heart function[48].
Rap1a utilizes a guanine nucleotide exchange factors (GEFs), that causes the dissociation of a bound GDP allowing for a new GTP molecule to bind. GTPase-activating proteins (GAPs) will then hydrolyze the newly bound GTP to GDP forcing the cycle to run in one direction. In this capacity, Rap1a rotates between the inactive GDP-bound and the active GTP-bound substrate. In addition, Rap1a has been demonstrated to be activated by at three second messengers, specifically cyclic AMP (cAMP), calcium, and diacylglycerol[49]. It is now recognized that a number of GEFs can be directly activated by cAMP whereby cAMP binding causes a conformational change in the GEF permitting nucleotide exchange. Of particular interest are the GEFs known to activate Rap1a. These are commonly referred to as cAMP-GEF or more specifically Epac (Exchange Protein directly Activated by cAMP). Epac proteins have been demonstrated to bind cAMP and activate Rap1a GTPases[50]. Conversely, Rap1a-GAP will hydrolyze GTP at the asparagine side chain, thereby rendering Rap1a inactive.
The dynamic control of Rap1a activation has been shown to be facilitated by protein kinase A (PKA) and Epac through cAMP-dependent cascades[51]. Both PKA and Epac proteins contain a cAMP binding domain and are sensitive to fluctuations to mediate Rap1a activation[48]. While PKA can phosphorylate the C-terminus of Rap1a, PKA-mediated activation is not necessary for cAMP stimulation of Rap1 by Epac. In fact, there have been extensive studies that have established Epac’s involvement in various cAMP-related cellular functions, such as cellular adhesion, that were previously attributed to PKA[52,53]. These cAMP sensitive proteins may act independently, synergistically, or possible antagonistically depending upon cellular distribution, concentration, and location to regulate Rap1a-mediated cellular functions. Our understanding of the Rap1a pathway is centered on the biological responses elicited by PKA-dependent pathways triggering downstream ERK1/2 activation[30]. However, recent studies have suggested a PKA-independent pathway for Epac-Rap1a activation of downstream signaling effectors[54]. Precise investigation of the discrete role and involvement of Rap1a is necessary within a number of signaling model systems.
AGE/RAGE and Rap1a-induced ECM accumulation in diabetes
To date, there is paucity in the literature describing the interactions between Rap1a and the AGE/RAGE signal pathway in T2DM. Early studies described Rap as being up-regulated in multiple organs of diabetic rats[55]. Of note, these studies also demonstrated that diacylglycerol can activate a Rap/Raf/MAPK-mediated signal cascade through PKC, however no specific PKC isoform was identified[55]. Furthermore, in a study by Panchatcharam et al[56], increased Rap1 expression was reported in smooth muscle cells under hyperglycemic conditions, yet no distinction between Rap1a or Rap1b subtypes was made. Taken together, there is evidence that Rap1a under hyperglycemic conditions will increase downstream kinase activity via ERK1/2 activation, and these events would ultimately influence other signaling pathways, including the AGE/RAGE cascade, to promote ECM accumulation to contribute to cardiac complications in diabetic patients.
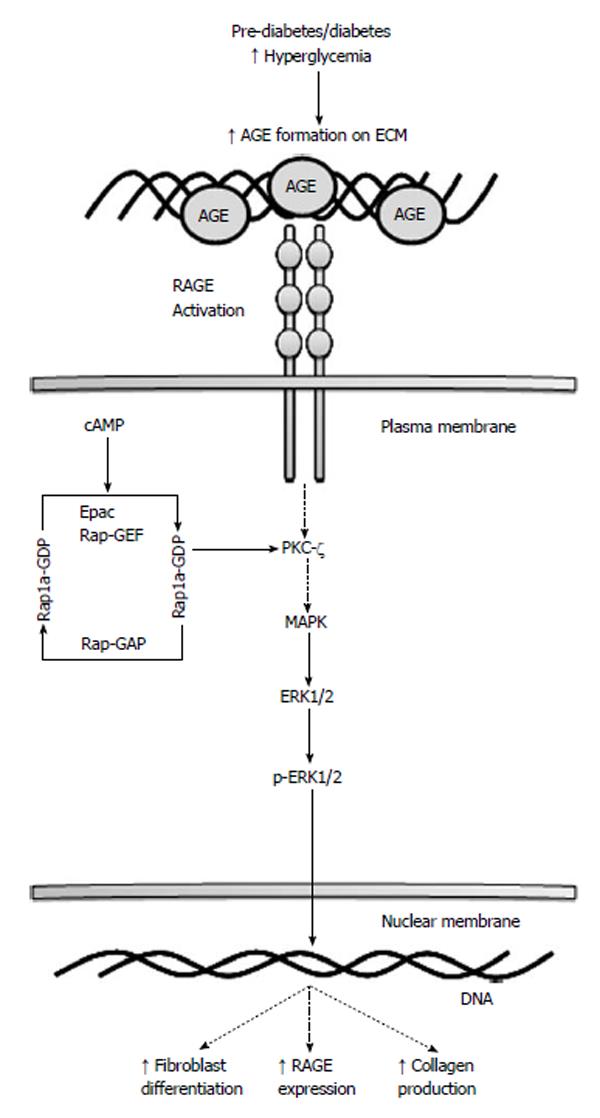
Both the AGE/RAGE signaling cascade and Rap1a utilize and activate similar signaling pathways, such as ERK1/2 MAPK, NF-κB and JNK, which are involved in cell growth, ECM synthesis and myofibroblasts differentiation. It has been demonstrated that fibroblasts treated with transforming growth factor-β, a known fibrosis mediator, myofibroblasts differentiation and ECM deposition is increased[17,57]. Furthermore, studies by Yan et al[57], showed that major molecular mediators, like ERK1/2 MAPK, involved in fibroblast growth factor-2 mediated angiogenesis were down regulated when Rap1a was depleted. Lastly, Jeyaraj et al[48] implicated Rap1a in roles that were intimately associated with the ECM remodeling process. Taken together, Rap1a and AGE/RAGE have been demonstrated to associate with increased myofibroblast formation and interstitial fibrosis independently. Figure 1 illustrates Rap1a’s potential role in mediating the AGE/RAGE signaling pathway as discussed in the context of this review. While there is some evidence of a functional interplay between AGE/RAGE and Rap1a, the exact molecular interactions have not been fully characterized.
Figure 1 Rap1a in advanced glycation end product/the receptor for advanced glycation end product signaling.
A potential role for Rap1a as a molecular switch mediating the AGE/RAGE signaling pathway in type 2 diabetes mellitus. Increased Rap1a activity may stimulate PKC-ζ to further promote matrix accumulation, RAGE expression and fibroblast differentiation to myofibroblasts. AGE: Advanced glycation end product; RAGE: The receptor for AGE; ECM: Extracellular matrix; cAMP: Cyclic AMP; GAP: GTPase-activating protein; PKC-ζ: The ζ isotype of protein kinase C; MAPK: Mitogen-activated protein kinase; ERK: Extracellular signal-regulated kinase.
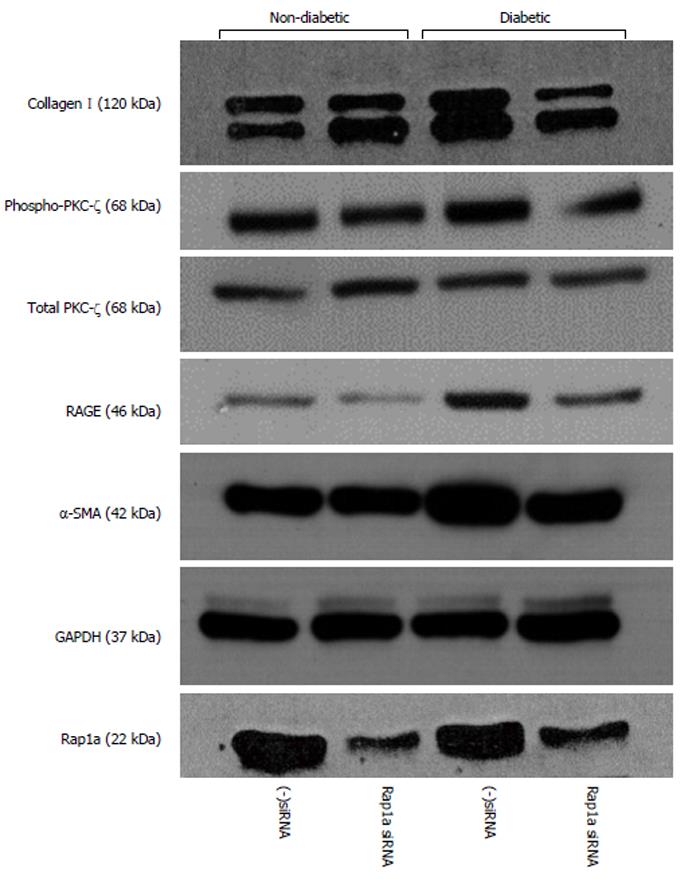
A series of studies by our laboratory suggest that Rap1a plays a role in fibrosis and myofibroblast differentiation in isolated diabetic and non-diabetic fibroblasts. Silencing Rap1a mRNA in diabetic fibroblasts returned profibrotic markers to nondiabetic levels. Isolated cardiac fibroblasts from 16 wk-old non-diabetic (heterozygous, wt/db) and diabetic (homozygous, db/db) mice were treated with siRNA targeted to Rap1a and a negative control of scrambled siRNA (data not shown) was used. 48-h post siRNA treatment, noticeable decreases were measured, not only in Rap1a expression, but also RAGE, collagen I, phospho-PKC-ζ, and α-smooth muscle actin protein expression (Figure 2). Inhibiting Rap1a protein expression down-regulated the molecular switch used to activate PKC-ζ to promote AGE/RAGE-mediated fibrosis. While these studies are still in a preliminary stage, we are working to expand our understanding of the significance of these alterations using not only siRNA technology, but also generating a double knockout mouse model to ascertain the role Rap1a plays in diabetic cardiomyopathy.
Figure 2 siRNA Rap1a knockdown in diabetic cardiac fibroblasts.
Cardiac fibroblasts were isolated from age-matched 16 wk-old db/wt (non-diabetic) and db/db (diabetic) mice and using siRNA targeted to Rap1a silenced transcription and translation of Rap1a resulting in noticeable decreases not only in Rap1a expression, but also the downstream signaling outcomes RAGE, collagen I, phospho-PKC-ζ and α-SMA protein expression. RAGE: The receptor for the advanced glycation end product; PKC-ζ: The ζ isotype of protein kinase C; α-SMA: α-smooth muscle actin; GAPDH: Glyceraldehyde 3-phosphate dehydrogenase.
CONCLUSION
From the evidence that is presented, a cellular and molecular mechanism for Rap1a-mediated activation of AGE/RAGE-dependent myocardial remodeling exists. This review is the first of its kind to provide Rap1a as a unique target for therapeutic strategies aimed at reducing chronic hyperglycemia-mediated ECM production and accumulation in diabetic patients. While much still needs to be performed to increase our understanding of this causal relationship, our laboratory is working towards defining the signaling cascade involving Rap1a and PKA in the AGE/RAGE signaling cascade which ultimately mediates fibroblast myocardial remodeling. These studies provide insight into the inter-signaling components of this cascade that could ultimately help in reducing ECM production and accumulation during hyperglycemia in T2DM patients.
ACKNOWLEDGMENTS
The authors would like to thank Dr. Donna M Gordon, Neeta Kumari, Rebecca A Worsham and Carter G Holland for their assistance in preparing this manuscript.
P- Reviewer: Georgescu A, Kusmic C S- Editor: Tian YL L- Editor: A E- Editor: Liu SQ