Abstract
Purpose
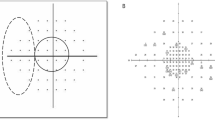
To assess the pattern and the local spatial frequency distribution of visual field defects (VFDs) in eyes with clinically diagnosed optic neuritis (ON) and their currently unaffected fellow eyes, using threshold-related, slightly supraliminal perimetry, ensuring high spatial resolution.
Methods
Records obtained with the Tübingen Automatic perimeter (TAP, Oculus Inc., Dudenhofen, Germany) and the Octopus 101 perimeter (Haag-Streit Inc, Koeniz, Switzerland), using a standardized grid of 191 static targets within the central 30° visual field, were analysed retrospectively. VFDs were assigned to 15 classes.
Results
Visual fields (VF) from 99 patients (26 male and 73 female subjects, aged from 18 to 51 years) with clinically diagnosed, acute ON (52 right eyes, 48 left eyes affected, one bilateral involvement) were evaluated. Central scotomas were the most common finding in associated eyes, covering 41% of all VFDs in affected eyes. Nerve fibre bundle defects were found in 29% and paracentral scotomas in 14% of all VFDs. Fellow eyes were perimetrically normal in 65% of the clinically monocular ONs. Nerve fibre bundle defects were found in 21% and diffuse scotomas in 9% of the fellow eyes.
Conclusions
Central scotomas and retinal nerve fibre bundle defects are the most common VFDs in acute ON. Small central and paracentral scotomas that most probably would have been missed by automated thresholding perimetry with its relatively coarse grid could be detected by threshold-related, slightly supraliminal strategy. Of the fellow eyes in clinically apparent monocular optic neuritis, 35% present with visual field defects.







Similar content being viewed by others
References
Aulhorn E, Karmeyer H (1977) Frequency distribution in early glaucomatous visual field defects. Docum Ophthal Proc Series 14:75–83
Bajandas FJ, Kline LB (1988) Neuro-ophthalmology review manual. Slack, Thorofare, USA
Beck RW, Kupersmith MJ, Cleary PA, Katz B (1993) Fellow eye abnormalities in acute unilateral optic neuritis. Experience of the optic neuritis treatment trial. Ophthalmology 100:691–697
Berliner M (1935) Acute optic neuritis in demyelinating diseases of the nervous system. Arch Ophthalmol 13:83–98
Compston A (2004) Mechanisms of axon-glial injury of the optic nerve. Eye 18:1182–1187
Fang JP, Donahue SP, Lin RH (1999) Global visual field involvement in acute unilateral optic neuritis. Am J Ophthalmol 128:554–565
Frederiksen JL, Larsson HB, Ottovay E, Stigsby B, Olesen J (1991) Acute optic neuritis with normal visual acuity. Comparison of symptoms and signs with psychophysiological, electrophysiological and magnetic resonance imaging data. Acta Ophthalmol Copenh 69:357–366
Gerling J, Meyer JH, Kommerell G (1998) Visual field defects in optic neuritis and anterior ischemic optic neuropathy: distinctive features. Graefes Arch Clin Exp Ophthalmol 236:188–192
Hickman SJ, Brex PA, Brierley CM, Silver NC, Barker GJ, Scolding NJ, Compston DA, Moseley IF, Plant GT, Miller DH (2001) Detection of optic nerve atrophy following a single episode of unilateral optic neuritis by MRI using a fat-saturated short-echo fast FLAIR sequence. Neuroradiology 43:123–128
Hyllested K, Møller PM (1961) Follow-up on patients with a history of optic neuritis. Acta Ophthalmol (Copenh) 39:655–662
Katz J, Tielsch JM, Quigley HA, Sommer A (1995) Automated perimetry detects visual field loss before manual Goldmann perimetry. Ophthalmology 102:21–26
Keltner JL, Johnson CA, Beck RW, Cleary PA, Spurr JO (1993) Quality control functions of the Visual Field Reading Center (VFRC) for the Optic Neuritis Treatment Trial (ONTT). Control Clin Trials 14:143–159
Keltner JL, Johnson CA, Spurr JO, Beck RW (1993) Baseline visual field profile of optic neuritis. The experience of the optic neuritis treatment trial. Optic Neuritis Study Group. Arch Ophthalmol 111:231–234
Keltner JL, Johnson CA, Spurr JO, Beck RW (1994) Visual field profile of optic neuritis. One-year follow-up in the Optic Neuritis Treatment Trial. Arch Ophthalmol 112:946–953
Keltner JL, Johnson CA, Spurr JO, Beck RW (1999) Comparison of central and peripheral visual field properties in the Optic Neuritis Treatment Trial (ONTT). Am J Ophthalmol 128:543–553
Nikoskelainen E (1975) Symptoms, signs and early course of optic neuritis. Acta Ophthalmol (Copenh) 53:254–272
Schiefer U, Wilhelm H (1995) Gesichtsfeld-Kompendium. Klin Monatsbl Augenheilkd 206:206–238
Szatmáry G, Biousse V, Newman NJ (2002) Can Swedish interactive thresholding algorithm fast perimetry be used as an alternative to Goldmann perimetry in neuro-ophthalmic practice? Arch Ophthalmol 120:1162–1173
The Optic Neuritis Study Group (1991) The clinical profile of optic neuritis. Experience of the Optic Neuritis Treatment Trial. Arch Ophthalmol 109:1673–1678
Topouzis F, Coleman AL, Yu F, Mavroudis L, Anastasopoulos E, Koskosas A, Pappas T, Dimitrakos S, Wilson MR (2004) Sensitivity and specificity of the 76-suprathreshold visual field test to detect eyes with visual field defect by Humphrey threshold testing in a population-based setting: the Thessaloniki eye study. Am J Ophthalmol 137:420–425
Trip SA, Schlottmann PG, Jones SJ, Altmann DR, Garway-Heath DF, Thompson AJ, Plant GT, Miller DH (2005) Retinal nerve fiber layer axonal loss and visual dysfunction in optic neuritis. Ann Neurol 58:383–391
Acknowledgement
The authors are indebted to Dipl.-Inf. R. Burth for retrieving the data from the electronic data base, and to Dr. rer. nat. J. Paetzold for his support in analyzing the spatial frequency distribution. Supported in part by Finland’s Eye Foundation, the Evald and Hilda Nissi Foundation and the Finnish Ophthalmologists Council.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nevalainen, J., Krapp, E., Paetzold, J. et al. Visual field defects in acute optic neuritis - distribution of different types of defect pattern, assessed with threshold-related supraliminal perimetry, ensuring high spatial resolution. Graefes Arch Clin Exp Ophthalmol 246, 599–607 (2008). https://doi.org/10.1007/s00417-007-0722-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-007-0722-2