Summary
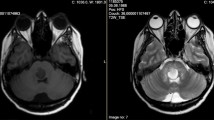
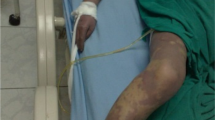
A 14-year-old girl was suffering from meningococcal sepsis with initial endophthalmitis. During a secondary and prolonged fever attack including aseptic meningitis, temporary complications such as pericarditis, arthralgic pains, headache and localized phlebitis were observed. There were three relapses of pericarditis within nine months. Their course was benign. The discussion deals with the pathogenesis of these complications as metastatic and immunologic reactions. The possibility of these complications should be considered during diagnostic investigation and therapeutic treatment.
Zusammenfassung
Bei einer 14jährigen Patientin wird eine Meningokokkensepsis mit initialer Endophthalmitis beschrieben. Während eines sekundären, prolongierten Fiebers mit aseptischer Meningitis traten als passagere Komplikationen eine Perikarditis, Arthralgien und eine lokale Phlebitis auf. Die gutartig verlaufende Perikarditis rezidivierte innerhalb von neun Monaten dreimal. In der Diskussion über die Pathogenese der genannten Komplikationen wird auf die metastatischen bzw. immunologischen Reaktionen des Krankheitsverlaufes Bezug genommen. Bei diagnostischen und therapeutischen Maßnahmen sollten diese Komplikationen berücksichtigt werden.
Similar content being viewed by others
Literature
Duke-Elder, St. Meningococcal uveitis. In:Duke-Elder, St. (ed.): System of ophthalmology, Vol. IX. Diseases of the uveal tract. Henry Kimptom, London 1966, pp. 229–230.
Lazar, N. K. Early ocular complication of epidemic meningitis. Arch. Ophthalmol. 16 (1936) 847–856.
Haider, S. Metastatic endophthalmitis. A rare complication of meningococcal meningitis. Postgrad. Med. J. 49 (1973) 567–574.
Jensen, A. D., Naidoff, M. A. Bilateral meningococcal endophthalmitis. Arch. Ophthalmol. 99 (1973) 396–398.
Shuttleworth, F. N., Bensteadt, J. G. Primary meningococcal ophthalmia. Br. Med. J. 2 (1947) 568–569.
Gamel, J. W., Allansmith, M. R. Metastatic staphylococcal endophthalmitis presenting as chronic iridocyclitis. Am. J. Ophthalmol. 77 (1974) 454–458.
Meyers, S. M. The incidence of fundus lesions in septicemica. Am. J. Ophthalmol. 88 (1979) 661–667.
Char, D. H., Stein, P., Masi, R., Christensen, M. Immunecomplexes in uveitis. Am. J. Ophthalmol. 87 (1979) 678–681.
Greenwood, B. M., Onyewotu, I. I., Whittle, H. C. Complement and meningococcal infection. Br. Med. J. 1 (1976) 797–799.
Jay, W. M., Schanzlin, D. J., Fritz, K. J. Medical therapy of metastatic meningococcal endophthalmitis. Am. J. Ophthalmol. 87 (1979) 567–568.
Snip, R. C., Michels, R. G. Pars plana vitrectomy in the management of endogenousCandida endophthalmitis. Am. J. Ophthalmol. 82 (1976) 699–704.
Eichenbaum, D. M., Jaffee, N. S., Clayman, H. M., Light, D. S. Pars plana vitrectomy as a primary treatment for acute bacterial endophthalmitis. Am. J. Ophthalmol. 86 (1978) 176–181.
Baum, J. L., Barza, M., Lugar, J., Onigman, P. The effect of corticosteroids in the treatment of experimental bacterial endophthalmitis. Am. J. Ophthalmol. 80 (1975) 513–517.
Herman, R. A., Rubin, H. A. Meningococcal pericarditis without meningitis presenting as tamponade. N. Engl. J. Med. 290 (1974) 143–144.
Pierce, H. I., Cooper, E. B. Meningococcal pericarditis. Arch. Intern. Med. 129 (1972) 918–922.
O'Connell, B. Pericarditis following meningococcal meningitis. Am. J. Dis. Child. 126 (1973) 265–267.
Wansbrough-Jones, M. H., Wong, O. P. Meningococcal pericarditis without meningitis. Br. Med. J. 2 (1973) 344–345.
Morse, J. R., Oretsky, M. I., Hudson, J. A. Pericarditis as a complication of meningococcal meningitis. Ann. Intern. Med. 74 (1971) 212–217.
Greenwood, B. M., Whittle, H. C., Bryceson, A. D. M. Allergic complications of meningococcal disease II; Immunological investigations. Br. Med. J. 2 (1973) 737–740.
Whittle, H. C., Abdullahi, M. T., Fakunle, F. A., Greenwood, B. M., Breyceson, A. D. M., Parry, E. H. O., Turk, J. L. Allergic complications of meningococcal disease I; Clinical aspects. Br. Med. J. 2 (1973) 733–737.
Sotto, M. N., Langer, B., Hoshinu-Shimizu, S., Thales de Brito Pathogenesis of cutaneous lesions in acute meningococcemia in humans: light, immunofluorescent and electron microscopic studies of skin biopsy specimens. J. Infect. Dis. 133 (1976) 506–514.
Hoffman, T. A., Edwards, E. A. Group-specific polysaccharide antigen and humoral antibody response in disease due toNeisseria meningitidis. J. Infect. Dis. 126 (1972) 636–649.
Davis, J. A. S., Peters, N., Mohammed, I., Major, G. A. C., Holborow, E. J. Circulating immune complexes in a patient with meningococcal disease. Br. Med. J. 2 (1976) 1445–1446.
Larson, H. E., Nicholson, K. G., Loewi, G., Tyrrell, D. A. J., Posner, J. Arthritis after meningococcal meningitis. Br. Med. J. 1 (1977) 618.
Sundal, E., Wacher, H., Rosenthal, M. Die allergische Reaktion auf das Meningokokken-Antigen. Schweiz. Med. Wschr. 107 (1977) 1900–1903.
Siemes, H., Siegert, M., Aldenhoff, P. Occurrence of M-proteins in the CSF of a child with a prolonged meningococcal meningitis. J. Clin. Lab. Immunol. 2 (1979) 31–36.
Zervas, J., Valassi-Adam, H., Constantopoulos, C., Zoumboulakis, D., Fessas, F., Matsaniatis, N. HLA-antigens in children with meningococcal meningitis. ESPR, Athens 1980, Abstract No. 9.
Geczy, A. F., Bashir, H. V., Alexander, K., Edmonds, J. P. Cross reactivity between environmental agents and HLA- B 27. Lancet I (1980) 50.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Stephani, U., Bleckmann, H. Rare complications in a case of generalized meningococcal disease: Immunologic reaction versus bacterial metastasis. Infection 10, 23–27 (1982). https://doi.org/10.1007/BF01640833
Received:
Issue Date:
DOI: https://doi.org/10.1007/BF01640833