Abstract
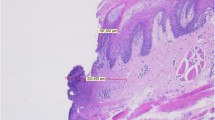
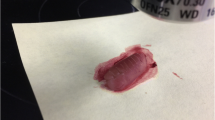
In oral pathology, laser devices can provide important advantages, especially in the treatment of certain lesions. However, there is controversy about the use of some wavelengths in the analysis of suspected dysplastic or neoplastic lesions, raising doubt about the laser’s suitability for use in biopsy procedures. In recent studies, the KTP and diode lasers have been used in biopsy procedures without histological artefacts. The aim of this in vitro study was to evaluate the exact extent of peripheral thermal damage to oral soft tissues caused by an Er:YAG laser (λ 2,940 nm) without water cooling. The study was performed on five swine cadaver tongues. Nine samples from each tongue were taken by the same operator using the Er:YAG laser with increasing energies (from 60 to 150 mJ) and fluencies (from 21 to 53 J/cm2). In addition to the laser samples, a specimen obtained using a scalpel was used as control. The samples were placed in 10% formalin solution and were examined by optical microscopy by two blinded pathologists who assigned a thermal damage score (from 0 to 3) to each sample. The Er:YAG laser produced less damage at 80 and 100 mJ and 28 and 35 J/cm2 (intermediate parameters). Although in some samples thermal damage was minimally visible, in all samples histological evaluation was clearly possible. The study demonstrated that the Er:YAG laser can be safely used in oral biopsy investigations while ensuring a successful histological evaluation, which is fundamental to correct clinical management.







Similar content being viewed by others
References
Bende T, Seiler T, Wollensak J (1991) Photoablation with the Er:YAG laser in ocular tissues. Fortschr Ophthalmol 88(1):12–16
Walsh JT Jr, Flotte TJ, Deutsch TF (1989) Er:YAG laser ablation of tissue: effect of pulse duration and tissue type on thermal damage. Lasers Surg Med 9(4):314–326
Araki AT, Ibraki Y, Kawakami T, Lage-Marques JL (2006) Er:Yag laser irradiation of the microbiological apical biofilm. Braz Dent J 17(4):296–299
Lopes BM, Theodoro LH, Melo RF, Thompson GM, Marcantonio RA (2010) Clinical and microbiologic follow-up evaluations after non-surgical periodontal treatment with erbium:YAG laser and scaling and root planing. J Periodontol 81(5):682–691
Gentil De Moor RJ, Delme KI (2010) Laser-assisted cavity preparation and adhesion to erbium-lased tooth structure: part 2. present-day adhesion to erbium-lased tooth structure in permanent teeth. J Adhes Dent 12(2):91–102
Hamamci N, Akkurt A, Başaran G (2010) In vitro evaluation of microleakage under orthodontic brackets using two different laser etching, self etching and acid etching methods. Lasers Med Sci 25(6):811–816
Catone GA, Alling CC (1997) Laser application in oral and maxillofacial surgery, 1st edn. W.B. Saunders, Philadelphia
Pick RM, Colvard MD (1993) Current status of lasers in soft tissue dental surgery. J Periodontol 64:589–602
Goharkhay K, Moritz A, Wilder-Smith P, Schoop U, Kluger Wakolitsch S et al (1999) Effects on oral soft tissue produced by a diode laser in vitro. Lasers Surg Med 25:401–406
Eversole LR (1997) Laser artifacts and diagnostic biopsy. Oral Surg Med Oral Pathol Oral Radiol Endod 83:639–640
Convissar RA (1997) Laser biopsy artefact. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 84:458
Rizoiu IM, DeShazer LG, Eversole LR (1995) Soft tissue cutting with a pulsed 20 Hz Er,Cr:YSGG laser. Proc SPIE 2396:273–283
Gendelman H, Actis AB, Ouri HO (1993) Neodymium-YAG and CO2 lasers in treatment of pre-cancerous lesions of the oral cavity. Acta Stomatol Belg 90(2):95–101
Romeo U, Del Vecchio A, Ripari F, Palaia G, Chiappafreddo C, Tenore G, Visca P (2007) Effects of different laser devices on oral soft tissue: in vitro experience. J Oral Laser Appl 7:155–159
Romeo U, Palaia G, Del Vecchio A, Tenore G, Gambarini G, Gutknecht N, De Luca M (2010) Effects of KTP laser on oral soft tissues. An in vitro study. Lasers Med Sci 25(4):539–543
Van As G (2004) Erbium laser in dentistry. Dent Clin North Am 48:1017–1059
Fried NM, Tesfaye Z, Ong AM, Rha KH, Hejazi P (2003) Optimization of the erbium:YAG laser for precise incision of ureteral and urethral tissues: in vitro and in vivo results. Lasers Surg Med 33(2):108–114
Stübinger S, Ghanaati S, Saldamli B, Kirkpatrick CJ, Sader R (2009) Er:YAG laser osteotomy: preliminary clinical and histological results of a new technique for contact-free bone surgery. Eur Surg Res 42(3):150–156
Romeo U, Del Vecchio A, Palaia G, Tenore G, Visca P, Maggiore C (2009) Bone damage induced by different cutting instruments – an in vitro study. Braz Dent J 20(2):162–168
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Romeo, U., Libotte, F., Palaia, G. et al. Histological in vitro evaluation of the effects of Er:YAG laser on oral soft tissues. Lasers Med Sci 27, 749–753 (2012). https://doi.org/10.1007/s10103-011-0969-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-011-0969-z