Abstract
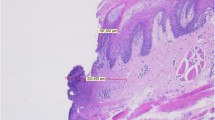
Since the introduction of laser in clinical practice, different wavelengths have been used for oral surgery on the basis of the different characteristics and affinities of each one. The aim of this study was a comparison of different laser wavelengths in relation to both thermal increase and “histological quality” in a model of soft tissue surgery procedures. Thermal evaluation was realized, during laser-assisted surgery excision performed on a bovine tongue, by a thermal camera device to evaluate thermal increase on the surface of the sample and with four thermocouples to evaluate thermal increase on the depth of the specimen; temperature was recorded before starting surgical procedure and at the peak of every excision. The quality of excision, in terms of tissue damage and regularity, was realized by two blind examiners on the basis of established criteria. The highest superficial thermal increase was recorded for Superpulse 5-W CO2 laser, the lowest one for Er:YAG laser. The highest in depth thermal increase was recorded for 5 W Diode laser, the lowest one for Er:YAG laser. The best quality of incision was obtained with a 3-W CO2 laser and 3-W diode laser; epithelial, stromal, and vascular damages were evaluated with different degrees for all the used wavelengths with the best result, in terms of “tissue respect,” for Er:YAG laser. In all the surgical procedures performed, thermal increase was evaluated until the end of the procedure; at remaining tissue level, thermal decrease was evaluable in the few seconds after surgery. The Er:YAG laser was the device with a lower influence on thermal increase; CO2 and diode lasers revealed a good histological quality. Further studies may be necessary to test the reliability of laser devices for the excision of all the types of specimens needing histological evaluation and diagnosis.






Similar content being viewed by others
References
Frame JW, Morgan D, Rhys Evans PH (1988) Tongue resection with the CO2 laser: the effects of past radiotherapy on postoperative complications. Br J Oral Maxillofac Surg 26(6):464–471
Wang X, Ishizaki NT, Matsumoto K (2005) Healing process of skin after CO2 laser ablation at low irradiance: a comparison of continuous-wave and pulsed mode. Photomed Laser Surg 23(1):20–26
Niemz MH (2007) Laser-tissue interactions. Fundamentals and applications. 3rd edn, Springer
Sperandio FF, Meneguzzo DT, Ferreira LS, da Ana PA, Azevedo LH, de Sousa SC (2011) Different air–water spray regulations affect the healing of Er, Cr:YSGG laser incisions. Lasers Med Sci 26(2):257–265
Fornaini C, Rocca JP, Merigo E, Meleti M, Manfredi M, Nammour S, Vescovi P (2011) Low energy KTP laser in oral soft tissue surgery: a 52 patients clinical study. Med Oral Med Buc Cir Buc 17(2):e287–e291
Gómez-Santos L, Arnabat-Domínguez J, Sierra-Rebolledo A, Gay-Escoda C (2010) Thermal increment due to ErCr:YSGG and CO2 laser irradiation of different implant surfaces. A pilot study. Med Oral Patol Oral Cir Bucal 15(5):e782–e787
Sun H, Mikula E, Kurtz RM, Juhasz T (2010) Temperature increase in human cadaver retina during direct illumination by femtosecond laser pulses. J Refract Surg 26(4):272–277
George J, Bensafi A, Schmitt AM, Black D, Dahan S, Loche F, Lagarde JM (2008) Validation of a non-contact technique for local skin temperature measurements. Skin Res Technol 14(4):381–384
Vescovi P, Corcione L, Meleti M, Merigo E, Fornaini C, Manfredi M, Bonanini M, Govoni P, Rocca JP, Nammour S (2010) Nd:YAG laser versus traditional scalpel. A preliminary histological analysis of specimens from the human oral mucosa. Lasers Med Sci 25(5):685–691
Rizzo LB, Ritchey JW, Higbee RG, Bartels KE, Lucroy MD (2004) Histologic comparison of skin biopsy specimens collected by use of carbon dioxide or 810-nm diode lasers from dogs. J Am Vet Med Assoc 225(10):1562–1566
Oelgiesser D, Blasbalg J, Ben-Amar A (2003) Cavity preparation by Er-YAG laser on pulpal temperature rise. Am J Dent 16(2):96–98
Martins GR, Cavalcanti BN, Rode SM (2006) Increases in intrapulpal temperature during polymerization of composite resin. J Prosthet Dent 96(5):328–331
Sulieman M, Rees JS, Addy M (2006) Surface and pulp chamber temperature rises during tooth bleaching using a diode laser: a study in vitro. Br Dent J 200(11):631–634
Augustin G, Davila S, Mihoci K, Udiljak T, Vedrina DS, Antabak A (2008) Thermal osteonecrosis and bone drilling parameters revisited. Arch Orthop Trauma Surg 128(1):71–77
Augustin G, Davila S, Udiljak T, Vedrina DS, Bagatin D (2009) Determination of spatial distribution of increase in bone temperature during drilling by infrared thermography: preliminary report. Arch Orthop Trauma Surg 129(5):703–709
Sedlin ED, Hirsch C (1966) Factors affecting the determination of the physical properties of femoral cortical bone. Acta Orthop Scand 37(1):29–48
Geminiani A, Caton JG, Romanos GE (2011) Temperature change during non-contact diode laser irradiation of implant surfaces. Lasers Med Sci 27(2):339–342
DiBernardo BE, Reyes J, Chen B (2009) Evaluation of tissue thermal effects from 1064/1320-nm laser-assisted lipolysis and its clinical implications. J Cosmet Laser Ther 11(2):62–69
Miserendino LJ, Abt E, Wigdor H, Miserendino CA (1993) Evaluation of thermal cooling mechanisms for laser application to teeth. Lasers Surg Med 13(1):83–88
Silverman EB, Read RW, Boyle CR, Cooper R, Miller WW, McLaughlin RM (2007) Histologic comparison of canine skin biopsies collected using monopolar electrosurgery, CO2 laser, radiowave radiosurgery, skin biopsy punch, and scalpel. Vet Surg 36(1):50–56
Reimer SB, Séguin B, DeCock HE, Walsh PJ, Kass PH (2005) Evaluation of the effect of routine histologic processing on the size of skin samples obtained from dogs. Am J Vet Res 66(3):500–505
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Merigo, E., Clini, F., Fornaini, C. et al. Laser-assisted surgery with different wavelengths: a preliminary ex vivo study on thermal increase and histological evaluation. Lasers Med Sci 28, 497–504 (2013). https://doi.org/10.1007/s10103-012-1081-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-012-1081-8