Abstract
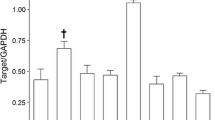
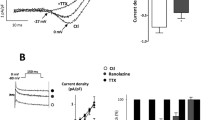
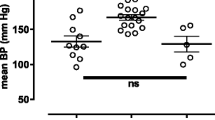
The L-type calcium channel (LCC) plays a regulatory role in various physical and pathological processes. In the vasculature, LCCs mediate agonist-induced vascular smooth muscle contraction. However, whether LCC-mediated vessel responses to certain vasoconstrictors vary among species remains unclear. The coronary arteries were dissected from the hearts of rats and mice. Coronary arterial ring contraction was measured using the Multi Myograph system. High K+ (60 mM)-induced coronary artery contractions were stronger in rats than in mice, whereas CaCl2-induced contraction curves did not differ significantly between the two groups. Endothelin-1, U46619 (thromboxane A2 receptor agonist), and 5-hydroxytryptamine (5-HT) induced concentration-dependent vasoconstriction of coronary arterial rings in rats and mice. The vessel rings of mice were more sensitive to ET-1 and U46619 and less sensitive to 5-HT than those of rats. The LCC blocker nifedipine significantly inhibited coronary artery contractions induced by ET-1, U46619, and 5-HT. The inhibitory effect of 1 μM nifedipine on ET-1- and 5-HT-induced coronary artery contractions was stronger in mice than in rats, whereas its effect on U46619-induced vessel contractions was weaker in mice than in rats. The 5-HT2A receptor and LCC mRNA levels were higher in the coronary arteries of rats than in those of mice, whereas the expressions of the ETA and TXA2 receptors and Orai1 mRNA levels were comparable between the two groups. LCC plays an important role in coronary arterial contraction. Rats and mice show different responses to vasoconstrictors and LCC blockers, suggesting that the coronary arteries of rats and mice have different biological characteristics.





Similar content being viewed by others
References
Alapati VR, McKenzie C, Blair A, Kenny D, MacDonald A, Shaw AM (2009) Mechanisms of U46619- and 5-HT-induced contraction of bovine pulmonary arteries: role of chloride ions. Br J Pharmacol 151:1224–1234
Benitah JP, Alvarez JL, Gomez AM (2010) L-type Ca2+ current in ventricular cardiomyocytes. J Mol Cell Cardiol 48:26–36
Bolotina VM (2012) Orai1, STIM1, and iPLA2 determine arterial vasoconstriction. Arterioscler Thromb Vasc Biol 32:1066–1067
Dominguez-Rodriguez A, Diaz I, Rodriguez-Moyano M, Calderon-Sanchez E, Rosado JA, Ordonez A, Smani T (2012) Urotensin-II signaling mechanism in rat coronary artery: role of STIM1 and Orai1-dependent store operated calcium influx in vasoconstriction. Arterioscler Thromb Vasc Biol 32:1325–1332
Elmoselhi AB, Grover AK (1997) Endothelin contraction in pig coronary artery: receptor types and Ca(2+)-mobilization. Mol Cell Biochem 176:29–33
Halcox JP, Nour KR, Zalos G, Quyyumi AA (2001) Coronary vasodilation and improvement in endothelial dysfunction with endothelin ET(A) receptor blockade. Circ Res 89:969–976
Halcox JP, Nour KR, Zalos G, Quyyumi AA (2007) Endogenous endothelin in human coronary vascular function: differential contribution of endothelin receptor types A and B. Hypertension 49:1134–1141
Higashino R, Sato R, Jin H, Inoue N, Fukuta Y, Kurimoto T, Tamaki H (1997) Inhibitory effects of efonidipine hydrochloride on contraction induced by several vasoconstrictors in porcine coronary artery: comparison with effects of nifedipine and nisoldipine. J Cardiovasc Pharmacol 29:624–630
Ito A, Shimokawa H, Nakaike R, Fukai T, Sakata M, Takayanagi T, Egashira K, Takeshita A (1994) Role of protein kinase C-mediated pathway in the pathogenesis of coronary artery spasm in a swine model. Circulation 90:2425–2431
Katugampola SD, Davenport AP (2001) Thromboxane receptor density is increased in human cardiovascular disease with evidence for inhibition at therapeutic concentrations by the AT(1) receptor antagonist losartan. Br J Pharmacol 134:1385–1392
Kawanabe Y, Masaki T, Hashimoto N (2006) Involvement of phospholipase C in endothelin 1-induced stimulation of Ca++ channels and basilar artery contraction in rabbits. J Neurosurg 105:288–293
Kizub IV, Klymenko KI, Soloviev AI (2014) Protein kinase C in enhanced vascular tone in diabetes mellitus. Int J Cardiol 174:230–242
Kruse HJ, Bauriedel G, Heimerl J, Hofling B, Weber PC (1994) Role of L-type calcium channels on stimulated calcium influx and on proliferative activity of human coronary smooth muscle cells. J Cardiovasc Pharmacol 24:328–335
Kuga T, Shimokawa H, Hirakawa Y, Kadokami Y, Arai Y, Fukumoto Y, Kuwata K, Kozai T, Egashira K, Takeshita A (2000) Increased expression of L-type calcium channels in vascular smooth muscle cells at spastic site in a porcine model of coronary artery spasm. J Cardiovasc Pharmacol 35:822–828
Matchkov VV, Kudryavtseva O, Aalkjaer C (2012) Intracellular Ca2+ signalling and phenotype of vascular smooth muscle cells. Basic Clin Pharmacol Toxicol 110:42–48
Nichols DE, Nichols CD (2008) Serotonin receptors. Chem Rev 108:1614–1641
Salamanca DA, Khalil RA (2005) Protein kinase C isoforms as specific targets for modulation of vascular smooth muscle function in hypertension. Biochem Pharmacol 70:1537–1547
Soboloff J, Rothberg BS, Madesh M, Gill DL (2012) STIM proteins: dynamic calcium signal transducers. Nat Rev Mol Cell Biol 13:549–565
Somlyo AP, Somlyo AV (2003) Ca2+ sensitivity of smooth muscle and nonmuscle myosin II: modulated by G proteins, kinases, and myosin phosphatase. Physiol Rev 83:1325–1358
Acknowledgments
This work was supported by the National Natural Science Foundation of China (grant numbers 81273516, 81270222, 81302779, and 81470440) and by Guangdong Provincial Natural Science Foundation (S2013010014762 and S2013040014689).
Conflict of interest
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Hui Yang and Su-Juan Kuang contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 17.8 kb)
Rights and permissions
About this article
Cite this article
Yang, H., Kuang, SJ., Rao, F. et al. Species-specific differences in the role of L-type Ca2+ channels in the regulation of coronary arterial smooth muscle contraction. Naunyn-Schmiedeberg's Arch Pharmacol 389, 151–157 (2016). https://doi.org/10.1007/s00210-015-1173-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-015-1173-7