Abstract
Purpose
This study aimed to review the literature on the prevalence of sleep-disordered breathing (SDB) in patients with acute coronary syndrome (ACS).
Methods
Relevant studies were searched on PubMed, EMBASE, and Cochrane Library through December 2014. Data were extracted using standardized forms. Pooled prevalence of all SDB (apnea-hypopnea index (AHI) > 5), moderate-to-severe SDB (AHI > 15), and severe SDB (AHI > 30) in ACS patients was calculated using DerSimonian-Laird random-effects model. Sensitivity analysis was performed based on races and diagnostic methods of SDB.
Results
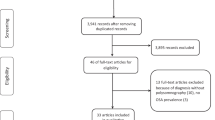
A total of 32 studies were included in the present meta-analysis, examining 3360 patients. The meta-analysis indicated that pooled prevalence of all SDB (AHI > 5), moderate-to-severe SDB (AHI > 15), and severe SDB (AHI > 30) in ACS patients were 69 % (95 % confidence interval (CI) = 61, 77 %), 43 % (95 % CI = 36, 49 %), and 25 % (95 % CI = 17, 33 %), respectively. Sensitivity analysis indicated that the pooled prevalence of SDB in Western population was similar to that in Asian population. However, diagnostic methods of SDB seemed to have various impacts on the prevalence of all SDB (AHI > 5), moderate-to-severe SDB (AHI > 15), and severe SDB (AHI > 30).
Conclusions
High prevalence of all SDB, moderate-to-severe SDB, and severe SDB was found in ACS patients. It is clinically important to screen for SDB in patients with ACS.






Similar content being viewed by others
References
Young T, Palta M, Dempsey J, et al. (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Vozoris NT (2012) Sleep apnea-plus: prevalence, risk factors, and association with cardiovascular diseases using United States population-level data. Sleep Med 13(6):637–644
Kohler M, Stradling JR (2010) Mechanisms of vascular damage in obstructive sleep apnea. Nat Rev Cardiol 7(12):677–685
Somers VK, White DP, Amin R, et al. (2008) Sleep apnea and cardiovascular disease: an American Heart Association/American College of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council on Cardiovascular Nursing. In collaboration with the National Heart, Lung, and Blood Institute National Center on Sleep Disorders Research (National Institutes of Health). Circulation 118(10):1080–1111
Fiuzat M, Oldenberg O, Whellan DJ, et al. (2016) Lessons learned from a clinical trial: design, rationale, and insights from The Cardiovascular Improvements with Minute Ventilation-targeted Adaptive Servo-Ventilation (ASV) Therapy in Heart Failure (CAT-HF) Study. Contemp Clin Trials 47:158–164
Shah NA, Yaggi HK, Concato J, et al. (2010) Obstructive sleep apnea as a risk factor for coronary events or cardiovascular death. Sleep Breath 14(2):131–136
Nakashima H, Kurobe M, Minami K, et al. (2015) Effects of moderate-to-severe obstructive sleep apnea on the clinical manifestations of plaque vulnerability and the progression of coronary atherosclerosis in patients with acute coronary syndrome. Eur Heart J Acute Cardiovasc Care 4(1):75–84
Liu B, Guo R, Zhou S, et al. (2014) Effects of obstructive sleep apnea on cardiac function and clinical outcomes in Chinese patients with ST-elevation myocardial infarction. Sci World J 2014:908582
Ben Ahmed H, Boussaid H, Hamdi I, et al. (2014) Prevalence and predictors of obstructive sleep apnea in patients admitted for acute myocardial infarction. Ann Cardiol Angeiol (Paris) 63(2):65–70
Loo G, Tan AY, Koo CY, et al. (2014) Prognostic implication of obstructive sleep apnea diagnosed by post-discharge sleep study in patients presenting with acute coronary syndrome. Sleep Med 15(6):631–636
Kukwa W, Glowczynska R, Filipiak KJ, et al. (2013) Serum EPO and VEGF levels in patients with sleep-disordered breathing and acute myocardial infarction. Sleep Breath 17(3):1063–1069
Ludka O, Stepanova R, Vyskocilova M, et al. (2014) Sleep apnea prevalence in acute myocardial infarction—the Sleep Apnea in Post-acute Myocardial Infarction Patients (SAPAMI) Study. Int J Cardiol 176(1):13–19
Low TT, Hong WZ, Tai BC, et al. (2013) The influence of timing of polysomnography on diagnosis of obstructive sleep apnea in patients presenting with acute myocardial infarction and stable coronary artery disease. Sleep Med 14(10):985–990
Garcia-Rio F, Alonso-Fernández A, Armada E, et al. (2013) CPAP effect on recurrent episodes in patients with sleep apnea and myocardial infarction. Int J Cardiol 168(2):1328–1335
Hayashi H, Fukuma N, Kato K, et al. (2013) Clinical backgrounds and the time course of sleep-disordered breathing in patients after myocardial infarction. J Nippon Med Sch 80(3):192–199
Hein T, Loo G, Ng WY, Tai BC, et al. (2013) Relationship between apnoea-hypopnoea index and angiographic coronary disease phenotypes in patients presenting with acute myocardial infarction. Acute Card Care 15(2):26–33
Hetzenecker A, Buchner S, Greimel T, et al. (2013) Cardiac workload in patients with sleep-disordered breathing early after acute myocardial infarction. Chest 143(5):1294–1301
Buchner S, Greimel T, Hetzenecker A, et al. (2012) Natural course of sleep-disordered breathing after acute myocardial infarction. Eur Respir J 40(5):1173–1179
Sert Kuniyoshi FH, Zellmer MR, Calvin AD, et al. (2011) Diagnostic accuracy of the Berlin questionnaire in detecting sleep-disordered breathing in patients with a recent myocardial infarction. Chest 140(5):1192–1197
Fumagalli S, Tarantini F, Cipriani C, et al. (2010) Obstructive sleep apnea after myocardial infarction. Int J Cardiol 145(3):550–552
Konecny T, Kuniyoshi FH, Orban M, et al. (2010) Under-diagnosis of sleep apnea in patients after acute myocardial infarction. J Am Coll Cardiol 56(9):742–743
Yao LM (2010) Effects of obstructive sleep apnea on restenosis following coronary artery stent implantation. Journal of Clinical Rehabilitative Tissue Engineering Research 14(9):1700–1702
Lee CH, Khoo SM, Tai BC, et al. (2009) Obstructive sleep apnea in patients admitted for acute myocardial infarction. Prevalence, predictors, and effect on microvascular perfusion. Chest 135(6):1488–1495
Kuniyoshi FH, Garcia-Touchard A, Gami AS, et al. (2008) Day-night variation of acute myocardial infarction in obstructive sleep apnea. J Am Coll Cardiol 52(5):343–346
Tsukamoto K, Ohara A (2006) Temporal worsening of sleep-disordered breathing in the acute phase of myocardial infarction. Circ J 70(12):1553–1556
Junker-Neff A, Eberle R, V Arnim T, et al. (2005) Is there an association between the sleep apnea syndrome and the circadian peak of myocardial infarction in the morning hours? Dtsch Med Wochenschr 130(49):2818–2822
Moruzzi P, Sarzi-Braga S, Rossi M, et al. (1999) Sleep apnoea in ischaemic heart disease: differences between acute and chronic coronary syndromes. Heart 82(3):343–347
Yano Y, Ohmori T, Shimada K, et al. (2012) Association of sleep onset of acute coronary syndrome with sleep apnea syndrome and abnormal diurnal variation of hemostasis and adipokine levels. Blood Coagul Fibrinolysis 23(7):590–596
Schiza SE, Simantirakis E, Bouloukaki I, et al. (2012) Sleep disordered breathing in patients with acute coronary syndromes. J Clin Sleep Med 8(1):21–26
Areias V, Romero J, Cunha K, et al. (2012) Sleep apnea-hypopnea syndrome and acute coronary syndrome—an association not to forget. Rev Port Pneumol 18(1):22–28
Faria R, Areias V, Romero J, et al. (2011) Acute coronary syndrome and sleep apnea syndrome, a surprising association? Eur Heart J 32(SUPPL.1):99
Takama N, Kurabayashi M (2007) Possibility of close relationship between sleep disorder breathing and acute coronary syndrome. J Cardiol 49(4):171–177
Yumino D, Tsurumi Y, Takagi A, et al. (2007) Impact of obstructive sleep apnea on clinical and angiographic outcomes following percutaneous coronary intervention in patients with acute coronary syndrome. Am J Cardiol 99(1):26–30
Mehra R, Principe-Rodriguez K, Kirchner HL, et al. (2006) Sleep apnea in acute coronary syndrome: high prevalence but low impact on 6-month outcome. Sleep Med 7(6):521–528
Nakagawa Y, Kishida K, Mazaki T, et al. (2011) Impact of sleep-disordered breathing, visceral fat accumulation and adiponectin levels in patients with night-time onset of acute coronary syndrome. Am J Cardiol 108(9):1266–1271
Meng S, Fang L, Wang CQ, et al. (2009) Impact of obstructive sleep apnoea on clinical characteristics and outcomes in patients with acute coronary syndrome following percutaneous coronary intervention. J Int Med Res 37(5):1343–1353
Ishibashi Y, Osada N, Sekiduka H, et al. (2009) Peak time of acute coronary syndrome in patients with sleep disordered breathing. J Cardiol 53(2):164–170
BaHammam A, Al-Mobeireek A, Al-Nozha M, et al. (2005) Behaviour and time-course of sleep disordered breathing in patients with acute coronary syndromes. Int J Clin Pract 59(8):874–880
Van den Broecke S, Jobard O, Montalescot G, et al. (2014) Very early screening for sleep-disordered breathing in acute coronary syndrome in patients without acute heart failure. Sleep Med 15(12):1539–1546
Buchner S, Eglseer M, Debl K, et al. (2015) Sleep disordered breathing and enlargement of the right heart after myocardial infarction. Eur Respir J 45(3):680–690
Qaseem A, Holty JE, Owens DK, et al. (2013) Management of obstructive sleep apnea in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med 159(7):471–483
Liberati A, Altman DG, Tetzlaff J, et al. (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62(10):e1–34
Berry RB, Budhiraja R, Gottlieb DJ, et al. (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8(5):597–619
von Elm E, Altman DG, Egger M, et al. (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370(9596):1453–1457
Sutton AJ, Abrams KR, Jones DR, et al. (2000) Methods for meta-analysis in medical research. John Wiley & Sons, Ltd, Chichester, England
Batham A, Narula D, Toteja T, et al. (2007) Systematic review and meta-analysis of prevalence of hepatitis B in India. Indian Pediatr 44(9):663–674
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Fleiss JL (1993) The statistical basis of meta-analysis. Stat Methods Med Res 2(2):121–145
Egger M, Davey Smith G, Schneider M, et al. (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Shah N, Redline S, Yaggi HK, et al. (2013) Obstructive sleep apnea and acute myocardial infarction severity: ischemic preconditioning? Sleep Breath 17(2):819–826
Nakashima H, Henmi T, Minami K, et al. (2013) Obstructive sleep apnoea increases the incidence of morning peak of onset in acute myocardial infarction. Eur Heart J Acute Cardiovasc Care 2(2):153–158
Nakashima H, Muto S, Amenomori K, et al. (2011) Impact of obstructive sleep apnea on myocardial tissue perfusion in patients with ST-segment elevation myocardial infarction. Circ J 75(4):890–896
Nakashima H, Katayama T, Takagi C, et al. (2006) Obstructive sleep apnoea inhibits the recovery of left ventricular function in patients with acute myocardial infarction. Eur Heart J 27(19):2317–2322
Joyeux-Faure M, Stanke-Labesque F, Lefebvre B, et al. (2005) Chronic intermittent hypoxia increases infarction in the isolated rat heart. J Appl Physiol (1985) 98(5):1691–1696
Ramond A, Godin-Ribuot D, Ribuot C, et al. (2013) Oxidative stress mediates cardiac infarction aggravation induced by intermittent hypoxia. Fundam Clin Pharmacol 27(3):252–261
Buchner S, Satzl A, Debl K, et al. (2014) Impact of sleep-disordered breathing on myocardial salvage and infarct size in patients with acute myocardial infarction. Eur Heart J 35(3):192–199
Netzer NC, Stoohs RA, Netzer CM, et al. (1999) Using the Berlin questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131(7):485–491
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Szymanski FM, Filipiak KJ, Hrynkiewicz-Szymanska A, et al. (2013) Clinical characteristics of patients with acute coronary syndrome at high clinical suspicion for obstructive sleep apnea syndrome. Hell J Cardiol 54(5):348–354
Correia LC, Souza AC, Garcia G, et al. (2012) Obstructive sleep apnea affects hospital outcomes of patients with non-ST-elevation acute coronary syndromes. Sleep 35(9):1241–125A
Loo G, Hein T, Tai BC, et al. (2013) Screening of hospitalized patients at high risk of obstructive sleep apnea in general cardiology service. Int J Cardiol 164(3):368–370
Jesus EV, Dias-Filho EB, Mota Bde M, et al. (2010) Suspicion of obstructive sleep apnea by Berlin questionnaire predicts events in patients with acute coronary syndrome. Arq Bras Cardiol 95(3):313–320
Bitter T, Westerheide N, Hossain SM, et al. (2012) Symptoms of sleep apnoea in chronic heart failure—results from a prospective cohort study in 1,500 patients. Sleep Breath 16(3):781–791
Collop NA (2008) Portable monitoring for the diagnosis of obstructive sleep apnea. Curr Opin Pulm Med 14(6):525–529
Kushida CA, Littner MR, Morgenthaler T, et al. (2005) Practice parameters for the indications for polysomnography and related procedures: an update for 2005. Sleep 28(4):499–521
Skinner MA, Choudhury MS, Homan SD, et al. (2005) Accuracy of monitoring for sleep-related breathing disorders in the coronary care unit. Chest 127(1):66–71
Oldenburg O, Lamp B, Faber L, et al. (2007) Sleep-disordered breathing in patients with symptomatic heart failure: a contemporary study of prevalence in and characteristics of 700 patients. Eur J Heart Fail 9(3):251–257
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Comments
This study examined the prevalence of SDB in patients with heart disease showing that it is common and therefore likely to be under diagnosed in patients presenting primarily with heart disease. It can be seen the relationship is present in all populations studied. Given that patients with both SDB and heart disease are predominantly not sleepy the goal of treatment should be outcomes driven which was not examined in this meta-analysis.
Ian Wilcox
NSW, Australia
Rights and permissions
About this article
Cite this article
Huang, Z., Zheng, Z., Luo, Y. et al. Prevalence of sleep-disordered breathing in acute coronary syndrome: a systemic review and meta-analysis. Sleep Breath 21, 217–226 (2017). https://doi.org/10.1007/s11325-016-1398-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1398-9