Abstract
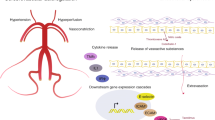
Posterior reversible encephalopathy syndrome (PRES) is a clinicoradiological entity characterized by a typical brain edema. Its pathogenesis is still debated through hypoperfusion and hyperperfusion theories, which have many limitations. As PRES occurs almost exclusively in clinical situations with arginine vasopressin (AVP) hypersecretion, such as eclampsia and sepsis, we hypothesize that AVP plays a central pathophysiologic role. In this review, we discuss the genesis of PRES and its symptoms through this novel approach. We theorize that AVP axis stimulation precipitates PRES development through an increase in AVP secretion or AVP receptor density. Activation of vasopressin V1a receptors leads to cerebral vasoconstriction, causing endothelial dysfunction and cerebral ischemia. This promotes cytotoxic edema through hydromineral transglial flux dysfunction and may increase endothelial permeability, leading to subsequent vasogenic brain edema. If our hypothesis is confirmed, it opens new perspectives for better patient monitoring and therapies targeting the AVP axis in PRES.


Similar content being viewed by others
References
Hinchey J, Chaves C, Appignani B, Breen J, Pao L, Wang A, Pessin MS, Lamy C et al (1996) A reversible posterior leukoencephalopathy syndrome. N Engl J Med 334:494–500. https://doi.org/10.1056/NEJM199602223340803
Gao B, Lyu C, Lerner A, McKinney AM (2018) Controversy of posterior reversible encephalopathy syndrome: what have we learnt in the last 20 years? J Neurol Neurosurg Psychiatry 89:14–20. https://doi.org/10.1136/jnnp-2017-316225
Toledano M, Fugate JE (2017) Posterior reversible encephalopathy in the intensive care unit. In: Wijdicks EFM, Kramer AH (eds) Handbook of clinical neurology, 3rd series. Elsevier, Chapter 26, Volume 141, pp 467–483
Fugate JE, Claassen DO, Cloft HJ, Kallmes DF, Kozak OS, Rabinstein AA (2010) Posterior reversible encephalopathy syndrome: associated clinical and radiologic findings. Mayo Clin Proc 85:427–432. https://doi.org/10.4065/mcp.2009.0590
Garg RK, Kumar N, Malhotra HS (2018) Posterior reversible encephalopathy syndrome in eclampsia. Neurol India 66:1316–1323. https://doi.org/10.4103/0028-3886.241364
Bartynski WS, Boardman JF, Zeigler ZR, Shadduck RK, Lister J (2006) Posterior reversible encephalopathy syndrome in infection, sepsis, and shock. AJNR Am J Neuroradiol 27:2179–2190
Graham BR, Pylypchuk GB (2014) Posterior reversible encephalopathy syndrome in an adult patient undergoing peritoneal dialysis: a case report and literature review. BMC Nephrol 15(10). https://doi.org/10.1186/1471-2369-15-10
Gavrilovici C, Miron I, Voroneanu L, Bădărau S, Stârcea M (2017) Posterior reversible encephalopathy syndrome in children with kidney disease. Int Urol Nephrol 49:1793–1800. https://doi.org/10.1007/s11255-017-1684-x
Mizutani M, Nakamori Y, Sakaguchi H, Kageyama Y, Oya E, Ino K, Suzuki K, Sekine T (2013) Development of syndrome of inappropriate secretion of ADH and reversible posterior leukoencephalopathy during initial rituximab-CHOP therapy in a patient with diffuse large B-cell lymphoma. Rinsho Ketsueki 54:269–272
Mohanlal S, Ghildiyal RG, Kondekar A et al (2016) A commonly missed well known entity- acute intermittent porphyria: a case report. J Clin Diagn Res 10:SD01–SD02. https://doi.org/10.7860/JCDR/2016/20464.8609
Sun I, Sun A, Gercek A, Kilic T (2007) Desmopressin-induced hypertension as a rare cause of hypertensive encephalopathy. J Neurosurg Anesthesiol 19:289–290. https://doi.org/10.1097/ANA.0b013e318150e0f8
Wei R, Jin L, Huang J, Luo B (2012) Desmopressin-induced posterior reversible encephalopathy syndrome. Intern Med 51:3081–3084
Ohtonari T, Hashimoto M, Urasaki E, Yokota A, Araki S, Asayama K, Shirahata A (2005) Prolonged cerebral salt wasting following craniopharyngioma surgery and posterior reversible encephalopathy syndrome: a case report. No To Shinkei 57:57–63
Ozyurek H, Oguz G, Ozen S, Akyuz C, Oguz KK, Anlar B, Aysun S (2005) Reversible posterior leukoencephalopathy syndrome: report of three cases. J Child Neurol 20:990–993. https://doi.org/10.1177/08830738050200121201
Katano K, Kakuchi Y, Nakashima A, Nakahama K, Kawano M (2010) Apparent diffusion coefficient map based on diffusion-weighted magnetic resonance imaging is useful in diagnosing the brainstem variant of reversible posterior leukoencephalopathy syndrome with uremia. Clin Exp Nephrol 14:479–482. https://doi.org/10.1007/s10157-010-0293-0
Aulakh P, Fatakhov E, Koch CF, Kapil S (2013) Posterior reversible encephalopathy syndrome with documented hyponatraemia. BMJ Case Rep 2013:bcr2013009311. https://doi.org/10.1136/bcr-2013-009311
Jeon J-S, Park S-P, Seo J-G (2014) Posterior reversible encephalopathy syndrome due to hyponatremia. J Epilepsy Res 4:31–33 https://doi.org/2014.4.1.31
Eroglu N, Bahadir A, Erduran E (2017) A case of ALL developing posterior reversible encephalopathy secondary to hyponatremia. J Pediatr Hematol Oncol 39:e476–e478. https://doi.org/10.1097/MPH.0000000000000827
Parikh P, Duhame D, Monahan L, Woroniecki R (2015) Renal artery stenosis precipitates hyponatremic hypertensive syndrome and posterior reversible leukoencephalopathy. Front Pediatr 3. https://doi.org/10.3389/fped.2015.00040
Duchnowska R, Miciuk B, Bodnar L, Waśniewski L, Szczylik C (2013) Severe neurological symptoms in a patient with advanced renal cell carcinoma treated with sunitinib. J Oncol Pharm Pract 19:186–189. https://doi.org/10.1177/1078155212457967
Bartynski WS, Tan HP, Boardman JF, Shapiro R, Marsh JW (2008) Posterior reversible encephalopathy syndrome after solid organ transplantation. AJNR Am J Neuroradiol 29:924–930. https://doi.org/10.3174/ajnr.A0960
How J, Blattner M, Fowler S, Wang-Gillam A, Schindler SE (2016) Chemotherapy-associated posterior reversible encephalopathy syndrome: a case report and review of the literature. The Neurologist 21(6):112–117. https://doi.org/10.1097/NRL.0000000000000105
Tlemsani C, Mir O, Boudou-Rouquette P, Huillard O, Maley K, Ropert S, Coriat R, Goldwasser F (2011) Posterior reversible encephalopathy syndrome induced by anti-VEGF agents. Target Oncol 6:253–258. https://doi.org/10.1007/s11523-011-0201-x
Shah RR (2017) Anti-angiogenic tyrosine kinase inhibitors and reversible posterior leukoencephalopathy syndrome: could hypomagnesaemia be the trigger? Drug Saf 40:373–386. https://doi.org/10.1007/s40264-017-0508-3
Parikh NS, Schweitzer AD, Young RJ, Giambrone AE, Lyo J, Karimi S, Knobel A, Gupta A et al (2017) Corticosteroid therapy and severity of vasogenic edema in posterior reversible encephalopathy syndrome. J Neurol Sci 380:11–15. https://doi.org/10.1016/j.jns.2017.06.044
Loens S, Conzen J, Welte GS, Scharn N, Schrader C, Weissenborn K (2015) Reversible posterior leukoencephalopathy syndrome after withdrawal of antipsychotic medication in the context of lithium intoxication. Gen Hosp Psychiatry 37:274.e3–274.e5. https://doi.org/10.1016/j.genhosppsych.2015.02.011
Fitzgerald RT, Fitzgerald CT, Samant RS, Kumar M, Ramakrishniah R, van Hemert R, Angtuaco EJ (2015) Lithium toxicity and PRES: a novel association. J Neuroimaging 25:147–149. https://doi.org/10.1111/jon.12094
McKinney AM, Short J, Truwit CL et al (2007) Posterior reversible encephalopathy syndrome: incidence of atypical regions of involvement and imaging findings. AJR Am J Roentgenol 189:904–912. https://doi.org/10.2214/AJR.07.2024
Ishikawa H, Natsume N, Matsui K, Tsuda H (2013) Acute alcohol withdrawal accompanied by posterior reversible encephalopathy syndrome. Psychiatry Clin Neurosci 67:189–189. https://doi.org/10.1111/pcn.12033
Mengi T, Seçil Y, Çoban A, Beckmann Y (2017) Posterior reversible encephalopathy syndrome triggerred by alcohol withdrawal. Turk Psikiyatri Derg 28:217–220
Bazuaye-Ekwuyasi E, Chow RD, Schmalzle S (2017) An atypical subacute presentation of posterior reversible encephalopathy syndrome. J Community Hosp Intern Med Perspect 7:269–274. https://doi.org/10.1080/20009666.2017.1369381
Castillo A, Payne JD, Nugent K (2017) Posterior reversible leukoencephalopathy syndrome after kratom ingestion. Proc (Baylor Univ Med Cent) 30:355–357
Schweitzer AD, Parikh NS, Askin G, Nemade A, Lyo J, Karimi S, Knobel A, Navi BB et al (2017) Imaging characteristics associated with clinical outcomes in posterior reversible encephalopathy syndrome. Neuroradiology 59:379–386. https://doi.org/10.1007/s00234-017-1815-1
Song T, Rao Z, Tan Q, Qiu Y, Liu J, Huang Z, Wang X, Lin T (2016) Calcineurin inhibitors associated posterior reversible encephalopathy syndrome in solid organ transplantation: report of 2 cases and literature review. Medicine (Baltimore) 95:e3173. https://doi.org/10.1097/MD.0000000000003173
Bartynski WS (2008) Posterior reversible encephalopathy syndrome, part 2: controversies surrounding pathophysiology of vasogenic edema. Am J Neuroradiol 29:1043–1049. https://doi.org/10.3174/ajnr.A0929
Gao B, Yu BX, Li RS, Zhang G, Xie HZ, Liu FL, Lv C (2015) Cytotoxic edema in posterior reversible encephalopathy syndrome: correlation of MRI features with serum albumin levels. Am J Neuroradiol 36:1884–1889. https://doi.org/10.3174/ajnr.A4379
Canney M, Kelly D, Clarkson M (2015) Posterior reversible encephalopathy syndrome in end-stage kidney disease: not strictly posterior or reversible. AJN 41:177–182. https://doi.org/10.1159/000381316
Lee VH, Wijdicks EFM, Manno EM, Rabinstein AA (2008) Clinical spectrum of reversible posterior leukoencephalopathy syndrome. Arch Neurol 65:205–210. https://doi.org/10.1001/archneurol.2007.46
Zaman SR (2012) Posterior reversible encephalopathy syndrome postautologous peripheral stem cell transplantation for multiple myeloma. BMJ Case Rep 2012:bcr2012006331. https://doi.org/10.1136/bcr-2012-006331
Matias-Guiu JA, García-Ptacek S, Ordás CM, Marcos-Dolado A, Porta-Etessam J (2012) Recurrent reversible posterior encephalopathy syndrome with a response to nimodipine. Neurologia 27:378–380. https://doi.org/10.1016/j.nrl.2011.12.013
Merayo-Chalico J, Barrera-Vargas A, Juárez-Vega G, Alcocer-Varela J, Arauz A, Gómez-Martín D (2018) Differential serum cytokine profile in patients with systemic lupus erythematosus and posterior reversible encephalopathy syndrome: serum cytokines in SLE and PRES. Clin Exp Immunol 192:165–170. https://doi.org/10.1111/cei.13095
Lv C, Gao B (2015) Serum lactate dehydrogenase as a predictor of outcome in posterior reversible encephalopathy syndrome: imperative to unify. Am J Neuroradiol 36:E29–E30. https://doi.org/10.3174/ajnr.A4243
Fischer M, Schmutzhard E (2017) Posterior reversible encephalopathy syndrome. J Neurol 264:1608–1616. https://doi.org/10.1007/s00415-016-8377-8
Fang X-B, Chen D-J, He F, Chen J, Zhou Z, Liang YL, Zhang WX (2018) Predictors of oedema type in reversible posterior leukoencephalopathy syndrome with preeclampsia or eclampsia. Pregnancy Hypertens 11:71–76. https://doi.org/10.1016/j.preghy.2017.12.011
Morgenthaler NG, Müller B, Struck J et al (2007) Copeptin, a stable peptide of the arginine vasopressin precursor, is elevated in hemorrhagic and septic shock. Shock 28:219–226. https://doi.org/10.1097/SHK.0b013e318033e5da
Lozić M, Šarenac O, Murphy D, Japundžić-Žigon N (2018) Vasopressin, central autonomic control and blood pressure regulation. Curr Hypertens Rep 20:11. https://doi.org/10.1007/s11906-018-0811-0
Sato K, Numata T, Saito T, Ueta Y, Okada Y (2011) V2 receptor-mediated autocrine role of somatodendritic release of AVP in rat vasopressin neurons under hypo-osmotic conditions. Sci Signal 4:ra5. https://doi.org/10.1126/scisignal.2001279
Milutinović-Smiljanić S, Šarenac O, Lozić-Djurić M, Murphy D, Japundžić-Žigon N (2013) Evidence for involvement of central vasopressin V1b and V2 receptors in stress-induced baroreflex desensitization. Br J Pharmacol 169:900–908. https://doi.org/10.1111/bph.12161
Koshimizu T, Nakamura K, Egashira N, Hiroyama M, Nonoguchi H, Tanoue A (2012) Vasopressin V1a and V1b receptors: from molecules to physiological systems. Physiol Rev 92:1813–1864. https://doi.org/10.1152/physrev.00035.2011
Li T, Wang P, Wang SC, Wang Y-F (2017) Approaches mediating oxytocin regulation of the immune system. Front Immunol 7:693. https://doi.org/10.3389/fimmu.2016.00693
Swart RM, Hoorn EJ, Betjes MG, Zietse R (2011) Hyponatremia and inflammation: the emerging role of interleukin-6 in osmoregulation. NEP 118:p45–p51. https://doi.org/10.1159/000322238
Palin K, Moreau ML, Sauvant J, Orcel H, Nadjar A, Duvoid-Guillou A, Dudit J, Rabié A, Moos F (2009) Interleukin-6 activates arginine vasopressin neurons in the supraoptic nucleus during immune challenge in rats. Am J Physiol Endocrinol Metab 296(6):1289–1299. https://doi.org/10.1152/ajpendo.90489.2008
Ohbuchi T, Haam J, Tasker JG (2015) Regulation of neuronal activity in hypothalamic vasopressin neurons. Interdiscip Inf Sci 21:225–234. https://doi.org/10.4036/iis.2015.B.07
Stokum JA, Gerzanich V, Simard JM (2016) Molecular pathophysiology of cerebral edema. J Cereb Blood Flow Metab 36:513–538. https://doi.org/10.1177/0271678X15617172
Wang Y-F, Parpura V (2018) Astroglial modulation of hydromineral balance and cerebral edema. Front Mol Neurosci 11. https://doi.org/10.3389/fnmol.2018.00204
Barreca T, Gandolfo C, Corsini G, del Sette M, Cataldi A, Rolandi E, Franceschini R (2001) Evaluation of the secretory pattern of plasma arginine vasopressin in stroke patients. Cerebrovasc Dis 11:113–118. https://doi.org/10.1159/000047622
Jia S-W, Liu X-Y, Wang SC, Wang Y-F (2016) Vasopressin hypersecretion-associated brain edema formation in ischemic stroke: underlying mechanisms. J Stroke Cerebrovasc Dis 25:1289–1300. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.02.002
Szmydynger-Chodobska J, Chung I, Koźniewska E, Tran B, Harrington FJ, Duncan JA, Chodobski A (2004) Increased expression of vasopressin v1a receptors after traumatic brain injury. J Neurotrauma 21:1090–1102. https://doi.org/10.1089/0897715041651033
Krieg SM, Trabold R, Plesnila N (2017) Time-dependent effects of arginine-vasopressin V1 receptor inhibition on secondary brain damage after traumatic brain injury. J Neurotrauma 34:1329–1336. https://doi.org/10.1089/neu.2016.4514
Park J, Masaki T, Mezaki Y, Yokoyama H, Nakamura M, Maehashi H, Fujimi TJ, Gouraud SS et al (2017) Alpha-1 antichymotrypsin is involved in astrocyte injury in concert with arginine-vasopressin during the development of acute hepatic encephalopathy. PLoS One 12:e0189346. https://doi.org/10.1371/journal.pone.0189346
Magaña SM, Matiello M, Pittock SJ et al (2009) Posterior reversible encephalopathy syndrome in neuromyelitis optica spectrum disorders. Neurology 72:712–717. https://doi.org/10.1212/01.wnl.0000343001.36493.ae
Alonso G, Gallibert E, Lafont C, Guillon G (2008) Intrahypothalamic angiogenesis induced by osmotic stimuli correlates with local hypoxia: a potential role of confined vasoconstriction induced by dendritic secretion of vasopressin. Endocrinology 149:4279–4288. https://doi.org/10.1210/en.2008-0387
Tahara A, Tsukada J, Tomura Y, Yatsu T, Shibasaki M (2011) Vasopressin regulates rat mesangial cell growth by inducing autocrine secretion of vascular endothelial growth factor. J Physiol Sci 61:115–122. https://doi.org/10.1007/s12576-010-0128-5
Afsar B (2017) Pathophysiology of copeptin in kidney disease and hypertension. Clin Hypertens 23:13. https://doi.org/10.1186/s40885-017-0068-y
Łukaszyk E, Małyszko J (2015) Copeptin: pathophysiology and potential clinical impact. Adv Med Sci 60:335–341. https://doi.org/10.1016/j.advms.2015.07.002
Enhörning S, Christensson A, Melander O (2018) Plasma copeptin as a predictor of kidney disease. Nephrol Dial Transplant 34:74–82. https://doi.org/10.1093/ndt/gfy017
Sandgren JA, Scroggins SM, Santillan DA, Devor EJ, Gibson-Corley KN, Pierce GL, Sigmund CD, Santillan MK et al (2015) Vasopressin: the missing link for preeclampsia? Am J Phys Regul Integr Comp Phys 309:R1062–R1064. https://doi.org/10.1152/ajpregu.00073.2015
Scroggins SM, Santillan DA, Lund JM, Sandgren JA, Krotz LK, Hamilton WS, Devor EJ, Davis HA et al (2018) Elevated vasopressin in pregnant mice induces T-helper subset alterations consistent with human preeclampsia. Clin Sci 132:419–436. https://doi.org/10.1042/CS20171059
Conrad KP (2016) G-protein-coupled receptors as potential drug candidates in preeclampsia: targeting the relaxin/insulin-like family peptide receptor 1 for treatment and prevention. Hum Reprod Update 22:647–664. https://doi.org/10.1093/humupd/dmw021
Mendelova A, Holubekova V, Grendar M, Zubor P, Svecova I, Loderer D, Snahnicanova Z, Biringer K et al (2018) Association between 3’UTR polymorphisms in genes ACVR2A, AGTR1 and RGS2 and preeclampsia. Gen Physiol Biophys 37:185–192. https://doi.org/10.4149/gpb_2017028
Jochberger S, Dörler J, Luckner G, Mayr VD, Wenzel V, Ulmer H, Morgenthaler NG, Hasibeder WR et al (2009) The vasopressin and copeptin response to infection, severe sepsis, and septic shock. Crit Care Med 37:476–482. https://doi.org/10.1097/CCM.0b013e3181957532
Palmiere C, Augsburger M (2014) Copeptin as a diagnostic biomarker for sepsis-related deaths. Peptides 59:75–78. https://doi.org/10.1016/j.peptides.2014.07.011
Jiang L, Feng B, Gao D, Zhang Y (2015) Plasma concentrations of copeptin, C-reactive protein and procalcitonin are positively correlated with APACHE II scores in patients with sepsis. J Int Med Res 43:188–195. https://doi.org/10.1177/0300060514561136
Battista S, Audisio U, Galluzzo C, Maggiorotto M, Masoero M, Forno D, Pizzolato E, Ulla M et al (2016) Assessment of diagnostic and prognostic role of copeptin in the clinical setting of sepsis. Biomed Res Int 2016:3624730. https://doi.org/10.1155/2016/3624730
Thanadetsuntorn C, Ngamjanyaporn P, Setthaudom C, Hodge K, Saengpiya N, Pisitkun P (2018) The model of circulating immune complexes and interleukin-6 improves the prediction of disease activity in systemic lupus erythematosus. Sci Rep 8:2620. https://doi.org/10.1038/s41598-018-20947-4
Savioli B, Abdulahad WH, Brouwer E, Kallenberg CGM, de Souza AWS (2017) Are cytokines and chemokines suitable biomarkers for Takayasu arteritis? Autoimmun Rev 16:1071–1078. https://doi.org/10.1016/j.autrev.2017.07.023
Robertson GL (2006) Regulation of arginine vasopressin in the syndrome of inappropriate antidiuresis. Am J Med 119:S36–S42. https://doi.org/10.1016/j.amjmed.2006.05.006
Ellison DH, Berl T (2007) Clinical practice. The syndrome of inappropriate antidiuresis. N Engl J Med 356:2064–2072. https://doi.org/10.1056/NEJMcp066837
Lee G, Lee SE, Ryu K-H, Yoo ES (2013) Posterior reversible encephalopathy syndrome in pediatric patients undergoing treatment for hemophagocytic lymphohistiocytosis: clinical outcomes and putative risk factors. Blood Res 48:258–265. https://doi.org/10.5045/br.2013.48.4.258
Camara-Lemarroy CR, Gonzalez-Moreno EI, de Ortiz-Corona J, Ortiz-Corona JJ, Yeverino-Castro SG, Sanchez-Cardenas M, Nuñez-Aguirre S, Villarreal-Alarcon MA et al (2014) Posterior reversible encephalopathy syndrome due to malignant hypercalcemia: physiopathological considerations. J Clin Endocrinol Metab 99:1112–1116. https://doi.org/10.1210/jc.2013-3487
Gavras I, Hatinoglou S, Benetos A, Gavras H (1986) Calcium stimulates vasopressin release. J Hypertens 4:451–454
Yamamoto S, Morimoto I, Tanaka Y, Yanagihara N, Eto S (2002) The mutual regulation of arginine-vasopressin and PTHrP secretion in dissociated supraoptic neurons. Endocrinology 143:1521–1529. https://doi.org/10.1210/endo.143.4.8720
Zheng X, Liu X, Wang Y, Zhao R, Qu L, Pei H, Tuo M, Zhang Y et al (2018) Acute intermittent porphyria presenting with seizures and posterior reversible encephalopathy syndrome: two case reports and a literature review. Medicine (Baltimore) 97:e11665. https://doi.org/10.1097/MD.0000000000011665
Takata T, Kume K, Kokudo Y, Ikeda K, Kamada M, Touge T, Deguchi K, Masaki T (2017) Acute intermittent porphyria presenting with posterior reversible encephalopathy syndrome, accompanied by prolonged vasoconstriction. Intern Med 56:713–717. https://doi.org/10.2169/internalmedicine.56.7654
Li Y, Qu H, Wang H, Deng H, Liu Z (2015) Novel A219P mutation of hydroxymethylbilane synthase identified in a Chinese woman with acute intermittent porphyria and syndrome of inappropriate antidiuretic hormone. Ann Hum Genet 79:310–312. https://doi.org/10.1111/ahg.12107
Cottet-Maire F, Avdonin PV, Roulet E, Buetler TM, Mermod N, Ruegg UT (2001) Upregulation of vasopressin V1A receptor mRNA and protein in vascular smooth muscle cells following cyclosporin a treatment. Br J Pharmacol 132:909–917. https://doi.org/10.1038/sj.bjp.0703878
Blankenstein KI, Borschewski A, Labes R, Paliege A, Boldt C, McCormick JA, Ellison DH, Bader M et al (2017) Calcineurin inhibitor cyclosporine a activates renal Na-K-Cl cotransporters via local and systemic mechanisms. Am J Physiol Ren Physiol 312:F489–F501. https://doi.org/10.1152/ajprenal.00575.2016
Gullner HG, Campbell WB, Pettinger WA (1979) Role of substance P in water homeostasis. Life Sci 24:2351–2359
Berardi R, Rinaldi S, Caramanti M, Grohè C, Santoni M, Morgese F, Torniai M, Savini A et al (2016) Hyponatremia in cancer patients: time for a new approach. Crit Rev Oncol Hematol 102:15–25. https://doi.org/10.1016/j.critrevonc.2016.03.010
Liamis G, Filippatos TD, Elisaf MS (2016) Electrolyte disorders associated with the use of anticancer drugs. Eur J Pharmacol 777:78–87. https://doi.org/10.1016/j.ejphar.2016.02.064
Cross SN, Ratner E, Rutherford TJ, Schwartz PE, Norwitz ER (2012) Bevacizumab-mediated interference with VEGF signaling is sufficient to induce a preeclampsia-like syndrome in nonpregnant women. Rev Obstet Gynecol 5:2–8
Hagman H, Bendahl P-O, Melander O, Sundberg J, Johnsson A, Belting M (2017) Vasoactive peptides associate with treatment outcome ofbevacizumab-containing therapy in metastatic colorectal cancer. Acta Oncol 56:653–660. https://doi.org/10.1080/0284186X.2017.1302098
Chen H, Modiano MR, Neal JW, Brahmer JR, Rigas JR, Jotte RM, Leighl NB, Riess JW et al (2014) A phase II multicentre study of ziv-aflibercept in combination with cisplatin and pemetrexed in patients with previously untreated advanced/metastatic non-squamous non-small cell lung cancer. Br J Cancer 110:602–608. https://doi.org/10.1038/bjc.2013.735
Berardi R, Santoni M, Rinaldi S, Nunzi E, Smerilli A, Caramanti M, Morgese F, Torniai M et al (2016) Risk of hyponatraemia in cancer patients treated with targeted therapies: a systematic review and meta-analysis of clinical trials. PLoS One 11:e0152079. https://doi.org/10.1371/journal.pone.0152079
Liapis K, Apostolidis J, Charitaki E, Panitsas F, Harhalakis N, Nikiforakis E (2008) Syndrome of inappropriate secretion of antidiuretic hormone associated with imatinib. Ann Pharmacother 42:1882–1886. https://doi.org/10.1345/aph.1L410
Janczar S, Zalewska-Szewczyk B, Mlynarski W (2017) Severe hyponatremia in a single-center series of 84 homogenously treated children with acute lymphoblastic leukemia. J Pediatr Hematol Oncol 39:e54–e58. https://doi.org/10.1097/MPH.0000000000000758
Hill J, Shields J, Passero V (2016) Tyrosine kinase inhibitor-associated syndrome of inappropriate secretion of anti-diuretic hormone. J Oncol Pharm Pract 22:729–732. https://doi.org/10.1177/1078155215592023
Cheung PW, Nomura N, Nair AV, Pathomthongtaweechai N, Ueberdiek L, Lu HAJ, Brown D, Bouley R (2016) EGF receptor inhibition by erlotinib increases aquaporin 2-mediated renal water reabsorption. J Am Soc Nephrol 27:3105–3116. https://doi.org/10.1681/ASN.2015080903
Erkut ZA, Pool C, Swaab DF (1998) Glucocorticoids suppress corticotropin-releasing hormone and vasopressin expression in human hypothalamic neurons. J Clin Endocrinol Metab 83:2066–2073. https://doi.org/10.1210/jcem.83.6.4881
De Kruif MD, Lemaire LC, Giebelen IA et al (2008) The influence of corticosteroids on the release of novel biomarkers in human endotoxemia. Intensive Care Med 34:518–522. https://doi.org/10.1007/s00134-007-0955-x
Coiro V, Volpi R, Volta E, Melani A, Maffei ML, Chiodera P (2011) Inhibitory effect of dexamethasone on arginine-vasopressin release induced by physical exercise in man. J Investig Med 59:599–601. https://doi.org/10.2310/JIM.0b013e318209a5b3
Mastropietro CW, Miletic K, Chen H, Rossi NF (2014) Effect of corticosteroids on arginine vasopressin after pediatric cardiac surgery. J Crit Care 29:982–986. https://doi.org/10.1016/j.jcrc.2014.07.007
Li Q, Lv F, Wei Y, Yan B, Xie P (2013) Posterior reversible encephalopathy syndrome in a patient with systemic lupus erythematosus after cessation of oral prednisone. Neurol Sci 34:2241–2242. https://doi.org/10.1007/s10072-013-1479-5
Kimura R, Yanagida M, Kugo A, Taguchi S, Matsunaga H (2010) Posterior reversible encephalopathy syndrome in chronic alcoholism with acute psychiatric symptoms. Gen Hosp Psychiatry 32:447.e3–447.e5. https://doi.org/10.1016/j.genhosppsych.2009.11.006
Coppens S, Naeije G, Mavroudakis N (2011) Posterior reversible encephalopathy syndrome following disulfiram intoxication. J Neurol 258:1548–1550. https://doi.org/10.1007/s00415-011-5945-9
Baek HS, Lee S-J (2015) A case of posterior reversible encephalopathy syndrome associated with acute pancreatitis and chronic alcoholism. Gen Hosp Psychiatry 37:192.e3–192.e5. https://doi.org/10.1016/j.genhosppsych.2014.12.004
Godino A, Renard GM (2018) Effects of alcohol and psychostimulants on the vasopressin system: behavioural implications. J Neuroendocrinol 30:e12611. https://doi.org/10.1111/jne.12611
Hundt W, Zimmermann U, Pöttig M et al (2001) The combined dexamethasone-suppression/CRH-stimulation test in alcoholics during and after acute withdrawal. Alcohol Clin Exp Res 25:687–691
Zimmermann U, Hundt W, Spring K, Grabner A, Holsboer F (2003) Hypothalamic-pituitary-adrenal system adaptation to detoxification in alcohol-dependent patients is affected by family history of alcoholism. Biol Psychiatry 53:75–84
Kinoshita H, Jessop DS, Finn DP, Coventry TL, Roberts DJ, Ameno K, Jiri I, Harbuz MS (2001) Acetaldehyde, a metabolite of ethanol, activates the hypothalamic-pituitary-adrenal axis in the rat. Alcohol Alcohol 36:59–64
Edvardsson B (2015) Venlafaxine as single therapy associated with hypertensive encephalopathy. SpringerPlus 4:97. https://doi.org/10.1186/s40064-015-0883-0
Gizowski C, Trudel E, Bourque CW (2017) Central and peripheral roles of vasopressin in the circadian defense of body hydration. Best Pract Res Clin Endocrinol Metab 31:535–546. https://doi.org/10.1016/j.beem.2017.11.001
Filippatos T, Elisaf M, Liamis G (2018) Pharmacological management of hyponatremia. Expert Opin Pharmacother 19:1337–1344. https://doi.org/10.1080/14656566.2018.1504920
Ameli PA, Ameli NJ, Gubernick DM, Ansari S, Mohan S, Satriotomo I, Buckley AK, Maxwell CW Jr et al (2014) Role of vasopressin and its antagonism in stroke related edema. J Neurosci Res 92:1091–1099. https://doi.org/10.1002/jnr.23407
Choi K-S, Cho Y, Jang B-H, Kim W, Ahn C, Lim TH, Yi HJ (2017) Prognostic role of copeptin after traumatic brain injury: a systematic review and meta-analysis of observational studies. Am J Emerg Med 35:1444–1450. https://doi.org/10.1016/j.ajem.2017.04.038
Lehrich RW, Ortiz-Melo DI, Patel MB, Greenberg A (2013) Role of vaptans in the management of hyponatremia. Am J Kidney Dis 62:364–376. https://doi.org/10.1053/j.ajkd.2013.01.034
Acknowledgments
The authors warmly thank Mark Nunn (mark.nunn@gmail.com) for correcting the English.
Author information
Authors and Affiliations
Contributions
Bérenger Largeau conceived the idea, wrote the manuscript, and performed the selection and summary of published literature on the relationship between PRES and AVP. Olivier Le Tilly, Bénédicte Sautenet, Charlotte Salmon Gandonnière, Chantal Barin-Le Guellec, and Stephan Ehrmann helped to design, write, and revise the paper.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Largeau, B., Le Tilly, O., Sautenet, B. et al. Arginine Vasopressin and Posterior Reversible Encephalopathy Syndrome Pathophysiology: the Missing Link?. Mol Neurobiol 56, 6792–6806 (2019). https://doi.org/10.1007/s12035-019-1553-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-019-1553-y