Abstract
Background
With increasing life expectancy, fragility fractures of the pelvic ring (FFP) are becoming frequent. In elderly, osteoporosis leads to a decrease of bone strength and resistance to the ligament’s traction; this represents the most important difference between FFP and fractures in young patients. Usually, these fractures are underestimated and treatment is often conservative.
Aims
To evaluate clinical and surgical outcomes of surgically treated patients with FFP.
Methods
We retrospectively enrolled 14 patients, in our Trauma Center, underwent surgery procedures for FFP between 2012 and 2014. All patients attended clinical and radiological investigation at 1, 3, and 6 months postoperatively and every year after surgery with a mean follow-up of 22 months.
Results
At 6-month follow-up, 11 patients resulted asymptomatic: able to maintain standing position and walk without crunches. Two patients were able to walk with one crunch. The patient with history of previous acetabular fracture walks with two crunches and is still waiting for total hip arthroplasty.
Discussion
The compromised health status and the diminished bone-healing capacity, in elderly, decrease chances for a good clinical outcome. In literature, many authors suggest that mortality rate in patients with FFP is similar to those with hip fracture. Diagnosis of FFP is very important: these fractures are highly disabling in elderly and can lead to displacement and instability. For these reasons, correct diagnosis and well-conduct preoperative plan are necessary to improve stability of fractures and support bone healing. After diagnosis, an anti-osteoporotic treatment is indicated to improve bone quality and bone healing.
Conclusions
Our study shows encouraging results and demonstrates that minimally or less invasive osteosynthesis technique could lead to good outcome in these patients.


Similar content being viewed by others
References
Rommens PM, Wagner D, Hofmann A (2012) Surgical management of osteoporotic pelvic fractures: a new challenge. Eur J Trauma Emerg Surg 38:499–509
Tile M, Hear T, Vrahas M (2003) Biomechanics of the pelvic ring. In: Tile M, Helfet DL, Kellam JF (eds) Fractures of the pelvis and acetabulum, 3rd edn. Lippincott Williams & Wilkins, Philadelphia, pp 32–45
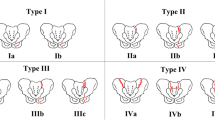
Rommens PM, Hofmann A (2013) Comprehensive classification of fragility fractures of the pelvic ring. Recommendations for surgical treatment. Injury 44:1733–1744
Marrinan S, Pearce MS, Jiang XY et al (2015) Admission for osteoporotic pelvic fractures and predictors of length of hospital stay, mortality and loss of independence. Age Ageing 44:258–261
Benzinger P, Becker C, Kerse N et al (2013) Pelvic fracture rates in community-living people with and without disability and in residents of nursing homes. JAMDA 14:673–678
D’Imporzano M, Liuni FM, Tarantino U (2011) Acetabular fragility fractures in elderly patients. Aging Clin Exp Res 23(2 Suppl):71–73
Rommens PM, Ossendorf C, Pairon P et al (2015) Clinical pathways for fragility fractures of the pelvic ring: personal experience and review of the literature. J Orthop Sci 20:1–11
Rommens PM, Wagner D, Hofmann A (2012) Osteoporotic fractures of the pelvic ring. Z Orthop Unfall 150:e107–e118
Soles GL, Ferguson TA (2012) Fragility fractures of the pelvis. Curr Rev Musculoskelet Med 5:222–228
Krappinger D, Struve P, Schmid R et al (2009) Fractures of the pubic rami: a retrospective review of 534 cases. Arch Orthop Trauma Surg 129:1685–1690
Linstrom NJ, Heiserman JE, Kortman KE et al (2009) Anatomical and biomechanical analyses of the unique and consistent locations of sacral insufficiency fractures. Spine (Phila Pa 1976) 34:309–315
Lefaivre KA, Padalecki JR, Starr AJ (2009) What constitutes a Young and Burgess lateral compression-I (OTA 61-B2) pelvic ring disruption? A description of computed tomography-based fracture anatomy and associated injuries. J Orthop Trauma 23:16–21
Tarantino U, Saturnino L, Scialdoni A et al (2013) Fracture healing in elderly patients: new challenges for antiosteoporotic drugs. Aging Clin Exp Res 25(Suppl 1):S105–S108
Blake SP, Connors AM (2004) Sacral insufficiency fracture. Br J Radiol 77:891–896
Longhino V, Bonora C, Sansone V (2011) The management of sacral stress fractures: current concepts. Clin Cases Miner Bone Metab 8:19–23
Bastian JD, Keel MJ, Heini PF et al (2012) Complications related to cement leakage in sacroplasty. Acta Orthop Belg 78:100–105
Tsiridis E, Upadhyay N, Gamie Z et al (2007) Percutaneous screw fixation for sacral insufficiency fractures: a review of three cases. J Bone Joint Surg Br 89:1650–1653
Butler CL, Given CA II, Michel S et al (2005) Percutaneous sacroplasty for the treatment of sacral insufficiency fractures. AJR 184:1956–1959
Iundusi R, Scialdoni A, Arduini M et al (2013) Stress fractures in the elderly: different pathogenetic features compared with young patients. Aging Clin Exp Res 25(Suppl 1):S89–S91
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Arduini, M., Saturnino, L., Piperno, A. et al. Fragility fractures of the pelvis: treatment and preliminary results. Aging Clin Exp Res 27 (Suppl 1), 61–67 (2015). https://doi.org/10.1007/s40520-015-0430-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-015-0430-4