Abstract
Background
Sarcopenia and osteopenia/osteoporosis show a high prevalence in old age and incur a high risk for falls, fractures, and further functional decline. Physical performance and bone metabolism in patients suffering from the so-called osteosarcopenia—the combination of sarcopenia and osteopenia—are currently still unknown.
Aims
This study investigates physical performance and bone metabolism in osteosarcopenic, prefrail, community-dwelling older adults.
Methods
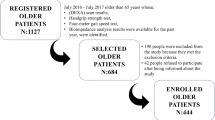
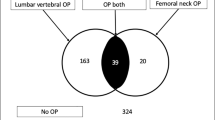
68 prefrail adults between 65 and 94 years were assigned to four groups according to mean DXA results: osteosarcopenic [low T-score and low appendicular lean mass (aLM)], sarcopenic (low aLM), osteopenic (low T-score), and controls. Multiple linear regression analysis, adjusted for age, gender, physical activity, and 25-OH-vitamin D3 serum level, was used to identify the influence of being osteosarcopenic, sarcopenic, or osteopenic on physical performance (hand grip, chair rise test, sit-to-stand power, gait speed, SPPB) and serum markers for increased bone turnover [osteocalcin, β-crosslaps and procollagen type 1 amino-terminal propeptide (P1NP)].
Results
Only osteosarcopenic participants showed significantly reduced hand grip strength, increased chair rising time, and STS power time as well as significantly increased bone turnover markers.
Discussion
Due to low physical performance and high bone turnover, older adults with osteosarcopenia have to be regarded as the most at-risk population for fractures and further functional decline.
Conclusions
Up-to-date osteoporosis and post-fracture management of older persons should aim at both, bone and muscle.

Similar content being viewed by others
References
Kanis JA, on behalf of the World Health Organization Scientific Group. Assessment of osteoporosis at the primary health-care level. Technical Report. World Health Organization Collaborating Centre for Metabolic Bone Diseases, University of Sheffield, UK. 2007: Printed by the University of Sheffield.World Health Organization: Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Technical Report Series 843, Geneva WHO 1994
Thomas DR (2010) Sarcopenia. Clin Geriatr Med 26:331–346
Landi F, Liperoti R, Russo A et al (2012) Sarcopenia as a risk factor for falls in elderly individuals: results from the ilSIRENTE study. Clin Nutr 31:652–658
Isaacson J, Brotto M (2014) Physiology of mechanotransduction: how do muscle and bone “talk” to one another? Clin Rev Bone Miner Metab 12:77–85
Edwards MH, Dennison EM, Aihie Sayer A et al (2015) Osteoporosis and sarcopenia in older age. Bone 80:126–130
Kawao N, Kaji H (2015) Interactions between muscle tissues and bone metabolism. J Cell Biochem 116:687–695
Garnero P, Sornay-Rendu E, Duboeuf F et al (1999) Markers of bone turnover predict postmenopausal forearm bone loss over 4 years: the OFELY study. J Bone Miner Res 14:1614–1621
Binkley N, Buehring B (2009) Beyond FRAX??: it’s time to consider “sarco-osteopenia”. J Clin Densitom 12:413–416
Kull M, Kallikorm R, Lember M (2012) Impact of a new sarco-osteopenia definition on health-related quality of life in a population-based cohort in northern Europe. J Clin Densitom 15:32–38
Yu R, Leung J, Woo J (2014) Incremental predictive value of sarcopenia for incident fracture in an elderly Chinese cohort: results from the Osteoporotic Fractures in Men (MrOs) Study. J Am Med Dir Assoc 15:551–558
Huo YR, Suriyaarachchi P, Gomez F et al (2015) Phenotype of osteosarcopenia in older individuals with a history of falling. J Am Med Dir Assoc 16:290–295
Drey M, Pfeifer K, Sieber CC et al (2010) The fried frailty criteria as inclusion criteria for a randomized controlled trial: personal experience and literature review. Gerontology 57:11–18
Fried LP, Tangen CM, Walston J et al (2001) Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 56:M146–M156
Guralnik JM, Simonsick EM, Ferrucci L et al (1994) A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 49:M85–M94
Lindemann U, Claus H, Stuber M et al (2003) Measuring power during the sit-to-stand transfer. Eur J Appl Physiol 89:466–470
Liu CK, Fielding RA (2011) Exercise as an intervention for frailty. Clin Geriatr Med 27:101–110
Pereira FB, Leite AF, De Paula AP (2015) Relationship between pre-sarcopenia, sarcopenia and bone mineral density in elderly men. Arch Endocrinol Metab 59:59–65
Cederholm T, Cruz-Jentoft AJ, Maggi S (2013) Sarcopenia and fragility fractures. Eur J Phys Rehabil Med 49:111–117
Rizzoli R, Stevenson JC, Bauer JM et al (2014) The role of dietary protein and vitamin D in maintaining musculoskeletal health in postmenopausal women: a consensus statement from the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO). Maturitas 79:122–132
Zoch ML, Clemens TL, Riddle RC (2015) New insights into the biology of osteocalcin. Bone 8:229–236
Acknowledgement
The authors want to thank the volunteer participants and John Hoppe for providing language help.
The members of the FiAT intervention group: Astrid Zech, Department of Exercise Physiology, Institute of Sports Science, Friedrich Schiller University of Jena, Jena, Germany; Ellen Freiberger, Institute for Biomedicine of Aging, University of Erlangen-Nürnberg, Nürnberg, Germany; Klaus Pfeifer, University of Erlangen-Nürnberg, Institute of Sport Science and Sport, Erlangen, Germany.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Funding
Michael Drey and Jürgen M. Bauer were supported by a Forschungskolleg Geriatrie Grant from the Robert Bosch Foundation, Stuttgart, Germany. The reagents for bone marker measurements were kindly provided from Roche Diagnostics.
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
The members of the FiAT intervention group are mentioned in the Acknowledgement.
Rights and permissions
About this article
Cite this article
Drey, M., Sieber, C.C., Bertsch, T. et al. Osteosarcopenia is more than sarcopenia and osteopenia alone. Aging Clin Exp Res 28, 895–899 (2016). https://doi.org/10.1007/s40520-015-0494-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-015-0494-1