Abstract
Objective
Breast cancer is the leading cause of cancer death among Hispanic women. Unfortunately, few studies disaggregate Hispanic patients by race to understand its implications on treatment and clinical outcomes such as mortality. The aim of this study is to examine surgical management and overall mortality among different subgroups of women who self-identify as Hispanic.
Methods
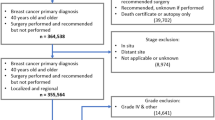
Hispanic female patients, ages 18–90, stages I–III, diagnosed with breast cancer between 2010 and 2015 from the National Cancer Data Base were identified. The study cohort was divided into three ethnoracial categories: (1) Hispanic White (HW), 2) Hispanic Black (HB), and 3) Hispanic Other (HO). Descriptive statistics and multivariate models were constructed to determine the relationship between sociodemographic factors, clinical variables, surgical management, and mortality when disaggregated by race.
Results
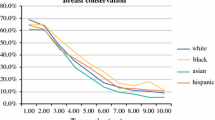
There were 56,675 Hispanic women who met the study criteria. Most where HW (n=50,599, 89.3%) and the rest were HB (n=1,334, 2.4%) and HO (n=4,742, 8.3%). There was no difference between the three groups on receipt of breast conservation therapy (P=0.12). HB (48.5%) and HO (46.6%) women were more likely to undergo reconstruction than those who identified as HW (38.7%) (P<0.001). Additionally, HB (38.3%) women were more likely to undergo tissue-based reconstruction than HW (29.0%) and HO women (30%) (P=0.0008). There was no difference between the groups in the utilization of contralateral prophylactic mastectomy (CPM) (P=0.078). On multivariable analysis, there was no difference in mortality between HB and HW patients (HR 1.18, 95%CI 0.92–1.51; Ref HW). However, HO women had a 24% relative risk reduction in mortality (HR 0.76, 95% CI 0.63–0.92; HW ref).
Conclusion
Findings from this study suggest there are ethnoracial disparities in reconstruction utilization and mortality among Hispanic women. Future studies should examine how culture, language, healthcare access, and patient preferences contribute to these disparities.

Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the American College of Surgeons and the American Cancer Society, but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are however available from the authors upon reasonable request and with permission of the American College of Surgeons and the American Cancer Society.
The National Cancer Database (NCDB) is a joint project of the Commission on Cancer (CoC) of the American College of Surgeons and the American Cancer Society. The CoC 's NCDB and the hospitals participating in the CoC’s NCDB are the source of the de-identified data used herein; they have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors
Code Availability
Not applicable.
References
Haile RW, John EM, Levine AJ, Cortessis VK, Unger JB, Gonzales M, et al. A review of cancer in U.S. Hispanic populations. Cancer Prev Res (Phila). 2012;5(2):150–63.
DeSantis CE, Ma J, Goding Sauer A, Newman LA, Jemal A. Breast cancer statistics, 2017, racial disparity in mortality by state. CA Cancer J Clin. 2017;67(6):439–48.
Lynce F, Graves KD, Jandorf L, Ricker C, Castro E, Moreno L, et al. Genomic disparities in breast cancer among Latinas. Cancer Control. 2016;23(4):359–72.
Akinyemiju T, Sakhuja S, Vin-Raviv N. Racial and socio-economic disparities in breast cancer hospitalization outcomes by insurance status. Cancer Epidemiol. 2016;43:63–9.
Sighoko D, Hunt BR, Irizarry B, Watson K, Ansell D, Murphy AM. Disparity in breast cancer mortality by age and geography in 10 racially diverse US cities. Cancer Epidemiol. 2018;53:178–83.
Iqbal J, Ginsburg O, Rochon PA, Sun P, Narod SA. Differences in breast cancer stage at diagnosis and cancer-specific survival by race and ethnicity in the United States. JAMA. 2015;313(2):165–73.
Warner ET, Tamimi RM, Hughes ME, Ottesen RA, Wong YN, Edge SB, et al. Racial and ethnic differences in breast cancer survival: mediating effect of tumor characteristics and sociodemographic and treatment factors. J Clin Oncol. 2015;33(20):2254–61.
Ooi SL, Martinez ME, Li CI. Disparities in breast cancer characteristics and outcomes by race/ethnicity. Breast Cancer Res Treat. 2011;127(3):729–38.
Pinheiro PS, Callahan KE, Siegel RL, Jin H, Morris CR, Trapido EJ, et al. Cancer mortality in Hispanic ethnic groups. Cancer Epidemiol Biomark Prev. 2017;26(3):376–82.
National Cancer Database [https://www.facs.org/quality-programs/cancer/ncdb]
National Cancer Database Participants User File (PUF) 2017 Data Dictionary [https://www.facs.org/-/media/files/quality-programs/cancer/ncdb/puf_data_dictionary_2017.ashx]
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines), Breast Cancer [https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf]
DeSantis CE, Ma J, Gaudet MM, Newman LA, Miller KD, Goding Sauer A, et al. Breast cancer statistics, 2019. CA Cancer J Clin. 2019;69(6):438–51.
Jackson DK, Li Y, Eskander MF, Tsung A, Oppong BA, Bhattacharyya O, et al. Racial disparities in low-value surgical care and time to surgery in high-volume hospitals. J Surg Oncol. 2021;123(2):676–86.
Alderman AK, Hawley ST, Janz NK, Mujahid MS, Morrow M, Hamilton AS, et al. Racial and ethnic disparities in the use of postmastectomy breast reconstruction: results from a population- based study. J Clin Oncol. 2009;27(32):5325–30.
Shi R, Taylor H, McLarty J, Liu L, Mills G, Burton G. Effects of payer status on breast cancer survival: a retrospective study. BMC Cancer. 2015;15:211.
Mamounas EP. NSABP breast cancer clinical trials: recent results and future directions. Clin Med Res. 2003;1(4):309–26.
Ambroggi M, Biasini C, Del Giovane C, Fornari F, Cavanna L. Distance as a barrier to cancer diagnosis and treatment: review of the literature. Oncologist. 2015;20(12):1378–85.
Braithwaite D, Moore DH, Satariano WA, Kwan ML, Hiatt RA, Kroenke C, Caan BJ. Prognostic impact of comorbidity among long-term breast cancer survivors: results from the LACE study. Cancer Epidemiol Biomarkers Prev. 2012;21(7):1115–25.
Butler PD, Familusi O, Serletti JM, Fox JP. Influence of race, insurance status, and geographic access to plastic surgeons on immediate breast reconstruction rates. Am J Surg. 2018;215(6):987–94.
Nelson JA, Nelson P, Tchou J, Serletti JM, Wu LC. The ethnic divide in breast reconstruction: a review of the current literature and directions for future research. Cancer Treat Rev. 2012;38(5):362–7.
Tseng JF, Kronowitz SJ, Sun CC, Perry AC, Hunt KK, Babiera GV, et al. The effect of ethnicity on immediate reconstruction rates after mastectomy for breast cancer. Cancer. 2004;101(7):1514–23.
Roughton MC, DiEgidio P, Zhou L, Stitzenberg K, Meyer AM. Distance to a plastic surgeon and type of insurance plan are independently predictive of postmastectomy breast reconstruction. Plast Reconstr Surg. 2016;138(2):203e–11e.
Obeng-Gyasi S, Timsina L, Miller KD, Ludwig KK, Fisher CS, Haggstrom DA. The implications of insurance status on presentation, surgical management, and mortality among nonmetastatic breast cancer patients in Indiana. Surgery. 2018;164(6):1366–71.
Abdel-Rahman O. Impact of NCI socioeconomic index on the outcomes of nonmetastatic breast cancer patients: analysis of SEER census tract-level socioeconomic database. Clin Breast Cancer. 2019;19(6):e717–22.
Newman LA, Mason J, Cote D, Vin Y, Carolin K, Bouwman D, et al. African-American ethnicity, socioeconomic status, and breast cancer survival: a meta-analysis of 14 studies involving over 10,000 African-American and 40,000 White American patients with carcinoma of the breast. Cancer. 2002;94(11):2844–54.
Champion CD, Thomas SM, Plichta JK, Parrilla Castellar E, Rosenberger LH, Greenup RA, et al. Disparities at the intersection of race and ethnicity: examining trends and outcomes in Hispanic women with breast cancer. JCO Oncol Pract. 2020:Op2000381.
Adhikari K, Chacón-Duque JC, Mendoza-Revilla J, Fuentes-Guajardo M, Ruiz-Linares A. The genetic diversity of the Americas. Annu Rev Genomics Hum Genet. 2017;18:277–96.
González Burchard E, Borrell LN, Choudhry S, Naqvi M, Tsai HJ, Rodriguez-Santana JR, et al. Latino populations: a unique opportunity for the study of race, genetics, and social environment in epidemiological research. Am J Public Health. 2005;95(12):2161–8.
Funding
Samilia Obeng-Gyasi is funded by the Paul Calabresi Career Development Award (K12 CA133250).
Author information
Authors and Affiliations
Contributions
Conception or design of the work: Ahamd Hamad, Yaming Li, Allan Tsung, Bridget Oppong, Mariam Eskander, Oindrila Bhattacharyya, and Samilia Obeng-Gyasi.
Data collection: Ahamd Hamad, Yaming Li, Allan Tsung, Bridget Oppong, Mariam Eskander, Oindrila Bhattacharyya, and Samilia Obeng-Gyasi.
Data analysis and interpretation: Ahamd Hamad, Yaming Li, Allan Tsung, Bridget Oppong, Mariam Eskander, Oindrila Bhattacharyya, and Samilia Obeng-Gyasi.
Drafting the article: Ahamd Hamad, Yaming Li, Allan Tsung, Bridget Oppong, Mariam Eskander, Oindrila Bhattacharyya, and Samilia Obeng-Gyasi.
Critical revision of the article: Ahamd Hamad, Yaming Li, Allan Tsung, Bridget Oppong, Mariam Eskander, Oindrila Bhattacharyya, and Samilia Obeng-Gyasi.
Corresponding author
Ethics declarations
Ethical Approval Statement
For this type of study, formal consent is not required.
Ethics Approval
The Ohio State University Office of Responsible Research Practices deemed this study IRB exempt.
Consent to Participate
This study was a retrospective review of a National Cancer database and no consent to participate was required.
Consent for Publication
This study was a retrospective review of a National Cancer database and no consent to publish study results was required.
Conflict of Interest/Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
Unadjusted and adjusted examination of differences in survival by race (DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Hamad, A., Li, Y., Tsung, A. et al. Hispanic Ethnicity and Breast Cancer: Disaggregating Surgical Management and Mortality by Race. J. Racial and Ethnic Health Disparities 9, 1568–1576 (2022). https://doi.org/10.1007/s40615-021-01096-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-021-01096-3